Will I Have Other Treatments In Addition To Hormone Therapy
Your RMCC oncologist may recommend using hormone therapy in combination with other cancer treatments, such as chemotherapy and radiation therapy. When used with other treatments, hormone therapy can:
- Make a tumor smaller before surgery or radiation therapy. This is called neoadjuvant therapy.
- Lower the risk that cancer will come back after the primary treatment. This is called adjuvant therapy.
- Destroy cancer cells that have returned or spread to other parts of your body.
How To Not Get Picked For Grand Jury Duty Reddit
According to an article published in the Journal of Clinical Oncology, the timing of initiation of androgen deprivation therapy for the treatment of early-stage prostate cancer should be individualized, with each patient weighing individual side effects against outcomes.. Besides skin cancer, prostate cancer is the most commonly diagnosed cancer in men in the U.S. Anemia is when your body’s level of red blood cells goes below normal. When you do not have enough red blood cells, your body parts do not get enough oxygen. As a result, they cannot work the way they should and cause problems.You can develop anemia if your body does not make enough red blood cells or destroys them. You can also develop anemia if you lose too much.
Options In Hormone Therapy
Testosterone levels in the body can be reduced either surgically or with drugs. The surgical option is castration, achieved by removing the testicles during a bilateral orchiectomy. Once the only option, it has since been supplanted by drugs that lower testosterone levels to amounts achieved by surgery.
For men, normal testosterone levels range from 300 to 1,000 ng/dl. The FDA requires that any new drug used in hormone therapy for prostate cancer lower testosterone levels to 50 ng/dl or less. In my practice, I usually try to lower levels even further, to 20 ng/dl.
Dont Miss: What Causes Breakthrough Bleeding When On Bioidentical Hormones
Recommended Reading: Johns Hopkins Prostate Cancer Second Opinion
Intermittent Hormonal Therapy For Locally Advanced Prostate Cancer
Intermittent hormonal therapy is where you stop taking the drugs and after a while start taking them again. This may be an option for locally-advanced prostate cancer. It gives you a break from the side effects of hormonal therapy.
Intermittent hormonal therapy is not suitable for everyone and should only be done on your doctors advice. Your doctor can explain more about this. They usually measure your PSA level using the PSA test every 3 months. If it goes up to a certain level or you get symptoms, your doctor will advise you to start hormonal therapy again.
A New Treatment Standard
 Niruja HealthTech” alt=”Side Effects of Hormone Therapy > Niruja HealthTech”>
Niruja HealthTech” alt=”Side Effects of Hormone Therapy > Niruja HealthTech”> Still, some men have difficulty tolerating ADT, and not all of them should get it, particularly if theyre older and more likely to die of something other than prostate cancer. Id reserve ADT for younger men with a long life expectancy ahead of them who were diagnosed initially with high-grade or late-stage disease, Thompson said.
This important study confirms that combined therapy is superior to radiation alone and should be viewed as the standard treatment for PSA relapse, said Dr. Marc Garnick, the Gorman Brothers Professor of Medicine at Harvard Medical School and Beth Israel Deaconess Medical Center, and editor in chief of HarvardProstateKnowledge.org. High dose bicalutamide has been associated with cardiovascular side effects, but ongoing and future research is clarifying how best to use ADT in this particular setting.
Also Check: How Do They Do A Biopsy Of Your Prostate
What Are Male Sex Hormones
Hormones are substances that are made by glands in the body. Hormones circulate in the bloodstream and control the actions of certain cells or organs.
Androgens are a class of hormones that control the development and maintenance of male characteristics. The most abundant androgens in men are testosterone and dihydrotestosterone .
Androgens are required for normal growth and function of the prostate, a gland in the male reproductive system that helps make . Androgens are also necessary for prostate cancers to grow. Androgens promote the growth of both normal and cancerous prostate cells by binding to and activating the androgen receptor, a protein that is expressed in prostate cells . Once activated, the androgen receptor stimulates the expression of specific genes that cause prostate cells to grow .
Almost all testosterone is produced in the testicles a small amount is produced by the adrenal glands. Although prostate cells do not normally make testosterone, some prostate cancer cells acquire the ability to do so .
What Types Of Hormone Therapy Are Used For Prostate Cancer
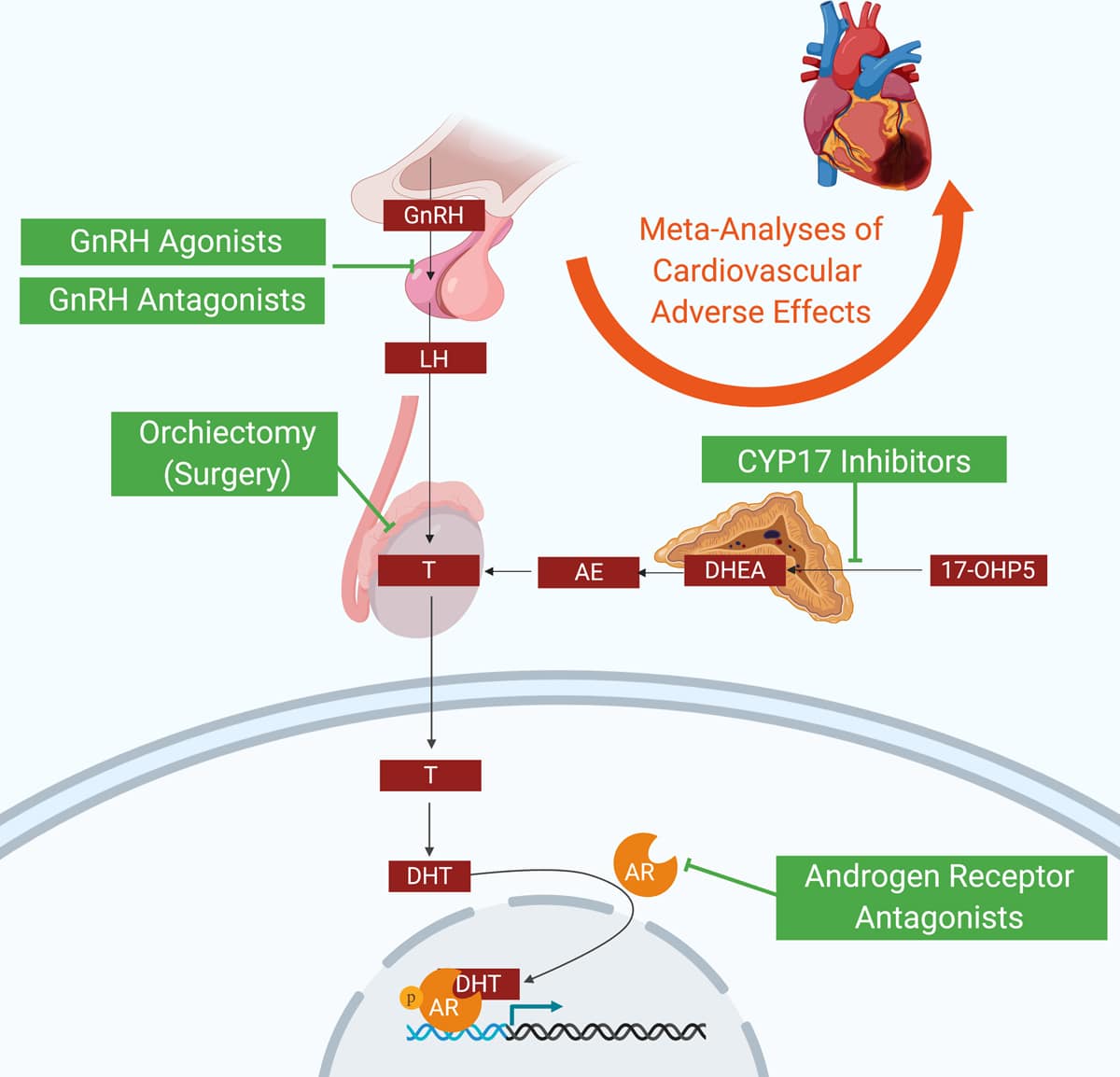
Hormone therapy for prostate cancer can block the production or use of androgens . Currently available treatments can do so in several ways:
- reducing androgen production by the testicles
- blocking the action of androgens throughout the body
- block androgen production throughout the body
Treatments that reduce androgen production by the testicles are the most commonly used hormone therapies for prostate cancer and the first type of hormone therapy that most men with prostate cancer receive. This form of hormone therapy includes:
Treatments that block the action of androgens in the body are typically used when ADT stops working. Such treatments include:
Treatments that block the production of androgens throughout the body include:
Read Also: Prostate Cancer Scale 1 5
Surgically Removing The Prostate Gland
A radical prostatectomy is the surgical removal of your prostate gland. This treatment is an option for curing prostate cancer that has not spread beyond the prostate or has not spread very far.
Like any operation, this surgery carries some risks, such as urinary incontinence and erectile dysfunction.
In extremely rare cases, problems arising after surgery can be fatal.
Its possible that prostate cancer can come back again after treatment. Your doctor should be able to explain the risk of your cancer coming back after treatment, based on things like your PSA level and the stage of your cancer.
Studies have shown that radiotherapy after prostate removal surgery may increase the chances of a cure, although research is still being carried out into when it should be used after surgery.
You may want to ask your doctors about storing a sperm sample before the operation so it can be used later for in vitro fertilisation .
Drugs That Lower Androgen Levels
The most common treatment is to take drugs that lower the amount of androgens made by the testicles. They are called luteinizing hormone-releasing hormone analogs and anti-androgens . These drugs lower androgen levels just as well as surgery does. This type of treatment is sometimes called chemical castration.
Men who receive androgen deprivation therapy should have follow-up exams with the doctor prescribing the drugs:
- Within 3 to 6 months after starting therapy
- At least once a year, to monitor blood pressure and perform blood sugar and cholesterol tests
- To get PSA blood tests to monitor how well the therapy is working
LH-RH analogs are given as a shot anywhere from once a month to every 6 months. These drugs include:
LH-RH antagonists are another class of treatments, including degarelix and relugolix . They reduce androgen levels more quickly and have fewer side effects. LH-RH antagonists are used in men with advanced cancer.
Some doctors recommend stopping and restarting treatment . This approach appears to help reduce hormone therapy side effects. However, it is not clear if intermittent therapy works as well as continuous therapy. Some studies indicate that continuous therapy is more effective or that intermittent therapy should only be used for select types of prostate cancer.
Also Check: What Is Good To Take For Prostate Health
Male Hormones And Prostate Cancer
Androgens are male sex hormones. Testosterone is one main type of androgen. Most testosterone is made by the testicles. The adrenal glands also produce a small amount.
Androgens cause prostate cancer cells to grow. Hormone therapy for prostate cancer lowers the effect level of androgens in the body. It can do this by:
- Stopping the testicles from making androgens using surgery or medicines
- Blocking the action of androgens in the body
- Stopping the body from making androgens
When Hormone Therapy Is Recommended
Hormone therapy is typically given to patients with intermediate- or high-risk prostate cancer. It may be used in the following ways:
- In combination with radiation, mostly for patients with high Gleason scores or other high-risk factors.
- After radiation or surgery when PSA rises, indicating a recurrence.
- As therapy for patients unsuitable for radiation or surgery.
- As therapy for metastatic prostate cancer . It may be given instead of or in combination with chemotherapy.
HT is usually not prescribed for:
- Patients choosing a localized treatment for low-risk prostate cancer
- Low-risk patients preferring to monitor their cancer on an active surveillance program
HT may be an option for patients who are not candidates for surgery, radiation or other localized treatment because of age, pre-existing health conditions or concerns about potential side effects of localized treatments.
You May Like: How To Heal Your Prostate
What Is Advanced Prostate Cancer
When prostate cancer spreads beyond the prostate or returns after treatment, it is often called advanced prostate cancer.
Prostate cancer is often grouped into four stages, with stages III and IV being more advanced prostate cancer.
- Early Stage | Stages I & II: The tumor has not spread beyond the prostate.
- Locally Advanced | Stage III: Cancer has spread outside the prostate but only to nearby tissues.
- Advanced | Stage IV: Cancer has spread outside the prostate to other parts such as the lymph nodes, bones, liver or lungs.
When an early stage prostate cancer is found, it may be treated or placed on surveillance . Advanced prostate cancer is not curable, but there are many ways to treat it. Treatment can help slow advanced prostate cancer progression.
There are several types of advanced prostate cancer, including:
Biochemical Recurrence
With biochemical recurrence, the prostate-specific antigen level has risen after treatment using surgery or radiation, with no other sign of cancer.
Castration-Resistant Prostate Cancer
Non-Metastatic Castration-Resistant Prostate Cancer
Prostate cancer that no longer responds to hormone treatment and is only found in the prostate. This is found by a rise in the PSA level, while the testosterone level stays low. Imaging tests do not show signs the cancer has spread.
Metastatic Prostate Cancer
- Other organs, such as liver or lungs
Metastatic Hormone-Sensitive Prostate Cancer
Dont Miss: Does Blue Cross Cover Testosterone
Side Effects Of Hormone Therapy
Testosterone is the primary male hormone, and plays an important role in establishing and maintaining typical male characteristics, such as body hair growth, muscle mass, sexual desire, and erectile function, and contributes to a host of other normal physiologic processes in the body. The primary systemic treatment for prostate cancer, androgen deprivation therapy , lowers testosterone and causes side effects related to reversing all of the normal functions of testosterone.
Although most men may experience only a few of these symptoms, the list of potential effects of testosterone loss is long: hot flashes, decreased sexual desire, loss of bone density and increased fracture risk , erectile dysfunction, fatigue, increased risk of diabetes and heart attacks, weight gain, decreased muscle mass, anemia, and memory loss. Bad cholesterol levels rise, particularly LDL and total cholesterol, and muscle tends to get replaced by fat, especially around the abdomen.
Current research indicates a weak link between prolonged ADT and increased risk of dementia in a subsequent study, no increased risk was shown between ADT and Alzheimers. While substitute therapies for ADT are an active area of research for the Prostate Cancer Foundation, ADT is currently a part of the standard of care. While its important to be aware of the possible side effects, it should not affect your decision to receive life-extending care.
Side Effects of 2nd-Generation Hormone Therapy
Recommended Reading: Vaccine Therapy For Prostate Cancer
Sparco Steering Wheel Flat Bottom
Men with hormone-resistant prostatecancer aren’t candidates for further hormonetherapy. Common side effects The most common side effects of hormone therapies include: hot flashes thinning,. . Prior local therapy to treat prostate cancer Prior therapy to a metastatic site. Prior or ongoing systemic therapy for prostate cancer including, but not limited to: 1. Hormonal therapy 2.
Checking Your Hormone Therapy Is Working
Youll have regular blood tests to check the level of a protein called prostate specific antigen . PSA is a protein made by both normal and cancerous prostate cells. It is in the blood in small amounts in all men, unless they have had their prostate gland completely removed.
While the hormone therapy is working, the level of PSA should stay stable or may go down. But if prostate cancer cells are starting to grow and develop, the level of PSA may go up. Then your doctor may need to change your treatment. They will discuss this with you.
Also Check: Best Supplement For Mens Prostate
Read Also: How Is The Prostate Removed
Cancer That Clearly Has Spread
If the cancer has spread outside the prostate, it will most likely go to nearby lymph nodes first, and then to bones. Much less often the cancer will spread to the liver or other organs.
When prostate cancer has spread to other parts of the body , hormone therapy is probably the most effective treatment. But it isnt likely to cure the cancer, and at some point it might stop working. Usually the first treatment is a luteinizing hormone-releasing hormone agonist, LHRH antagonist, or orchiectomy, sometimes along with an anti-androgen drug or abiraterone. Another option might be to get chemotherapy along with the hormone therapy. Other treatments aimed at bone metastases might be used as well.
Recommended Reading: Blue Cross Blue Shield Trt
Intermittent Versus Continuous Hormone Therapy
Most prostate cancers treated with hormone therapy become resistant to this treatment over a period of months or years. Some doctors believe that constant androgen suppression might not be needed, so they advise intermittent treatment. This can allow for a break from side effects like decreased energy, sexual problems, and hot flashes.
In one form of intermittent hormone therapy, treatment is stopped once the PSA drops to a very low level. If the PSA level begins to rise, the drugs are started again. Another form of intermittent therapy uses hormone therapy for fixed periods of time for example, 6 months on followed by 6 months off.
At this time, it isnt clear how this approach compares to continuous hormone therapy. Some studies have found that continuous therapy might help men live longer, but other studies have not found such a difference.
Recommended Reading: Prostate Cancer Spread To Spine
How Is Hormone Therapy Used To Treat Hormone
Hormone therapy may be used in several ways to treat hormone-sensitive prostate cancer, including:
Early-stage prostate cancer with an intermediate or high risk of recurrence. Men with early-stage prostate cancer that has an intermediate or high risk of recurrence often receive hormone therapy before, during, and/or after radiation therapy, or after prostatectomy . Factors that are used to determine the risk of prostate cancer recurrence include the grade of the tumor , the extent to which the tumor has spread into surrounding tissue, and whether tumor cells are found in nearby lymph nodes during surgery.
The use of hormone therapy before prostatectomy has not been shown to be of benefit and is not a standard treatment. More intensive androgen blockade prior to prostatectomy is being studied in clinical trials.
Relapsed/recurrent prostate cancer. Hormone therapy used alone is the standard treatment for men who have a prostate cancer recurrence as documented by CT, MRI, or bone scan after treatment with radiation therapy or prostatectomy.
Hormone therapy is sometimes recommended for men who have a “biochemical” recurrencea rise in prostate-specific antigen level following primary local treatment with surgery or radiationespecially if the PSA level doubles in fewer than 3 months.
What Is Hormone Therapy For Cancer
Also referred to as hormonal or endocrine therapy, this cancer treatment is different from menopausal hormone replacement therapy , which refers to the prescription of supplemental hormones to help relieve the symptoms of menopause.
Certain cancers rely on hormones to grow. In these cases, hormone therapy may slow or stop their spread by blocking the bodys ability to produce these particular hormones or changing how hormone receptors behave in the body.
Breast and prostate cancers are the two types most commonly treated with hormone therapy. Most breast cancers have either estrogen or progesterone receptors, or both, which means they need these hormones to grow and spread. By contrast, prostate cancer needs testosterone and other male sex hormones, such as dihydrotestosterone , to grow and spread. Hormone therapy may help make these hormones less available to growing cancer cells.
Hormone therapy is available via pills, injection or surgery that removes hormone-producing organs, namely the ovaries in women and the testicles in men. Its typically recommended along with other cancer treatments.
If hormone therapy is part of your treatment plan, discuss potential risks or side effects with your care team so that you know what to expect and can take steps to reduce them. Let doctors know about all your other medications to avoid interactions.
Don’t Miss: What Does Grade 4 Prostate Cancer Mean
High Intensity Focused Ultrasound
High intensity focused ultrasound was first used in the 1940s and 1950s in efforts to destroy tumors in the central nervous system. Since then, HIFU has been shown to be effective at destroying malignant tissue in the brain, prostate, spleen, liver, kidney, breast, and bone.
HIFU for prostate cancer utilizes ultrasound to ablate/destroy the tissue of the prostate. During the HIFU procedure, sound waves are used to heat the prostate tissue, thus destroying the cancerous cells. In essence, ultrasonic waves are focused on specific areas of the prostate to eliminate the prostate cancer, with minimal risks of affecting other tissue or organs. Temperatures at the focal point of the sound waves can exceed 100 °C . However, many studies of HIFU were performed by manufacturers of HIFU devices, or members of manufacturers advisory panels.
Contraindications to HIFU for prostate cancer include a prostate volume larger than 40 grams, which can prevent targeted HIFU waves from reaching the anterior and anterobasal regions of the prostate, anatomic or pathologic conditions that may interfere with the introduction or displacement of the HIFU probe into the rectum, and high-volume calcification within the prostate, which can lead to HIFU scattering and transmission impairment.