After Prostatectomy: What To Expect
At the hospital : You should expect to be in the hospital for one night. At Johns Hopkins, all rooms on the urology floor are private. Here, nurses help patients get moving shortly after surgery to prevent blood clots and other postoperative risks.
First few days at home : After youre sent home, you might find that regular ibuprofen or acetaminophen will be sufficient pain management for the first few days. If over-the-counter medications arent enough, your doctor can help you with alternatives.
One week after surgery : After your surgery site heals, your catheter will be removed. This is usually seven to 10 days after surgery. This can easily be done at your doctors office. Some people decide to take out their catheter at home. If thats the case, ask your doctor for instructions first.
This is also about the time your surgeon will call you with the final pathology results. He or she will discuss what you should know and whether further treatment is necessary.
One month after surgery : Doctors recommend no strenuous activity or heavy lifting for at least one month after surgery. Most people take off work for three to four weeks. If you work from home, you could return to work sooner.
- Urinary incontinence
- Erectile dysfunction
Recovery from surgery takes time. These side effects are often temporary. However, if they are affecting your quality of life, ask your doctor about options that can help.
Persistent Psa After Radical Prostatectomy How To Interpret The Data
Although PSA should be 0 after surgery, some patients are faced with one of two scenarios: PSA recurrence or PSA persistence.Persistent PSA after radical prostatectomy is the detection of a PSA higher than 0 within the first three months after prostatectomy. The distinction is that the PSA has not recurred, but rather persisted after surgery.
The key difference this small distinction makes is the prediction of the course the disease will take. A persistent PSA after radical prostatectomy or other forms of treatment can, unfortunately, mean cancer has progressed and metastasized. In many cases, the best course of secondary treatment is hormone therapy.
Radical Prostatectomy Retropubic Or Suprapubic Approach
You’ll be positioned on the operating table, lying on your back.
An incision will be made from below the navel to the pubic region.
The doctor will usually perform a lymph node dissection first. The nerve bundles will be released carefully from the prostate gland and the urethra will be identified. The seminal vesicles may also be removed if necessary.
The prostate gland will be removed.
A drain will be inserted, usually in the right lower area of the incision.
Recommended Reading: Herbal Treatment For Enlarged Prostate
Does Viagra And Cialis Work After Prostate Removal
During recovery, medications like Viagra and Cialis will help. Viagra can restore impotence and contributes to more pleasurable sex life.
A study published in the Journal of Urology reported that 53% from a total of 80 men who underwent radical prostatectomy had their erection function restored after taking Viagra.
But is Viagra an addictive drug?
Many men experienced a high rate of improvement in their sexual performance due to medications such as Viagra, Cialis, or Levitra. If you have been wondering whether these medications are addictive, you should know that the active ingredient in Viagra, sildenafil, is not an addictive substance.
These medications work by increasing the blood flow to the penis and facilitate the erection process. Addiction is brain-triggered, but Viagra does not target the nervous processes in the brain. That is why it is considered a safe option for those who want to faster recover their sexual potency after prostate cancer treatment.
Read Also: Will Prostatitis Go Away On Its Own
What Happens After Urethral Sling Surgery
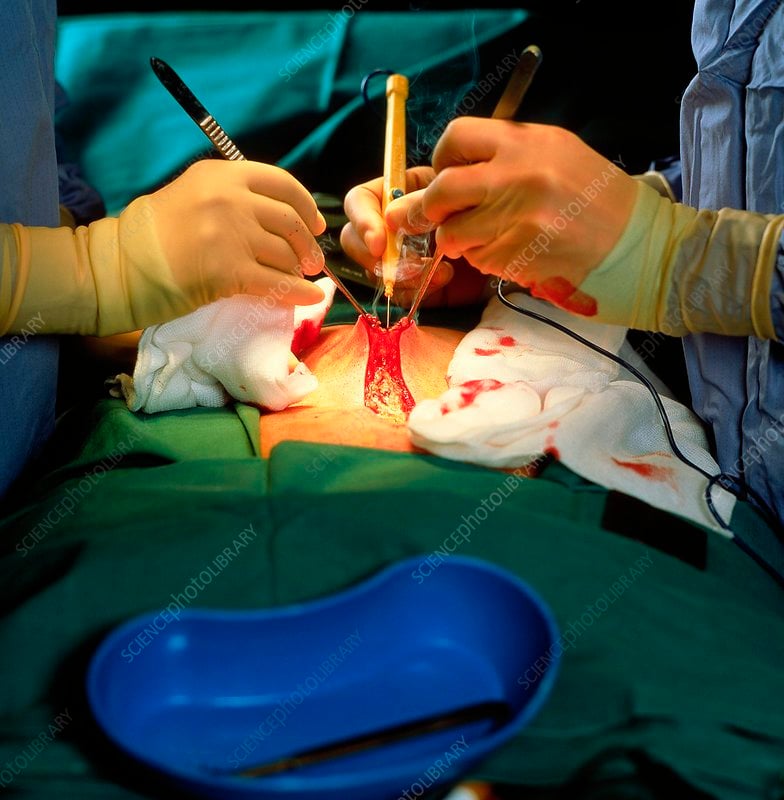
Patients usually recover from this surgery quickly. It’s best to limit demanding activities for approximately six weeks after surgery to avoid having the sling loosen before healing is complete.
After surgery, there may be swelling that makes it difficult to urinate. You’ll have a catheter coming out of the urethra for two to three days. After this, the catheter is removed and just about everyone is able to void on their own. In rare cases, the catheter may have to be reinserted for a few days or up to a week if you cannot urinate.
After the swelling goes down, youll gradually be able to urinate on your own and empty your bladder. However, your normal urination pattern may not return for a few weeks.
The majority of men who’ve had this procedure have been cured of their urinary incontinence and no longer use pads. The others usually improve to the point where they don’t use as many pads as they were before.
Don’t Miss: What Are The Side Effects Of Prostate Radiation Therapy
Penile Rehabilitation After Prostate Removal May Include:
- Prescription medications. Medications, called phosphodiesterase-5 inhibitors, work for many men unless their nerve bundles were damaged or removed. These medications include Viagra and Cialis.
- An injection. Your body makes prostaglandin E1, a substance that helps your body have an erection. A made-made version is now available. Your doctor can teach you to inject this at the base of your penis about 5-to-10 minutes before intercourse. The injection is virtually painless this medication is also available as a suppository placed into the tip of your penis.
- Vacuum devices. These devices draw the air from around your penis. The vacuum created brings blood into your penis, creating an erection.
- Penile implants. A device is surgically implanted into your penis. Penile implants provide a lasting solution for ED, lasting 10 or 15 years. There are risks, but if none of the other penile rehabilitation methods work, many men agree that a penile implant is a cosmetically-acceptable solution for their prostate cancer-related erectile dysfunction.
Interpreting The Data On Prostate Cancer Recurrence
Depending on these factors, secondary treatment can be individualized to best manage the case at hand. Using the PSA in this way can be crucial in mapping out a predicted course of the disease and helping patients manage their disease as best as possible. Some factor combinations could predict a localized, slow-moving cancer best treated and cured with radiation therapy by targeting the remaining prostate cells. For example, if the Gleason score is less than 7, the PSA level started to rise more than 2 years after surgery and the PSA Doubling Time is almost a year, the chances to be cancer-free for a longer period of time are higher. .
Other factor combinations could predict aggressive, metastatic disease, in which case hormonal treatment may be the best treatment. For example, if the Gleason Score is greater than 8, the PSA level started to rise less than 2 years after surgery and the PSA Doubling Time is less than 10 months, there are greater chances to develop metastatic cancer. .
Still in other cases, when evaluating all the aspects of the PSA and the patient, no treatment may be the best treatment, says Dr. Samadi, Director of Mens Health at St.Francis Hospital.
Recommended Reading: Is Drinking Beer Bad For Prostate Cancer
How Will Prostate Surgery Affect My Sex Life
Experienced robotic surgeons like Dr. David Samadi dont open the endopelvic fascia during surgery, which spares the rick of damage to nerve bundles that control sexual function. The recovery of the function, however, is not immediate and you should not feel discouraged if weeks or even a few months after surgery you experience erectile dysfunction. It is not an indication of long-term damage.
One major change that you will notice in your sex life is the absence of sperm. Having no prostate, the body will not produce semen during the orgasm. The sperm cells will be simply reabsorbed by the body them. This is not harmful and you shouldnt be worried about it. Plenty of men deal with the problem with the help of medication that improves erectile dysfunction.
What Is A Urethral Sling Procedure And How Does It Help With Urinary Incontinence
In the urethral sling procedure, a synthetic mesh tape is placed around part of the urethra, moving the urethra into a new position. This is a minimally invasive procedure, which means that the surgeon only has to make a small incision in the perineum .
Your provider may recommend a urethral sling procedure if you have mild to moderate urinary incontinence after a radical prostatectomy that hasnt improved using other more conservative measures. It’s highly successful in helping men overcome incontinence, or reduce episodes of leaking urine.
Before the surgery, the provider may do some tests, including the following:
- A urodynamic study, to test how well the bladder is working.
- A 24-hour pad test .
- A cystoscopy, a test in which the doctor looks inside the bladder with an instrument called a cystoscope.
You dont have to donate any of your own blood before surgery.
Read Also: How Do I Know If I Have Prostatitis
Recurrent Prostate Cancer When Is It Happening
According to the Prostate Cancer Foundation, about 20-30% of men have PSA recurrence after five years of initial prostate cancer treatment .
As a patient, the prospect of PSA recurrence can be very worrisome. What many patients do not know is that not all modified levels of PSA after prostate cancer treatment indicate recurrent prostate cancer. Some types of levels are much more troublesome than others and treatment approaches can vary tremendously case by case. Not all changes in the PSA mean recurrent prostate cancer after robotic surgery or other forms of treatment. Elevated PSA after prostate removal may also indicate other conditions, that is why the PSA check is essential after surgery.
Gene And Protein Expression
About 20,000 protein coding genes are expressed in human cells and almost 75% of these genes are expressed in the normal prostate. About 150 of these genes are more specifically expressed in the prostate, with about 20 genes being highly prostate specific. The corresponding specific proteins are expressed in the glandular and secretory cells of the prostatic gland and have functions that are important for the characteristics of semen, including prostate-specific proteins, such as the prostate specific antigen , and the Prostatic acid phosphatase.
In the developing embryo, at the hind end lies an inpouching called the cloaca. This, over the fourth to the seventh week, divides into a urogenital sinus and the beginnings of the anal canal, with a wall forming between these two inpouchings called the urorectal septum. The urogenital sinus divides into three parts, with the middle part forming the urethra the upper part is largest and becomes the urinary bladder, and the lower part then changes depending on the biological sex of the embryo.
Recommended Reading: Gleason Score 7 Prostate Cancer Treatment Options
Life After Prostate Removal
Categories:Cancer Survivorship,Prostate Cancer,Survivorship & Side Effects
For many men with prostate cancer, prostate removal is never needed because the cancer is often slow-growing and managed with non-surgical treatments. But, if the cancer has grown beyond the prostate, the oncologist may recommend prostate removal surgery, also called a prostatectomy. If you are going to have prostate removal surgery, this information can help you in your discussion with the doctors.
Questions To Ask Your Doctor Or Nurse
You may find it helpful to keep a note of any questions you have to take to your next appointment.
- What type of surgery do you recommend for me and why?
- What type of surgery do you recommend for me? Will you try to do nerve-sparing surgery?
- How many of these operations have you done and how many do you do each year?
- Can I see the results of radical prostatectomies youve carried out?
- What pain relief will I get after the operation?
- How and when will we know whether the operation has removed all of the cancer?
- How often will my PSA level be checked?
- What is the chance of needing further treatment after surgery?
- What is the risk of having urinary problems or erection problems and what support can you offer me?
Also Check: Prostate Cancer Center Of New Jersey
Blood And Lymphatic Vessels
The prostate receives blood through the inferior vesical artery, internal pudendal artery, and middle rectal arteries. These vessels enter the prostate on its outer posterior surface where it meets the bladder, and travel forward to the apex of the prostate. Both the inferior vesical and the middle rectal arteries often arise together directly from the internal iliac arteries. On entering the bladder, the inferior vesical artery splits into a urethral branch, supplying the urethral prostate and a capsular branch, which travels around the capsule and has smaller branches which perforate into the prostate.
The veins of the prostate form a network the prostatic venous plexus, primarily around its front and outer surface. This network also receives blood from the deep dorsal vein of the penis, and is connected via branches to the vesical plexus and internal pudendal veins. Veins drain into the vesical and then internal iliac veins.
The lymphatic drainage of the prostate depends on the positioning of the area. Vessels surrounding the vas deferens, some of the vessels in the seminal vesicle, and a vessel from the posterior surface of the prostate drain into the external iliac lymph nodes. Some of the seminal vesicle vessels, prostatic vessels, and vessels from the anterior prostate drain into internal iliac lymph nodes. Vessels of the prostate itself also drain into the obturator and sacral lymph nodes.
-
Microscopic glands of the prostate
Approaches To Radical Prostatectomy Surgeons Can Use Different Approaches And Techniques Toremove The Prostate They Can Make A Large Incision To Reach The Prostate They Can Also Use Laparoscopic Orrobotic Techniques Which Are Done Through Smaller Incisions In The Pelvis Laparoscopicand Robotic Types Of Surgery Are Less Invasive Than An Open Radicalprostatectomy Men Often Have Shorter Recovery Times Less Blood Loss Lesspain And Shorter Hospital Stays With These Procedures Retropubic Radicalprostatectomy Is Done Through An Incision In The Lower Abdomen The Surgeoncan Also Remove Lymph Nodes From The Pelvis Through The Same Incision Incanada A Retropubic Radical Prostatectomy Is The Most Common Approach Toremoving The Prostate To Treat Cancer
Perineal radical prostatectomyis done through an incision in the area between the scrotum and the anus. This surgery usually doesn’t take as long to do as aretropubic radical prostatectomy, but it may lead to more problems with gettingan erection . In addition, surgeons can’t removepelvic lymph nodes through the same incision so they would have to do aseparate procedure through a small cut in the lower abdomen to remove them.
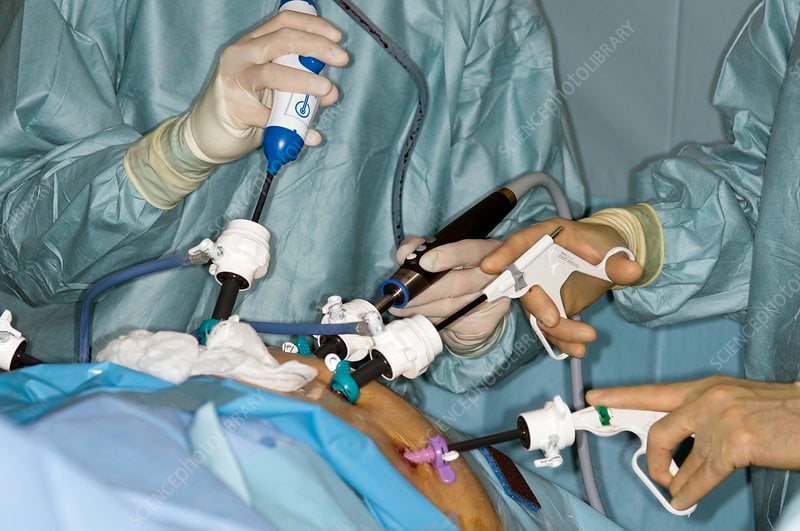
Laparoscopic radical prostatectomyuses a laparoscope and other surgical instruments passed through small cuts. A laparoscopicprostatectomy has some advantages over an open radical prostatectomy, includingless blood loss and pain, shorter hospital stays, faster recovery and less timewith a catheter.
Robotic radicalprostatectomy is a type of robotic surgery. The surgeon sits near theoperating table and uses remote controls to move robotic arms. The robotic armshave tiny video cameras and surgical instruments that remove tissue throughsmall cuts. The robotic arms can bend and turn like a human wrist. A roboticprostatectomy also has advantages over an open radical prostatectomy includingless blood loss and pain, shorter hospital stays, faster recovery and less timewith a catheter.
Don’t Miss: Can Garlic Shrink Enlarged Prostate
How Long Does Urinary Incontinence After Prostate Surgery Last
It’s impossible to say exactly how long it lasts. The chances of you having urinary problems may be influenced by your age, weight and the physical characteristics of your urethra .
However, a majority of men are eventually continent after a radical prostatectomy. In many cases, men are able to go safely without any kind of incontinence product after about three months. This is especially true of men who are healthy overall and fall into the age range of 40 to 60 years. If you are having persistent problems, its important to know that there are ways to treat urinary incontinence after prostate surgery.
During Surgery For Bph
The vast majority of BPH surgeries are performed using a transurethral technique, of which there are several types. With each, a tube-like instrument called a cystoscope or resectoscope reaches the prostate gland via the urethra.
Some transurethral techniques include:
- Transurethral resection of the prostate : An electrified wire loop is used to remove prostate tissue. This is the most common surgery used to treat BPH.
- Transurethral electrovaporization of the prostate : Electrical energy applied through an electrode is used to heat and vaporize an area of enlarged prostate tissue.
- Transurethral incision of the prostate : No prostate tissue is removed, but two deep cuts are made starting in the bladder neck . The purpose of these cuts is to widen the urethra in order to improve urine flow.
- Laser energy is used to vaporize prostate tissue.
- Laser enucleation of the prostate: A holium or thulium laser is used to remove large chunks of excess prostate tissue that is blocking urine flow.
- Prostate urethral lift: Implants are placed in the prostate to lift the prostate and keep the urethra open.
- Prostate water vapor therapy: Targeted, controlled doses of stored thermal energy in water vapor are used to decrease prostate tissue.
Recommended Reading: What Is The Test For Prostate Cancer
Risks Of The Procedure
As with any surgical procedure, certain complications can occur. Somepossible complications of both the retropubic and perineal approaches to RPmay include:
Some risks associated with surgery and anesthesia in general include:
-
Reactions to medications, such as anesthesia
-
Difficulty with breathing
-
Bleeding
-
Infection
One risk associated with the retropubic approach is the potential forrectal injury, causing fecal incontinence or urgency.
There may be other risks depending on your specific medical condition. Besure to discuss any concerns with your doctor prior to the procedure.