How Soon Can We Detect This
One of the main advantages of surgery over radiotherapy for prostate cancer is that following prostate removal, the PSA should be very low , which we can of course detect with blood tests. If metastasis occurs, because the metastatic cells originated in the prostate and therefore make PSA, the PSA level in the blood starts to rise. Once it has reached a given threshold additional or salvage treatment will be discussed.
A PSA level of more than 0.2 ng/ml defines biochemical recurrence. At this stage the cancer is still much too small to be seen on scanning. If it can be seen on a scan it is termed clinical recurrence, which generally does not occur until the PSA level is more than 0.5 ng/ml. Symptoms, such as bone pain, dont usually occur until the PSA is more than 20 ng/ml.
Prostate Cancer Survival Rates: What They Mean
As cancer diagnoses go, prostate cancer is often a less serious one. Prostate cancer is frequently slow-growing and slow to spread. For many men, prostate cancer is less serious than their other medical conditions.
For these reasons, and possibly because of earlier detection of low-grade prostate cancers, prostate cancer has one of the highest survival rates of any type of cancer. WebMD takes a look at prostate cancer survival rates and what they mean to you.
Prostate Cancer Survival By Age
Five-year survival for prostate cancer shows an unusual pattern with age: survival gradually increases from 91% in men aged 15-49 and peaks at 94% in 60-69 year olds survival falls thereafter, reaching its lowest point of 66% in 80-99 year olds patients diagnosed with prostate cancer in England during 2009-2013. The higher survival in men in their sixties is likely to be associated with higher rates of PSA testing in this age group.
Prostate Cancer , Five-Year Net Survival by Age, Men, England, 2009-2013
Read Also: Side Effects Of Prostate Cancer Drugs
What Factors Increase The Chance Of Cancer Recurrence
The likelihood of metastasis occurring increases with higher grade and stage of the cancer as the more aggressive and developed the cancer is, the higher the chance of it breaking out of the prostate. More specifically:
- High Gleason grades
- High clinical stages
- Positive surgical margins .
However, most prostate cancers are cured with surgery. As an example, using my results from operations performed on over 2,300 men with a variety of stages and grades, 96.3% of operations resulted in full cancer cure. Some combinations of minor prostate cancer had a 100% cancer cure rate, but the higher you go, the lower the full cancer cure rate.
The commonest sites of recurrence of prostate cancer following surgery are:
- the prostate bed 80% of recurrence cases
- lymph nodes 15% of cases
- bones 5% of cases.
Baus Radical Prostatectomy Audit
The British Association of Urological Surgeons now publishes the results of radical prostatectomy for surgery performed in the UK. Details of the operations performed by each surgeon and centre are given, with information about the technique used, transfusion rates, postoperative complications and length of stay for individual surgeons and units. The responsibility of entering the data, however, lies with the individual surgeons and is not always complete.
For more information and guidance on treatment for prostate cancer as well as radical prostatectomies visit Mr Neil Haldars Top Doctors profile today.
You May Like: What Does Low Grade Prostate Cancer Mean
Remission And The Chance Of Recurrence
A remission is when cancer cannot be detected in the body and there are no symptoms. This may also be called having no evidence of disease or NED.
A remission can be temporary or permanent. This uncertainty causes many people to worry that the cancer will come back. Although there are treatments to help prevent a recurrence, such as hormonal therapy and radiation therapy, it is important to talk with your doctor about the possibility of the cancer returning. There are tools your doctor can use, called nomograms, to estimate someones risk of recurrence. Understanding your risk of recurrence and the treatment options may help you feel more prepared if the cancer does return. Learn more about coping with the fear of recurrence.
In general, following surgery or radiation therapy, the PSA level in the blood usually drops. If the PSA level starts to rise again, it may be a sign that the cancer has come back. If the cancer returns after the original treatment, it is called recurrent cancer.
When this occurs, a new cycle of testing will begin again to learn as much as possible about the recurrence, including where the recurrence is located. The cancer may come back in the prostate , in the tissues or lymph nodes near the prostate , or in another part of the body, such as the bones, lungs, or liver . Sometimes the doctor cannot find a tumor even though the PSA level has increased. This is known as a PSA-only or biochemical recurrence.
You May Like: How To Fix A Swollen Prostate
Stage Iv Prostate Cancer Prognosis
Prostate cancers detected at the distant stage have an average five-year survival rate of 28 percent, which is much lower than local and regional cancers of the prostate. This average survival rate represents stage IV prostate cancers that have metastasized beyond nearby areas to lymph nodes, organs or bones in other parts of the body.
Don’t Miss: How Many Men Die Of Prostate Cancer
Differences Among Risk Groups
Men with PCa have been classified into low-, intermediate- and high-risk Groups for tumor recurrence and disease specific mortality, based on PSA level, clinical or pathological staging and GS. High-risk patients have PSA level 20ng/mL or GS 8 or clinical/pathological stage T2c . Lymph-node positive and PSM have also been reported as poor prognosis factors.
Risk Group classification predicts biochemical and clinical progression as well as PCa specific mortality and overall survival. The risk of disease progression in these groups has been validated for patients submited to RP in many studies. In patients from Mayo Clinic, BCR rates were 2.3 and 3.3-fold greater in high and intermediate-risk in comparison with low-risk patients, respectively. In those patients, mortality rates in high and intermediate-risk patients were greater than 11 and 6-fold over low-risk men .
Therefore, it is crutial to understand the role of each clinical and pathologic feature in PCa BCR and disease progression.
Early Mortality Of Prostatectomy Vs Radiotherapy As A Primary Treatment For Prostate Cancer: A Population
- Department of Radiation Oncology, University Hospital Halle , Halle , Germany
Objective: To assess the extent of early mortality and its temporal course after prostatectomy and radiotherapy in the general population.
Methods: Data from the Surveillance, Epidemiology, and End Results database and East German epidemiologic cancer registries were used for the years 20052013. Metastasized cases were excluded. Analyzing overall mortality, year-specific Cox regression models were used after adjusting for age , risk stage, and grading. To estimate temporal hazards, we computed year-specific conditional hazards for surgery and radiotherapy after propensity-score matching and applied piecewise proportional hazard models.
Results: In German and US populations, we observed higher initial 3-month mortality odds for prostatectomy approaching the null effect value not before 24-months after diagnosis. During the observational period, we observed a constant hazard ratio for the 24-month mortality in the US population comparing surgery and radiotherapy. The same was true in the German cohort . Considering low-risk cases, the adverse surgery effect appeared stronger.
There is strong evidence from two independent populations of a considerably higher early to midterm mortality after prostatectomy compared to radiotherapy extending the time of early mortality considered by previous studies up to 36-months.
You May Like: What Is The Survival Rate For Stage 3 Prostate Cancer
Multiple Imputation And Missing Data
We used multiple imputation to impute missing data taking the variables of T-stage and histopathologic grading, age, and treatment into account. Missing data were mostly confined to the grading parameter in the German data . For propensity score matched analyses and year-specific Cox regression analyses, we used PROC MI in SAS. In piecewise proportional hazard models, we applied the mice package in R. Matching results for the complete data are shown in Table S2, which indicate equal mean values and proportions between treatment groups.
Staging Spread And Survival Rates
As with all cancers, doctors use the term stage to describe the characteristics of the primary tumor itself, such as its size and how far prostate cancer has spread when it is found.
Staging systems are complicated. The staging system for most cancers, including prostate cancer, uses three different aspects of tumor growth and spread. It’s called the TNM system, for tumor, nodes, and metastasis:
- T, for tumor describes the size of the main area of prostate cancer.
- N, for nodes, describes whether prostate cancer has spread to any lymph nodes, and how many and in what locations.
- M, for metastasis, means distant spread of prostate cancer, for example, to the bones or liver.
Using the TNM system, each man’s prostate cancer can be described in detail and compared to other men’s prostate cancer. Doctors use this information for studies and to decide on treatments.
As far as survival rates for prostate cancer go, however, the staging system is pretty simple. As we’ve mentioned, in terms of survival rates, men with prostate cancer can be divided into two groups:
Show Sources
Also Check: Remedios Caseros Para Desinflamar La Prostata
The Stages Of Prostate Cancer: What You Need To Know
After a prostate cancer diagnosis, your oncologist will refer to the stage of your cancer. All cancers are categorized into four distinct stages, each of which identifies the progress of the growth of cancerous cells within clinically defined standards. These stages help doctors determine the most appropriate care for each patient based on his or her condition, and can also provide easy-to-understand context for your diagnosis. Learn more about the stages of prostate cancer, how each stage will affect your treatment plan and the survival rates for each stage, then contact Regional Cancer Care Associates to schedule a consultation.
Results Of Oncological Treatment
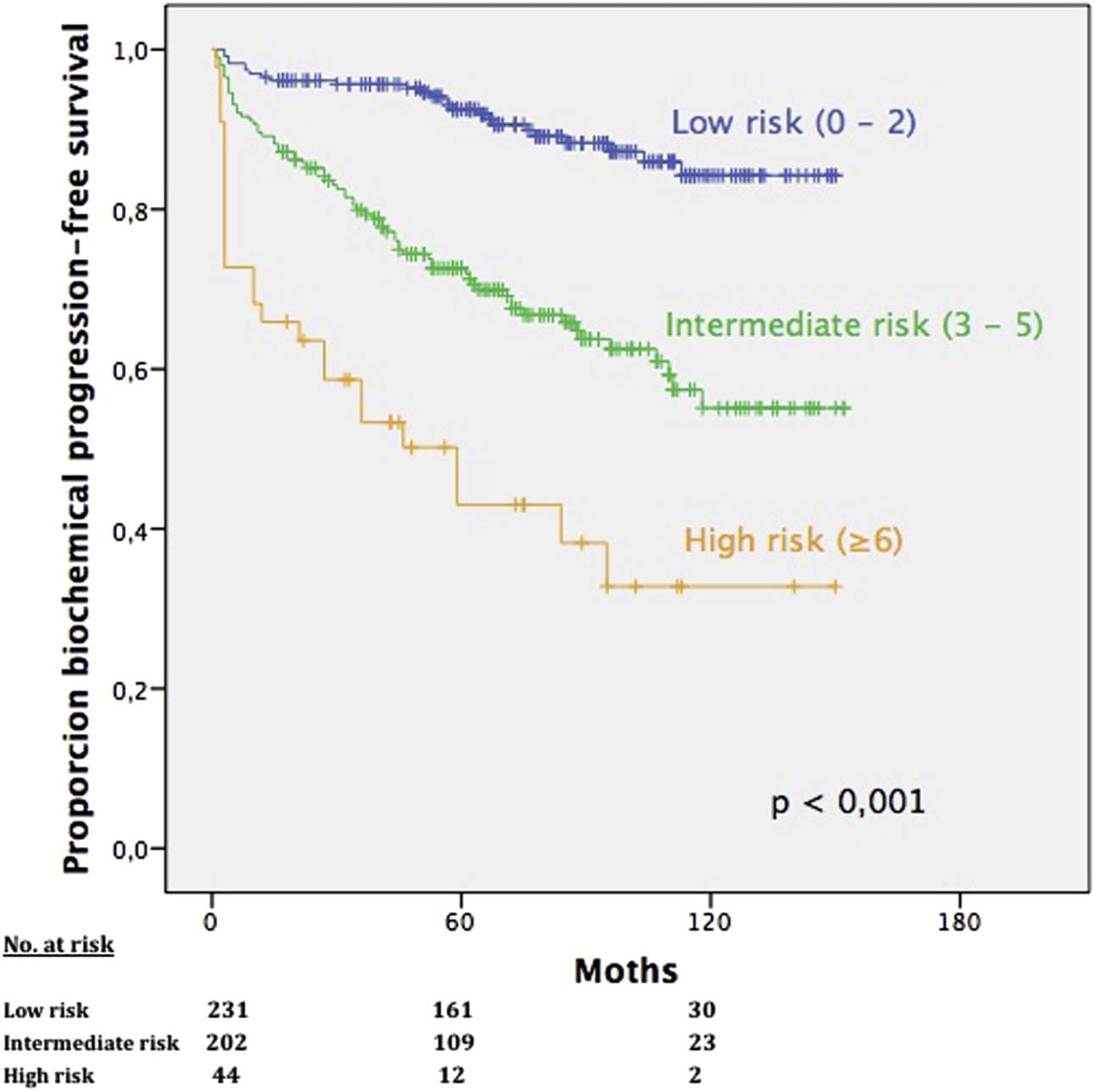
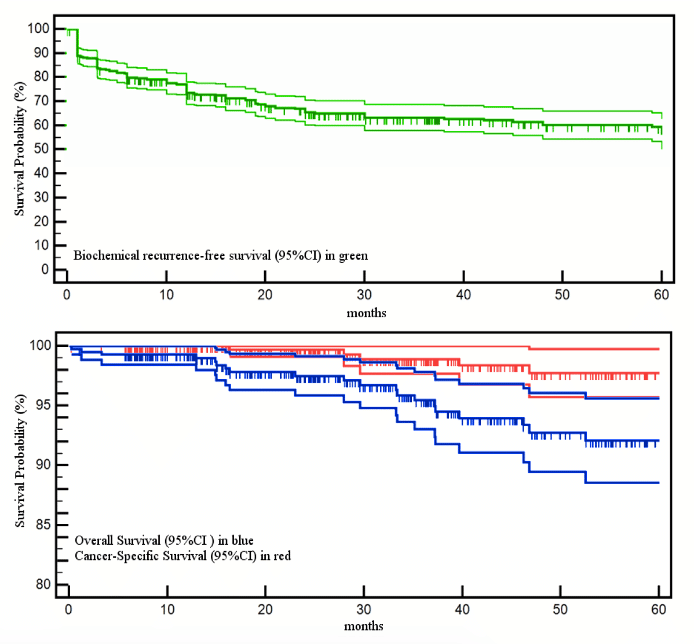
Figure 1 shows the KaplanMeier curves for carcinoma-specific survival in patients with tumor stage pT3a, pT3b, pT4, pN1 and/or preoperative PSA > 20 ng/mL and/or prostatectomy Gleason score 8.
Prostate carcinoma-specific survival after radical prostatectomy for patients with confirmed locally advanced tumors and/or confirmed lymph-node metastases and/or preoperative PSA > 20 ng/mL and or Gleason score 8 in the prostatectomy specimen. The dotted lines show the 95% confidence interval. a) Prostate carcinoma-specific survival, stratified according to pT stage. b) Prostate carcinoma-specific survival in patients with lymph-node metastases. c) Prostate carcinoma-specific survival in patients with preoperative PSA > 20 ng/mL. d) Prostate carcinoma-specific survival in patients with prostatectomy Gleason score 8.
The 10-year carcinoma-specific survival rates were:
- 98% for patients with stage pT3a
- 87% for patients with stage pT3b
- 77% for patients with stage pT4
- 81% for patients with confirmed lymph-node metastases
Among patients with a high-risk tumor constellation, the 10-year carcinoma-specific and 10-year overall survival rates were 93% and 85% respectively for those with a preoperative PSA level > 20 ng/mL and 70% and 58% for those with a prostatectomy Gleason score 8 . The corresponding 10-year biochemically recurrence-free survival rates were 32% and 25%.
Recommended Reading: Natural Remedies For Prostate Swelling
Psa Levels After Treatment
A continuous rise in your PSA level can be the first sign that your cancer has come back. This should be picked up by your regular PSA tests.
The exact change in PSA level that suggests your cancer has come back will depend on which treatment you had. Speak to your doctor or nurse about your own situation.
Your PSA level should drop so low that its not possible to detect it at six to eight weeks after surgery. This is because the prostate, which produces PSA, has been removed. A rise in your PSA level may suggest that you still have some prostate cancer cells.
After radiotherapy or brachytherapy, your PSA should drop to its lowest level after 18 months to two years. Your PSA level wont fall to zero as your healthy prostate cells will continue to produce some PSA.
Your PSA level may actually rise after radiotherapy treatment, and then fall again. This is called PSA bounce. It could happen up to three years after treatment. It is normal, and doesnt mean that the cancer has come back.
If your PSA level rises by 2 ng/ml or more above its lowest level, this could be a sign that your cancer has come back. Your doctor will continue to check your PSA level and will talk to you about further tests and treatment options.
Early Mortality And Year Of Diagnosis
For year-specific survival analyses, we used Cox regression models estimating the average of the hazard ratio during the time of 24-months for the years of diagnosis between 2005 and 2013 according to the time of diagnosis. Models were adjusted for age, age squared, grading differentiation between a Gleason score below and above 6, and risk , respectively, allowing for the interaction between year of diagnosis and each main effect covariate, and thus for a temporal variation of potential confounders.
Recommended Reading: Does Cialis Help With Enlarged Prostate
Prostate Cancer Survival Rates Are Favorable Overall
Thinking about survival rates for prostate cancer takes a little mental stretching. Keep in mind that most men are around 70 when diagnosed with prostate cancer. Over, say, five years, many of these men will die from other medical problems unrelated to prostate cancer.
To determine the prostate cancer survival rate, these men are subtracted out of the calculations. Counting only the men who are left provides what’s called the relative survival rate for prostate cancer.
Taking that into consideration, the relative survival rates for most kinds of prostate cancer are actually pretty good. Remember, we’re not counting men with prostate cancer who die of other causes:
- 92% of all prostate cancers are found when they are in the early stage, called local or regional. Almost 100% of men who have local or regional prostate cancer will survive more than five years after diagnosis.
- Fewer men have more advanced prostate cancer at the time of diagnosis. Once prostate cancer has spread beyond the prostate, survival rates fall. For men with distant spread of prostate cancer, about one-third will survive for five years after diagnosis.
Many men with prostate cancer actually will live much longer than five years after diagnosis. What about longer-term survival rates? According to the American Society of Clinical Oncology, for men with local or regional prostate cancer:
- the relative 10-year survival rate is 98%
- the relative 15-year survival rate is 95%
Advancing Prostate Cancer Care
At Memorial Sloan Kettering, we tailor multimodal approaches to the individual features of each patients cancer. Radical prostatectomy is a complex procedure that requires a high level of technical precision. We provide state-of-the-art surgical techniques, including minimally invasive robotic and nerve-sparing surgery. Over the past few decades, we have dramatically reduced surgical complications by incorporating imaging test results in surgical plans to ensure the avoidance of other structures and the minimization of the risk of incontinence and erectile dysfunction. Our multidisciplinary prostate cancer team includes radiation oncologists who provide the latest radiotherapy approaches, including image-guided and intensity-modulated radiation therapy, stereotactic radiosurgery, proton therapy, and brachytherapy.
The field of prostate cancer care is evolving rapidly. We continue to explore new ways to improve outcomes and safety and effectiveness through clinical trials, in which we are testing new drugs and drug combinations, surgery and radiation therapy techniques, diagnostic approaches, and strategies for improving quality of life for men undergoing treatment for prostate cancer.
Disclosure: Peter Scardino sits on a clinical advisory board for OPKO Health outside the submitted study he also holds a patent issued by OPKO.
Read Also: Super Beta Prostate Supplement Side Effects
Where Do These Numbers Come From
The American Cancer Society relies on information from the SEER database, maintained by the National Cancer Institute , to provide survival statistics for different types of cancer.
The SEER database tracks 5-year relative survival rates for prostate cancer in the United States, based on how far the cancer has spread. The SEER database, however, does not group cancers by AJCC TNM stages . Instead it groups cancers into localized, regional, and distant stages.
- Localized: There is no sign that the cancer has spread outside the prostate.
- Regional: The cancer has spread outside the prostate to nearby structures or lymph nodes.
- Distant: The cancer has spread to parts of the body farther from the prostate, such as the lungs, liver, or bones.
Stage 2 Prostate Cancer Survival Rate
Stage 2 prostate cancer occurs when the tumor starts spreading within the limits of the prostate gland. Stage 2 can follow three different scenarios.
- Stage IIA: PSA reading nears 20ng/mL, the Gleason score remains at 6. The location of the tumor is in one-half of the prostate gland
- Stage IIB: PSA reading nears 20ng/mL, the Gleason score reaches 7. The location of the tumor is in one-half of the prostate gland or on both of its sides
- Stage IIC: PSA reading nears 20ng/mL, the Gleason score is at either 7 or 8. The location of the tumor is in one-half of the prostate gland or on both of its sides.
Stage 2 prostate cancer survival rate for the first 5 years records a slight decrease from 99% to 97.5%. This means that around 97 out of 100 men diagnosed with prostate cancer are going to survive their disease for at least 5 years.
The treatment plan for stage 2 prostate cancer takes into consideration the removal of the prostate gland as well as the nearby lymph nodes. Hormone therapy is discussed with the patient but only when administered along with radiation therapy. Brachytherapy is also anticipated. Active surveillance remains a viable treatment plan for stage IIA and IIB prostate cancer cases.
Recommended Reading: Prostate Cancer Family History Risk