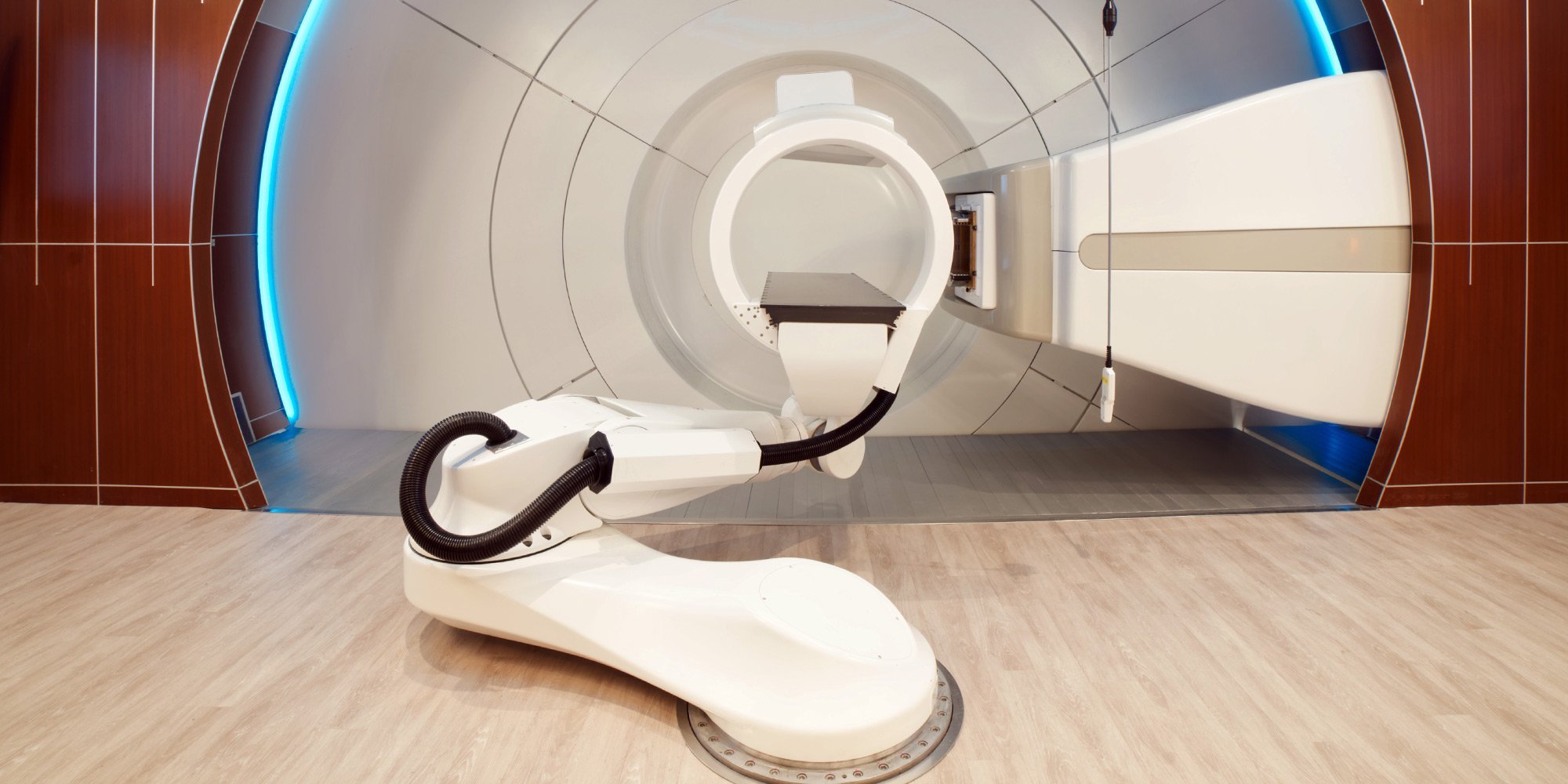
How Proton Therapy Works
A machine called a synchrotron or cyclotron speeds up protons. The high speed of the protons creates high energy. This energy makes the protons travel to the desired depth in the body. The protons then give the targeted radiation dose in the tumor.
With proton therapy, there is less radiation dose outside of the tumor. In regular radiation therapy, x-rays continue to give radiation doses as they leave the person’s body. This means that radiation damages nearby healthy tissues, possibly causing side effects.
The Success Rate Of Prostate Surgery
Survival rates can tell you how many people with the same type and stage of cancer are still alive 5 years after being diagnosed. For example, if you have stage 3 colon cancer, there is a 66% chance that 5 years later, you will be alive. But the rates cannot tell you how long you will live. However, they may help give you an idea of how likely your treatment will be successful.
Survival rates are estimates. They are based on data from many people who have had cancer before. These numbers might be confusing because they dont tell you what will happen, but they can help doctors decide treatments. Talk with your doctor to see if these statistics apply to you because they know about your situation.
A relative survival rate tells how likely a person is to survive a particular type of cancer. I.e., if the 5-year close survival rate for prostate cancer is 90%, it means that men who have this type of cancer are about 90% as likely as other men to live a minimum of 5 years after being diagnosed with the disease.
New Study Compares Long
- By Charlie Schmidt, Editor, Harvard Medical School Annual Report on Prostate Diseases
Prostate cancer therapies are improving over time. But how do the long-term side effects from the various options available today compare? Results from a newly published study are providing some valuable insights.
Investigators at Vanderbilt University and the University of Texas MD Anderson Cancer Center spent five years tracking the sexual, bowel, urinary, and hormonal status of nearly 2,000 men after they had been treated for prostate cancer, or monitored with active surveillance . Cancers in all the men were still confined to the prostate when diagnosed.
Dr. Karen Hoffman, a radiation oncologist at MD Anderson and the studys first author, said the intent was to provide information that could help men choose from among the various therapeutic options. Surgical and radiation techniques have changed significantly in the last few decades, and at the same time, active surveillance has become an increasingly acceptable strategy, she said. We wanted to understand the adverse events associated with contemporary approaches from the patients perspective.
Roughly two-thirds of the men enrolled in the study had favorable risk cancer, which is nonaggressive and slow-growing. A quarter of these men chose active surveillance, and the rest were treated with one of three different methods:
Also Check: Water Vapor Treatment For Prostate
Read Also: Best Cancer Center For Prostate Cancer
Benefits Of Proton Therapy
Since proton therapy precisely targets even the most difficult to treat and reach tumors, it allows for higher doses of radiation to be delivered to the prostate with fewer side effects. Unlike treatment with conventional X-ray therapy , treatment with proton therapy can be achieved using just two beams. Some of the benefits of proton therapy include:
- Precise, accurate delivery of even high radiation doses to kill cancerous cells in the prostate
- Minimal impact to surrounding, healthy tissues and vital organs, such as the bladder and rectum
- Less invasive treatment is painless and requires no downtime
- Provided in a comfortable, outpatient setting with free parking
Proton Therapy Advantages And Disadvantages
Proton radiation may represent an incremental improvement over IMRT due to the reduced exposure of surrounding normal body tissues to radiation. Therefore, in the situations outlined above where IMRT would normally be considered, men may prefer to choose proton radiation over IMRT. The purported advantages of proton radiation over IMRT remain theoretical and clinically unproven. No head to head studies comparing the IMRT and proton radiation exist.
Disadvantages associated with proton radiation are related to its high cost and the fact that not all insurance programs cover proton radiation. In addition, there are relatively few centers doing proton radiation, so geographic inconvenience can be a major factor considering that numerous visits are required over a 5 to 9-week period.
Men considering treatment for prostate cancer need to do their homework. Side effects from radiation can be irreversible. The selection of optimal radiation varies with patient circumstances. Many factors need to be considered when radiation is contemplated.
Also Check: Best Foods For Prostate Health
Recommended Reading: Rf Therapy For Enlarged Prostate
When Is Brachytherapy Alone The Right Choice
For a patient with disease that is confined to the prostate and not too aggressive, brachytherapy alone is a good option. With the use of sophisticated real-time computer-based planning, we can use brachytherapy to deliver radiation in an extraordinarily precise way, with minimal exposure to the surrounding normal tissues. It is also convenient for the patient as it is done in an outpatient setting and most people are able to get back to work the next day.
But brachytherapy is not right for everyone. For some patients with less-aggressive disease, a watch-and-wait approach would also be very reasonable. At MSK, our philosophy is that when the disease is caught very early meaning a low PSA level, or nonaggressive disease as reflected by a Gleason score of 6 with evidence of cancer in only a few of the biopsy samples and no evidence from the MRI of a significant amount of disease then it would be very appropriate to do active surveillance and hold off on treatment.
How Can I Choose From Among The Options
In addition to talking with family and friends, you will need a team of physicians to help advise you. You should meet with everyone involved in your treatment planning before choosing a treatment, including:
- your primary care doctor
- a urologist to discuss surgery
- a radiation oncologist to discuss radiation therapy
- a medical oncologist to discuss hormone suppression, if your cancer is more advanced
After you meet with these doctors, you can make an informed decision regarding your treatment options. You may have an early-stage or moderately advanced cancer with no evidence of spread to other organs . If so, your two major treatment options are active surveillance , surgery or radiation therapy .
You may have advanced cancer and require hormonal suppression therapy or chemotherapy. If so, you will need a medical oncologist to administer these drugs. Doctors use hormone-ablation therapy to treat advanced prostate cancer. It suppresses androgen because these hormones stimulate most prostate cancer growth. Your internist, urologist, radiation oncologist or medical oncologist may administer the treatment. Depending on the stage of the cancer, your doctor may use hormone suppression therapy and radiation therapy to help control your disease. You may receive hormone suppression therapy for as little as four to six months, or for as long as two to three years.
Also Check: Radiation Treatment For Prostate Cancer After Prostatectomy
Are There Side Effects Of The Combination Approach
There is a slightly higher chance that patients who receive the combined therapy will have rectal irritation or urinary side effects, both of which are common with any radiation treatment given to the prostate. But at MSK, we routinely use sophisticated planning techniques that help us reduce the dose given to normal tissues such as the rectum, bladder, and urethra, lessening the chances of side effects and complications.
In addition, at MSK, we routinely use a rectal spacer gel, which we inject between the prostate and the rectum while the patient is under mild anesthesia, to create a buffer between these two tissues. By creating this space, we can further reduce the dose of radiation that the rectum is exposed to. This leads to fewer side effects for the patient. The rectal spacer gel is biodegradable and after a few months dissolves on its own within the body, causing no harm or long-term effects.
Potential Benefits Of Pt And Reported Clinical Outcomes Of Prostate Treatments
Given the different beam characteristics of protons and photons, a modulated proton beam confines dose deposition to the target region, with a rapid depth- and lateral-dose fall-off favoring normal tissue sparing and target dose escalation. Several dosevolume comparison studies showed that both passive scattering and pencil beam scanning PT reduced the mean dose and percentage of volume receiving low dose in the rectum and bladder compared with IMRT. In the prostate, PT maintained dose coverage, demonstrating superior dose conformity over IMRT. In most circumstances, a simple bilateral proton beam is employed for localized prostate cancer. Other arrangements, such as anteriorposterior or anterioroblique beams may be used in patients with a hip prosthesis or previously irradiated hip . Nevertheless, PT has consistently been shown to have a smaller irradiated volume of normal tissue and lower integral non-target dose , as illustrated in Figure 1. A systematic review showed that the risk of radiation-induced second primary cancer appears to be small , but does increase over time . As prostate cancer survival improves, the risk of radiation-induced second malignancies becomes more relevant .
Integral dose comparison of volumetric modulated RapidArc therapy -full rotation and photon therapy -bilateral in prostate treatment plans. The most significant differences were in the 10% and 30% isodose distributions of the 78-Gy prescription.
Recommended Reading: Cancer De Prostata Con Metastasis Osea
Who Is A Good Candidate
In most cases, you will be a good candidate for proton therapy if you were initially offered radiotherapy as an option. Patients who receive radiotherapy usually have no problems being a candidate for proton treatment. They are usually patients in an early stage or those with localized prostate cancer. It is also useful to keep advanced cancer under control for as long as possible and treat recurrent prostate cancer cases.
However, some patients may not benefit from proton therapy if they have one of these problems :
- In patients with hip replacements, because proton beams often cant reach beyond the prosthesis. In some proton therapy centers, these patients can still get a session when a hip replacement is limited to one side. But bilateral replacement makes it impossible to treat the patient with proton beam therapy.
- In patients with advanced prostate cancer in which treating the pelvic lymph nodes is fundamental. Since proton beam radiation is less likely to reach other tissues than the prostate, it is not applicable when treating surrounding lymph nodes.
- In overweight patients, because the proton beam can only go through a determined depth. This depth depends on the beams energy, and some centers may have a higher energy device that solves the problem.
Types Of Prostate Cancer Treated At The New York Proton Center
The New York Proton Center treats the following prostate cancers and genitourinary cancers with proton therapy.
Localized prostate cancer, which includes stage 1, stage 2, and stage 3 cancer, that has not grown into nearby tissues or more distant body parts. There are three types:
- Very-low-risk and low-risk prostate cancer, each of which are unlikely to grow or spread for a long time, if at all.
- Intermediate-risk prostate cancer, which may grow or spread in a few years.
- High-risk prostate, which has the highest likelihood of spreading and, even after treatment, recurring.
Prostate cancer will sometimes grow quickly and spread to lymph nodes, pea-sized pieces of tissue that filter a waste product called lymph. When this happens, a larger area needs to be targeted for treatment that includes the prostate gland and the lymph nodes. Proton therapy is particularly beneficial when treating large areas in the pelvis.
Data suggest that men who have undergone prostatectomy for prostate cancer may benefit from follow-up treatment with proton therapy, depending on several factors:
- Gleason score
- Seminal vesicle and lymph nodes involvement
- PSA levels
Bladder cancers have a high correlation to prostate cancer. The types are named for the cells they affect, usually in the bladder wall.
Kidney cancer patients are at increased risk of prostate cancer.
Proton therapy can treat these recurrent tumors more safely than other methods, giving patients a better chance for a cure.
You May Like: Hdr Brachytherapy Prostate Cancer Side Effects
Proton Therapy Fact Sheet
About Us
The National Association for Proton Therapy is a non-profit organization founded to educate and increase public awareness about the clinical benefits of proton beam therapy. Founded in 1990, the NAPT advocates to ensure patient choice and access to affordable proton therapy and to encourage cooperative research and innovation to advance the appropriate and cost-effective utilization of proton therapy.
Quick Links
External Beam Radiation Therapy: How It Works
EBRT refers to the external delivery of any type of radiation, and can use several different types of energy including photons, electrons, and heavy particles . Additionally, there has been an evolution in the methods to deliver this energy , progressing from two-dimensional radiation therapy to three-dimensional conformal radiation therapy , and, more recently, intensity-modulated radiation therapy .
Dose distribution curves of photon and proton beams. The spread-out Bragg peak is demonstrated here to cover the entire target with the maximal dosage.
Schematic of multileaf collimator. Individually positioned tungsten leaflets conform the shape of the beam to the target as used in three-dimensional conformal radiation therapy.
Advances in image guidance such as on-board imaging units have helped to deliver the radiation more accurately to the prostate. These have dramatically decreased the uncertainty in target localization and improved the accuracy of radiotherapy to the prostate. However, despite all of these advances, the physical parameters of a photon beam will always include both entrance and exit doses and, ultimately, a significant volume of normal tissue receiving low to moderate doses.
You May Like: Benign Prostatic Hyperplasia Is Commonly Associated With
How Effective Is Modern Radiation Treatment Of Prostate Cancer
Thanks to improvements in technology and daily imaging, radiation therapy can deliver a higher radiation dose directly to the tumor while sparing surrounding healthy tissue. Doctors use different imaging techniques to see the prostate and surrounding tissues in three dimensions. This allows the doctor to tailor the radiation more precisely to the individual patient’s unique needs. Treatment planning allows them to estimate and minimize radiation exposure to the rectum, small bowel, bladder, and hips. This helps reduce the risk of side effects and complications. The goal is to safely provide a high dose of radiation, which improves the chance of cure. For similar stage and prostate cancer types, radiation therapy is as effective as surgery.
Questions To Ask Your Doctor Radiographer Or Nurse
- Will I have a planning session at a different time to the treatment, or immediately before?
- Will I have external beam radiotherapy or hormone therapy as well?
- What side effects might I get?
- How will we know if the treatment has worked?
- What should my PSA level be after treatment and how often will you test it?
- If my PSA continues to rise, what other treatments are available?
Also Check: How Do I Know If I Have Prostate Problems
What Are The Results Of Using Proton Therapy In Patients
For patients facing prostate cancer, treatments and side effects present unique challenges in choosing a therapy. Proton radiation for prostate cancer treats the disease with successful outcomes and a low risk of side effects.
For thousands with cancer of the prostate, proton therapy has offered an effective, virtually painless option for prostate cancer treatment. Since the University of Florida Health Proton Therapy Institute opened in 2006, thousands have undergone proton therapy for prostate cancer, and prostate cancer patients at the UF Health Proton Therapy Institute enjoy a close-knit community of fellow patients, caregivers and spouses. Today, prostate cancer is one of many types of cancer treated at the Institute.
Survivor Spotlight
If I Choose Radiation Therapy Will Surgical Treatment Still Be An Option
Your doctor may use radiation therapy as your primary treatment. It is important to note that the cure rates for surgery and radiation are similar. Therefore, you have the same risk of cancer recurring if surgery is performed.
If it is not successful, your doctor will likely not consider surgery or repeat radiation therapy due to the risk of serious complications. If your doctor recommends surgery after radiation or additional radiation, the doctor performing the re-treatment or surgery should have a significant level of experience. There are experimental clinical studies being evaluated for use of very localized re-irradiation for this group of patients. Some patients for whom radiation is not effective are treated with systemic therapy or closely monitored. Additional treatment will depend on the PSA level and rate of rise of the PSA.
Read Also: Is Keytruda Approved For Prostate Cancer
Ideas For Future Studies Of Proton Therapy
Despite the studys limitations, these intriguing findings raise questions that should inform future prospective phase 3 trials, Dr. Buchsbaum said, although there are barriers to large studies of proton therapy.
For instance, it is particularly encouraging that proton therapy appeared to be safer in a group of older and sicker patients who typically experience more side effects, Dr. Baumann noted.
Dr. Buchsbaum agreed that proton therapy may be especially helpful for older and sicker patients, but he noted that ongoing phase 3 trials were not designed to analyze this group of patients.
And because proton therapy may cause fewer side effects, future trials could also explore whether combining proton therapy with chemotherapy might be more tolerable for patients, the authors wrote.
For example, both chemotherapy and traditional radiation for lung cancer can irritate the esophagus, making it painful and difficult for patients to eat. But proton therapy might limit damage to the esophagus, making it easier for a patient to tolerate the combination, Dr. Baumann explained.
Future studies could also explore whether combining proton therapy with higher doses of chemotherapy might increase cures without causing more side effects, he added.
Dr. Buchsbaum agreed, saying that it would be worthwhile to explore this possibility. Just asking the question: Is more effective? might not be giving it a fair opportunity to demonstrate its benefit to society, he said.