Stages Of Prostate Cancer
In order to determine the stage of a patients prostate cancer, most doctors start by using the TNM staging system, which helps describe different aspects of the cancers growth.
- T the T category measures the size and extent of the Tumor
- N the N category measures whether and how far the cancer has spread to the Lymph Nodes
- M the M category whether the cancer has spread to other organs in the body (a process called Metastasis
The score for each of these categories is determined based on a pre-determined set of criteria. Your doctor cannot feel or see the tumor with a score of T1. A score of T3 means that the tumor has begun to grow outside of the prostate.
After calculating the TNM categories, doctors will combine the TNM score with the patients Gleason score and PSA levels assigning of a specific stage to the patients cancer.
Prostate cancer prognosis and survival rates can help give patients an idea of their chances of surviving the disease based on the stage and time of diagnosis. While some patients may find this information helpful, others may not want to know.
Seminal Vesicle Invasion: What Is The Best Adjuvant Treatment After Radical Prostatectomy
Cyrille Bastide
Departments of Urology
Cyrille Bastide
Departments of Urology
Study Type Therapy
Level of Evidence2b
Whats known on the subject? and What does the study add?
Seminal vesicle invasion in prostate cancer has a poor prognosis. Nowadays, there is no consensus about the best adjuvant treatment after radical prostatectomy when seminal vesicle invasion is observed in the specimen.
To our knowledge, this is the first comparative study between different adjuvant treatments after radical prostatectomy when seminal vesicle invasion is observed in the specimen.
Cysts In Other Organs
Seminal vesicles, pancreas, and arachnoid membrane cysts are present in 40% , 5%, and 8% of patients, respectively.68â73 Seminal vesicle cysts rarely result in infertility.74 Defective sperm motility is another cause of male infertility in ADPKD.75 Pancreatic cysts are almost always asymptomatic, with very rare occurrences of recurrent pancreatitis and possibly chance associations of intraductal papillary mucinous tumor or carcinoma reported in ADPKD.76â78 Arachnoid membrane cysts are asymptomatic, but may increase the risk for subdural hematomas.70,79 Spinal meningeal diverticula may occur with increased frequency and rarely present with intracranial hypotension due to cerebrospinal fluid leak.80 Ovarian cysts are not associated with ADPKD.81,82
Juan Andrés RamÃrez-González, Andrea Sansone, in, 2022
Also Check: Prostate Cancer Stage 2b Prognosis
Survivability For Prostate Cancer According To Stage
Relative survival looks at a persons chances of surviving after diagnosis compared to a healthy person from the general population who shares similar characteristics, such as age, sex, and race.
For prostate cancer, relative survival depends on the stage of the disease . It is important to note that this prognostic grouping, also established by the UICC, is more accurate than stage grouping in assessing a survival prognostic.
Perineural Invasion And Seminal Vesicle Involvement Predict Pelvic Lymph Node Metastasis In Men With Localized Carcinoma Of The Prostate
Stone NN, Stock RG, Parikh D, et al.
J Urol. 1998 160:17221726 .
In an effort to evaluate the ability of the presence of biopsy PNI to predict a subsequent finding of lymphatic or seminal vesicle involvement by prostate cancer, Stone and associates evaluated 212 men who presented with clinically localized prostate cancer and underwent staging pelvic lymph node dissection. Using univariate and multivariate analyses, the presence of biopsy PNI was correlated with the likelihood of metastatic prostate cancer found on pelvic lymphadenectomy. Stone and colleagues found that biopsy PNI was a better predictor of lymph node metastasis than serum prostate-specific antigen , biopsy Gleason score, or clinical stage. The authors concluded that men with biopsy PNI seeking definitive therapy for clinically localized prostate cancer should be counseled for staging pelvic lymph node dissection before definitive therapy. The potential role of biopsy PNI in predicting an increased likelihood of seminal vesicle invasion or lymphatic metastasis warrants further research. Additional support of the predictive power of PNI for lymphatic metastasis could strengthen the argument for staging lymph node dissection in the large number men with this biopsy finding who choose to undergo brachytherapy or external beam radiotherapy for clinically localized prostate cancer.
You May Like: Prostate Cancer In Young Men
New Diagnosis: Where Do I Start
You are not alone. The good news is that most prostate cancers are slow-growing and that with early detection and treatment, it can be cured. Increasing your knowledge by reviewing sections such as Coping with cancer, Choosing your treatment as well as other areas of the web site helps relieve the stress and helps make decisions clearer.
Over the last 12 months, approximately 4,600 Quebecers were diagnosed with prostate cancer. This represents an average of 12 men per day. You are definitely not alone in your fight against prostate cancer. The good news is that we know most prostate cancers are slow-growing, which means that with early detection and treatment, it can even be cured.
Once diagnosed, men will go through understandable and normal reactions, such as fear, denial, anger, helplessness and feeling of loss of control over their life. Once reality sets in, a constructive way to deal with the disease is to learn as much as you can about it. Increasing your knowledge about prostate cancer helps relieve the natural fear of the unknown, and makes the decision-making process easier.
Frequently Asked Questions
Click here for the full list of prostate cancer-related FAQs.
Questions about survival
Talk to your doctor about your prognosis. A prognosis depends on many factors, including:
- your age
- certain characteristics of the cancer
- the treatments chosen
- how the cancer responds to treatment
We are here for you
What Does It Mean If My Biopsy Report Mentions The Word Core
The most common type of prostate biopsy is a core needle biopsy. For this procedure, the doctor inserts a thin, hollow needle into the prostate gland. When the needle is pulled out it removes a small cylinder of prostate tissue called a core. This is often repeated several times to sample different areas of the prostate.
Your pathology report will list each core separately by a number assigned to it by the pathologist, with each core having its own diagnosis. If cancer or some other problem is found, it is often not in every core, so you need to look at the diagnoses for all of the cores to know what is going on with you.
Read Also: Prostate Cancer Active Surveillance Diet
Seminal Vesicle Invasion Predicts Decreased Survival In Bladder Cancer
1. Concomitant seminal vesicle invasion in patients with urothelial carcinoma of the bladder and prostatic stromal infiltration was associated with decreased cancer-specific and overall survival rates.
2. Incorporation of cSVI into multivariate analysis increased accuracy in predicting mortality events.
Evidence Rating Level: 2
Relevant Reading: Radical Cystectomy for Urothelial Carcinoma of the Bladder Without Neoadjuvant or Adjuvant Therapy: Long-Term Results in 1100 Patients
Understanding Your Prostate Pathology Report
At least initially, the pathology report is one of the most important factors in the management of your prostate health, especially if you have been diagnosed with cancer. For example, it can provide valuable information about the location and extent of the cancer, thus helping your physician decide whether to recommend active surveillance, hormone treatment, radiation therapy, or surgery.
With that in mind, you might think that preparing and reading a pathology report would be straightforward but unfortunately the opposite is true. Pathology reports are not prepared uniformly . In fact, they can vary considerably even within a single institution. They may not be labeled thoroughly or contain enough specifics for you and your doctor to make a good treatment decision.
In this article you will learn what your pathology report should include and how to make sense of the information it contains. Other articles on this site explain when to about the pathology report and why it is sometimes necessary to have a repeat biopsy, as well as what questions to ask to obtain the information you need to decide which treatment is best for you.
You May Like: What Happens When A Man Has Prostate Cancer
What Does It Mean If My Biopsy Mentions That There Is Perineural Invasion
Perineural invasion means that cancer cells were seen surrounding or tracking along a nerve fiber within the prostate. When this is found on a biopsy, it means that there is a higher chance that the cancer has spread outside the prostate. Still, perineural invasion doesnt mean that the cancer has spread, and other factors, such as the Gleason score and amount of cancer in the cores, are more important. In some cases, finding perineural invasion may affect treatment, so if your report mentions perineural invasion, you should discuss it with your doctor.
Perineural Invasion Associated With Increased Cancer
Beard. IJROBP 2006 66:403
The significance of PNI with respect to prognosis after surgery has been inconsistently demonstrated, with some investigators showing a clear risk of upstaging, upgrading, or adverse outcomes in their PNI+ patients, and others showing no effect whatsoever. There is less information on the association between outcomes after RT and PNI, but theavailable data suggest that PNI is associated with unfavorable outcomes after RT. Previously, an unfavorable outcome was defined as freedom from PSA failure. To the best of our knowledge, this is the first report demonstrating a survival decrement in the PNI+ patient population. However, the results must be viewed as preliminary, given the small number of events, relatively short follow-up, and retrospective nature of the analysis.
Purpose: To identify an association between perineural invasion and cancer-specific survival in patients with prostate cancer after standard-dose external beam radiation therapy .
Results: At a median follow-up of 4.5 years, 84 patients have died, 15 of 84 from prostate cancer. PNI was the only significant predictor of prostate cancer-specific mortality after RT . The estimated prostate cancerspecific mortality was 14% at 8 years for PNI+ patients vs. 5% for PNI patients .
Don’t Miss: Prostate Cancer How Long To Live
Metastasis And Contiguous Spread
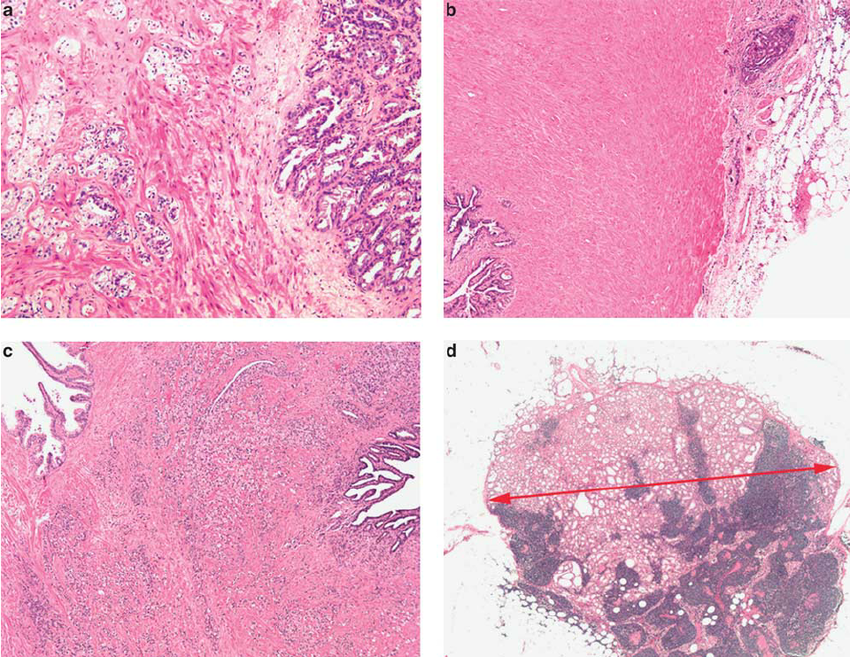
Seminal vesicle involvement by prostatic adenocarcinoma is common, observed in about 12% of contemporary radical prostatectomy specimens from patients with cancer clinically confined to the prostate . There are three patterns of seminal vesicle invasion: direct spread along the ejaculatory duct complex into the seminal vesicles prostatic capsular perforation followed by extension into the periprostatic soft tissues and spread into the seminal vesicles and isolated deposits of cancer in the seminal vesicles .171-175 Intraepithelial spread most likely results from direct invasion of carcinoma from the muscular wall of seminal vesicles rather than extension from the ejaculatory duct system in the invaginated extraprostatic space.176 Endorectal coil MRI is accurate in detecting seminal vesicle invasion according to radical prostatectomy correlation studies, with loss of architectural contour as a dominant feature.177 Bilateral invasion portends a worse prognosis than does unilateral invasion.178
Rectal adenocarcinoma occasionally invades the seminal vesicles and prostate, and may cause diagnostic difficulty.184 Metastases to the seminal vesicles and retrovesicular space from other organs are rare, including renal cell carcinoma, seminoma, malignant thymoma, and melanoma.185-189
David G. Bostwick, in, 2008
Perineural Invasion In Prostate Needle Biopsy Specimens: Correlation With Extraprostatic Extension At Resection
Vargas SO, Jiroutek M, Welch WR, et al.
Am J Clin Pathol. 1999 111:223228 .
Positing that PNI extensive enough to be sampled on needle biopsy may signal an increased risk of extraprostatic extension of cancer, Vargas and associates evaluated the preoperative needle biopsy specimens and corresponding prostates of 340 men who underwent radical prostatectomy between 1995 and 1997 in an attempt to correlate biopsy PNI with extraprostatic tumor extension. PNI was present in 16.7% of these biopsy specimens and correlated with higher Gleason scores and an increased incidence of extraprostatic tumor extension after radical prostatectomy. In this cohort of patients, all presenting after the widespread availability of PSA testing, biopsy PNI had a sensitivity of 32% and specificity of 88% for predicting extraprostatic tumor extension. Biopsy PNI had a positive predictive value of 42% for extraprostatic tumor extension. Using multivariate logistic regression, Vargas and associates found biopsy PNI to independently predict extraprostatic tumor extension. Despite this, when serum PSA was included in the multivariate analysis, PNI provided no additional ability to predict extraprostatic extension on final pathologic analysis.
Read Also: Do Prostate Supplements Really Work
What Are Grade Groups
Grade Groups are a new way to grade prostate cancer to address some of the issues with the Gleason grading system.
As noted above, currently in practice the lowest Gleason score that is given is a 6, despite the Gleason grades ranging in theory from 2 to 10. This understandably leads some patients to think that their cancer on biopsy is in the middle of the grade scale. This can compound their worry about their diagnosis and make them more likely to feel that they need to be treated right away.
Another problem with the Gleason grading system is that the Gleason scores are often divided into only 3 groups . This is not accurate, since Gleason score 7 is made up of two grades , with the latter having a much worse prognosis. Similarly, Gleason scores of 9 or 10 have a worse prognosis than Gleason score 8.
To account for these differences, the Grade Groups range from 1 to 5 :
- Grade Group 1 = Gleason 6
- Grade Group 2 = Gleason 3+4=7
- Grade Group 3 = Gleason 4+3=7
- Grade Group 4 = Gleason 8
- Grade Group 5 = Gleason 9-10
Although eventually the Grade Group system may replace the Gleason system, the two systems are currently reported side-by-side.
What Are Prostate Cancer Survival Rates By Stage
Staging evaluation is essential for the planning of treatment for prostate cancer.
- A basic staging evaluation includes the patient examination, blood tests, and the prostate biopsy including ultrasound images of the prostate.
- Further testing and calculations may be performed to best estimate a patient’s prognosis and help the doctor and patient decide upon treatment options.
Prognosis refers to the likelihood that cancer can be cured by treatment, and what the patient’s life expectancy is likely to be as a consequence of having had a prostate cancer diagnosis.
If cancer is cured, your life expectancy is what it would have been had you never been diagnosed with prostate cancer. If cancer cannot be cured due to it recurring in distant locations as metastases, or recurs either locally or in an area no longer able to be treated in a curative manner, then estimates can be made of what is likely to be your survival-based again on group statistics for people who have been in the same situation.
Nomograms are charts or computer-based tools that use complex math from the analysis of many patients’ treatment results.
The prognosis for prostate cancer varies widely and depends on many factors, including the age and health of the patient, the stage of the tumor when it was diagnosed, the aggressiveness of the tumor, and cancer’s responsiveness to treatment, among other factors.
The 5 and 10-year survival rate of prostate cancer chart
| Stage and 5-Year Survival |
|---|
Also Check: What Is Proton Therapy For Prostate Cancer
The Seminal Vesicle And Its Role In Prostate Cancer
Doru Paul, MD, is triple board-certified in medical oncology, hematology, and internal medicine. He is an associate professor of clinical medicine at Weill Cornell Medical College and attending physician in the Department of Hematology and Oncology at the New York Presbyterian Weill Cornell Medical Center.
A seminal vesicle is one of a pair of small tubular glands. These glands are positioned inside the body: above the prostate, behind the bladder, and in front of the rectum. One sits toward the left and the other sits toward the right. Each is roughly two inches long, on average.
The primary function of the seminal vesicles involves the production of fluid that mixes with sperm and makes up a significant percentage of semen. The fluid that the seminal vesicles produce is rich in sugars because it’s designed to feed sperm. It’s also sticky, so that semen stays in the vagina long enough for a sperm to fertilize an egg.
If a man develops prostate cancer and it metastasizes , the disease will often spread to the seminal vesicles.
Data Acquisition And Definitions
RPs were conducted by several surgeons using open, laparoscopic, or robotic modality. All pathological specimens were evaluated by a staff pathologist with genitourinary expertise. The following variables were compared between the categorical groups: age body mass index pre-biopsy prostate-specific antigen level pathologic Gleason score pathologic characteristics including extracapsular extension , positive surgical margin , and lymph node invasion radiologic findings, including ECE and lymph node enlargement and BCR. BCR was defined as two consecutive rises in PSA, with the last PSA 0.2ng/ml or higher after the RP.
Recommended Reading: What Is A Fusion Biopsy Of The Prostate
Perineural Invasion On Prostate Biopsy: Does It Mean That I Have Advanced Prostate Cancer
The simple answer is NO, however it should change your treatment game plan.
A member of one of my support groups who has been doing active surveillance for about 5 years recently reported that their current biopsy indicated that they now have perineural invasion . They did not understand what was the significance of this finding and they wanted to know if they now had advanced prostate cancer.
In reality, PNI is found in almost 30% of positive biopsies.
However, before I discuss the significance of this finding it is important to understand what this means. When a pathologist finds that there is PNI they are saying that they have found prostate cancer cells surrounding or tracking along a nerve fiber within the prostate. This does not mean that the cancer has left the gland.
Not withstanding this the importance of this finding , it takes on a new light when you realize that nerves within the prostate travel outside of the gland through microscopic holes in the prostate capsule. The capsule is the outer covering of the prostate gland, which for some period of time can manage to contain cancer cells within the gland. In essence it is a barrier protecting the rest of your body from prostate cancer cells.
However, the nerves do pierce the capsule and can offer an easy exit point for cancer cells from the gland to the rest of your body.
Simply put, the presence of PNI doubles the chance of a man having T3 disease .
Stone NN, Stock RG, Parikh D, et al.J Urol. 1998 160:17221726.