What Is Prostate Cancer Screening
The diagnosis of prostate cancer usually follows a biopsy prompted by a significantly elevated initial PSA level, an increase in PSA levels over time, or an abnormal digital rectal examination. According to JAMA, patients with a prostate cancer history benefit from extended PSA monitoring. Elevated PSA levels may help determine when to go in for a prostate MRI and hopefully avoid unnecessary or repeat prostate biopsies.
The American Journal of Mens Health reports that prostate cancer diagnosis occurs most often in men older than 50. Other factors influencing the rate of prostate cancer are ethnicity and family history. Screening is vital because localized prostate cancer sometimes causes no symptoms or warning signs.
Magnetic Resonance Imaging And Ultrasound Fusion Guided Prostate Biopsy
The MRI/US Fusion Guided Prostate Biopsy combines magnetic resonance imaging and ultrasound technologies, enabling a targeted biopsy that is able to focus directly on suspicious areas of the prostate, unlike the traditional method. This advanced screening technique is also able to detect prostate cancer much sooner than with previous tests and marks one of the most significant advances in prostate screening in 30 years. It is expected to be especially helpful among men with a history of negative biopsies who are still suspected of having cancer due to persistently abnormal lab results, patients with enlarged prostates, and men who are being monitored based on certain test results. When cancer is detected, the technique provides a more accurate understanding of the disease, which allows physicians to offer better counsel to patients, who in turn can make more informed decisions regarding their care.
Preparation For The Biopsy
You cannot take aspirin or other blood thinners, such as Plavix, Eliquis, Brilinta, Pradaxa, Coumadin, Warfarin, Ibuprofen, Naproxen, Aleeve, Advil, Celebrex, Ecotrin, and many others for several days prior to your scheduled biopsy. If you take any of these or other anticoagulants please discuss this with your Urologist beforehand. It might be necessary that you also consult with your Cardiologist prior to stopping.
Recommended Reading: What Causes Your Prostate To Enlarge
Targeted Biopsy: A Smarter Way To Take Prostate Tissue Samples
Carter: Targeted biopsy finds higher-grade cancers that standard biopsy has missed.
For years, the biggest frustration with the prostate biopsy has been that it is “blind.” That is, although they are guided by ultrasound, urologists doing a biopsy really cant see whether one area of the prostate looks any different from another so they do the best they can by trying to sample tissue in a systematic way throughout the gland. The problem with this approach, says urologist H. Ballentine Carter, M.D., the Bernard L. Schwartz Distinguished Professor of Urologic Oncology, is that “we often miss significant prostate cancers. About half of men require a repeat biopsy within five years because of concerns that cancer is hiding there and was simply missed.”
Good news: Biopsy is getting a whole lot smarter with a new approach called multi-parametric MRI -guided biopsy, also known as fusion or targeted biopsy.
At Johns Hopkins, radiologists use a grading system from 1-5 based on results of the mpMRI to indicate the likelihood that cancer is present. Grade 1-2 means a low suspicion of cancer grade 3, right in the middle, is “indeterminate suspicion,” and grade 4-5 suggests a high suspicion.
“Prostate MRI can be used to assess the probability that cancer is present, and also the probability that a high-grade cancer is present,” says Carter. “But MRI cannot diagnose prostate cancer only a biopsy can do that.”
Where Do We Perform Prostate Biopsy
Prostate fusion biopsy is performed at the HIFU CLINIC Prostate Cancer Treatment Center at Carolina Medical Center, one of the most modern hospitals in Poland.
HIFU CLINIC Prostate Cancer Treatment Center is the only medical center in this part of Europe that utilizes the Koelis Trinity fusion biopsy system the most modern specialist equipment in this part of Europe .
Don’t Miss: Best Supplement For Men’s Prostate
What Are The Limitations Of Ultrasound
A biopsy can only show if there is cancer in the samples taken, so it is possible that cancer in unsampled areas of the prostate might be missed.
For MRI-guided biopsies, high-quality images are assured only if you are able to remain perfectly still while the images are being recorded. If you are anxious, confused or in severe pain, you may find it difficult to lie still during imaging, and the resulting images may not be of sufficient quality to be useful as a diagnostic tool.
Likewise, the presence of an implant or other metallic object sometimes makes it difficult to obtain clear MR images. A person who is very large may not fit into the opening of certain types of MRI machines.
MR imaging cannot always distinguish between cancer tissue and inflammation or the presence of blood products within the prostate, which sometimes occurs related to a prostate biopsy. To avoid confusing the two on imaging, prostate MR imaging may be performed six to eight weeks after prostate biopsy, if possible, to allow any residual bleeding to resolve itself.
MRI typically costs more and may take more time to perform than other imaging methods. Talk to your insurance provider if you have concerns about the cost of MRI.
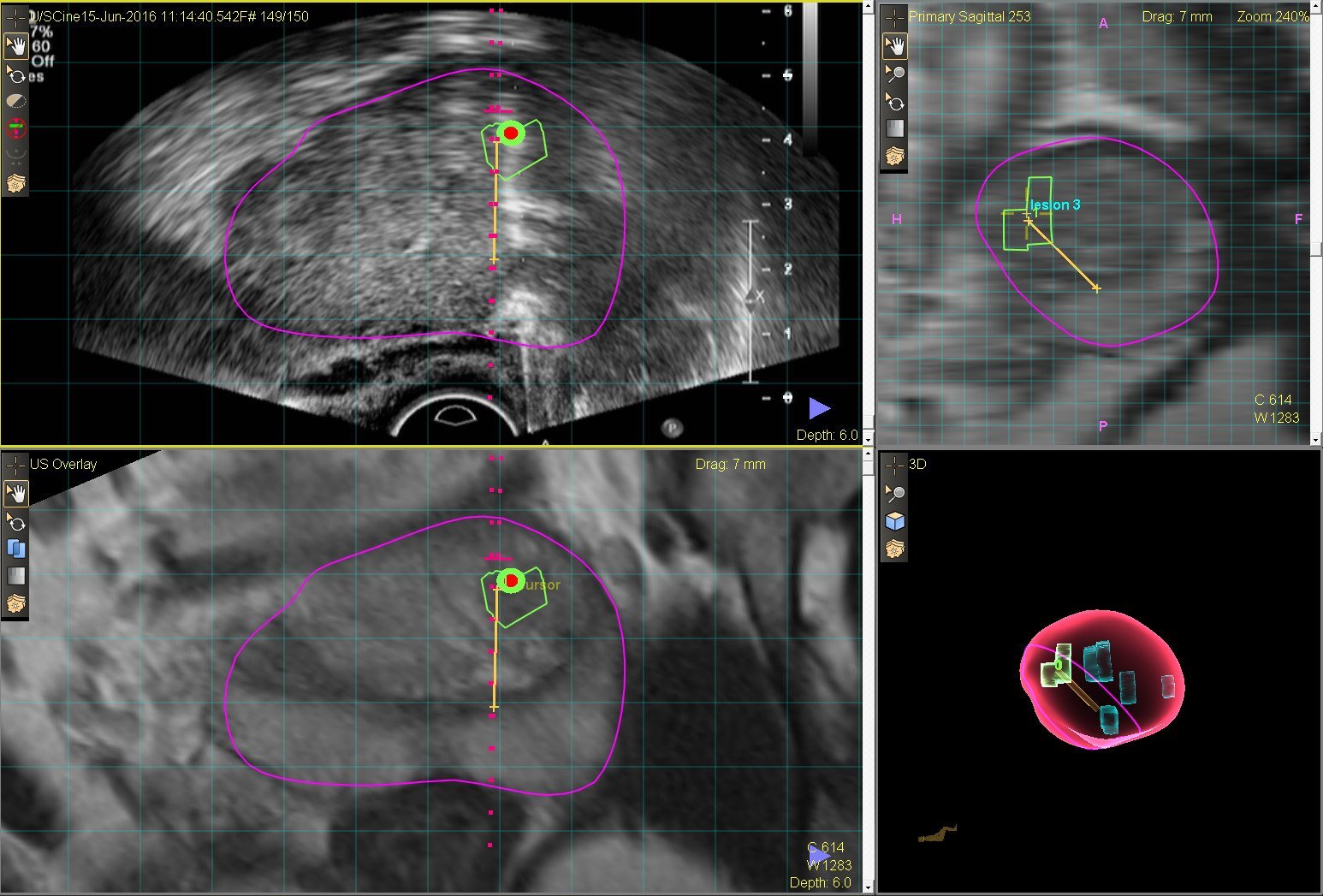
Homing In On Prostate Cancer With Fusion Biopsy
by Daniel Marchalik, MD, UrologyOctober 5, 2017
Left Image: The target from an MRI is merged with an ultrasound image for targeting. Right Image: The biopsy locations are captured by the MRI-Ultrasound fusion technology.
Ideally, doctors would catch every case of prostate cancer early, before it has time to grow and spread. Early detection gives men more options, whether that involves treatment or active surveillance to make sure the cancer doesnt continue to develop.
But standard approaches cant always locate the prostate cancer. Thats an issue for many of my patients. One man had previously had five standard biopsies, all of which were negative for prostate cancer. But he still had high levels of PSA, or prostate-specific antigen, which is a potential indicator of prostate cancer. I told him, You really should get an MRI.
The patients MRI test showed there was an abnormality in an area of the prostate where we dont usually see tumorsone thats difficult for us to access during a standard biopsy. So we used an advanced technique called an MRI/ultrasound fusion biopsy, which uses both MRI and ultrasound, to help detect this patients prostate cancer.
This patient would not have been diagnosed as early as he was without having an MRI/ultrasound fusion biopsy. And this is just one of the many examples Ive seen of this technologys value to patients.
Also Check: How Is Prostate Test Done
What Does An Elevated Psa Mean
The PSA test, which detects the level of prostate-specific antigen in a mans blood, is a valuable screening tool for prostate cancer. While the normal PSA range can vary based on a patients age and other factors, a PSA of 4.0 ng/mL or higher is generally considered abnormal for men over 60. Most cases of an abnormal or elevated PSA result can be attributed to a benign condition, though a PSA elevation can also be an indicator of prostate cancer. The most common causes of an elevated PSA include:
- Age
- BPH
- Inflamed prostate
- Injury or trauma to the prostate
- Recent ejaculation
- Prostate cancer
Depending on the degree of elevation, the patients PSA history, the patients risk for prostate cancer, and other factors, further diagnostic testing and/or biopsy may be required to rule out disease. Kasraeian Urology is proud to offer the most advanced prostate cancer screening tools available in Greater Jacksonville, including:
- MRI/US fusion biopsy
- ExoDx
% Less Detection Of Insignificant Cancer 3 Times Less Biopsy Core: Less Complication And Side Effects Mri/us Fusion Cancer Detection Rate
PRECISION study : MRI-Targeted or standard Biopsy for Prostate-Cancer Diagnosis
V.Kasivisvanathanet al. May 2018
For this reason:
- In cases of negative results, the hypothesis of cancer cannot be ruled out.
- In cases of low-positive results, suspicion of more aggressive cancer may remain.
Conventional Biopsy : Possible results
25% of cases Biopsy misses the tumor
Fortuitous reaching of non significant cancer
Underestimation of tumors size
Delaying the diagnosis, under- or overestimating the aggressiveness of the disease and, ultimately, failing to provide the best possible care for the patient.
However, the evolution of medical imaging techniques together with advances in fusion technologies have changed the landscape where practices are concerned.
In technical terms, targeted biopsies are made possible by the fusion of ultrasound images of the prostate with MRI scans or PET sequences, in real time during the procedures.
You May Like: Gleason 8 Prostate Cancer Treatment
What Does The Equipment Look Like
Ultrasound equipment:
Ultrasound scanners consist of a console containing a computer and electronics, a video display screen and a transducer or probe that is used to do the scanning. The transducer sends out inaudible high frequency sound waves into the body and then listens for the returning echoes. The principles are similar to sonar used by boats and submarines.
The ultrasound image is displayed on a video screen that looks like a computer or television monitor. The resulting image is based on the amplitude and frequency of the signal. The ultrasound image makes an image taking into account signal travel time, tissue composition, and type of body structure through which the sound travels.
The ultrasound probe used in prostate biopsies is about the size of a finger. Once the probe is placed in the rectum, the biopsy is performed with a spring-driven needle core biopsy device, or biopsy gun. The handheld device includes a long but very thin needle specially designed to open inside the prostate, take the sample and then close.
MRI equipment:
The traditional MRI unit is a large cylinder-shaped tube surrounded by a circular magnet. You will lie on a table that slides into the center of the magnet.
Prostate 3t Multiparametric Mri
Experts agree that MRI is the most sensitive imaging technique in relation to other imaging technologies at this time. Todays features include a number of parameters captured by a powerful 3 Tesla magnet that reveal much more than just prostate anatomy, enabling visual definition of even small prostate cancer tumors:
- Diseased tissue shows up as anatomical differences See Fig. 2a
- The movement of water molecules in tumor cells, different from normal cells See Fig. 2b
- The presence of certain chemicals in tumor cells, unlike normal cells See Fig. 2c
- Changes in the uptake and washout of contrast agents, another specific way to characterize cancer cells See Fig. 2d
In addition to these multiparametric indicators of a cancer, our powerful 3T magnet provides very high resolution of tumors.
Studies designed to correlate tumors identified by mpMRI in pre-prostatectomy patients confirm the accuracy of the MRI images when read by an experience radiologist, then compared with the surgically removed prostate specimens. According to an authoritative Dutch center, Multiparametric -MRI has been shown to be highly accurate in detecting and localizing intermediately aggressive and highly aggressive cancers. However, they caution that the experience of the radiologist conducting prostate MRI is crucial to how well images are captured and interpreted according to the highest standards.
Fig. 2a: T2 weighted images show suspected tumor activity
You May Like: Diet And Prostate Cancer Progression
Mri Fusion Prostate Biopsy
New River Urology is pleased to offer the first MRI-Ultrasound fusion prostate biopsy procedure in the Lowcountry.
For almost 30 years, urologists have utilized ultrasound to guide the prostate biopsy procedure. This is essentially a blind technique whereby ultrasound is merely used to ensure that the biopsy needles have hit the prostate. This has led to false negative biopsies in many instances, as well as over detection of slow growing, non-lethal cancers which may not even require any treatment.
Recent advances in MRI technology now allow us to identify potentially lethal cancers that before could not be visualized on ultrasound. We can now offer patients a screening prostate MRI and if a suspicious lesion is found, specifically target that lesion with our biopsy procedure using a fusion ultrasound device. Using this MRI targeted biopsy, the detection rate of insignificant cancers is lower than with systematic blind ultrasound guided biopsy. Further, when MRI findings have been correlated with pathologic findings, tumor localization appears to be significantly better with MRI than with the digital rectal examination or with ultrasound guided blind biopsy, and in the detection of prostate cancer that is clinically significant, MRI appears superior to all other imaging modalities evaluated to date.
Who should have a targeted prostate biopsy?
Our Locations
How Is The Biopsy Procedure Performed
Ultrasound-guided biopsy procedure:
The ultrasound-guided prostate biopsy is carried out by a radiologist or urologist, assisted by a sonographer and often a nurse who helps look after the patient.
You may have a small enema inserted into your rectum half an hour or so before the procedure to clean out your bowels and clear the rectum of feces so that the prostate may be seen more clearly with the ultrasound and to lower the risk of infection.
You may also be given antibiotics just before the procedure as an additional safeguard against infection. You also may receive medication for pain and anxiety. Sometimes an injection of local anesthetic or sedative will be given in the area of the rectum to minimize discomfort during the procedure.
The procedure is often carried out after you have been given a light general anesthetic, which means you will be asleep or sedated during the procedure. If the procedure is carried out using an anesthetic, an anesthesiologist will be present.
During the procedure, you will be asked to lie on your left side with your legs bent.
The physician will first carry out a DRE with a gloved finger.
An ultrasound probe will then be inserted into your rectum. The probe is sterilized, covered with condoms to ensure protection from any infection or contamination, and lubricated to help it glide easily into your rectum.
The entire ultrasound-guided biopsy procedure is usually completed within 45 minutes or less.
MRI-guided biopsy procedure:
Don’t Miss: Prostate Cancer Statistics By Age
What Happens After An Mri
You may resume your normal activities and diet immediately. You may be sore for a few days, and you also may see small amounts of blood in your urine, stool, and semen. However, these symptoms usually last only a few days. A high fever or flu-like symptoms within a few days of the biopsy should cause you to seek attention in a local emergency room to get treated for an infection.
Last reviewed by a Cleveland Clinic medical professional on 11/03/2016.
References
Mr/ultrasound Fusion Biopsy For A Targeted Diagnosis
At Fox Chase, we offer the latest in imaging and prostate biopsy technology in order to improve the care we can offer to our patients. Employing the power of the technique called multiparametric magnetic resonance imaging , our world-class radiology team can localize tumors within the prostate with a high degree of accuracy, identifying tumors that historically went unrecognized. This technology can give patients piece of mind that aggressive disease is not being missed and uncover aggressive cancer in some individuals with tumors in uncommon and remote locations in the prostate.
Using UroNav Ultrasound /MRI fusion technology, which allows precise targeting with biopsy to evaluate lesions found on mp-MRI, we are now less likely to miss aggressive disease and, thus, potentially minimize the need for repeated prostate biopsies in the future. Furthermore, we can better assure men who choose active surveillance for low-risk prostate cancer that an aggressive tumor is not missed or overlooked. Indeed, Fox Chase is one of the first institutions in the Delaware Valley to offer US/MRI fusion capabilities to patients undergoing prostate biopsy.
Why a Fusion Biopsy?
Fusion Biopsies vs. Traditional Biopsies
Biopsies guided by MR/ultrasound fusion enable both physicians and patients to make more informed decisions ranging from prostate cancer diagnosis to treatment optionssuch as active surveillance or more radical interventions.
You may be a candidate if you:
Also Check: How To Fix A Swollen Prostate
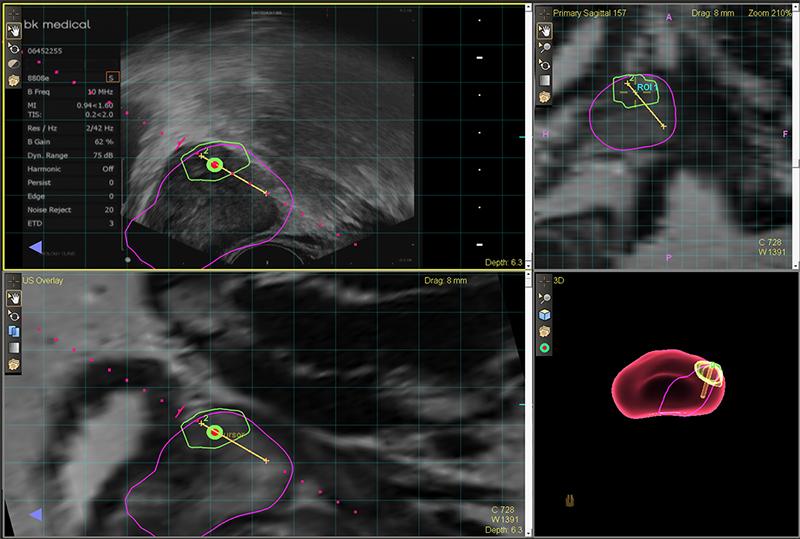
Koelis Technology For Fusion Biopsy
For over a decade KOELIS® has assisted urologists and radiologists from around the world in their routine clinical practice providing the latest technology for personalized prostate cancer.
We propose precise real-time 3D transrectal ultrasound fusion-guided transperinal and transrectal prostate biopsy against conventional and random systematic biopsy to increase sampling quality with KOELIS Trinity®. In a simple process and device, KOELIS Trinity® cartographer is a powerful diagnostic tool to plan, implement, review and control a personalized care solution. It creates a detailed and personalized map of the patients prostate showing accurate core distribution since our image-based cartographer is equipped with the Organ-Based Tracking® technology. Without changing the usual clinical practices, this technique brings an increased quality control over biopsy localizations. A precise, individual prostate biopsy mapping is a value for the accurate diagnosis and the further management of each patient.
Health innovation as a passion
At KOELIS®, we innovate every day in collaboration with world-renowned universities and hospitals to offer physicians new advancements in imaging and a greater field of view in order to bring personalized answers to every patient, in the respect of their quality of life.
Do you have questions about our precision fusion technology? Find the common inquiries or contact us !
To locate a clinic equipped with our solutions: Discover our interactive map.
Who Needs A Fusion Prostate Biopsy
Your doctor typically recommends a fusion prostate biopsy after multiple prostate-specific antigen tests. PSA testing uses a sample of your blood to test the levels of prostate-specific antigen. If multiple tests produce worrisome results, a biopsy is the next step.
Traditional biopsies rely on ultrasound to test tissue from random parts of the prostate. Although ultrasound helps with the placement of the needle, it does not allow your doctor to see which parts of the prostate are showing signs of cancer.
With the introduction of MRI technology, your doctor produces a 3D image of your prostate, allowing the team to test tissue from worrisome areas. Fusion prostate biopsies increase the accuracy of prostate cancer screening and reduce the need for repeated biopsies.
Read Also: Prostate Cancer In African American Males