Latest Clinical Studies Of Pbt
The dosimetry advantage of protons over photons has already been established . However, do the potential advantages of the proton beam significantly transfer into clinical benefits for patients? Can the advanced techniques such as 360° rotational gantries and intensity-modulated proton therapy further minimize toxicity and/or improve the clinical outcome? To date, there is not enough evidence to answer these questions due to small cohorts of patients in most published studies and the limited prospective data of comparisons between proton and photon radiotherapy. In this part, we present the clinical experiences and studies in the past few years, which may be provide a valuable understanding of the true value and advantage of PBT.
I Am A Uk Resident Living In One Of The Devolved Administrations Can I Receive Nhs Funded Proton Beam Therapy At The Christie
The NHS in England is a residence-based system, unlike many other countries, which have insurance-based healthcare systems. This means that visitors to England may have to pay for NHS healthcare, depending on their circumstances.
The devolved administrations, Scotland, Wales and Northern Ireland can access proton beam therapy at The Christie if the respective administrations approve it.
Further information can be found at NHS Choices.
Recovering From Prostate Cancer Treatment
If youve been through first-line treatment, but still have cancer, your doctor will adjust your treatment accordingly.
After surgery, radiation, or chemotherapy, you may be told that youre cancer free. But youll still need to be monitored for recurrence. If youve been taking hormone therapy, you may need to continue to do so.
Periodic PSA testing can help gauge effectiveness of hormone therapy. The pattern of PSA levels can also help monitor for recurrence.
The process of recovery is different for everyone. Much depends on the stage at diagnosis and the extent of treatment. Your age and general health also play a role. Your doctor will take all these factors into consideration to give you an idea of what to expect, including:
- the schedule for follow-up exams and tests
- how to deal with short- and long-term side effects
- diet and other lifestyle recommendations
- signs and symptoms of recurrence
Read Also: Aggressive Prostate Cancer Survivor Stories
How Do I Prepare For Proton Therapy
Proton therapy facilities are growing in number, but the treatment is still not available everywhere. Your doctor can let you know if theres a proton treatment center near you. If there is, there are a few things to think about in advance.
Treatment usually means going in five days a week for four to eight weeks, so youll want to clear your calendar. Although the actual treatment only takes a few minutes, you should probably block 45 minutes to an hour for the whole procedure.
Before you start treatment, youll have an initial consultation so the radiation team can get set up for future visits. Using a series of images and other data, theyll determine exactly how youll need to be positioned during therapy. It may involve the use of customized immobilization devices. This can be an involved procedure, but its necessary to ensure that protons are delivered precisely to improve your outlook.
No other preparation is necessary.
How Proton Beam Therapy Works
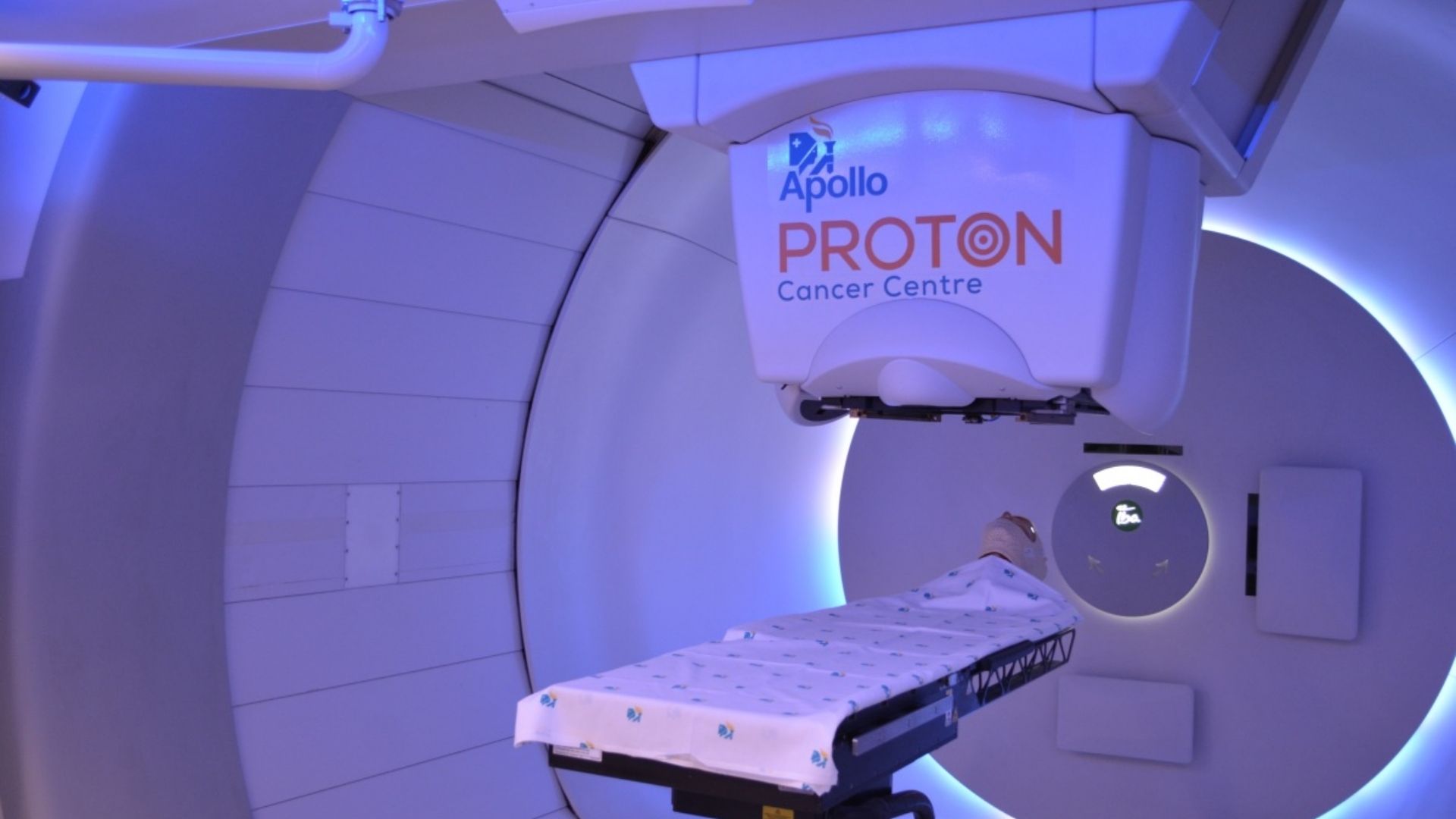
Proton therapy is an advanced form of radiation treatment that uses protons instead of X-rays.
In regular radiation therapy, the beam of energy goes into the body, through the tumor, and out the other side. This exit dose of radiation might affect healthy tissue beyond the tumor. Protons, in contrast, are larger particles than those used in regular radiation. They release more of their energy within the tumor itself. This burst of energy can appear on a graph as what is called the Bragg peak.
After delivering the energy to the tumor, the protons stop: They do not exit the tumor and go into healthy tissue on the other side.
In this way, proton therapy reduces radiation exposure and potential damage to healthy tissue, especially in sensitive areas such as the brain, eyes, spinal cord, heart, major blood vessels and nerves.
Read Also: Effects Of Having Prostate Removed
External Beam Radiation Therapy: How It Works
EBRT refers to the external delivery of any type of radiation, and can use several different types of energy including photons, electrons, and heavy particles . Additionally, there has been an evolution in the methods to deliver this energy , progressing from two-dimensional radiation therapy to three-dimensional conformal radiation therapy , and, more recently, intensity-modulated radiation therapy .
Dose distribution curves of photon and proton beams. The spread-out Bragg peak is demonstrated here to cover the entire target with the maximal dosage.
Schematic of multileaf collimator. Individually positioned tungsten leaflets conform the shape of the beam to the target as used in three-dimensional conformal radiation therapy.
Advances in image guidance such as on-board imaging units have helped to deliver the radiation more accurately to the prostate. These have dramatically decreased the uncertainty in target localization and improved the accuracy of radiotherapy to the prostate. However, despite all of these advances, the physical parameters of a photon beam will always include both entrance and exit doses and, ultimately, a significant volume of normal tissue receiving low to moderate doses.
Proton Therapy Success Stories
Its one thing to hear about the success rate of proton therapy treatment for prostate cancer. Its another thing to hear the success stories straight from the mouths of survivors.
Walter Knight, an Army pilot, biker, and all around adventurer, was diagnosed with prostate cancer only six weeks after being prescribed testosterone for his anemia.
There are unending volumes in thousands of books that attempt to describe the kaleidoscope of feelings and emotions that follow a diagnosis of metastatic cancer, said Knight in his journal entitled the Proton Chronicles. Im sure that like many, I attempted to rationalize or even justify the situation, but when faced with real mortality, your life and that of your family is forever altered.
After considering surgery and consulting multiple online forums, Knight finally decided on proton therapy to treat his cancer. Over the course of 20 hypofractionated treatments, Knight continued to bike on his favorite trails and play hockey in the local ice rink.
Its really kind of difficult to get your head around the whole situation, said Knight about his proton treatment. This is happening at the cellular level and its absolutely painless.
Earl Malpass, a mission pilot and pastor, also received proton therapy after being diagnosed with prostate cancer. Malpass, whos lived in Alaska for over 15 years with his wife, Lynn, chose to seek medical care in other states after receiving his diagnosis.
Recommended Reading: Things To Know About Prostate Cancer
How Does It Work
When doses of protons enter a tumor, they deposit most of their energy at a specific target, destroying cancerous cells and preserving surrounding healthy tissue. This differs from conventional radiation therapy because a less significant dose of protons enter the body, therefore reducing damage to surrounding healthy tissue and critical organs. The result is a smaller chance for side effects and secondary cancers. With proton therapy for prostate cancer, treatments typically take only 15 to 20 minutes each day and are delivered five days a week for approximately eight weeks.
There is little to no recovery time after treatment, and the risk of immediate post-treatment impotency is minimized, especially in those with good sexual function prior to treatment. Most patients tolerate the treatments extremely well and are able to continue to work, exercise and remain sexually active during their treatment course and immediately after treatment is complete.
When Is Proton Therapy Appropriate
Proton therapy is not effective at treating certain cancers, such as those that have spread widely. Since the radiation focuses on a targeted area, it is impractical to use this treatment for cancers that have metastasized to more than a few places. Most importantly, proton therapy is most often used for cancers requiring radiation that are near extremely sensitive organs and tissues. In fact, proton therapy is used predominantly to treat the following types of cancer:
Treatment of these cancers using traditional radiation have a higher potential risk for both immediate and permanent damage to nearby tissues and cellular death.
Read Also: Does Prostate Cancer Have A Cure
Precision Of Proton Therapy
Proton therapy is precise, and therefore better able to avoid surrounding organs. The radiation dose deposited by protons increases gradually until it peaks suddenly, called the Bragg Peak, and then falls to zero. Radiation oncologists can control where the Bragg Peak occurs, pinpointing it to peak exactly within the prostate.
The images below show the amount and location of radiation that the body receives during treatment with proton therapy and X-rays/IMRT . Proton therapy limits the radiation delivered outside the prostate.
Who Are They Looking For
This study is looking for people who have been diagnosed with adenocarcinoma of the prostate within the last year. Only patients with early stage tumors will be accepted.
Patients with cancer spread beyond the prostate, who already underwent surgery, radiation therapy or chemotherapy cannot take part in this trial. Patients who received hormone therapy will also be excluded. Other conditions, such as autoimmune diseases , HIV infection, inflammatory bowel disease and previous hip replacement surgery also represent exclusion criteria.
Don’t Miss: What Is Good To Take For Prostate Health
Proton Vs Photon Radiation
Proton radiation is different from other types of radiation, which rely on photons. Photon radiation comes in three types: intensity-modulated radiation therapy , radioactive seed radiation , and stereotactic body radiation therapy . Sometimes a combination of brachytherapy in conjunction with one of the other types of beam radiation is used.
All types of radiation are effective, resulting in the death of cancer cells. All can potentially cause side effects if the radiation touches adjacent normal organs, such as the bladder, rectum, and urethra.
Theoretical Causes For Concern

There are some potential disadvantages to PBT for prostate cancer. There is no widely used method for confirming the proton range or that the SOBP is encompassing the prostate in vivo. However, the algorithms used to calculate the doses appear accurate enough that this is not generally a significant concern if sufficient compensation is used. Positron emission tomography scanning and similar technologies are being developed that may allow for in vivo determination of proton dose and range. Another possible disadvantage is the increased sensitivity of PBT to target motion because of the steep dose depletion beyond the SOBP. The prostate is not completely fixed and varies in position depending on the fullness of the bladder and rectum. However, fiducial markers with pretreatment localization and placement of rectal balloons to fix the prostate in location have been successfully employed to compensate for this issue.
You May Like: Foods To Avoid For Prostate
Spaceoar Vs Rectal Balloon
If you’ve heard about the rectal balloons used during proton therapy, you need not worry about that daily discomfort. Some of our patients use SpaceOAR, the first FDA-cleared spacing device to protect the rectum in men undergoing radiation therapy for prostate cancer. The SpaceOAR System is intended to temporarily position the anterior rectal wall away from the prostate during radiotherapy for prostate cancer, creating space to protect the rectum from radiation exposure. Placed through a small needle at UW Medicine, the hydrogel is administered as a liquid, but quickly solidifies into a soft gel that expands the space between the prostate and rectum. The hydrogel spacer maintains this space until radiation therapy is complete. The spacer then liquefies and is absorbed and cleared from the body in the patients urine.
Certain prostate cancer patients do not need any kind of spacer placed. Talk to your physician to determine which approach is most appropriate for you.
See additional resources below for more.
Who Is A Good Candidate
In most cases, you will be a good candidate for proton therapy if you were initially offered radiotherapy as an option. Patients who receive radiotherapy usually have no problems being a candidate for proton treatment. They are usually patients in an early stage or those with localized prostate cancer. It is also useful to keep advanced cancer under control for as long as possible and treat recurrent prostate cancer cases.
However, some patients may not benefit from proton therapy if they have one of these problems :
- In patients with hip replacements, because proton beams often cant reach beyond the prosthesis. In some proton therapy centers, these patients can still get a session when a hip replacement is limited to one side. But bilateral replacement makes it impossible to treat the patient with proton beam therapy.
- In patients with advanced prostate cancer in which treating the pelvic lymph nodes is fundamental. Since proton beam radiation is less likely to reach other tissues than the prostate, it is not applicable when treating surrounding lymph nodes.
- In overweight patients, because the proton beam can only go through a determined depth. This depth depends on the beams energy, and some centers may have a higher energy device that solves the problem.
Recommended Reading: Can Your Prostate Grow Back After Surgery
Current Indications For Proton Therapy In The Management Of Prostate Cancer
Proton therapy is indicated in several clinical scenarios in the management of patients with prostate cancer in light of its potential to reduce the risk for acute and late toxicities related to dosimetric advantages compared with photon-based radiation therapy. The indications for proton therapy are listed in Table 1 and are summarized below.
Comparisons of and indications for intensity-modulated radiotherapyvolumetric modulated arc radiotherapy , double-scattering proton therapy , and intensity-modulated proton therapy .
Potential Disadvantages Of Proton Therapy
Depending on techniques compared, there may be disadvantages in dose distribution with proton therapy compared with IMRT. For example, Trofimov et al found that IMRT provided better conformality of the high-dose volume to the target than double-scattered proton therapy did. The average conformality index was 2.73 with IMRT and 3.11 with the double-scattered proton therapy plans . Similarly, in a comparison of IMRT to double-scattered proton therapy, Underwood et al found that IMRT provided better high-dose conformality than proton therapy did when evaluating prescription isodose lines. In addition, IMRT provided lower volumes of both rectum- and bladder-receiving doses in the range of V50 to V70 compared with double-scattered proton therapy. This shortfall of double-scattered proton therapy can be eliminated by using IMPT, which is a more refined delivery method of proton particles using PBS. Trofimov et al found that IMPT provided a better conformality index than IMRT did when delivering high-dose radiation therapy to the prostate.
Read Also: Best Thing For Healthy Prostate
What Happens During Proton Beam Treatment
Once you are ready and in position, the therapists will leave the room so they can operate the proton beam machine. A video camera helps them see and hear you so you will not be alone.
The treatment itself takes only a few minutes. A large machine speeds up protons and creates energy. The proton beam focuses this energy into the body, at the precise depth where the tumor is located. The gantry might move around your body and treat the tumor from several positions.
You will not feel the proton beam as it enters the body or as it is treating the tumor.
Developing The Uk Proton Beam Therapy Service
The government committed £250 million capital investment for both NHS proton beam therapy centres. This includes the buildings and PBT cyclotron and gantries, providing 6 NHS treatment rooms .
Both Trusts have more information about the new proton beam therapy centres on their websites. This includes information on the clinical facilities, their location and, for UCLH, progress on construction.
You May Like: Newest Prostate Cancer Treatment Options
What Types Of Radiotherapy Are There
There are two common types of external beam radiotherapy:
- intensity-modulated radiotherapy
- 3-dimensional conformal radiotherapy .
Intensity-modulated radiotherapy
This is the most common type of external beam radiotherapy in the UK. A computer uses the scans from your radiotherapy planning session to map the location, size and shape of your prostate. The radiotherapy machine gives beams of radiation that match the shape of the prostate as closely as possible. This helps to avoid damaging the healthy tissue around it, reducing the risk of side effects.
The strength of the radiation can be controlled so that different areas get a different dose. This means a higher dose of radiation can be given to the prostate without causing too much damage to surrounding tissue.
3D conformal radiotherapy
As with IMRT, the radiation beams are mapped to the size, shape and position of the prostate. But the strength of the radiation cant be controlled in 3D-CRT, so all areas are treated with the same dose.
IMRT is now the standard type of external beam radiotherapy for prostate cancer in most hospitals, but some still use 3D-CRT. They are both effective ways of treating prostate cancer. Ask your doctor or radiographer which type of radiotherapy youre being offered.
Other types of radiotherapy
Stereotactic radiotherapy
Proton beam therapy
Read more about clinical trials. Or to find out about taking part in a clinical trial, ask your doctor or nurse, or speak to our Specialist Nurses.
Proton Therapy Vs Traditional Radiation Therapy
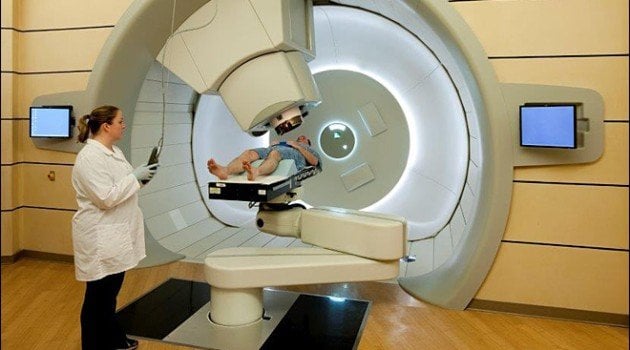
So, what makes proton therapy so much more successful than other prostate cancer treatments? The answer lies in the protons themselves.
Unlike proton therapy, traditional radiation treatment uses photons, which deliver low levels of radiation to the cancer tissues. These lower levels of radiation, in addition to the lower mass of the beam in comparison to a proton treatment, mean the radiation will cause damage to both the cancerous tissue and the surrounding healthy tissue.
On the other hand, proton therapy uses positively charged subatomic particles called protons, which are located in the nucleus of an atom. Because the mass of the proton beam is higher than the photon beam, a clinician can control the proton radiation in the patients body. The electrons in the patients body slow down the protons delivered from the beam. This results in an energy release that can destroy cancerous tissue, but avoid unnecessary radiation to surrounding areas. Unlike traditional radiation therapy, the clinician can use the proton beam to target the cancer cells in the body specifically, allowing for a more successful and far less damaging procedure.
Read Also: Hormone Therapy For Prostate Cancer Survival Rates