Active Surveillance And Watchful Waiting
If prostate cancer is in an early stage, is growing slowly, and treating the cancer would cause more problems than the disease itself, a doctor may recommend active surveillance or watchful waiting.
Active surveillance. Prostate cancer treatments may seriously affect a person’s quality of life. These treatments can cause side effects, such as erectile dysfunction, which is when someone is unable to get and maintain an erection, and incontinence, which is when a person cannot control their urine flow or bowel function. In addition, many prostate cancers grow slowly and cause no symptoms or problems. For this reason, many people may consider delaying cancer treatment rather than starting treatment right away. This is called active surveillance. During active surveillance, the cancer is closely monitored for signs that it is worsening. If the cancer is found to be worsening, treatment will begin.
ASCO encourages the following testing schedule for active surveillance:
-
A PSA test every 3 to 6 months
-
A DRE at least once every year
-
Another prostate biopsy within 6 to 12 months, then a biopsy at least every 2 to 5 years
Treatment should begin if the results of the tests done during active surveillance show signs of the cancer becoming more aggressive or spreading, if the cancer causes pain, or if the cancer blocks the urinary tract.
Management Of Bowel Dysfunction
Short of treating individual symptoms as needed, there are few, if any, treatment options for bowel dysfunction following radiation therapy. Laser therapy can stop rectal bleeding caused by radiation. Anti-diarrheal agents can help with loose bowel movements. Increasing fiber intake through whole grains, fruits and vegetables, or fiber supplements can also help.Avoiding foods that might irritate the gastrointestinal tract is important, but complete elimination of fibrous, bulky foods can lead to constipation and straining, which in turn can exacerbate rectal bleeding.
During Watchful Waiting Or Active Surveillance
If you choose observation or active surveillance, your PSA level will be monitored closely to help decide if the cancer is growing and if treatment should be considered.
Your doctor will watch your PSA level and how quickly it is rising. Not all doctors agree on exactly what PSA level might require further action . Again, talk to your doctor so you understand what change in your PSA might be considered cause for concern.
Read Also: Hdr Brachytherapy Prostate Cancer Side Effects
Radiation Dose Technique And The Effect Of Dose Escalation
Traditionally, the three randomized trials for ART used 6065Gy typically with 3D simulation . In some cases, the treatment volumes were typically very generous being described as approximately 10cm×10cm in the anteriorposterior fields with the inferior border at the ischial tuberosities. The lateral fields extended from the anterior aspect of the pubic symphysis and split the rectum posteriorly . In 3-Dimensional Conformal Radiation Therapy , the target volume should include the bladder neck , periprostatic tissues/clips, and the seminal vesicle bed . Inferiorly, the vesicourethral anastomosis should be included. The anastomosis is the most frequent area of positive prostate biopsies . By placing the inferior field edge at the top of the bulb of the penis and adding a margin for uncertainties, there should be adequate coverage. Laterally, the field should extend to about the medial aspect of each obturator internus muscle. Although the rectum is a landmark posteriorly, and its movement has been a matter of possible target missing, for this reason, a generous margin posteriorly is recommended in international guidelines . The superior margin is more subjective and should be guided by the extent of disease at the prostate base and whether the seminal vesicles are involved .
Remission And The Chance Of Recurrence
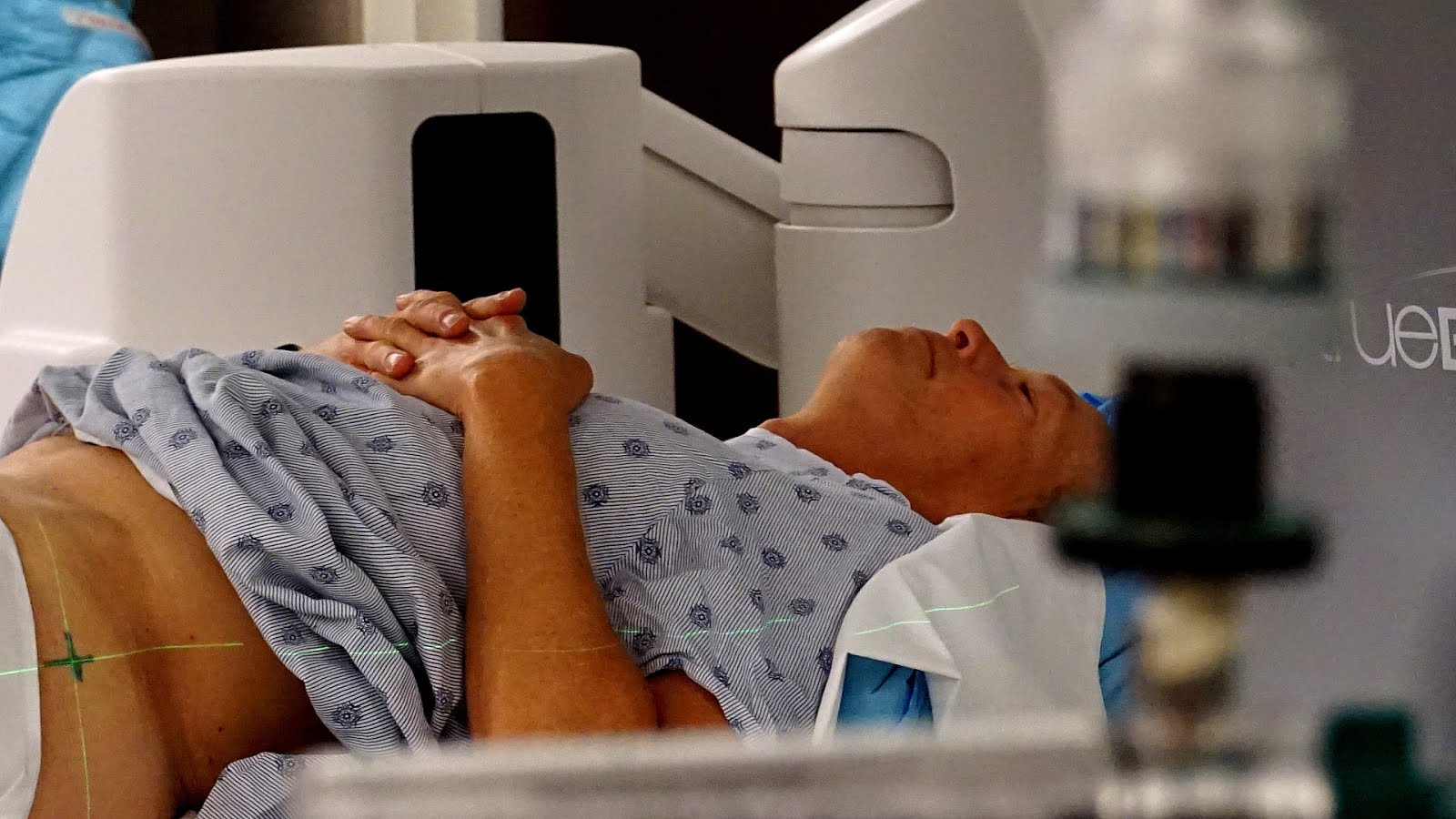
A remission is when cancer cannot be detected in the body and there are no symptoms. This may also be called having no evidence of disease or NED.
A remission can be temporary or permanent. This uncertainty causes many people to worry that the cancer will come back. Although there are treatments to help prevent a recurrence, such as hormonal therapy and radiation therapy, it is important to talk with your doctor about the possibility of the cancer returning. There are tools your doctor can use, called nomograms, to estimate someone’s risk of recurrence. Understanding your risk of recurrence and the treatment options may help you feel more prepared if the cancer does return. Learn more about coping with the fear of recurrence.
In general, following surgery or radiation therapy, the PSA level in the blood usually drops. If the PSA level starts to rise again, it may be a sign that the cancer has come back. If the cancer returns after the original treatment, it is called recurrent cancer.
When this occurs, a new cycle of testing will begin again to learn as much as possible about the recurrence, including where the recurrence is located. The cancer may come back in the prostate , in the tissues or lymph nodes near the prostate , or in another part of the body, such as the bones, lungs, or liver . Sometimes the doctor cannot find a tumor even though the PSA level has increased. This is known as a PSA-only or biochemical recurrence.
You May Like: How To Fix A Swollen Prostate
Psa Levels After Treatment
A continuous rise in your PSA level can be the first sign that your cancer has come back. This should be picked up by your regular PSA tests.
The exact change in PSA level that suggests your cancer has come back will depend on which treatment you had. Speak to your doctor or nurse about your own situation.
Your PSA level should drop so low that its not possible to detect it at six to eight weeks after surgery. This is because the prostate, which produces PSA, has been removed. A rise in your PSA level may suggest that you still have some prostate cancer cells.
After radiotherapy or brachytherapy, your PSA should drop to its lowest level after 18 months to two years. Your PSA level wont fall to zero as your healthy prostate cells will continue to produce some PSA.
Your PSA level may actually rise after radiotherapy treatment, and then fall again. This is called PSA bounce. It could happen up to three years after treatment. It is normal, and doesnt mean that the cancer has come back.
If your PSA level rises by 2 ng/ml or more above its lowest level, this could be a sign that your cancer has come back. Your doctor will continue to check your PSA level and will talk to you about further tests and treatment options.
Tips To Get The Most From Your Follow
Write down any questions or concerns beforehand
It’s easy to forget what you want to say once youre at your appointment.
Bring someone with you
It can be hard to take everything in at your appointments. Some people find it helpful to take someone with them, to listen and discuss things with later. If your appointment is on the phone, you could ask a friend or family member to listen with you.
Make notes
It can help to write things down during or after your appointment. Theres space for this in the appointment diary in our booklet, Follow-up after prostate cancer treatment: What happens next?
Ask to record your appointment
You could do this using your phone or another recording device. You have the right to record your appointment if you want to because its your personal data. But let your doctor or nurse know if you are recording them.
Ask for help
If there is anything bothering you, let your doctor or nurse know.
Ask for copies of any letters
If your appointment is at the hospital, ask for a copy of the letter that is sent to your GP. This will happen automatically at some hospitals. It will help to remind you of what was said at your appointment. If you don’t understand the letter, call your main contact at the hospital or contact our Specialist Nurses.
You May Like: Can A 12 Year Old Get Prostate Cancer
The Grade Group And Psa Level Are Used To Stage Prostate Cancer
The stage of the cancer is based on the results of the staging and diagnostic tests, including the prostate-specific antigen test and the Grade Group. The tissue samples removed during the biopsy are used to find out the Gleason score. The Gleason score ranges from 2 to 10 and describes how different the cancer cells look from normal cells under a microscope and how likely it is that the tumor will spread. The lower the number, the more cancer cells look like normal cells and are likely to grow and spread slowly.
The Grade Group depends on the Gleason score. See the General Information section for more information about the Gleason score.
- Grade Group 1 is a Gleason score of 6 or less.
- Grade Group 2 or 3 is a Gleason score of 7.
- Grade Group 4 is a Gleason score 8.
- Grade Group 5 is a Gleason score of 9 or 10.
The PSA test measures the level of PSA in the blood. PSA is a substance made by the prostate that may be found in an increased amount in the blood of men who have prostate cancer.
What Are The Types Of Radiation Therapy Used For Prostate Cancer
Radiationtherapy for prostate cancer can be divided into two main categories.
Externalbeam radiation :Using a machine outside the body, beams of radiation are focused on theprostate gland. This can help relieve symptoms such as pain while limiting thedamage to the tissues surrounding the prostate.
The 4methods of external beam radiation are:
- Three-dimensional conformal radiation therapy
- Intensity modulated radiation therapy
- Stereotactic body radiation therapy
- Proton beam radiation therapy
Brachytherapy:Small radioactive pellets are inserted into the prostate, each one about thesize of a grain of rice. About 100 pellets are used to limit the damage tosurrounding tissues and organs. Brachytherapy is most often used forearly-stage cases and is sometimes combined with EBRT. The pellets can eitherbe inserted for a couple of days for high dosages or a few months for lowdosage depending on the patients overall status.
Also Check: High Blood Count In Prostate
Bowel Dysfunction After Prostate Cancer Treatment
The broad term of bowel dysfunction includes:
-
Diarrhea or frequent stools
-
Fecal incontinence or the inability to control bowel movements
-
Rectal bleeding
All of these side effects are far more common following external beam radiotherapy than any other primary therapy, but as techniques and dose planning strategies improve, even these rates have been dropping.
Cancer That Is Thought To Still Be In Or Around The Prostate
If the cancer is still thought to be just in the area of the prostate, a second attempt to cure it might be possible.
After surgery: If youve had a radical prostatectomy, radiation therapy might be an option, sometimes along with hormone therapy.
After radiation therapy: If your first treatment was radiation, treatment options might include cryotherapy or radical prostatectomy, but when these treatments are done after radiation, they carry a higher risk for side effects such as incontinence. Having radiation therapy again is usually not an option because of the increased potential for serious side effects, although in some cases brachytherapy may be an option as a second treatment after external radiation.
Sometimes it might not be clear exactly where the remaining cancer is in the body. If the only sign of cancer recurrence is a rising PSA level , another option for some men might be active surveillance instead of active treatment. Prostate cancer often grows slowly, so even if it does come back, it might not cause problems for many years, at which time further treatment could then be considered.
Factors such as how quickly the PSA is going up and the original Gleason score of the cancer can help predict how soon the cancer might show up in distant parts of the body and cause problems. If the PSA is going up very quickly, some doctors might recommend that you start treatment even before the cancer can be seen on tests or causes symptoms.
Read Also: Focused Ultrasound For Prostate Cancer
Adjuvant And Salvage Post
Sometimes, intensity modulated radiation therapy is given after a patient has had a prostatectomy. There are two situations where this treatment done. In the first situation, it may be known before the surgery or discovered after the surgery, that the cancer was more extensive than expected. The cancer may have penetrated the capsule which surrounds the prostate or extended into the seminal vesicles or extend to the edge of the surgical margin. In this case, your physicians may determine in consultation that a course of IMRT to the prostate bed and surrounding tissue is needed to reduce the risk of a recurrence and kill any microscopic prostate cancer cells that may be present. The goal of adjuvant post-prostatectomy radiation therapy is to reduce the risk or eliminate a recurrence of cancer in the prostate bed.
In the second situation where IMRT is given after a prostatectomy, usually months or years have passed since the surgery before evidence of a recurrence in the prostate bed develops. This is usually discovered by a rising PSA after surgery. In this situation, treatment called salvage post-prostatectomy IMRT is given to the prostate bed and surrounding tissue to kill the recurrent prostate cancer cells. The goal of this treatment is to eradicate the prostate cancer and lower the PSA.
Daily CT scans or Calypso beacons for daily localization and tracking is used with both adjuvant salvage post-prostatectomy radiation therapy.
Other Key Findings In The Study
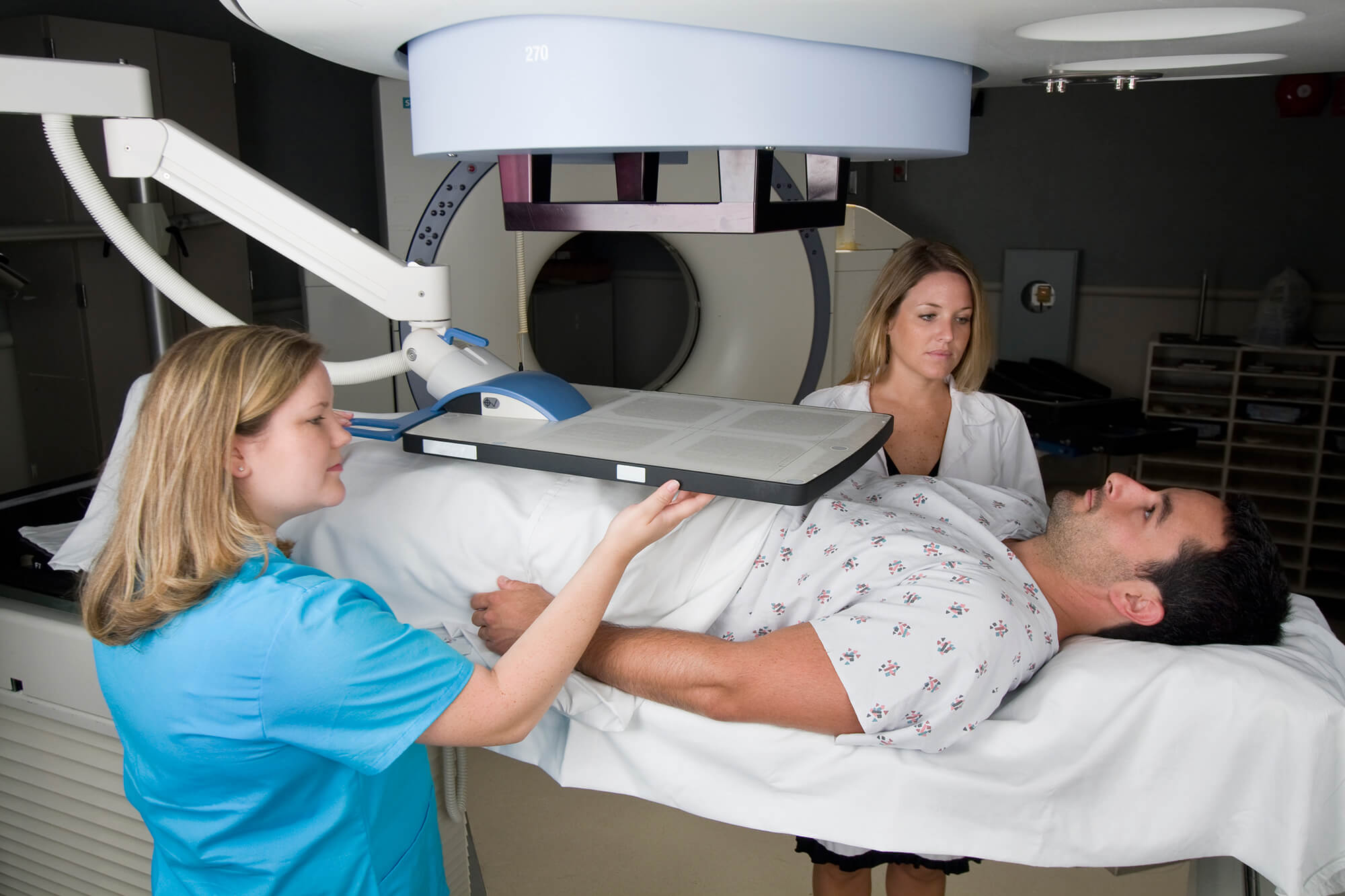
Patients who had lower PSA scores:
- Experienced an eight-year disease-free survival rate of 75 percent, compared with only 18 percent for those with the highest PSA scores.
- Had a 97 percent distant metastasis-free survival rate, compared with 73 percent for those with the highest PSA scores.
However, the study also indicated that, when a PSA is falling, there is no specific number that predicts future survivability.
While there is no magic number for the PSA that guarantees that prostate cancer has been cured in an individual patient, in general, the lower the PSA number, the better chances that the cancer will not return or spread, said Michael E. Ray, M.D., Ph.D., lead author of the study and a radiation oncologist at the University of Michigan Medical Center.
You May Like: Prostate Removal Pros And Cons
Do We Know Which Treatment Is Better For Prostate Cancer Brachytherapy Or External Beam Radiation
Its not a question of which therapy is better but rather which therapy is the most tailored, pinpointed radiation for the patients specific disease.
When it comes to early stages of disease, patients very frequently do well with either brachytherapy or external beam radiation. Success rates of around 90% or higher can be achieved with either approach. When the disease is somewhat more advanced based on the PSA level or the Gleason score or visible evidence of disease on an MRI we have learned over the years that higher doses of radiation are critical to achieving better results. Some evidence suggests that for patients with intermediate- or high-risk prostate cancer, a combined approach using brachytherapy along with external beam radiation may be best.
Data that we have published recently show that for patients with intermediate-risk disease, the combination of external beam radiation with brachytherapy not only provides better biochemical control, in terms of PSA level, but also reduces the risk of distant metastases, or spread of the disease. Another recent study from Canada, which compared outcomes in patients who were treated with external beam radiation or a combination approach, found superior results when the combined approach was used. These studies provide strong evidence that higher doses of radiation provide an important benefit to patients with intermediate-risk and high-risk prostate cancers.
Signs Of Prostate Cancer Include A Weak Flow Of Urine Or Frequent Urination
These and other signs and symptoms may be caused by prostate cancer or by other conditions. Check with your doctor if you have any of the following:
- Weak or interrupted flow of urine.
- Sudden urge to urinate.
- Frequent urination .
- Trouble starting the flow of urine.
- Trouble emptying the bladder completely.
- Pain or burning while urinating.
- Blood in the urine or semen.
- A pain in the back, hips, orpelvis that doesn’t go away.
- Shortness of breath, feeling very tired, fast heartbeat, dizziness, or pale skin caused by anemia.
Other conditions may cause the same symptoms. As men age, the prostate may get bigger and block the urethra or bladder. This may cause trouble urinating or sexual problems. The condition is called benign prostatic hyperplasia , and although it is not cancer, surgery may be needed. The symptoms of benign prostatic hyperplasia or of other problems in the prostate may be like symptoms of prostate cancer.
Read Also: What Does Low Grade Prostate Cancer Mean
Salvage Radiotherapy And Androgen Deprivation Therapy
GETUG-AFU 16 was the first randomized trial comparing SRT vs. SRT and short ADT as salvage treatment for biochemical recurrent prostate cancer after radical prostatectomy and was presented in abstract form at the American Association of Clinical Oncology 2015 Annual Meeting. The trial randomized 743 patients most of them having high intermediate risk features . The 5-year PFS was 62.1% vs. 79.6% for SRT and SRT+ADT, respectively . The 5-year OS was 94.8% for RT vs. 96.2% for SRT+ADT . Cause of death was progressive disease in 2.1% of the patients on SRT arm vs. 0.8% in the SRT+ADT arm. Acute toxicities occurred more frequently in SRT+ADT arm . This trial will require longer follow-up to see if the benefits observed in progression-free survival translate into the same OS benefit .