What Side Effects Will I Have
During your treatment, radiation must pass through your skin. You may notice some skin changes in the area exposed to radiation. Your skin may become red, swollen, warm, and sensitive, as if you have a sunburn. It may peel or become moist and tender. Depending on the dose of radiation you receive, you may notice a loss of hair or decreased perspiration within the treated area.
These skin reactions are common and temporary. They will subside gradually within four to six weeks of completing treatment. If skin changes appear outside the treated area, inform your doctor or primary nurse.
Long-term side effects, which can last up to a year or longer after treatment, may include a slight darkening of the skin, enlarged pores, increased or decreased sensitivity of the skin, and a thickening of tissue or skin.
Another possible side effect is erectile dysfunction and urinary symptoms such as frequency, bleeding, or, rarely, incontinence. Keep these side effects in mind when considering your treatment options. If you have any concerns, don’t hesitate to talk to your doctor about them.
Hdr Brachytherapy As Monotherapy
Despite promising initial results in the single-fraction experience, such treatment remains investigational, and the optimal single-fraction dosing regimen continues to be investigated. Specifically, the 19 Gy single-fraction dose was predicated on the assumption of the extremely low alpha-beta ratio for prostate cancer . Evidence shows that radioresponsiveness of prostate cancer may be heterogeneous and that certain cancers may, in fact, have alpha-beta ratios that are higher.28 For such tumors, 19 Gy may prove to be an insufficient dose , and continued evaluation of the optimal single-fraction HDR treatment approach is necessary.
Long Term Side Effects
The PACE-B clinical trial – taking place at The Institute of Cancer Research, London compared the long-term bowel and bladder side effects for patients receiving stereotactic body radiotherapy to those receiving standard radiotherapy treatment and found that, two years after treatment, nearly 90% of all patients on the trial experienced only minor side effects. 99% were free of severe side effects, suggesting that shortened treatment can be given without the risk of long-term higher toxicity.
874 patients with prostate cancer were randomised to two groups. 441 patients were allocated the current standard of care, receiving standard radiotherapy for either 39 doses over seven or eight weeks, or 20 doses over four weeks. 433 patients were allocated SBRT, receiving five doses of treatment over one or two weeks. For both groups of patients, 90 per cent of whom had intermediate risk prostate cancer, this was intended to be curative with no further treatment planned. Researchers found that patients in both groups had similar levels of side effects two years after treatment, which were very low overall. Results suggested that about one in 9 men receiving the SBRT radiotherapy over five sessions will get a moderate bladder side effect two years after treatment, compared to about 1 in 17 men receiving standard radiotherapy. Bladder side effects experienced by patients included urinary frequency and urgency.
References:
Also Check: Benign Prostatic Hyperplasia Is Commonly Associated With
Patient Selection And Technical Description
Successful implementation of HDR brachytherapy for prostate cancer begins with appropriate patient selection. Anatomic factors lending to successful HDR treatment are as follows: prostate volume of approximately 20-60 cc a central/straight urethral position that can be adequately avoided during transperineal needle implant absence of significant benign prostatic hypertrophy/median lobe or transurethral resection of the prostate defect at the prostate base adequate spacing between the prostate and rectum and adequate pubic arch width to avoid interference with needle placement. Clinical factors include general risks of both anesthesia and elective surgical procedures . Careful attention must be paid to baseline urinary function. Brachytherapy is not a good treatment option for patients with significant baseline obstructive uropathy. Risks for significant obstructive complications of brachytherapy increase substantially in such patients, and our practice typically will exclude patients with a baseline American Urologic Association symptom score > 15 if already on medication, or > 20 if previously untreated for obstructive symptoms.3 Any of these factors are relative contraindications to performing HDR brachytherapy and the treating physician should consider them on a patient-by-patient basis, weighing risks and benefits.
The Night Before Your Procedure
- Take the medications your healthcare provider told you to take the night before your procedure. Take them with a small sip of water.
- Shower using soap and water the night before or the morning of your procedure.
- Do not eat anything after midnight the night before your procedure. This includes hard candy and gum.
- Between midnight and up until 2 hours before your scheduled arrival time, you may drink a total of 12 ounces of water .
- Starting 2 hours before your scheduled arrival time, do not eat or drink anything. This includes water.
Also Check: Prostate Cancer Center Of New Jersey
Who Can I Contact If I Have Personal Concerns About My Treatment
Many hospitals and clinics have a staff social worker who can help you during your treatment. Check with your doctor to see if this is available to you.
The social worker can discuss any emotional issues or other concerns about your treatment or your personal situation and provide information about resources. The social worker can also discuss housing or transportation needs if necessary.
People dealing with certain medical issues find it helpful to share experiences with others in the same situation. Your doctor can provide a list of support groups if you are interested. Your social worker can provide additional information, and you can look online for support group resources.
Faq: Radiation Therapy For Prostate Cancer
Why would I choose radiation therapy?
Radiation therapy, including external beam radiation therapy and brachytherapy, is an alternative form of treatment for prostate cancer. EBRT may be used after other treatments, such as surgery, to manage cancer that has recurred or is at high risk of recurrence. Radiation therapy has an excellent record of success, providing long-term disease control and survival rates equivalent to other treatments, including surgery.
How should I expect to feel during radiation therapy?
Undergoing external beam radiation therapy is similar to having a routine X-ray. Radiation cannot be seen, smelled or felt. Generally, side effects don’t appear until the second or third week of treatment. Because radiation therapy is a local treatment, only the areas of the body where it is directed will experience side effects. Most patients will experience some or all of the following:
- Increase in the frequency of urination
- Urinary urgency
- Softer and smaller volume bowel movements
- Increased frequency of bowel movements
- Worsening of hemorrhoids or rectal irritation with occasional scant blood and fatigue
Many questions may arise during radiation therapy treatment. Your doctors will be available to answer questions throughout your treatment.
How should I expect to feel after radiation therapy?
Recommended Reading: Is Testicular Cancer The Same As Prostate Cancer
If I Choose Radiation Therapy Will Surgical Treatment Still Be An Option
If radiation therapy is used as the primary treatment, and the treatment is not successful, surgery or repeat radiation therapy are not considered to be desirable treatments due to the high risk of serious complications. It is important to note that the cure rates for surgery and radiation are similar. Therefore, you may have the same risk of cancer recurring if surgery is performed. If surgery is performed after radiation, or additional radiation is recommended, the physician performing the re-treatment should have a high level of experience. There are experimental clinical studies being evaluated for use of very localized re-irradiation for this group of patients. Some patients for which radiation is not effective are treated by systemic therapy or by close surveillance.
What Are The Side Effects Of Brachytherapy
- Frequent urination or urinary retention or burning with urination
- Erectile dysfunction
- Urethral stricture or narrowing of the urethra
- Diarrhea or blood in the stool
- Secondary cancers
For the short time that the seeds are giving off larger amounts of radiation, you should avoid close proximity to children or pregnant women. Make sure to talk with your radiation oncologist or oncology nurse for instruction about radiation safety and exposure for family members or pets.
If you are traveling through an airport following brachytherapy treatment, there is a chance that radiation detectors will be set off. Talk to your radiation oncologist and ask for a note to indicate youve just had radiation treatment.
Recommended Reading: How To Heal Your Prostate
Your Role On Your Radiation Therapy Team
Youll have a team of healthcare providers working together to provide the right care for you. Youre part of the team, and your role includes:
- Arriving on time for your procedure.
- Asking questions and talking about your concerns.
- Telling someone on your radiation therapy team when you have side effects or pain.
- Caring for yourself at home.
- Quitting smoking, if you smoke. If you want to quit, call our Tobacco Treatment Program at .
- Drinking liquids as instructed.
What Are The Different Types Of Internal Radiation Therapy
Brachytherapy and radiopharmaceuticals are both considered internal radiation therapies because they both work after being inserted inside the body, rather than being directed from outside. However, the similarities mostly end there. Brachytherapy works by implanting radioactive material into the prostate and is used for localized prostate cancer. Radiopharmaceuticals are injected into the bloodstream and are used for advanced, metastatic prostate cancer. Read on to find the details of each.
Don’t Miss: What Food Helps Prostate Problems
When Is Brachytherapy Alone The Right Choice
For a patient with disease that is confined to the prostate and not too aggressive, brachytherapy alone is a good option. With the use of sophisticated real-time computer-based planning, we can use brachytherapy to deliver radiation in an extraordinarily precise way, with minimal exposure to the surrounding normal tissues. It is also convenient for the patient as it is done in an outpatient setting and most people are able to get back to work the next day.
But brachytherapy is not right for everyone. For some patients with less-aggressive disease, a watch-and-wait approach would also be very reasonable. At MSK, our philosophy is that when the disease is caught very early meaning a low PSA level, or nonaggressive disease as reflected by a Gleason score of 6 with evidence of cancer in only a few of the biopsy samples and no evidence from the MRI of a significant amount of disease then it would be very appropriate to do active surveillance and hold off on treatment.
High Dose Stereotactic Body Radiotherapy
High dose stereotactic body radiotherapy treatment of men with newly diagnosed prostate cancer appears to result in shorter treatment times, less severe toxicity and excellent cancer control rates.1-6
Although prostate cancer generally responds well to radiation therapy, the possibility of radiation exposure to healthy tissue in the genitourinary and gastrointestinal systems can be of concern. SBRT is an advanced technique that precisely targets high doses of radiation to the cancer in a small number fractions, simultaneously avoiding surrounding tissue and reducing toxicity to non-cancerous cells.
Men with early stage prostate cancer can currently be treated with surgical prostatectomy, brachytherapy or external beam radiation therapy . SBRT, a form of EBRT condenses the radiation treatment for prostate cancer into as few as four to five sessions . The technique has become the standard of care for many non-surgical lung cancer patients, as it limits exposure to the heart and surrounding lungs. When treating tumors in the prostate, SBRT avoids the adjacent bladder, sex organs and rectum.
Recommended Reading: Soy Milk And Prostate Cancer
Dose And Fractionation For Hdr Boost
The American Brachytherapy Society consensus guidelines for HDR prostate brachytherapy was unable to recommend a particular dose fractionation schedule for HDR boost, reporting high biochemical control rates despite a wide variation in dose and fractionation . Recommendations from the European brachytherapy group, GEC/ESTRO reference the following published EBRT dose fractionation schedules :
-
45 Gy in 25 fractions over 5 weeks
-
46 Gy in 23 fractions over 4.5 weeks
-
35.7 Gy in 13 fractions over 3 weeks
-
37.5 Gy in 15 fractions over 3 weeks.
Combined with the following HDR brachytherapy schedules:
-
15 Gy in 3 fractions
-
1122 Gy in 2 fractions
-
1215 Gy in 1 fraction.
Focal boosting with increased dose to areas of gross disease is readily achieved with HDR. Most reports use multimodality fusion, where the planning image sets are co-registered with a diagnostic multiparametric MRI. This can involve either a rigid or elastic co-registration. The purpose of this strategy can either be to improve local control by dose escalation to the gross disease, and/or to reduce toxicity by selective dose de-escalation to the remainder or the gland. Such approaches are well tolerated, but it is not yet known how they compare with more conventional whole gland treatments .
Focal Therapy For Prostate Cancer
With recent advances in MRI and targeted biopsy, we are better able to locate the exact area of prostate cancer. Men who do not have an enlarged prostate, who have prostate cancer that is detected only in a single region of the prostate and have intermediate grade cancer can be a candidate for focal therapy. This type of therapy treats only the cancerous tissue and spares the normal prostate, thereby preserving urinary and sexual function
Here at UCLA we commonly use cryotherapy or HIFU to focally treat prostate cancer. Given that this is a relatively new form of treatment, we have established rigorous post-treatment protocols using MRI and biopsies to ensure that the cancer has been adequately treated.
You May Like: How To Reduce Prostate Cancer
Will Radiation Therapy Make Me Tired
Everyone have their own energy level, so radiation treatment will affect each person differently. Patients often feel fatigue after several weeks of treatment. For most patients, this fatigue is mild. However, a loss of energy may require some patients to change their daily routine.
If your doctor thinks you should limit your activity, they will discuss it with you.
To minimize fatigue while you are receiving radiation treatment:
- Be sure to get enough rest.
- Eat well-balanced, nutritious meals.
- Pace your activities and plan frequent rest periods.
Follow Your Healthcare Providers Instructions For Taking Aspirin
If you take aspirin or a medication that contains aspirin, you may need to change your dose or stop taking it 7 days before your procedure. Aspirin can cause bleeding.
Follow your healthcare providers instructions. Dont stop taking aspirin unless they tell you to. For more information, read the resource Common Medications Containing Aspirin, Other Nonsteroidal Anti-inflammatory Drugs , or Vitamin E.
Recommended Reading: Early Warnings Of Prostate Cancer
Prepare Your Nulytely Bowel Preparation Solution
On the morning of the day before your procedure, add lukewarm water to the NuLYTELY, filling it to the top of the line on the bottle. Add a flavor pack, if you choose. Use only a flavor pack that was provided with your NuLYTELY.
With the cap on, shake the NuLYTELY bottle until the powder is dissolved. The mixture will be clear, even if you used a flavor pack. If you prefer, you can place the bottle in the refrigerator to chill it. Many people have told us that NuLYTELY tastes better cold. Dont mix the NuLYTELY earlier than the morning before your procedure.
Complete A Health Care Proxy Form
If you havent already completed a Health Care Proxy form, we recommend you complete one now. If youve already completed one or have any other advance directives, bring them to your next appointment.
A health care proxy is a legal document that identifies the person who will speak for you if you cant communicate for yourself. The person you identify is called your health care agent.
Talk with your healthcare provider if youre interested in completing a health care proxy. You can also read the resources Advance Care Planning and How to Be a Health Care Agent for information about health care proxies, other advance directives, and being a health care agent.
Don’t Miss: After Effects Of Radiation For Prostate Cancer
Possible Side Effects Of Ebrt
Some of the side effects from EBRT are the same as those from surgery, while others are different.
Bowel problems: Radiation can irritate the rectum and cause a condition called radiation proctitis. This can lead to diarrhea, sometimes with blood in the stool, and rectal leakage. Most of these problems go away over time, but in rare cases normal bowel function does not return. To help lessen bowel problems, you may be told to follow a special diet during radiation therapy to help limit bowel movement during treatment. Sometimes a balloon-like device or gel is put between the rectum and the prostate before treatment to act like a spacer to lessen the amount of radiation that reaches the rectum.
Urinary problems: Radiation can irritate the bladder and lead to a condition called radiation cystitis. You might need to urinate more often, have a burning sensation while you urinate, and/or find blood in your urine. Urinary problems usually improve over time, but in some men they never go away.
Some men develop urinary incontinence after treatment, which means they cant control their urine or have leakage or dribbling. As described in the surgery section, there are different levels and types of incontinence. Overall, this side effect occurs less often with radiation therapy than after surgery. The risk is low at first, but it goes up each year for several years after treatment.
How Does External Beam Radiation Therapy Work
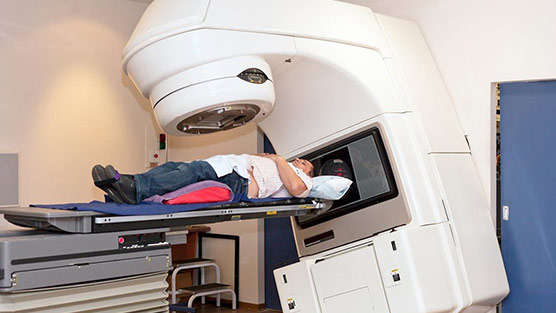
External beam radiation therapy, or EBRT, uses a machine to direct high-energy X-rays at the cancer in daily doses. The radiation beam is generated by a machine called a linear accelerator or LINAC. Using treatment planning computers and software, your treatment team controls the size and shape of the beam as well as how it is directed at your body to most effectively treat your tumor and minimize damage to surrounding normal tissue.
To minimize side effects, the treatments are typically given five days a week over a six-to-nine week period. The break in days allows the doctors to get enough radiation into the body to kill the cancer while giving healthy cells time to recover.
Watch our expert medical oncologist, Dr. Alicia Morgans from Vanderbilt-Ingram Cancer Center, discuss external beam radiation therapy:
Also Check: Gleason Score 7 Prostate Cancer Treatment Options