Radiation Dose Enough For Some Prostate Cancers
HealthDay Reporter
TUESDAY, April 30, 2019 — Treating men with low-risk prostate cancer with just one high dose of radiation may be safe and effective, British researchers report.
Therapy for prostate cancer typically involves low-dose radiation given over several days or weeks. Conversely, high-dose radiation is given once through a set of tiny tubes inserted directly into the tumor.
“For low-risk patients, a single dose of high-dose radiation is sufficient, but for medium- and high-risk patients, a single dose of 19 Gy isn’t enough. They will likely need a bigger dose or going back to multiple doses,” said lead researcher Hannah Tharmalingam. She’s a clinical research fellow at the Mount Vernon Cancer Centre in Northwood, England.
According to Tharmalingam, high-dose radiation could be more convenient for low-risk patients, and less time-consuming and costly for the medical system.
But one radiation oncologist fears that the side effects make it potentially dangerous.
For the study, Tharmalingam and her colleagues treated 441 prostate cancer patients between 2013 and 2018. The cancers were classified as low-, medium- or high-risk.
All of the men were treated with one high dose of 19 Gy of radiation, which is equivalent to the total amount of radiation given over several days with current treatments, Tharmalingam said.
In addition, 166 men were also given hormone therapy. None of the men, however, had surgery or chemotherapy.
Continued
Continued
Pagination
How Prostate Cancer Staging And Risk Stratification Affect Treatment Options
Your treatment choices are determined by several factors, including your cancers stage, aggressiveness and assigned risk stratification . Your age and current general health condition may also affect your choices.
Prostate cancer staging
Prostate cancer staging determines whether the cancer is confined to the prostate gland or whether theres evidence of metastasis, meaning its spread to other areas of the body.
Tools and methods to determine staging may include the prostate-specific antigen test, the digital rectal examination , the Gleason score and the American Joint Committee on Cancer TNM system, which provides information on the tumor, lymph node involvement and metastasis of a cancer. Imaging tests, such as a PET/CT scan, may also help determine your cancers stage.
The four stages of prostate cancer are subdivided into more precise categories, but we generally refer to three groups that indicate how far the cancer has spread:
Localized, meaning theres no indication that the cancer has spread beyond the prostate
Regional, meaning theres evidence of cancer cells in nearby lymph nodes or tissue
Distant, meaning theres evidence the cancer has spread to other organs or body parts farther from the prostate
Almost 90 percent of prostate cancers are diagnosed at the localized or regional stage. The five-year relative survival rate for men diagnosed with prostate cancer at these stages is nearly 100 percent.
Prostate cancer risk assessment
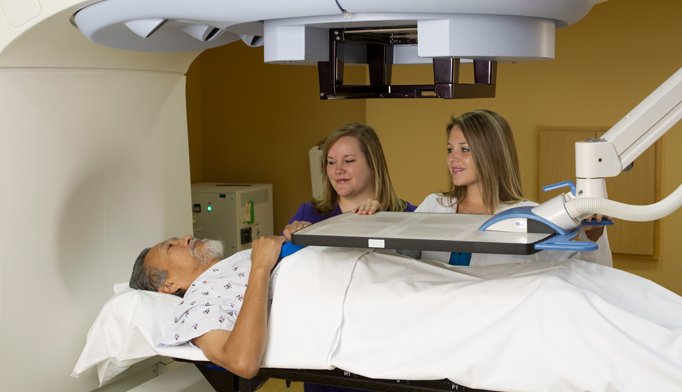
Meet Your Radiation Therapy Team
Your radiation therapy team is a group of healthcare providers. Their goal is to make your treatment as effective and comfortable as possible. This team includes:
Radiation Oncologist Dr. Selva is a radiation oncologist and medical director at the Reyna Cancer Center. He treats more prostate cancer patients than any radiation oncologist in the city. This incredible expertise helps you get the best results. As the radiation oncologist, he will:
- Lead the radiation therapy team
- Create your customized radiation therapy regimen, which includes the amount of radiation and how the treatment will be delivered.
- Closely monitor your progress throughout treatment.
- Direct any care needed if you experience side effects from radiation therapy.
Radiation Physicist The radiation physicist makes sure the machine that delivers radiation is working properly. The machine is a linear accelerator. It moves around you to deliver precise doses of radiation.
Radiation Nurse The radiation nurse will assist you through your treatment process and interact with the rest of your radiation team.
Radiation Therapist The radiation therapist works with you during each treatment. He or she will make sure you have the proper position for treatment. They will also operate the linear accelerator to deliver the radiation.
Dosimetrist The dosimetrist is a professional that calculates the proper radiation doses
Also Check: What Are Some Treatments For Prostate Cancer
Are There Side Effects Of The Combination Approach
There is a slightly higher chance that patients who receive the combined therapy will have rectal irritation or urinary side effects, both of which are common with any radiation treatment given to the prostate. But at MSK, we routinely use sophisticated planning techniques that help us reduce the dose given to normal tissues such as the rectum, bladder, and urethra, lessening the chances of side effects and complications.
In addition, at MSK, we routinely use a rectal spacer gel, which we inject between the prostate and the rectum while the patient is under mild anesthesia, to create a buffer between these two tissues. By creating this space, we can further reduce the dose of radiation that the rectum is exposed to. This leads to fewer side effects for the patient. The rectal spacer gel is biodegradable and after a few months dissolves on its own within the body, causing no harm or long-term effects.
Focal Therapy For Prostate Cancer
With recent advances in MRI and targeted biopsy, we are better able to locate the exact area of prostate cancer. Men who do not have an enlarged prostate, who have prostate cancer that is detected only in a single region of the prostate and have intermediate grade cancer can be a candidate for focal therapy. This type of therapy treats only the cancerous tissue and spares the normal prostate, thereby preserving urinary and sexual function
Here at UCLA we commonly use cryotherapy or HIFU to focally treat prostate cancer. Given that this is a relatively new form of treatment, we have established rigorous post-treatment protocols using MRI and biopsies to ensure that the cancer has been adequately treated.
Recommended Reading: Prevalence Of Prostate Cancer By Age
How Well It Works
Men with localized prostate cancer who have a low chance that their cancer will spread can choose active surveillance. One study compared active monitoring , surgery, and radiation in men who had localized prostate cancer and found that the risk of dying was very low and about the same, no matter what option men chose.footnote 3
Another study looked at men with low-risk localized prostate cancer and found that:footnote 4
- At 5 years, about 76 out of 100 men were untreated and still on active surveillance.
- At 10 years, about 64 out of 100 men were untreated and still on active surveillance.
- At 15 years, about 55 out of 100 men were untreated and still on active surveillance.
What The Research Shows About Radiation Vs Surgery
The ProtecT trial was a 10-year, randomized clinical study designed to compare radical prostatectomy, external-beam radiotherapy and active surveillance for the treatment of localized prostate cancer.
The results, published in 2016, showed that the rate of disease progression among men assigned to radiotherapy or radical prostatectomy was less than half the rate among men assigned to active monitoring. However, there was no significant difference in survival at the median 10-year mark for radiation therapy, surgery or active surveillance.
If youre interested in directly comparing treatment outcomes by treatment method and risk group , the Prostate Cancer Free Foundation provides an interactive graph on its website with information from data obtained from over 100,000 prostate cancer patients over a 15-year period.
As discussed earlier in the sections on the side effects of radiation therapy and surgery, the researchers conducting the ProtecT trial also looked at side effects and quality-of-life issues and found that the three major side effects of these two treatment options that affect quality of life after prostate cancer treatment are urinary incontinence, sexual dysfunction and bowel health.
The trial found that urinary leakage and erectile dysfunction were more common after surgery than after radiation therapy. Gastrointestinal bowel problems were more common after radiation therapy.
Read Also: How Do I Know If I Have Prostate Problems
A Biopsy Is Done To Diagnose Prostate Cancer And Find Out The Grade Of The Cancer
A transrectal biopsy is used to diagnose prostate cancer. A transrectal biopsy is the removal of tissue from the prostate by inserting a thin needle through the rectum and into the prostate. This procedure may be done using transrectal ultrasound or transrectal MRI to help guide where samples of tissue are taken from. A pathologist views the tissue under a microscope to look for cancer cells.
Sometimes a biopsy is done using a sample of tissue that was removed during a transurethral resection of the prostate to treat benign prostatic hyperplasia.
If cancer is found, the pathologist will give the cancer a grade. The grade of the cancer describes how abnormal the cancer cells look under a microscope and how quickly the cancer is likely to grow and spread. The grade of the cancer is called the Gleason score.
To give the cancer a grade, the pathologist checks the prostate tissue samples to see how much the tumor tissue is like the normal prostate tissue and to find the two main cell patterns. The primary pattern describes the most common tissue pattern, and the secondary pattern describes the next most common pattern. Each pattern is given a grade from 3 to 5, with grade 3 looking the most like normal prostate tissue and grade 5 looking the most abnormal. The two grades are then added to get a Gleason score.
Are There Any New Techniques Devices Or Trials In The Field That You’re Enthusiastic About
There are new radiation methods some of which weve adopted and some of which are still being tested. We now use a therapy called volumetric modulated arc therapy. It shapes the rays to conform to the shape of a tumor this allows us to be precise and quick with treatment. In the field, there is also growing interest in the hypofractionated radiation technique for prostate cancer, which means that you deliver more radiation in a given treatment but over fewer sessions. There are trials going on to compare the safety and efficacy of this type of treatment compared with standard. treatment
We are actively exploring new technologies that may reduce radiation-related side effects, be they better ways to track and adjust for prostate motion, or ways to reduce the dose of radiation that is delivered to the rectum and bladder.
Don’t Miss: Apple Cider Vinegar For Prostate
How Can I Reduce Skin Reactions
- Gently cleanse the treated area using lukewarm water and a mild soap such as Ivory, Dove, Neutrogena, Basis, Castile, or Aveeno Oatmeal Soap. Do not rub. Pat your skin dry with a soft towel or use a hair dryer on a cool setting.
- Try not to scratch or rub the treated area.
- Do not apply any ointment, cream, lotion, or powder to the treated area unless your radiation oncologist or nurse has prescribed it.
- Do not wear tight-fitting clothing or clothes made from harsh fabrics such as wool or corduroy. These fabrics can irritate the skin. Instead, choose clothes made from natural fibers such as cotton.
- Do not apply medical tape or bandages to the treated area.
- Do not expose the treated area to extreme heat or cold. Avoid using an electric heating pad, hot water bottle, or ice pack.
- Do not expose the treated area to direct sunlight, as sun exposure may intensify your skin reaction and lead to severe sunburn. Choose a sunscreen of SPF 30 or higher. Protect the treated area from direct sunlight even after your course of treatment is over.
Who Is Eligible For Radiation Therapy For Prostate Cancer
Since low-risk cancers can grow slowly, “when a patients cancer is small and not aggressive, we recommend observation instead of an immediate course of radiation,” says Dr. Yu.
Yale Medicine doctor also look at the patients overall health to decide whether he is a good candidate. “Someone with a connective tissue disease, such as lupus, scleroderma, dermatomyositis or an inflammatory bowel disease, such as ulcerative colitis or Crohns disease, is not a good candidate, because he can suffer an inflated reaction to the radiation,” says Dr. Yu.
Also Check: At What Age Do You Check For Prostate Cancer
How Does Hormone Therapy Work Against Prostate Cancer
Early in their development, prostate cancers need androgens to grow. Hormone therapies, which are treatments that decrease androgen levels or block androgen action, can inhibit the growth of such prostate cancers, which are therefore called castration sensitive, androgen dependent, or androgen sensitive.
Most prostate cancers eventually stop responding to hormone therapy and become castration resistant. That is, they continue to grow even when androgen levels in the body are extremely low or undetectable. In the past, these tumors were also called hormone resistant, androgen independent, or hormone refractory however, these terms are rarely used now because the tumors are not truly independent of androgens for their growth. In fact, some newer hormone therapies have become available that can be used to treat tumors that have become castration resistant.
The Grade Group And Psa Level Are Used To Stage Prostate Cancer
The stage of the cancer is based on the results of the staging and diagnostic tests, including the prostate-specific antigen test and the Grade Group. The tissue samples removed during the biopsy are used to find out the Gleason score. The Gleason score ranges from 2 to 10 and describes how different the cancer cells look from normal cells under a microscope and how likely it is that the tumor will spread. The lower the number, the more cancer cells look like normal cells and are likely to grow and spread slowly.
The Grade Group depends on the Gleason score. See the General Information section for more information about the Gleason score.
- Grade Group 1 is a Gleason score of 6 or less.
- Grade Group 2 or 3 is a Gleason score of 7.
- Grade Group 4 is a Gleason score 8.
- Grade Group 5 is a Gleason score of 9 or 10.
The PSA test measures the level of PSA in the blood. PSA is a substance made by the prostate that may be found in an increased amount in the blood of men who have prostate cancer.
Don’t Miss: How Is Prostate Removal Performed
Q: How Often Should I See My Doctor
Following EBRT, follow-up appointments with the doctor will help monitor the patients recovery and ensure any side effects are diminishing. The frequency of follow-ups will depend on the risk of cancer recurrence. PSA blood tests will start around the third month after treatment and are repeated every 3 to 4 months during the first 2 to 3 years and then every 6 months. Brachytherapy patients will have a CT scan of the prostate 3 to 4 weeks after the procedure. This scan will evaluate the quality of the implant.
What Types Of Hormone Therapy Are Used For Prostate Cancer
Hormone therapy for prostate cancer can block the production or use of androgens . Currently available treatments can do so in several ways:
- reducing androgen production by the testicles
- blocking the action of androgens throughout the body
- block androgen production throughout the body
Treatments that reduce androgen production by the testicles are the most commonly used hormone therapies for prostate cancer and the first type of hormone therapy that most men with prostate cancer receive. This form of hormone therapy includes:
Treatments that block the action of androgens in the body are typically used when ADT stops working. Such treatments include:
Treatments that block the production of androgens throughout the body include:
Also Check: How Is Prostate Test Done
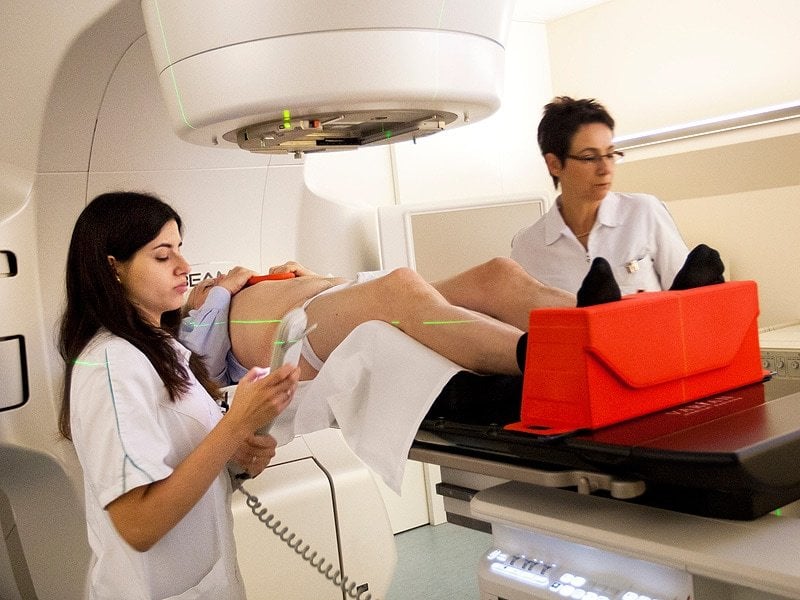
External Beam Radiation Therapy
In EBRT, beams of radiation are focused on the prostate gland from a machine outside the body. This type of radiation can be used to try to cure earlier stage cancers, or to help relieve symptoms such as bone pain if the cancer has spread to a specific area of bone.
You will usually go for treatment 5 days a week in an outpatient center for at least several weeks, depending on why the radiation is being given. Each treatment is much like getting an x-ray. The radiation is stronger than that used for an x-ray, but the procedure typically is painless. Each treatment lasts only a few minutes, although the setup time getting you into place for treatment takes longer.
Newer EBRT techniques focus the radiation more precisely on the tumor. This lets doctors give higher doses of radiation to the tumor while reducing the radiation exposure to nearby healthy tissues.
Remission And The Chance Of Recurrence
A remission is when cancer cannot be detected in the body and there are no symptoms. This may also be called having no evidence of disease or NED.
A remission can be temporary or permanent. This uncertainty causes many people to worry that the cancer will come back. Although there are treatments to help prevent a recurrence, such as hormonal therapy and radiation therapy, it is important to talk with your doctor about the possibility of the cancer returning. There are tools your doctor can use, called nomograms, to estimate someone’s risk of recurrence. Understanding your risk of recurrence and the treatment options may help you feel more prepared if the cancer does return. Learn more about coping with the fear of recurrence.
In general, following surgery or radiation therapy, the PSA level in the blood usually drops. If the PSA level starts to rise again, it may be a sign that the cancer has come back. If the cancer returns after the original treatment, it is called recurrent cancer.
When this occurs, a new cycle of testing will begin again to learn as much as possible about the recurrence, including where the recurrence is located. The cancer may come back in the prostate , in the tissues or lymph nodes near the prostate , or in another part of the body, such as the bones, lungs, or liver . Sometimes the doctor cannot find a tumor even though the PSA level has increased. This is known as a PSA-only or biochemical recurrence.
Don’t Miss: Can Prostate Cancer Come Back After Removal