What Are The Different Types Of Prostate Cancer Surgery
The most common one is called a radical prostatectomy. In this procedure, the entire prostate gland is removed, along with some of the surrounding tissue. In some cases, nearby lymph nodes are removed as well. There are several surgical approaches for this, including traditional open surgery. We can also use minimally invasive procedures, such as laparoscopic surgery and robot-assisted laparoscopic surgery.
A critical aspect of a radical prostatectomy is tailoring it to the individual features of each mans cancer. One size does not fit all. This means the exact same procedure is not appropriate for every person. The location, size, and other features of the cancer are considered to design an operation that is appropriate for the person.
In a laparoscopic radical prostatectomy, a surgeon inserts a tiny camera called a laparoscope through a small cut in the abdomen. The camera gives doctors a magnified, high-definition picture of the prostate gland. With that image as a guide, the surgeon can remove the prostate, seminal vesicles, and lymph nodes using special tools.
To do a robot-assisted procedure, a surgeon sits at a console that has a screen as well as hand, finger, and foot controls. The surgeons hand, wrist, finger, and foot movements control the robotic instruments inside the patient in real time.
How Radical Prostatectomy Affects A Relationship
A 2011 study of 63 men that had undergone a radical prostatectomy found that about 75 percent of them sought treatment for erectile dysfunction. Additionally, more than 50 percent reported having less sexual desire, and roughly an additional 40 percent were unable to have a satisfying orgasm.
The mental health effects of these symptoms were worse in highly sexually motivated participants. 52 percent reported that this had affected their self-esteem, and 36 percent said having performance anxiety.
Additionally, the last three items on the list above can be show-stoppers for a relationship. Few women can tolerate a high degree of urine leakage during sexual activity, and few men can handle the pain during intercourse.
What Treatments Are Available To Me If My Incontinence Doesnt Go Away After A Year
While kegels and behavioral therapy work well for most men with mild to moderate leaking, they may not be completely effective for some. Luckily, there are still some options for treating bladder leakage after prostate surgery.
Another surgery is sometimes needed when bladder leaks persist for more than a year after surgery. This may consist of having a urethral sling procedure, or an artificial urinary sphincter.
With a urethral sling procedure, a synthetic mesh tape is implanted to support the urethra. Up to an 80% improvement has been seen with this procedure and some men stop leaking completely.
An artificial urinary sphincter is used in patients who have more severe urinary incontinence that is not improving, or for those patients who may have had a lot of damage to the sphincter muscle after prostate surgery. An artificial urinary sphincter is a mechanical ring that helps close the exit from the bladder.
As will all surgeries, these come with pros and cons and potential complications. Be sure to discuss these options with your doctor.
Read Also: Is Testicular Cancer The Same As Prostate Cancer
Can I Have Sex During Treatment
There are a few factors that determine if sexual activity is safe during treatment.
- In general, sexual activity is fine during treatment as interest, energy, and comfort levels allow. While you may not feel up to sexual intimacy after surgeries or during chemotherapy and radiation hugging, kissing, holding hands, and massages may feel good and be comforting.
- If you had surgery involving the pelvic area , you may need to allow extra time for healing before having sex that involves penile stimulation or vaginal or rectal penetration . If you are being treated for oral cancer, use caution during oral sex.
- If you have a low white blood cell count or low platelet count , you may need to refrain from any sexual activity that involves vaginal or anal penetration. This is because there is an increased risk of infection or bleeding when your counts are low.
- If you have mouth sores , you should not perform oral sex.
- Do not have vaginal intercourse if you have open sores on your genitals.
- Do not have receptive anal sex if you have sores in the rectal area, rectal bleeding, or tears in the rectal tissue.
- If you received brachytherapy for prostate cancer , be sure to follow your oncology teams guidance about limiting close physical contact to avoid exposing your partner to radiation.
Loss Of Bladder Control

You may have some light dribbling or trouble controlling your bladder after a radical prostatectomy. This is known as urinary incontinence or urinary leakage. You may need to use a pad to manage urinary leakage for some days or weeks after the operation. Bladder control usually improves in a few weeks but it can take up to a year after the surgery. For about 5% of people, incontinence is ongoing and may need an operation to fix. In rare cases, incontinence may be permanent.
For help managing these problems, see Urinary problems.
Read Also: Does Enlarged Prostate Cause Constipation
Don’t Miss: Show Me A Picture Of A Man’s Prostate
Who Should Undergo Radical Prostatectomy
Men younger than age 75 with limited prostate cancer who are expected to live at least 10 more years tend to get the most benefit from radical prostatectomy.
Before performing radical prostatectomy, doctors first try to establish that the prostate cancer has not spread beyond the prostate. The statistical risk of spread can be determined from tables comparing the results of a biopsy and PSA levels. Further testing for spread, if needed, can include CT scans, bone scans, MRI scans, and ultrasound.
If it appears that the prostate cancer has not spread, a surgeon may first offer other options besides surgery. These can include radiation therapy, hormone therapy, or simply observing the prostate cancer over time, since many prostate cancers grow slowly. Depending on how high the risk of cancer spread, pelvic lymph node dissection may be considered, as well.
What Happens If Prostate Cancer Comes Back
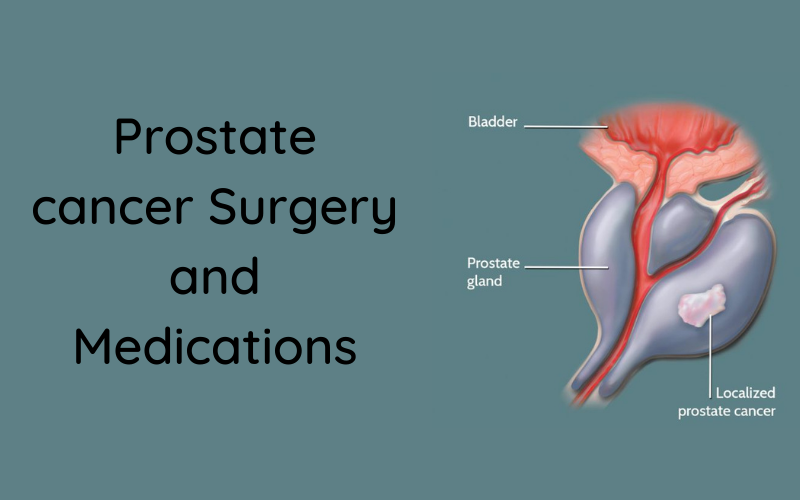
The prostate is a small gland about the size of a walnut that helps make seminal fluid. Its intertwined with your urinary tract system, resting below your bladder and surrounding the urethra. As you age, this gland continues to grow, sometimes resulting in benign prostatic hyperplasia. While this growth is normal, cancerous growth is not. Cancer occurs when the cells in your prostate gland begin to grow out of control.
While prostate cancer is common, especially among older men, its got a fairly positive outcome. When caught early and treated, most men survive and continue on with remission after five years. Unfortunately, for a small percentage of men, the cancer returns. To give you some clarity on this situation, heres what happens if prostate cancer comes back.
Recommended Reading: Perineural Invasion Meaning
You May Like: How Do They Remove The Prostate
Doctor Visits And Tests
Your doctor visits will usually include PSA blood tests, possibly with digital rectal exams if your prostate hasnt been removed. These will probably begin within a few months of finishing treatment. How often you need follow-up visits and tests might depend to some extent on the stage of your cancer and the chance of it coming back. Most doctors recommend PSA tests about every 6 months or so for the first 5 years after treatment, and at least yearly after that. Bone scans or other imaging tests might also be done, depending on your medical situation and symptoms.
Prostate cancer can recur even many years after treatment, which is why its important to keep regular doctor visits and report any new symptoms .
Prostatectomy: What To Expect
Many prostate cancer patients dont need surgery. But for young patients with prostate cancer that hasnt spread, a surgery called a prostatectomy can help them become cancer-free and put prostate cancer treatment behind them. John Davis, M.D., a urologist who performs hundreds of prostatectomies each year, explains what patients undergoing this procedure can expect, including prostatectomy side effects and risks.
What is a prostatectomy?
A prostatectomy is the surgical removal of all or part of the prostate gland. Prostate cancer surgery types include:
- Robotic prostate cancer surgery: In this procedure, called robotic radical prostatectomy, a surgeon makes several small incisions in the lower abdomen and uses a robotic device to remove the prostate.
- Open radical prostatectomy: The surgeon makes one large incision in the lower abdomen to remove the prostate.
Robotic radical prostatectomies have become increasingly common over the years, and most surgeons prefer to conduct the procedure this way because its a little easier on them. But its important to know that both methods are safe.
Who needs a prostatectomy?
For some patients, prostatectomies will be the only treatment they undergo. Others who may have a difficult time recovering from surgery or have more advanced cancer may also have chemotherapy or hormone therapy treatment as well.
How long does it take to recover from a prostatectomy?
What side effects do patients experience following prostate removal?
You May Like: What Medicine Is Good For Enlarged Prostate
Prostatectomy: What To Expect During Surgery And Recovery
If youve been diagnosed withprostate cancer, your doctor will consider many factors before recommending the besttreatment. For many men, that may mean a prostatectomy. In this surgery,doctors remove the entire prostate.
The Johns Hopkins Hospital performs more of these procedures than almostanywhere else in the world. One of the most common questions they hear frompatients: What should I expect after surgery?
Johns Hopkins urologistMohamad Allaf, M.D., explains the surgery and recovery.
What You Need To Know About The Prostate Removing The Prostate Due To Cancer
The main purpose of the prostate is to produce semen, a milky fluid that sperm swims in. During puberty, the body produces semen in a large number of cases, including enlarged prostate. This fluid causes the prostate to swell and cause a number of bladder-related symptoms. This is why the prostate is important to the body. It can be caused by many factors, including infection and inflammation.
A enlarged prostate can also cause blockages in the urethra. A blocked urethra can also damage the kidneys. A patient suffering from an enlargement of the prostate may have pain in his lower abdomen and genitals. If pain is present, a digital rectal examination will reveal hard areas. A doctor may prescribe surgery or perform an endoscopic procedure. If the enlarged prostate is not completely removed, it will shrink.
While the size of an enlarged prostate will influence the extent of urinary symptoms, men may experience a range of urinary symptoms. Some men have minimal or no symptoms at all. Some men will have a very enlarged prostate, whereas others will have a mild enlargement. Generally, the symptoms can stabilize over time. Some men may have an enlarged prostate but not notice it. If they have an enlarged colon, their physician can perform a TURP procedure.
Also Check: Most Common Symptoms Of Prostate Cancer
Where Does Prostate Cancer Spread
The most common place for prostate cancer to spread to is the bones. It can also spread to the lymph nodes, liver and lungs and other organs.
A large tumour in the prostate gland can spread into or press on areas around the prostate, such as the back passage or urethra. The urethra is the tube which carries urine from the bladder to the outside of the body.
You May Like: How To Reach Your Prostate
What Is The Recovery Time After Radical Prostatectomy
You may feel tired for a few weeks after surgery. Light exercise such as walking can help with the healing process. You should avoid heavy lifting for several weeks.
You may have urinary incontinence or leakage for weeks to months after the surgery, although most people recover continence after surgery. Recovery of sexual function is expected to take months. Your doctor may start you on a medication to help with recovery of erections.
Youll need regular follow-ups with your healthcare provider to monitor for evidence of cancer recurrence and manage effects from the surgery. They can work with you to improve any problems with erectile dysfunction or bladder control.
Recommended Reading: What Would Cause An Enlarged Prostate
What Will I Learn By Reading This
When you have treatment for your prostate cancer, you may have erectile dysfunction also known as impotence. Erectile dysfunction is a very common side effect . Side effects from prostate cancer treatment are different from one man to the next. They may also be different from one treatment to the next. Some men have no erectile dysfunction. The good news is that there are ways to deal with erectile dysfunction. In this booklet you will learn:
- What erectile dysfunction is
- Why prostate cancer treatment can cause erectile dysfunction
- What can be done about erectile dysfunction
- How erectile dysfunction may affect your sex life
- What your partner can expect
It is important for you to learn how to deal with erectile dysfunction so that you can continue to have a satisfying intimate relationship.
Recommended Reading: External Prostate Massage For Prostatitis
> > > This Simple Morning Test Will Fix Your Prostate
Another type of prostate issue is chronic prostatitis, or chronic pelvic pain syndrome. This condition causes pain in the lower back and groin area, and may cause urinary retention. Symptoms include leaking and discomfort. In severe cases, a catheter may be required to relieve the symptoms. If the problem is unresponsive to other treatments, your doctor may suggest a surgical procedure. If these do not work, your symptoms could progress and become chronic.
An acute bacterial infection can cause a burning sensation. Inflammation of the prostate can affect the bladder and result in discomfort and other symptoms. This is the most common urinary tract problem in men under 50, and the third most common in men over 65. The symptoms of acute bacterial prostatitis are similar to those of CPPS. Patients may experience a fever or chills as a result of the infection.
A bacterial infection can also lead to prostate issues. Acute bacterial infections can be hard to treat. Some men with a bacterial infection may need to take antibiotics to prevent or treat symptoms. Symptoms of the disease include fever and chills, pain in the lower back and the tip of the penis. Some men may have blood in the urine, frequent urination, and blood in the urine. If you suffer from acute bacterial prostatitis, a medical professional should be able to prescribe you the appropriate treatments to prevent the disease.
You May Like: Can Prostate Cancer Spread To Testicles
How Soon Can We Detect This
One of the main advantages of surgery over radiotherapy for prostate cancer is that following prostate removal, the PSA should be very low , which we can of course detect with blood tests. If metastasis occurs, because the metastatic cells originated in the prostate and therefore make PSA, the PSA level in the blood starts to rise. Once it has reached a given threshold additional or salvage treatment will be discussed.
A PSA level of more than 0.2 ng/ml defines biochemical recurrence. At this stage the cancer is still much too small to be seen on scanning. If it can be seen on a scan it is termed clinical recurrence, which generally does not occur until the PSA level is more than 0.5 ng/ml. Symptoms, such as bone pain, dont usually occur until the PSA is more than 20 ng/ml.
Life After Prostate Removal
Categories:Cancer Survivorship,Prostate Cancer,Survivorship & Side Effects
For many men with prostate cancer, prostate removal is never needed because the cancer is often slow-growing and managed with non-surgical treatments. But, if the cancer has grown beyond the prostate, the oncologist may recommend prostate removal surgery, also called a prostatectomy. If you are going to have prostate removal surgery, this information can help you in your discussion with the doctors.
Don’t Miss: How Painful Is A Biopsy Of The Prostate
Dry Orgasm And Infertility
Both the prostate and the glands responsible for semen production are removed during surgery, which is a common prostate cancer treatment. If you received this treatment, youd still be able to have an orgasm but youd no longer ejaculate.
This means that youll no longer be fertile. If you plan to have children in the future, you may consider banking your sperm before your surgery.
Prostate Surgery And Erectile Dysfunction
The short answer is yes prostate surgery is very likely to cause erectile dysfunction.
A prostatectomy, even though modern surgeries are nerve-sparing is likely to cause months of issues to a mans sex life.
Less invasive procedures that avoid the bundle of nerves and seminal vesicles next to the prostate will still likely cause ED, even if its a shorter-term issue.
Other surgeries are less likely to cause lasting damage, but the fact is that sexual dysfunction is a complicated issue. Men have to grapple with the mental side of it as well.
A cancer diagnosis can weigh heavily on a mans mind, which can impact both his sex drive as well as his ability to maintain an erection.
Theres also the fact that as we age, men experience a natural reduction in sex drive and are likely to be less able to get and maintain an erection.
The likelihood is that any surgery would just exacerbate the underlying issue.
Around 1 out of every 4 men over the age of sixty will experience some form of erectile dysfunction. Thats also the most likely group to undergo surgery, which is why the two are often linked, but not necessarily the sole cause.
If you have some pre-existing medical condition that impacts your floor muscles, sexual function or urine/ urinary function than you might find that the side effects of the surgery are more severe.
You should talk with your Urologist about any pre-existing medical conditions and how they might affect the treatment.
Read Also: What Supplements Are Good For Prostate Health