If Treatment Does Not Work
Recovery from cancer is not always possible. If the cancer cannot be cured or controlled, the disease may be called advanced or terminal.
This diagnosis is stressful, and for many people, advanced cancer may be difficult to discuss. However, it is important to have open and honest conversations with your health care team to express your feelings, preferences, and concerns. The health care team has special skills, experience, and knowledge to support patients and their families and is there to help. Making sure a person is physically comfortable, free from pain, and emotionally supported is extremely important.
People who have advanced cancer and who are expected to live less than 6 months may want to consider hospice care. Hospice care is designed to provide the best possible quality of life for people who are near the end of life. You and your family are encouraged to talk with the health care team about hospice care options, which include hospice care at home, a special hospice center, or other health care locations. Nursing care and special equipment, including a hospital bed, can make staying at home a workable option for many families. Learn more about advanced cancer care planning.
After the death of a loved one, many people need support to help them cope with the loss. Learn more about grief and loss.
Possible Side Effects Of Ebrt
Some of the side effects from EBRT are the same as those from surgery, while others are different.
Bowel problems: Radiation can irritate the rectum and cause a condition called radiation proctitis. This can lead to diarrhea, sometimes with blood in the stool, and rectal leakage. Most of these problems go away over time, but in rare cases normal bowel function does not return. To help lessen bowel problems, you may be told to follow a special diet during radiation therapy to help limit bowel movement during treatment. Sometimes a balloon-like device or gel is put between the rectum and the prostate before treatment to act like a spacer to lessen the amount of radiation that reaches the rectum.
Urinary problems: Radiation can irritate the bladder and lead to a condition called radiation cystitis. You might need to urinate more often, have a burning sensation while you urinate, and/or find blood in your urine. Urinary problems usually improve over time, but in some men they never go away.
Some men develop urinary incontinence after treatment, which means they cant control their urine or have leakage or dribbling. As described in the surgery section, there are different levels and types of incontinence. Overall, this side effect occurs less often with radiation therapy than after surgery. The risk is low at first, but it goes up each year for several years after treatment.
Radiation Dose Enough For Some Prostate Cancers
HealthDay Reporter
TUESDAY, April 30, 2019 — Treating men with low-risk prostate cancer with just one high dose of radiation may be safe and effective, British researchers report.
Therapy for prostate cancer typically involves low-dose radiation given over several days or weeks. Conversely, high-dose radiation is given once through a set of tiny tubes inserted directly into the tumor.
“For low-risk patients, a single dose of high-dose radiation is sufficient, but for medium- and high-risk patients, a single dose of 19 Gy isn’t enough. They will likely need a bigger dose or going back to multiple doses,” said lead researcher Hannah Tharmalingam. She’s a clinical research fellow at the Mount Vernon Cancer Centre in Northwood, England.
According to Tharmalingam, high-dose radiation could be more convenient for low-risk patients, and less time-consuming and costly for the medical system.
But one radiation oncologist fears that the side effects make it potentially dangerous.
For the study, Tharmalingam and her colleagues treated 441 prostate cancer patients between 2013 and 2018. The cancers were classified as low-, medium- or high-risk.
All of the men were treated with one high dose of 19 Gy of radiation, which is equivalent to the total amount of radiation given over several days with current treatments, Tharmalingam said.
In addition, 166 men were also given hormone therapy. None of the men, however, had surgery or chemotherapy.
Continued
Continued
Pagination
You May Like: Alternative Cures For Prostate Cancer
Lower Salvage Radiation Dose Are Outcomes The Same
A large randomized clinical trial, SAKK 09/10, found that a salvage radiation dose of 64 Gy over 32 treatments had equivalent biochemical outcomes compared to 70 Gy over 35 treatments.
They treated 350 patients from 2011 to 2014 at 28 hospitals in Germany, Switzerland, and Belgium. The patients were treated with either 3D-CRT or more modern radiation techniques. None had positive lymph nodes. Key patient characteristics were as follows:
- Biochemically recurrent after prostatectomy
- Positive margins in 45 percent
- Gleason score 8 in 18 percent
- No detectable tumors
After 6.2 years of follow-up, outcomes were as follows:
Oncological Outcomes
The stated purpose of SAKK 09/10 was to detect a difference in 6-year FFBP, and they detected no difference. But is that enough to change practice? The ICECAP working group cautions that 5-year metastasis-free survival, but not biochemical recurrence-free survival, is a good surrogate endpoint when overall survival would take too long to obtain in trials of primary therapy for localized prostate cancer. For trials of salvage therapy of recurrent prostate cancer after prostatectomy, some early analysis suggests that the 5-year occurrence of distant metastases may be a good surrogate endpoint. 6-year FFBP used in this trial is probably not a good surrogate endpoint.
There may be other ways to improve outcomes:
Radiation Therapy In Localized Disease:
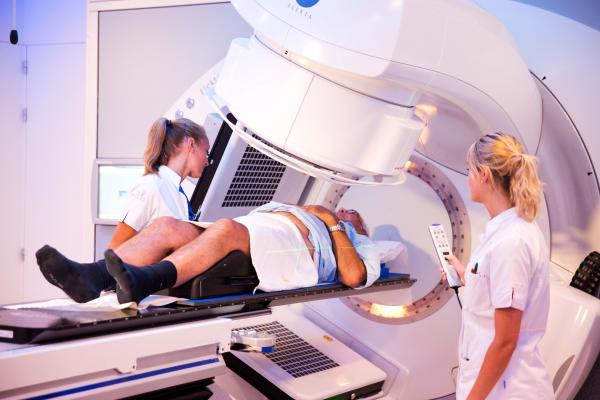
For men that need treatment for localized prostate cancer, external radiation therapy and brachytherapy can be alternatives to surgery. Modern radiation therapy is as effective as surgery when used to cure prostate cancer.
At this stage of disease, radiation therapy is used to attempt to cure the disease. However, it is also sometimes used if surgery didnt completely remove the cancer, or it came back in the area of the prostate after surgery.
These treatment options may require multiple visits. As always, it is important to consider costs and potential side effects. Scroll down to learn more about the different types of external radiation therapy or brachytherapy.
You May Like: Does Aspirin Help Enlarged Prostate
When Is Brachytherapy Alone The Right Choice
For a patient with disease that is confined to the prostate and not too aggressive, brachytherapy alone is a good option. With the use of sophisticated real-time computer-based planning, we can use brachytherapy to deliver radiation in an extraordinarily precise way, with minimal exposure to the surrounding normal tissues. It is also convenient for the patient as it is done in an outpatient setting and most people are able to get back to work the next day.
But brachytherapy is not right for everyone. For some patients with less-aggressive disease, a watch-and-wait approach would also be very reasonable. At MSK, our philosophy is that when the disease is caught very early meaning a low PSA level, or nonaggressive disease as reflected by a Gleason score of 6 with evidence of cancer in only a few of the biopsy samples and no evidence from the MRI of a significant amount of disease then it would be very appropriate to do active surveillance and hold off on treatment.
Side Effects Of Ebrt For Prostate Cancer
Many of the possible side effects of radiation therapy for prostate cancer involve the bladder and bowelthe prostate is very close to both. Although the goal is to target only the prostate with radiation, sometimes small amounts may cause problems to nearby areas of the body.
Some of the potential side effects from EBRT include:
- Bowel problems, including diarrhea, leakage or rectal bleeding
- Urinary symptoms, such as a need to urinate more frequently, incontinence or a burning sensation during urination
You May Like: Self Check Prostate Health Test
How Does Brachytherapy Work
Brachytherapy involves implanting small, permanent radioactive seeds or temporary needles into the cancerous prostate.
After you are identified as a good candidate for brachytherapy, an ultrasound is used to guide the placement of needles into the prostate. Depending on whether you and your doctor have chosen permanent/low-dose brachytherapy or temporary/high-dose brachytherapy, these needles are then used to either put in permanent seeds or temporary radiation sources.
Placement of seeds is a minimally invasive procedure and does not require incisions. Men undergoing the procedure can return to full activity in less than a week. This is done as an outpatient procedure before you begin treatment.
Side Effects Also A Concern
- Date:
- Washington University School of Medicine
- Summary:
- A new study shows that higher doses of radiation do not improve survival for many patients with prostate cancer, compared with the standard radiation treatment. The analysis included 104 radiation therapy oncology groups across North America.
A new study shows that higher doses of radiation do not improve survival for many patients with prostate cancer, compared with the standard radiation treatment. The analysis, which included 104 radiation therapy oncology groups across North America, was led by researchers at Washington University School of Medicine in St. Louis.
Past studies have shown that gradually escalating the radiation dose resulted in improved cancer control, such as slower tumor growth and lower levels of prostate-specific antigen , an indicator of cancer growth. The new study, published March 15 in JAMA Oncology, is the first that is large enough to examine whether these improved measurements translate into longer survival for patients.
While there was no difference in overall survival numbers, Michalski pointed out some differences in side effects and in whether further treatment was needed later. Such differences could help doctors and patients in deciding the best treatment course.
This work was supported by the National Institutes of Health , grant numbers U10CA180868, U10CA180822, U10CA37422, UG1CA189867, U24CA180803 and CA81647.
Story Source:
Recommended Reading: Prostate Cancer Lower Back Pain
What Happens To The Prostate After Radiation
The entire prostate gland is radiated when we treat the cancer. The prostate normally produces some of the fluid in the ejaculation. Radiation therapy has the side effect of damaging the glands in the prostate, so a lot less fluid is produced. The ejaculation may be dry or nearly dry. In addition, you will probably be sterile after radiation, but this is not 100% guaranteed and should not be relied upon as a form of birth control. You can still usually have erections because the nerves and blood vessels that go to the penis are not as damaged as the prostate gland.
The prostate gland will end up having a lot of scar tissue. It will shrink in size to about half its original weight within a couple years after finishing radiation. The urethra passes through the canter of the prostate gland like the hole of a doughnut. Sometimes this passage can widen, other times it can shrink after radiation. In summary, the prostate gland is heavily damaged from radiation and does not work normally afterwards.
Proton Beam Radiation Therapy
Proton beam therapy focuses beams of protons instead of x-rays on the cancer. Unlike x-rays, which release energy both before and after they hit their target, protons cause little damage to tissues they pass through and release their energy only after traveling a certain distance. This means that proton beam radiation can, in theory, deliver more radiation to the prostate while doing less damage to nearby normal tissues. Proton beam radiation can be aimed with techniques similar to 3D-CRT and IMRT.
Although in theory proton beam therapy might be more effective than using x-rays, so far studies have not shown if this is true. Right now, proton beam therapy is not widely available. The machines needed to make protons are very expensive, and they arent available in many centers in the United States. Proton beam radiation might not be covered by all insurance companies at this time.
You May Like: Bladder Recovery After Prostate Surgery
Shorter Course Of Post
After prostate cancer surgery, men can safely undergo fewer radiation treatments at higher doses, a new clinical trial shows.
Researchers found that the shorter regimen — given over five weeks, instead of seven — did not raise patients’ odds of lasting side effects.
Safety has been a “major concern” because when patients have fewer radiation treatments, the daily dose needs to be higher, explained Dr. Neha Vapiwala, a radiation oncologist who was not involved in the study.
But the new findings offer “level-one evidence” that a shorter course can be delivered safely, said Vapiwala, a professor at the University of Pennsylvania, in Philadelphia.
Prostate cancer is a highly treatable disease. In the United States, the 10-year survival rate stands at 98%, according to the American Society for Radiation Oncology. That means the impact of treatment choices on men’s quality of life is particularly critical.
A shorter course of radiation is obviously appealing for its convenience. The new study was designed to find out whether fewer treatments would come at the expense of lasting side effects.
According to lead researcher Dr. Mark Buyyounouski, “Preserving quality of life was a major priority when testing the shorter treatment course. It is important for patients to know that accepting a more convenient treatment doesn’t mean they have to compromise on quality of life.”
More information
Stereotactic Body Radiation Therapy Or Stereotactic Ablative Radiation Therapy
Guided by advanced imaging techniques, SBRT delivers large doses of radiation over a short period of time to a precise area. SBRT is commonly referred to by the names of the machines used to deliver the radiation. SBRT can offer some patients with localized prostate cancer the convenience of fewer treatments while maintaining treatment effectiveness and safety. SBRT may also be used to treat metastases for some patients to reduce tumor mass and potentially enhance survival.
You May Like: What Are The Chances Of Prostate Cancer Recurrence
Intensity Modulated Radiation Therapy
IMRT, an advanced form of 3D-CRT therapy, is the most common type of external beam radiation therapy for prostate cancer. It uses a computer-driven machine that moves around the patient as it delivers radiation. Along with shaping the beams and aiming them at the prostate from several angles, the intensity of the beams can be adjusted to limit the doses of radiation reaching nearby normal tissues. This lets doctors deliver an even higher radiation dose to the cancer.
Some newer radiation machines have imaging scanners built into them. This advance, known as image guided radiation therapy , lets the doctor take pictures of the prostate just before giving the radiation to make minor adjustments in aiming. This appears to help deliver the radiation even more precisely and results in fewer side effects.
A variation of IMRT is called volumetric modulated arc therapy . It uses a machine that delivers radiation quickly as it rotates once around the body. This allows each treatment to be given over just a few minutes. Although this can be more convenient for the patient, it hasnt yet been shown to be more effective than regular IMRT.
Treatment For Intermediate Risk Prostate Cancer
Intermediate risk prostate cancers are the most frequently treated prostate cancers. They are cancers that are confined to the prostate, often are Gleason 7 and have a PSA of less than 20. These cancers are treated in men with life expectancy greater than 10 years to prevent spread of the cancer in the long-term. There are a number of different effective treatment options for intermediate risk prostate cancer and the decision is often a personal one. Here at UCLA we recommend consultation with both Urologist and Radiation Oncologist to help men decide which treatment option is best for them.
You May Like: Gleason Score 7 Prostate Cancer Treatment Options
Your Role On Your Radiation Therapy Team
Youll have a team of healthcare providers working together to provide the right care for you. Youre part of the team, and your role includes:
- Arriving on time for your procedure.
- Asking questions and talking about your concerns.
- Telling someone on your radiation therapy team when you have side effects or pain.
- Caring for yourself at home.
- Quitting smoking, if you smoke. If you want to quit, call our Tobacco Treatment Program at .
- Drinking liquids as instructed.
Single Dose Of Targeted Radiotherapy Is Safe And Effective For Prostate Cancer
- Date:
- European Society for Radiotherapy and Oncology
- Summary:
- A single high dose of radiation that can be delivered directly to the tumor within a few minutes is a safe and effective technique for treating men with low-risk prostate cancer.
A single high dose of radiation that can be delivered directly to the tumour within a few minutes is a safe and effective technique for treating men with low risk prostate cancer, according to a study presented at the ESTRO 38 conference.
Radiotherapy traditionally involves a series of lower dose treatments that take place over several days or week. The new treatment is called high dose-rate brachytherapy and it delivers radiation via a set of tiny tubes.
Researchers say this technique could offer an effective treatment that is convenient for patients and brings potential time and cost savings for hospitals.
The research was presented by Dr Hannah Tharmalingam, a Clinical Research Fellow at Mount Vernon Cancer Centre, Northwood, and The Christie NHS Foundation Trust, Manchester, UK.
The research included 441 men with prostate cancer who were treated at one of seven UK hospitals between 2013 and 2018. Their cancers were classified, depending on how likely they were to spread, as either low risk , medium risk or high risk . All were treated with a single high dose of radiation 166 men also received hormone therapy but none had any surgery or chemotherapy.
Story Source:
Don’t Miss: Is There Any Cure For Prostate Cancer