What Is Prostate Seed Implantation
Prostate seed implantation is a type of radiation therapy that involves placing radioactive seeds into the prostate. PSI delivers a high dose of radiation to the prostate gland and sometimes the seminal vesicles, which lie on either side of the prostate gland.
Your doctors have decided that you are a candidate for PSI. Depending on the stage of your cancer, you may be treated with:
- Seed implant alone
- Seed implant with hormone ablation
- Seed implant and external beam radiation therapy with or without hormone ablation
The type of radioactive sources used in PSI come in the form of metallic seeds, about the size of a grain of rice. The number of seeds needed to treat your cancer is determined by the size of your prostate gland and the dose of radiation being used. Typically, between 70 and 150 seeds are placed at one time. The seeds give off their radiation slowly over several months. Within one year, the radioactivity can be considered gone however, the metallic seeds will remain in your prostate gland.
Brachytherapy Prostate Seed Implant
Patients who want to pursue brachytherapy as first line monotherapy, meaning alone and without other treatments, should exhibit these characteristics:
- PSA level 10 or lower
- DRE suggests no extension outside of prostate gland
- No history of benign prostatic hyperplasia
- Prostate gland volume below 60 grams or 60 cc
Not meeting all of these criteria, however, does not eliminate brachytherapy as a prostate cancer treatment option. Read on to see who else is opting for brachytherapy and why. Then speak with your doctor to see if brachytherapy is right for you.
Brachytherapy as Initial Monotherapy for Prostate Cancer Prostate cancer should be confined to the prostate for those considering interstitial radiation therapy. This treatment is most effective when the disease is confined within the cloud of radiation created by the radioactive pellets. In most patients, the cloud of radiation will extend about 5 mm outside the organ.
Patients who want to pursue brachytherapy as their primary treatment should have Gleason scores of 6 or less and PSA scores of 10 or less. They should also have prostate volumes which are below 60 grams or 66 cc. Those with benign prostatic hyperplasia are not candidates for prostate brachytherapy. The urinary side effects associated with brachytherapy are exacerbated if the patient already has BPH.
How Does Prostate Seed Implantation Work
Prostate seed implantation is a form of Low Dose Radiation brachytherapy. This means that the source of radiation is given in a low, continuous dose for a long amount of time.
Prostate seed implant diagram. Image courtesy of Cancer Research UK.
What to expect during prostate seed implantation:
- In most cases, prostate seed implantation is performed on an outpatient basis. In rare cases, you will be admitted to the hospital for the procedure.
- You will either be put under general anesthesia or have an epidural so you cannot feel anything below the waist.
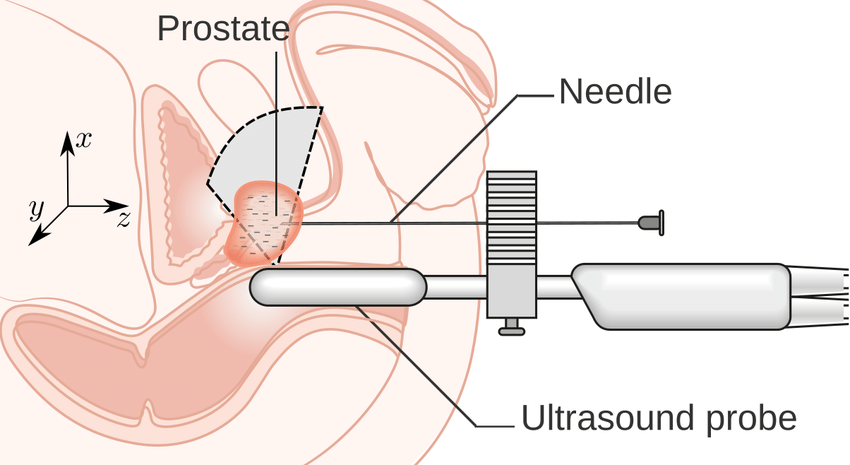
- The doctor will place an ultrasound probe into your back passage to help guide the placement of each individual seed.
- The doctor will then use a fine needle to insert between 80 120 radioactive seeds into your prostate gland.
- The seeds will give off radiation for the next several months before becoming inert.
- The seeds will not be removed after implantation.
After the procedure, you may be sleepy or feel some temporary tenderness. For outpatient procedures, you can generally go home after the anesthesia has worn off. For inpatient procedures, you may stay in the hospital for a day or until advised by your doctor.
You May Like: What Causes Prostate Psa Levels To Rise
A Brief History Of Prostate Treatment From Surgery To Radiation
Surgery has been the standard of care for prostate cancer for the past 150 years. Although effective, radical prostatectomies are invasive and not without complications. But then, shortly after the discovery of X-rays and radium at the turn of the last century, physicians began to explore how these modalities might improve survival and decrease potential side effects from the radical surgery. In 1917, Dr. Benjamin Barringer, chief of urology at what is now known as Memorial Sloan Kettering Hospital, espoused the use of radium needles for prostate cancer.
Initially, radioactive seed implantation was performed via free-hand technique, using direct visualization of the prostate to guide the radiation oncologist with seed placement. However, the results of this preliminary approach were hampered by suspect dose distribution in the prostate.
In 1987, Dr. John Blasko from Seattle described a reproducible system to implant radioactive iodine seeds in the prostate. This Seattle system employs a rectal ultrasound probe to directly visualize the prostate and a plastic template placed on the patients perineum . The template guides the placement of the needles that are loaded with radioactive seeds. This technique allows a reproducible, uniform dose distribution to the prostate.
At Princeton Radiation Oncology, our radiation oncologists have been performing the prostate seed procedure since 1997. We use the Seattle groups criteria for implant selection.
Where Does Sperm Go After Prostatectomy
You no longer ejaculate semen if you have had a radical prostatectomy. This is because the prostate gland and 2 glands called the seminal vesicles are removed. The seminal vesicles make the liquid part of the sperm. Your testicles will still make sperm cells but they will be reabsorbed back into your body.
Read Also: Prostate Cancer With Normal Psa
What Are The Results Of Radioactive Seed Implant Procedures
The success rate depends on the risk category of the prostate cancer and the type of success thats being measured. The most common measurement is related to prostate-specific antigen assessments after treatment. Grading is done with a system called the Gleason score. Using this method, the five-year success rates for the various risk groups are:
- Low-risk = 95%.
- Intermediate-risk = 90%.
- High-risk = 74%.
It is important to know that these numbers are heavily dependent on how frequently the PSA test is drawn after therapy. PSA tests should be done every six months after therapy. In reports of similar rates from other sources, one must make sure that the PSA tests are being drawn at least this frequently or a comparison cant be made.
Side Effects Are Part Of All Types Of Prostate Radiotherapy
A common misconception among prospective patients is that prostate implantation has fewer side effects than external beam radiation therapy. Nearly all patients suffer from some urethritis . Urinary retention requiring a temporary catheter occurs in 5% of patients.
To learn more about prostate seed implantation to treat prostate cancer, or to schedule a consultation, call . You can also reach us using our easy online form.
Also Check: Can Psa Test Detect Prostate Cancer
How Long Does The Brachytherapy Radiation Stay In The Body
After treatment, your body may give off a small amount of radiation for a short time. If the radiation is contained in a temporary implant, youll be asked to stay in the hospital and may have to limit your interactions with visitors. Pregnant women and children may not be allowed to visit you. Once the implant is removed, your body will no longer give off radiation.
Permanent implants give off small doses of radiation over a few weeks to months as they slowly stop giving off radiation. The radiation doesnt usually travel far, so the chance that others could be exposed to radiation is very small. Still, you may be asked to take precautions such as staying away from small children and pregnant women, especially right after treatment.
Intensity Modulated Radiation Therapy
IMRT, an advanced form of 3D-CRT therapy, is the most common type of external beam radiation therapy for prostate cancer. It uses a computer-driven machine that moves around the patient as it delivers radiation. Along with shaping the beams and aiming them at the prostate from several angles, the intensity of the beams can be adjusted to limit the doses of radiation reaching nearby normal tissues. This lets doctors deliver an even higher radiation dose to the cancer.
Some newer radiation machines have imaging scanners built into them. This advance, known as image guided radiation therapy , lets the doctor take pictures of the prostate just before giving the radiation to make minor adjustments in aiming. This appears to help deliver the radiation even more precisely and results in fewer side effects.
A variation of IMRT is called volumetric modulated arc therapy . It uses a machine that delivers radiation quickly as it rotates once around the body. This allows each treatment to be given over just a few minutes. Although this can be more convenient for the patient, it hasnt yet been shown to be more effective than regular IMRT.
You May Like: Should Prostate Cancer Be Treated
Why Choose Memorial Sloan Kettering For Brachytherapy
Memorial Sloan Kettering has long been a leader in brachytherapy, pioneering many advances in the field. In fact, MSK doctors were the first to use brachytherapy to treat cancers in the early 20th century.
That expertise continues today, as our medical physicists work with radiation oncologists to design the safest, most precise way to administer the brachytherapy using mathematical modeling and advanced computer programs. Through this collaboration, MSK specialists have developed highly specialized brachytherapy methods for specific diseases.
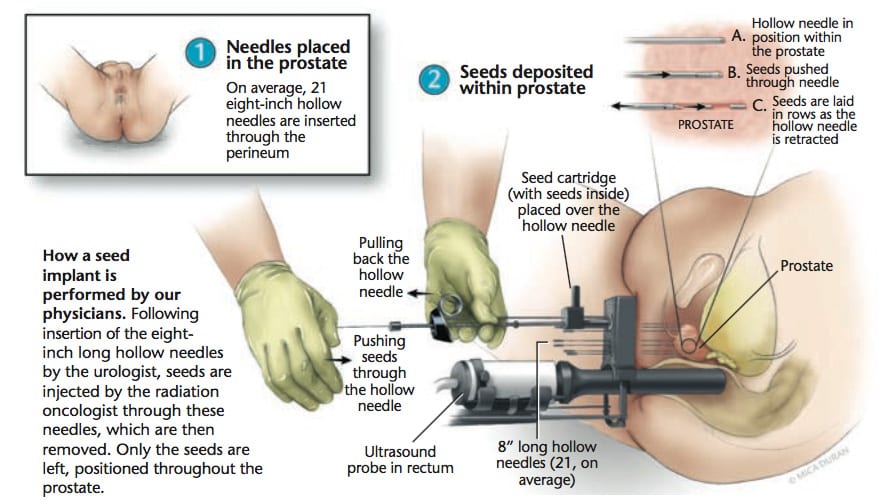
What Happens During The Procedure
The entire procedure takes approximately 90 minutes. Most patients go home the same day.
A radiation oncologist and urologist perform the procedure. Both physicians are actively involved in all aspects of the implantation, from the planning to the post-operative care. During the procedure, the urologist provides ultrasound guidance and the radiation oncologist places the radioactive seeds.
The procedure is performed as follows:
Recommended Reading: Show Me A Picture Of A Man’s Prostate
What Are The Benefits And Side Effects Of Prostate Seed Implantation
Unlike major surgery, daily radiation treatments, or external beam radiation therapy, seed implantation:
- Causes little interruption in your daily activities.
- Usually preserves continence.
- Less frequently causes erectile dysfunction.
The radiation can cause side effects, which may last for two to 12 months after the implant and will decrease gradually as the seeds lose their radioactivity.
Side effects, all of which are treatable, may include:
- Discomfort during urination
Proton Beam Radiation Therapy
Proton beam therapy focuses beams of protons instead of x-rays on the cancer. Unlike x-rays, which release energy both before and after they hit their target, protons cause little damage to tissues they pass through and release their energy only after traveling a certain distance. This means that proton beam radiation can, in theory, deliver more radiation to the prostate while doing less damage to nearby normal tissues. Proton beam radiation can be aimed with techniques similar to 3D-CRT and IMRT.
Although in theory proton beam therapy might be more effective than using x-rays, so far studies have not shown if this is true. Right now, proton beam therapy is not widely available. The machines needed to make protons are very expensive, and they arent available in many centers in the United States. Proton beam radiation might not be covered by all insurance companies at this time.
Recommended Reading: How Do You Keep Your Prostate Healthy
Case For Combined Treatment
For treatment to be effective in patients who have more aggressive or advanced stages of prostate cancer, it must be directed at both the prostate and the surrounding areas where cancer cells may have spread. To accomplish this, a seed implant is typically combined with a few weeks of IGRT and/or a temporary hormone blocking medicine.
The seed implant delivers a high dose of radiation to the prostate, where most or all of the cancer cells reside. The IGRT not only treats the cancer in the prostate, it also attacks cancer cells that may have spread outside the prostate.
How Is Hormone Therapy Used To Treat Hormone
Hormone therapy may be used in several ways to treat hormone-sensitive prostate cancer, including:
Early-stage prostate cancer with an intermediate or high risk of recurrence. Men with early-stage prostate cancer that has an intermediate or high risk of recurrence often receive hormone therapy before, during, and/or after radiation therapy, or after prostatectomy . Factors that are used to determine the risk of prostate cancer recurrence include the grade of the tumor , the extent to which the tumor has spread into surrounding tissue, and whether tumor cells are found in nearby lymph nodes during surgery.
The use of hormone therapy before prostatectomy has not been shown to be of benefit and is not a standard treatment. More intensive androgen blockade prior to prostatectomy is being studied in clinical trials.
Relapsed/recurrent prostate cancer. Hormone therapy used alone is the standard treatment for men who have a prostate cancer recurrence as documented by CT, MRI, or bone scan after treatment with radiation therapy or prostatectomy.
Hormone therapy is sometimes recommended for men who have a “biochemical” recurrencea rise in prostate-specific antigen level following primary local treatment with surgery or radiationespecially if the PSA level doubles in fewer than 3 months.
Don’t Miss: How To Heal Your Prostate
Who Is A Candidate For Prostate Seed Implantation At Princeton Radiation Oncology
Prostate seed implantation is not for everyone. Treatment decisions are based on important prognostic factors:
An ideal candidate should have a PSA level less than 10 and a Gleason grade 6 or less, with non-palpable disease. The size of the prostate is also an important factor. As a general rule, patients with prostate glands greater than 60cc are at increased risk for pelvic arch obstruction and poor dose distribution. Several months of androgen deprivation can be used to shrink large prostates to allow an optimal seed implant.
Patients whove previously had a vigorous transrectal resection of the prostate for benign prostatic hypertrophy may not be ideal candidates for this implant procedure. Higher rates of urinary complications have been reported for this subset of patients.
Will I Be Radioactive During Or After Internal Radiation Treatment
With internal radiation therapy, your body may give off a small amount of radiation for a short time.
If you have a temporary implant, youll be asked to stay in the hospital and might have to limit visitors during treatment. You also may be asked to stay a certain distance away from them. Pregnant women and children might not be allowed to visit you. Depending on the type of implant, once it is removed, your body will likely no longer give off radiation.
Over a few weeks to months, permanent implants will slowly stop giving off radiation. The radiation usually doesnt travel much farther than the area being treated, so the chances that others could be exposed to radiation is very small. Still, your health care team might ask you to take certain precautions such as staying away from small children and pregnant women, especially right after you get the implants.
Read Also: Prostate Cancer Types And Treatment
What Is Our Seed Implant Technique Why Is It So Important
To have optimal results from your prostate seed implant, it is essential that all areas of the prostate are covered with seeds, and that no sensitive areas outside the prostate are implanted. With our teams technique and experience, there is minimal risk of placement of needles or seeds too close to the bladder, rectum, urethra or nerves. Any motion of the prostate or change in its size or shape during the procedure can be immediately taken into account, ensuring perfect seed placement. Because seeds are precisely placed in the prostate, the risk of seeds migrating outside the prostate is less than 0.4%.
Radiation Therapy For Prostate Cancer
Radiation therapy uses high-energy rays or particles todestroy cancer cells. It is usually used to treat prostate cancer. Yourhealthcare team will consider your personal needs to plan the type and amountof radiation, and when and how it is given. You may also be given hormonetherapy together with radiation therapy.
Radiation therapy is given for different reasons. You mayhave radiation therapy to:
- destroy cancer cells in the body
- treat cancer that is not removed completely with surgery or that comesback after surgery
- relieve pain or control the symptoms of advanced prostate cancer
The following types of radiation therapy are most commonlyused to treat prostate cancer.
Read Also: Non Metastatic Castration Resistant Prostate Cancer
What Are Prostate Seed Implants
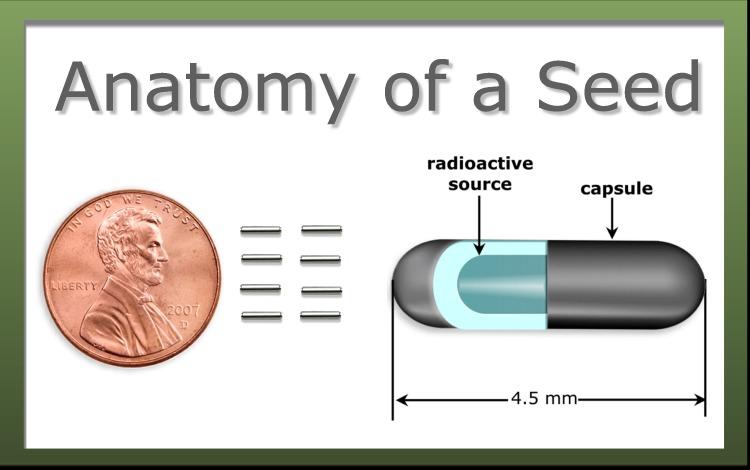
Seed size comparison. Image courtesy of the Nuclear Regulatory Commission .
Brachytherapy can be used to treat prostate cancer in the form of prostate seed implants. During this procedure, your doctor will place 80 120 small radioactive seeds into your prostate. This procedure may be performed on an inpatient or outpatient basis depending on the individual.
Over the next few months, the seeds release radiation into the prostate gland and shrink the tumor. The radiation from the seeds wears off over time, leaving the seeds inert. The seeds will not be removed following the procedure.
Brachytherapy may be used on its own or with another type of treatment.
How Will I Know That My Hormone Therapy Is Working
Doctors cannot predict how long hormone therapy will be effective in suppressing the growth of any individual mans prostate cancer. Therefore, men who take hormone therapy for more than a few months are regularly tested to determine the level of PSA in their blood. An increase in PSA level may indicate that a mans cancer has started growing again. A PSA level that continues to increase while hormone therapy is successfully keeping androgen levels extremely low is an indicator that a mans prostate cancer has become resistant to the hormone therapy that is currently being used.
Also Check: What Does Low Grade Prostate Cancer Mean
What Are The Side Effects Of Hormone Therapy For Prostate Cancer
Because androgens affect many other organs besides the prostate, ADT can have a wide range of side effects , including:
- loss of interest in sex
Studer UE, Whelan P, Albrecht W, et al. Immediate or deferred androgen deprivation for patients with prostate cancer not suitable for local treatment with curative intent: European Organisation for Research and Treatment of Cancer Trial 30891. Journal of Clinical Oncology 2006 24:18681876.
Zelefsky MJ, Eastham JA, Sartor AO. Castration-Resistant Prostate Cancer. In: Vincent T. DeVita J, Lawrence TS, Rosenberg SA, eds. DeVita, Hellman, and Rosenberg’s Cancer: Principles & Practice of Oncology, 9e. Philadelphia, PA: Lippincott Williams & Wilkins 2011.
Smith MR, Saad F, Chowdhury S, et al. Apalutamide and overall survival in prostate cancer. European Urology 2021 79:150158.