Top 5 Ingredients Of A Healthy Diet During Radiation Cancer Therapy
Radiation therapy is a type of cancer treatment that shrinks and destroys cancer cells. During radiation, its important to eat well. This keeps the body and its immune system strong, giving it the nutrients it needs to promote the regrowth of healthy tissues. Eating well during radiation also maintains energy, helps patients tolerate radiation side effects, lowers risks of infection, and speeds up recovery.
However, the nutrients and foods a person needs during cancer treatment vary based on the individual, how their body responds to radiation, the treatment area, and the length of treatment. While there is no one-size-fits-all radiation diet, there are some guidelines and tips that can help you find the best one during your cancer treatment.
Contents
Overview Of Radiation For Prostate Cancer
Radiation therapy has the same cure rate as surgery for prostate cancer that’s localized and locally advanced . This treatment uses high-intensity ionizing radiation, such as X-rays and gamma rays, to strategically pinpoint and destroy cancer cells.
Ionizing radiation is a kind of energy that can pass through living tissue. Low levels of ionizing radiation are used in medical tests such as X-rays and computed tomography scans. Radiation therapy for cancer differs from these common tests in intensity and frequency of use.
Radiation can be used to target cancer cells from outside the body. This technique is called external beam radiation.
Radiation can also be deposited internally in the form of seeds that are placed strategically in the prostate gland. This technique is called brachytherapy . You may be given one or both types of radiation during treatment.
Radiation therapy of either type may be used alone or in conjunction with other treatments. These treatments include surgery and hormone therapy called androgen deprivation therapy, in which levels of hormones that can stimulate the tumor are reduced.
In some instances, the Gleason score may be used as a tool to determine which treatments will be most effective for you. The Gleason score is a diagnostic tool that can help predict the aggressiveness of prostate cancer.
Your doctor may recommend radiation therapy at various stages of treatment, such as:
Incidence Of Seed Migration
We found that 0.36% of implanted seeds migrated to the chest in 20% of our patient population, similar to previous reports . It has been reported that the incidence of seed migration to the chest can be as high as 55% per patient population and 0.98% per number of implanted seeds . The variability of the incidence of seed migration to the chest among the reported results is considered to be attributed to different types of seeds , different designs of seed placement , different timings of follow-up radiographs, and different protocols of follow-up chest radiographs .
Table 2 Literature Survey of Seed Migration
In contrast, the incidence of seed migration to the abdomen and pelvis has been reported rarely . A possible reason is that the American Brachytherapy Society does not specifically recommend follow-up abdominal and pelvic radiographs after seed implantation . Therefore, in most institutions, follow-up abdominal and pelvic radiographs would not be undertaken routinely. However, we found that seed migration to the abdomen and pelvis occurred in 2.2% and 5.6%, respectively, of our patient population. Although the incidence of seed migration to the abdomen and pelvis is lower than that of seed migration to the chest, we would consider it advisable to undertake follow-up abdominal and pelvic radiographs after seed implantation.
Read Also: Latest News On Prostate Health
How Much Does Prostate Cancer Surgery Typically Cost
Prostate cancer surgery and care costs vary widely. Your costs can be influenced by:
-
Your insurance status
-
Your insurance coverage
Commonly, prostate cancer surgery involves a prostatectomy, which is a procedure to remove the prostate. A radical prostatectomy removes the gland and surrounding tissue.
Charges for a radical prostatectomy include:
-
Hospital fees, which comprise the majority of costs
-
Surgeon and anesthesiologist fees
According to a 2021 publication in the National Institute of Healths PubMed Central, the average list prices for a radical prostatectomy include:
-
An average $34,720 for hospital fees, with a range from $10,000 to $135,000.
-
An average $8,000 for physician fees, with a range from $4,028 to $18,720.
What Happens Before Radiation Therapy Treatment
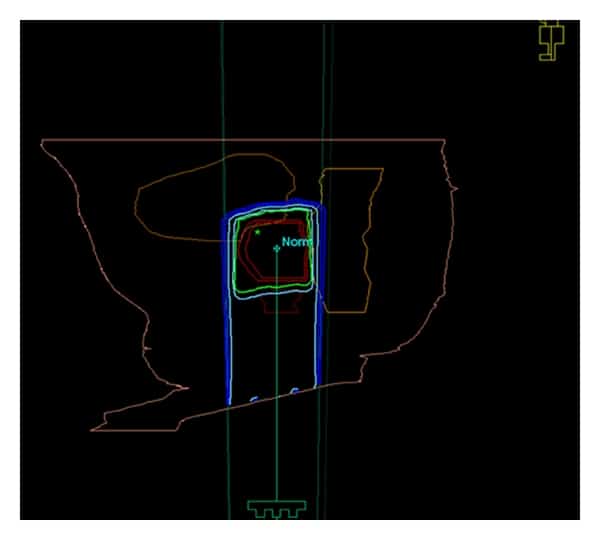
Each treatment plan is created to meet a patientâs individual needs, but there are some general steps. You can expect these steps before beginning treatment:
Meeting with your radiation oncologist. The doctor will review your medical records, perform a physical exam, and recommend tests. You will also learn about the potential risks and benefits of radiation therapy. This is a great time to ask any questions or share concerns you may have.
Giving permission for radiation therapy. If you choose to receive radiation therapy, your health care team will ask you to sign an âinformed consentâ form. Signing the document means:
-
Your team gave you information about your treatment options.
-
You choose to have radiation therapy.
-
You give permission for the health care professionals to deliver the treatment.
-
You understand the treatment is not guaranteed to give the intended results.
Simulating and planning treatment. Your first radiation therapy session is a simulation. This means it is a practice run without giving radiation therapy. Your team will use imaging scans to identify the tumor location. These may include:
Depending on the area being treated, you may receive a small mark on your skin. This will help your team aim the radiation beam at the tumor.
You may also be fitted for an immobilization device. This could include using:
Recommended Reading: Diagnostic Procedures For Prostate Cancer
Recommended Reading: Natural Ways To Reduce Prostate Swelling
Side Effects Of Radiation Therapy
Compared to earlier radiation methods, these modern techniques reduce the chance of urinary and bowel problems.
With several treatment options available, your doctor will work with you to develop and oversee a treatment plan that precisely addresses your prostate cancer while minimizing the risk to surrounding tissues.
This is why it is important to choose an experienced radiation oncologist who specializes in the management of prostate cancer. High volume centers where practitioners have significant experience and treat large numbers of patients with prostate cancer may be associated with good outcomes and fewer lasting problems related to treatment. The majority of patients who undergo radiation do not have permanent effects on bowel or urinary function, and patients who develop erectile difficulty after these therapies can often be treated successfully with medications such as sildenafil or tadalafil.
What Is The Experience Like For A Patient
The experience with our department begins with a consultation.
If you agree to receive radiation, you will have a noncontrast computed tomography scan to map your prostate and internal anatomy.
Next, we design a radiation treatment plan.
Youâll come in for daily radiotherapy sessions, each lasting about 15 minutes. Youâll check in, change into disposable shorts and wait in a men-only waiting area.
Yale Medicine radiation therapists then escort you to the treatment room, where youâll lie down in a custom body mold.
When your positioning is confirmed and adjusted, based on a CT scan or an implanted radio-frequency tracking device, treatment begins.
Men should be in and out of our department like clockwork, with minimal disruption to their day, says Dr. Yu. Radiation therapy may continue for up to nine weeks.
Once the course is complete, recovery typically requires a few months. Typically, at their one-month follow-up visit, patients report they are on the mend, says Dr. Yu.
Also Check: Are Colon Cancer And Prostate Cancer Related
What Is A Radiation Oncologist
If a patient is undergoing radiation, the cancer treatment plan may be managed by a radiation oncologist who carefully monitors the persons overall health and well-being through the process.
With advanced cancer, a patient may also be referred to a medical oncologist. This specialized doctor uses medicines such as chemotherapy and hormone therapy to treat cancers. Its common for several medical specialists to work together on a treatment plantheyre known as a cancer care team.
Diarrhea Flatulence Or Painful Defecation
These symptoms usually occur after the second or third week of treatment. Symptoms will resolve after the treatment ends. During radiation, dietary modification usually helps reduce the frequency and severity of diarrhea. Try to avoid or reduce fried foods, greasy foods and highly spiced foods. Reduce foods with insoluble fiber, such as lettuce and cauliflower, and increase low-fiber and soluable-fiber foods, such as bananas, mashed potatoes, applesauce, white rice, canned or cooked fruits and vegetables.
Maintain your intake of lean proteins, such as turkey, chicken and fish, and increase your fluid intake to avoid dehydration. Using moist toilet paper, baby wipes or sitz baths may help relieve rectal irritation. Your doctor may recommend anti-diarrheal medications. Contact your doctor if you see blood in your stool, if the diarrhea worsens or if you become light-headed or dizzy.
Don’t Miss: Side Effects Of Having Prostate Removed
Economic Analysis Of Various Radiotherapy Treatment Delivery Methods
Treatment techniques have evolved over the course of many years as a result of the technologic advancement. Improvements in treatment planning software as well as linear accelerators have allowed treatment techniques to transition from 2-dimensional treatment plans and techniques to 3-dimenesional treatment plans and then to IMRT. The increased work necessary for physicians, dosimetrists, and physicists needed to design and perform quality assurance resulted in increased reimbursement, both on the professional and technical sides. The development and implementation of IMRT was made possible by the further improvements in treatment planning software and linear accelerators, with the advent of multi-leaf collimators. IMRT treatment techniques, as reported elsewhere in this issue, made it possible to escalate the delivered radiotherapy dose while reducing both acute and late toxicity. The increased in delivered radiotherapy dose resulted in higher biochemical disease-free survival . IMRT was rapidly adopted as the standard of care in the treatment of prostate cancer because of these results without randomized clinical trials comparing IMRT to 3D conformal radiotherapy . Reimbursements for IMRT, however, were considerable higher when compared to 3DCRT dramatically increasing the overall cost of care for prostate cancer. Economic analyses using decision models were performed to provide evidence of cost-effectiveness of IMRT compared to 3DCRT.
Side Effects Of External Beam Radiation Therapy
Each type of external beam radiation therapy causes similar side effects. Some are temporary or self-resolving, but others may be long-lasting or permanent. In some instances, erectile dysfunction may start to occur several months after your treatment is complete.
Short-term side effects may include:
- Urinary symptoms such as urgency, needing to urinate often at night, and a weaker urine stream
- Loose bowel movements
- Redness or bruising at the radiation site
Long-term side effects may include:
- Erectile dysfunction, including difficulty getting and maintaining an erection hard enough for penetration
- Urinary dysfunction, including incontinence
- Rectal inflammation
You may be able to reduce your risk of some long-term side effects before beginning therapy. Before starting radiation, talk to your doctor about using a hydrogel spacer during treatments. This technique reduces exposure of healthy rectal tissue to radiation.
Your surgeon will insert hydrogel in the space between the prostate and rectum, increasing the distance between the rectum and the radiation beam. This technique may help you to avoid proctitis.
Erectile dysfunction affects most prostate cancer patients who have radiation, at least temporarily. When the nerves are left intact, this side effect usually improves.
Talk to your doctor about vessel-sparing radiation, which may preserve erectile function more effectively than some other forms, including standard external beam radiation.
Read Also: How Long Does Prostate Cancer Surgery Take
What Happens On Treatment Days
External radiation therapy requires regular sessions during a period of about five to eight weeks. For each treatment, the radiation therapist will help you onto the treatment table and into the correct position. Once the therapist is sure you are positioned well, they will leave the room and start the radiation treatment.
You will be under constant observation during the treatment. Cameras and an intercom are in the treatment room, so the therapist can always see and hear you. Be sure to remain still and relaxed during treatment. Let the therapist know if you have any problems or discomfort.
The therapist will be in and out of the room to reposition the machine and change your position. The treatment machine will not touch you, and you will feel nothing during the treatment. Once the treatment is complete, the therapist will help you off the treatment table.
The radiation therapist will take a port film, also known as an X-ray, on the first day of treatment and about every week thereafter. Port films verify that you are being positioned accurately during your treatments.
Port films do not provide diagnostic information, so radiation therapists cannot learn about your progress from these films. However, port films are important to help the therapists make sure the radiation is delivered to the precise area that needs treatment.
Also Check: Early Detection Of Prostate Cancer Can Be Done Through
What Symptoms Should I Look Out For
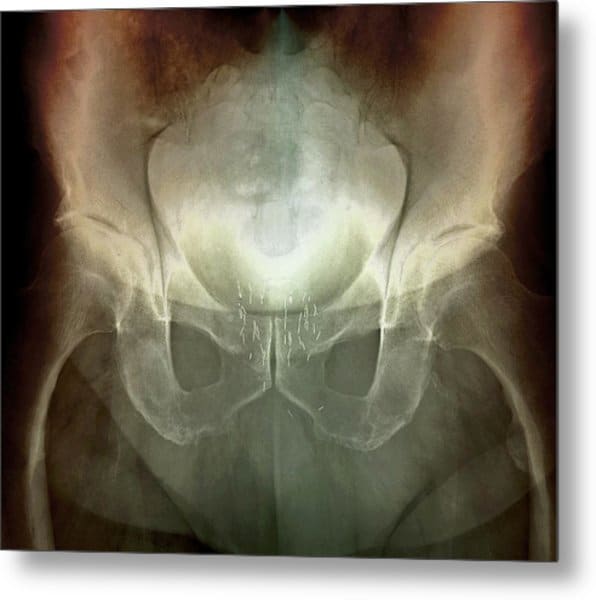
If your cancer does come back, the first sign is likely to be a rise in your PSA level, rather than any symptoms. And problems will often be side effects of treatment rather than a sign that your cancer has come back.
However, its important to let your doctor or nurse know if you do get any new symptoms or side effects, or are worried that your cancer might have come back. If your cancer has come back and has spread from the prostate to other parts of the body, it can cause symptoms, such as extreme tiredness â rel=ânofollowâ> fatigue), bone pain and problems urinating.
Your doctor or nurse can help find out what might be causing your symptoms and help you manage any side effects. They can also look at your PSA level and do other tests to see whether or not your cancer might have come back.
What other tests might I have?
If your doctor or nurse is concerned about your PSA level or if you have new symptoms that suggest your cancer might have come back, they may recommend that you have some other tests, such as a prostate biopsy, MRI scan, CT scan, bone scan or PET scan.
Your doctor or nurse will explain these tests to you if you need them, or you can get in touch with our Specialist Nurses for more information.
Also Check: Prostate Cancer And Radiotherapy Treatment
Whos Eligible For This Procedure
Permanent implants are relatively low-energy sources, and therefore have limited tissue penetration. A well-done implant treats the prostate and the surrounding few millimeters of adjacent tissue.
The best candidates for this procedure are patients with a cancer within or near the prostate. Patients with prostate cancer thats invading nearby structures like the bladder or rectum arent appropriate for this technique.
Original Medicare Covers Chemotherapy And Cancer Treatments
Medicare Part A and Part B make up Original Medicare, which covers some hospital and medical care needs.
Medicare Part B covers doctor visits, surgeries and outpatient hospital services, including chemotherapy. Medicare Part A provides coverage for inpatient hospital care.
How Medicare pays for chemotherapy depends on where you receive your treatment:
- Hospital outpatientYou will typically pay a Medicare Part B copayment for chemotherapy received in a hospital outpatient setting. Your copay will typically be a set dollar amount, rather than a percentage of costs.
- Doctors office or freestanding clinicAfter meeting your Part B deductible , youre typically responsible for paying 20% of the Medicare-approved amount for the treatment.
Original Medicare can also provide coverage for the following cancer treatment and screening services:
- Prostate cancer screenings
Don’t Miss: When To Get A Prostate Exam
Online Support Groups For Prostate Cancer
- Us TOO. This organization has more than 200 support groups in the United States and abroad.
- Prostate Cancer Research Institute. This website allows you to search for support groups by state.
- Cancer Care. This site offers 15-week online support groups for people diagnosed with prostate cancer. Co-sponsored by the National Alliance of State Prostate Cancer Coalitions.
- Male Care. This organization offers online support groups for people with prostate cancer and their partners or caregivers.
- Imerman Angels. This support community offers one-on-one support with a mentor.
Neoadjuvant And Adjuvant Hormone Therapy For Early
Hormone therapy is sometimes given in conjunction with a definitive prostate cancer treatment, such as radiation therapy, in order to improve health outcomes. When hormone therapy is given in advance of a primary treatment, its known as neoadjuvant therapy when its given during or after a primary treatment, its known as adjuvant therapy.
Also Check: How Do You Treat An Enlarged Prostate
Remove Devices From Your Skin
If you wear any of the following devices on your skin, the manufacturer recommends you remove it before your simulation or treatment:
- Continuous glucose monitor
Talk with your radiation oncologist about whether you may need to remove your device before your simulation or treatment. Make sure you have an extra device with you to put on after your simulation or treatment.
If youre not sure how to manage your glucose while your device is off, talk with the healthcare provider who manages your diabetes care before your appointment.
Prices And Where To Get It
The cost of a radical prostatectomy varies depending on insurance status and location of surgery.
Costs may include hospital fees, anesthesia fees, and surgeon fees. The average cost of hospital fees for prostatectomy in the United States is about $34,000. Anesthesiologist and surgeon fees average about $8,000. What out-of-pocket expenses the person being treated incurs will depend on their insurance.
The location of the procedure can be with a local surgeon, or the person being treated may travel to see a regional or national expert.
Recommended Reading: What Are The Side Effects Of Having Prostate Removed