I Am A Uk Resident Living In One Of The Devolved Administrations Can I Receive Nhs Funded Proton Beam Therapy At The Christie
The NHS in England is a residence-based system, unlike many other countries, which have insurance-based healthcare systems. This means that visitors to England may have to pay for NHS healthcare, depending on their circumstances.
The devolved administrations, Scotland, Wales and Northern Ireland can access proton beam therapy at The Christie if the respective administrations approve it.
Further information can be found at NHS Choices.
Comparative Studies Of Patient
A few retrospective comparisons have been published evaluating toxicity and patient-reported QOL for patients treated with photon or proton beam radiation. The results have been mixed with some studies finding that PT reduces the risk for acute side effects of radiation therapy, as well as bowel frequency and urgency in comparison to photon based radiation, while other studies suggest that PT yields equivalent or worse outcomes. For example, Gray et al. evaluated 3-dimensional conformal photon radiation, IMRT, and PT using prospectively collected patient-reported QOL data . In the first 3 months of follow-up, the authors reported worse patient-reported QOL in the bowel/rectal, urinary irritative/obstruction, and incontinence domains for patients treated with 3D conformal radiotherapy and IMRT when compared to patients treated with PT however, by 12 and 24 months of follow-up, no significant differences in patient-reported QOL were seen among the three groups.
Advantages Of Proton Therapy For Prostate Cancer
Proton therapy has proven to show remarkable promise and advantages over conventional therapy-especially in the treatment of prostate cancer. Proton radiation therapys accuracy and the control it gives physicians in terms of adapting treatment make it a non-invasive and low-risk option for prostate cancer treatment.
Also Check: How Long Does A Prostate Biopsy Take
Proton Therapy Treatment For Prostate Cancer Patients
Proton therapy is a form of radiation treatment for cancer patients. Also called proton beam therapy, proton therapy involves focusing proton particles into a beam, which is then delivered to the cancer cells in a non-surgical procedure. The positively charged particles can be controlled to stop at the tumor site, enabling the cancerous tissues to be destroyed with high levels of radiation without causing damage to nearby healthy tissue and vital organs. Proton therapy is considered more precise than other types of radiation therapy. It is also non-surgical, non-invasive, and has minimal side effects. Proton therapy treatment requires little to no recovery time, and the radiation has very little impact on a patients energy level compared to other cancer treatment options.
Proton therapy exhibits higher success rates in prostate cancer patients.
According to a study published by the University of Florida, prostate cancer patients who received proton therapy treatment were found to be free of cancer progression for five years after their treatment. Patients with low to medium risk prostate cancer experienced a success rate of 99%, while those with high risk prostate cancer experienced a success rate of 76%.
You May Like: Where Is The Prostate Cancer
Pencil Beam Scanning Proton Therapy
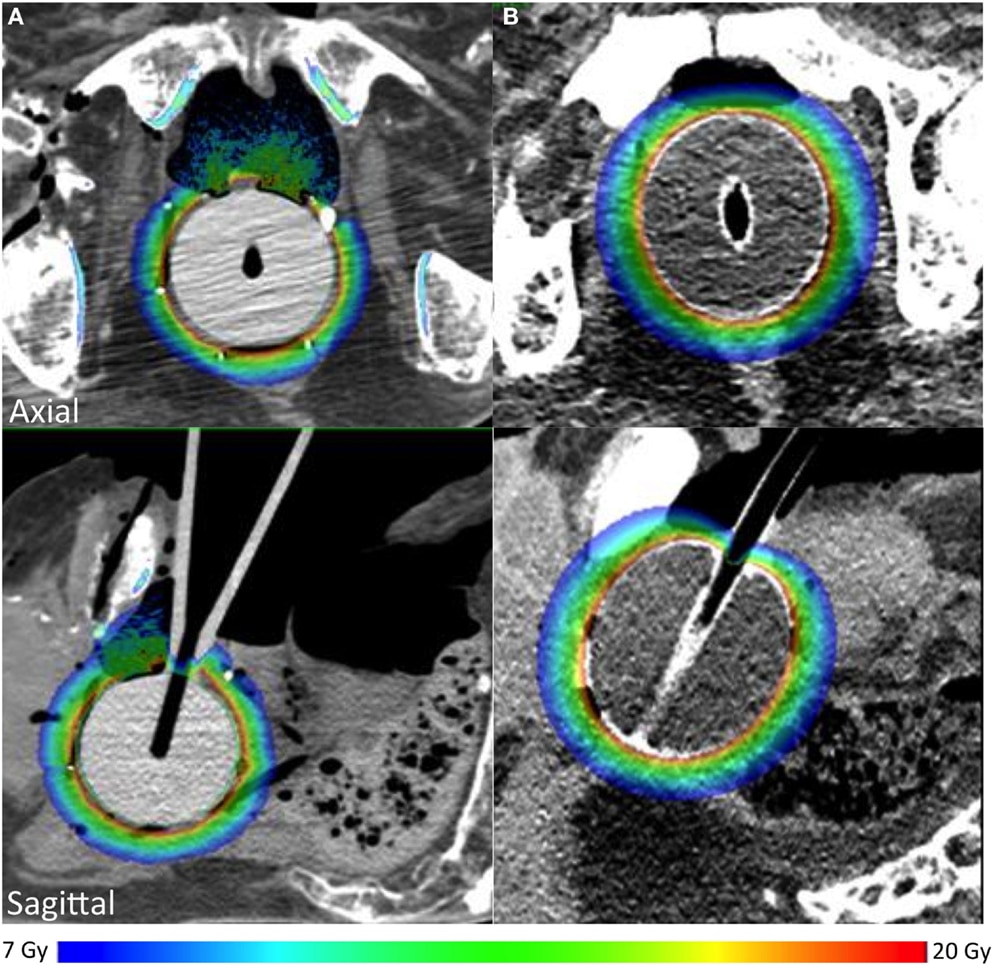
Pencil beam scanning is one of the most common ways to deliver proton therapy for prostate cancer. Another common method is double-scattered beam therapy.
With pencil beam scanning proton therapy, medical professionals are able to manipulate and focus the proton beams to a greater extent. This results in a more precise dose of radiation than double-scattered therapy, sparing surrounding tissue even more.
However, the difference in outcomes is minimal, according to
Side effects may include fatigue and skin redness or soreness where you had treatment. You may also have issues with incontinence or gastrointestinal side effects. Erectile dysfunction is another risk of radiation treatment.
Also Check: Natural Products For Prostate Health
Proton Therapy For Recurrent Prostate Cancer
For those with a recurrence of prostate cancer, additional radiation therapy with photons can increase the risk of side effects and isnt generally recommendation. In these cases, proton therapy can provide an optimal dose of radiation to your tumor while protecting the healthy tissue surrounding the prostate. This puts radiation back on the table as a treatment option for recurrent prostate cancer.
Dont Miss: What Pain Is Associated With Prostate Cancer
What Happens During Radiation Therapy
Radiation therapy uses high-energy x-rays or a stream of particles . High doses of radiation can destroy abnormal cancer cells. Each treatment destroys some of the cancer cells at a microscopic level. Patients do not feel the radiation during treatment. They will only hear some electrical noise and may see light from the machine.
Also Check: Can I Shrink My Prostate
Possible Risks And Side Effects Of Brachytherapy
Radiation precautions: If you get permanent brachytherapy, the seeds will give off small amounts of radiation for several weeks or months. Even though the radiation doesnt travel far, your doctor may advise you to stay away from pregnant women and small children during this time. If you plan on traveling, you might want to get a doctors note regarding your treatment, as low levels of radiation can sometimes be picked up by detection systems at airports.
There’s also a small risk that some of the seeds might move . You may be asked to strain your urine for the first week or so to catch any seeds that might come out. You may be asked to take other precautions as well, such as wearing a condom during sex. Be sure to follow any instructions your doctor gives you. There have also been reports of the seeds moving through the bloodstream to other parts of the body, such as the lungs. As far as doctors can tell, this is uncommon and doesnt seem to cause any ill effects.
These precautions arent needed after HDR brachytherapy, because the radiation doesnt stay in the body after treatment.
Bowel problems: Brachytherapy can sometimes irritate the rectum and cause a condition called radiation proctitis. Bowel problems such as rectal pain, burning, and/or diarrhea can occur, but serious long-term problems are uncommon.
Proton Therapy Success Stories
Its one thing to hear about the success rate of proton therapy treatment for prostate cancer. Its another thing to hear the success stories straight from the mouths of survivors.
Wally K.
Wally, an Army pilot, biker, and all around adventurer, was diagnosed with prostate cancer only six weeks after being prescribed testosterone for his anemia.
There are unending volumes in thousands of books that attempt to describe the kaleidoscope of feelings and emotions that follow a diagnosis of metastatic cancer, said Wally in his journal entitled the Proton Chronicles. Im sure that like many, I attempted to rationalize or even justify the situation, but when faced with real mortality, your life and that of your family is forever altered.
After considering surgery and consulting multiple online forums, Wally finally decided on proton therapy to treat his cancer. Over the course of 20 hypofractionated treatments, Knight continued to bike on his favorite trails and play hockey in the local ice rink.
Its really kind of difficult to get your head around the whole situation, said Knight about his proton treatment. This is happening at the cellular level and its absolutely painless.
Earl M.
Earl, a mission pilot and pastor, also received proton therapy after being diagnosed with prostate cancer. Having lived in Alaska for nearly two decades with his wife, Lynn, he chose to seek medical care in other states after receiving his diagnosis.
Read Also: Mri Prostate With And Without Contrast
Treat Prostate Cancer With Fewer Side Effects
Physicians at the Maryland Proton Treatment Center use the most advanced form of proton therapy, known as pencil-beam scanning, to target prostate cancer tumors with unmatched precision, while minimizing damage to healthy tissue.
Proton therapy is a non-invasive and low-risk option that often improves the quality of life for men with prostate cancer. Research has shown that proton therapy may reduce the risks for side effects in urinary, bowel and erectile function, both in the short- and long-term.
Like traditional radiation therapy, proton therapy is typically administered one time per weekday for several weeks. Most patients complete their appointments within one hour each day. At the Maryland Proton Treatment Center, we use a novel hydrogel spacer instead of a balloon to create space around the prostate, protecting healthy tissues and allowing us to more precisely target the prostate cancer. The spacer is less invasive for patients because it involves having one procedure before treatment begins, as opposed to having a balloon inserted each day.
Comparison image Proton Therapy is on the left, Photon Therapy is on the right
Types Of Radiation Therapy
There are two broad categories of radiation therapy: external beam radiation therapy and brachytherapy. They work as follows:
- In EBRT, an external source of radiation beams photons or particles into the tumor. In the modern era of radiation oncology, the most common external radiation source is a megavoltage linear accelerator equipped with devices that allow precise shaping of X-ray photons and accurate tumor targeting.
- In brachytherapy, radioactive sources are implanted in the tumor, either temporarily or permanently.
Prostate cancer may be treated with EBRT alone, brachytherapy alone, or a combination of the two.
You May Like: What Causes Prostate Psa Levels To Rise
Intensity Modulated Radiation Therapy
IMRT, an advanced form of 3D-CRT therapy, is the most common type of external beam radiation therapy for prostate cancer. It uses a computer-driven machine that moves around the patient as it delivers radiation. Along with shaping the beams and aiming them at the prostate from several angles, the intensity of the beams can be adjusted to limit the doses of radiation reaching nearby normal tissues. This lets doctors deliver an even higher radiation dose to the cancer.
Some newer radiation machines have imaging scanners built into them. This advance, known as image guided radiation therapy , lets the doctor take pictures of the prostate just before giving the radiation to make minor adjustments in aiming. This appears to help deliver the radiation even more precisely and results in fewer side effects.
A variation of IMRT is called volumetric modulated arc therapy . It uses a machine that delivers radiation quickly as it rotates once around the body. This allows each treatment to be given over just a few minutes. Although this can be more convenient for the patient, it hasnt yet been shown to be more effective than regular IMRT.
A Paucity Of Practicality Puts Photons Ahead Of Protons
Joseph K. Salama, MD, and Christopher G. Willett, MD
The authors are affiliated with the Department of Radiation Oncology at Duke University in Durham,North Carolina. Dr Salama is an associate professor and Dr Willett is the chairman and a professor.
Since Wilhelm Röntgens discovery of the x-ray in 1895 and its application to the treatment of cancer, advances in technology have led to consistently improved cancer outcomes. Isocentric treatments, computer controlled radiotherapy, megavoltage energy therapy, intensity modulation, volumetric therapy, and image guidance all have significantly advanced the therapeutic index of treatments by improving the chance for appropriate delivery of radiotherapy, while minimizing the exposure of surrounding uninvolved organs.1
Recently, many have advocated proton beam therapy as the next technologic leap forwardone that will further enhance the therapeutic index. Not surprisingly, this enthusiasm has paralleled the establishment of a large number of proton beam therapy centers and a doubling of the number of Medicare beneficiaries receiving proton beam therapy.2 Despite its many theoretical advantages, however, the data do not support a switch to proton therapy at this time.
Potential Advantages of Protons
Planning and Delivery of Radiation
Significant Advances in Photon Therapy
Proton Therapy for Children?
Dosimetric Benefit vs Clinical Benefit
The Issue of Cost
You May Like: How Do You Massage Your Prostate
Recommended Reading: What Kind Of Cancer Is Prostate Cancer
Delivery Of Hypofractionated Radiation Therapy
Although standard fractionation in prostate cancer is defined as doses of 76 to 80 Gy delivered in daily fractions of 1.8 to 2.0 Gy, moderately hypofractionated doses of 2.4 to 3.1 Gy have been used in an effort to make prostate cancer radiotherapy more convenient and less expensive for patients and insurers. In general, evidence has supported its noninferiority to conventional fractionation using photon-based radiation therapy in the management of low- to intermediate-risk prostate cancer , although 2 studies have shown a nonsignificant increase in late complications . In addition, a few studies have documented the safety and efficacy of moderate hypofractionation with proton therapy.
Henderson et al reported outcomes for 215 men treated with proton therapy on a prospective trial. Patients with low- and intermediate-risk disease were treated to 70 GyRBE and 72.5 GyRBE, respectively, using 2.5 GyRBE per fraction. With a median follow-up of 5.4 years, biochemical control rates were 98.3% and 92.7% for patients with low- and intermediate-risk disease. Furthermore, the risks for grade 3 GI or GU toxicity were 0.5% and 1.7%, respectively.
What Are The Side Effects Of Brachytherapy
- Frequent urination or urinary retention or burning with urination
- Erectile dysfunction
- Urethral stricture or narrowing of the urethra
- Diarrhea or blood in the stool
- Secondary cancers
For the short time that the seeds are giving off larger amounts of radiation, you should avoid close proximity to children or pregnant women. Make sure to talk with your radiation oncologist or oncology nurse for instruction about radiation safety and exposure for family members or pets.
If you are traveling through an airport following brachytherapy treatment, there is a chance that radiation detectors will be set off. Talk to your radiation oncologist and ask for a note to indicate youve just had radiation treatment.
You May Like: Ways To Prevent Prostate Cancer
Proton Beam Radiation Therapy
Proton beam therapy focuses beams of protons instead of x-rays on the cancer. Unlike x-rays, which release energy both before and after they hit their target, protons cause little damage to tissues they pass through and release their energy only after traveling a certain distance. This means that proton beam radiation can, in theory, deliver more radiation to the prostate while doing less damage to nearby normal tissues. Proton beam radiation can be aimed with techniques similar to 3D-CRT and IMRT.
Although in theory proton beam therapy might be more effective than using x-rays, so far studies have not shown if this is true. Right now, proton beam therapy is not widely available. The machines needed to make protons are very expensive, and they arent available in many centers in the United States. Proton beam radiation might not be covered by all insurance companies at this time.
What Are The Different Types Of Internal Radiation Therapy
Brachytherapy and radiopharmaceuticals are both considered internal radiation therapies because they both work after being inserted inside the body, rather than being directed from outside. However, the similarities mostly end there. Brachytherapy works by implanting radioactive material into the prostate and is used for localized prostate cancer. Radiopharmaceuticals are injected into the bloodstream and are used for advanced, metastatic prostate cancer. Read on to find the details of each.
Also Check: Prostate Cancer Types And Treatment
What To Expect During Ebrt
The first day of treatment may be longer than other sessions because additional imaging is performed that day as part of quality assurance. In most cases, you’ll be scheduled for daily treatments, Monday through Friday. SBRT may be scheduled every other day, instead of daily. You’ll be assigned a treatment time slot, typically but not necessarily at the same time each day. A specifically trained radiation therapist will administer your treatments.
During treatment, you’ll be asked to lie motionless on the treatment table. The area being treated will be exposed and positioned beneath the linac. To deliver the radiation, the head of the machine will move around your body to predetermined angles. On a gantry-based linac, such as a Varian TrueBeam, each treatment takes from five to 20 minutes. On the CyberKnife, each treatment is typically 30 to 60 minutes. Expect to be in the radiation oncology clinic approximately 30 to 60 minutes each day if the TrueBeam is used or 60 to 90 minutes with the CyberKnife.
Please note that many people will be involved in your treatment â your doctor, residents, nurses, therapists, dosimetrists â but your radiation oncologist will supervise your treatment and ensure all steps are being performed accurately.
Literature Search Results And Characteristics
Our searches of four databases yielded 6,378 articles. After 413 duplication records were removed, titles and abstracts of these records were screened for inclusion. Full texts of 46 records were read, and 33 studies met the inclusion criteria .
Figure 1 Flow diagram of the literature screening process and results.
Twenty PBT-related studies involved 48,765 patients with a median mean age of 66 years old. Median follow-up across all studies was 43.4 months . The included studies were published from 2010 to 2020. Most of the studies were from the USA , five from Japan , and one from Korea . For the trials from the USA, most of the studies set irradiation dose at 7082 GyE delivered in 544 fractions. For the five trials from Japan, the irradiation dose was usually set at 6380 GyE delivered in 2039 fractions. For one trial from Korea, they set irradiation dose at 3560 GyE delivered in 520 fractions. The basic characteristics of the included studies are shown in Table 1.
Table 1 Basic characteristics of included studies.
Also Check: How To Promote Good Prostate Health
Technical Delivery Of Proton Therapy
A minimum standard of treatment delivery must be followed to ensure the accuracy and effectiveness of proton therapy for prostate cancer. The goals of delivery should be to overcome 3 fundamental radiation therapy challenges: to minimize uncertainty regarding the precise location of the target during beam exposure, to maximize target coverage, and to minimize radiation exposure to organs at risk.
Although intrafraction and interfraction variability must be accounted for with both proton- and photon-based treatment planning, there is a proton-specific uncertainty called ârange uncertainty,â which refers to the effect on the proton beam range that the slight variations in prostate position may have on the composition of tissues in the beam path. Range uncertainty is based on modeling studies and includes the addition of a margin to the proximal and distal edge of the target.