What Is The Prognosis For People Who Have Prostate Cancer
Because prostate cancer tends to grow slowly, most men die from something other than the disease. Early detection is key to better outcomes. Almost all men 97% to 98% diagnosed with localized cancer that hasnt spread outside of the prostate live at least five years after diagnosis. When metastatic cancer has spread outside of the gland, one-third of men continue to survive after five years.
Treating Advanced Prostate Cancer
If the cancer has reached an advanced stage, it’s no longer possible to cure it. But it may be possible to slow its progression, prolong your life and relieve symptoms.
Treatment options include:
- hormone treatment
- chemotherapy
If the cancer has spread to your bones, medicines called bisphosphonates may be used. Bisphosphonates help reduce bone pain and bone loss.
How Is Prostate Cancer Diagnosed
Doctors describe the growth and spread of prostate cancer in stages. Doctors use these stages as guides when choosing treatment options or offering prognoses to their patients.
Prostate cancer staging is based on a number of different factors, including prostate cancer screening tests such as a digital rectal exam or prostate-specific antigen test and imaging studies like bones scans, MRIs, CT scans, and trans-rectal ultrasounds.
Read Also: Can You Reduce An Enlarged Prostate
Where Do These Numbers Come From
The American Cancer Society relies on information from the SEER database, maintained by the National Cancer Institute , to provide survival statistics for different types of cancer.
The SEER database tracks 5-year relative survival rates for prostate cancer in the United States, based on how far the cancer has spread. The SEER database, however, does not group cancers by AJCC TNM stages . Instead it groups cancers into localized, regional, and distant stages.
- Localized: There is no sign that the cancer has spread outside the prostate.
- Regional: The cancer has spread outside the prostate to nearby structures or lymph nodes.
- Distant: The cancer has spread to parts of the body farther from the prostate, such as the lungs, liver, or bones.
What Are Prostate Cancer Treatment Side Effects
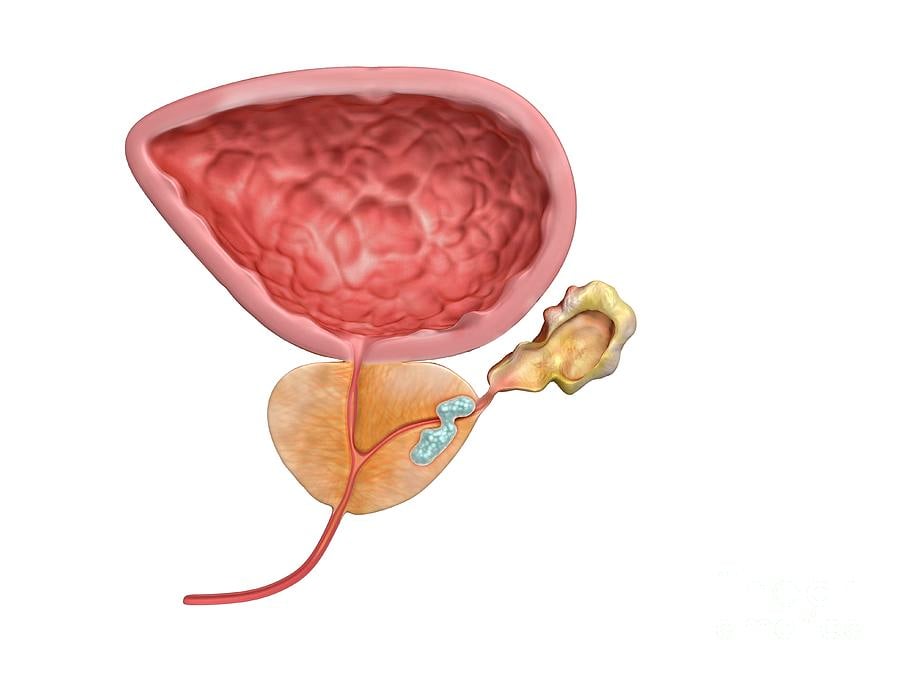
Some prostate cancer treatments can affect the bladder, erectile nerves and sphincter muscle, which controls urination. Potential problems include:
- Incontinence: Some men experience urinary incontinence. You may leak urine when you cough or laugh, or you may feel an urgent need to use the bathroom even when your bladder isnt full. This problem can improve over the first six to 12 months without treatment.
- Erectile dysfunction : Surgery, radiation and other treatments can damage the erectile nerves and affect your ability to get or maintain an erection. Some men regain erectile function within a year or two . In the meantime, medications like sildenafil or tadalafil can help by increasing blood flow to the penis.
- Infertility: Treatments can affect your ability to produce or ejaculate sperm, resulting in male infertility. If you think you might want children in the future, you can preserve sperm in a sperm bank before you start treatments. After treatments, you may undergo sperm extraction. This procedure involves removing sperm directly from testicular tissue and implanting it into a womans uterus.
Don’t Miss: What Is The Best Way To Treat Prostate Cancer
How Is Prostate Cancer Treated
For many men with prostate cancer, treatment is not immediately necessary.
If the cancer is at an early stage and not causing symptoms, a policy of “watchful waiting” or “active surveillance” may be adopted. This involves carefully monitoring your condition.
Some cases of prostate cancer can be cured if treated in the early stages. Treatments include surgically removing the prostate, radiotherapy and hormone therapy.
Some cases are only diagnosed at a later stage when the cancer has spread. If the cancer spreads to other parts of the body, typically the bones, it cannot be cured and treatment is focused on prolonging life and relieving symptoms.
All treatment options carry the risk of significant side effects, including erectile dysfunction and urinary incontinence. For this reason, many men choose to delay treatment until there is a risk the cancer might spread.
Newer treatments, such as high-intensity focused ultrasound or cryotherapy, aim to reduce these side effects. Some hospitals may offer them as an alternative to surgery, radiotherapy or hormone therapy. However, the long-term effectiveness of these treatments are not yet known.
Read more about treating prostate cancer
What Questions Should I Ask My Healthcare Provider
If you have prostate cancer, you may want to ask your healthcare provider:
- Why did I get prostate cancer?
- What is my Gleason score? What is my Grade Group? What do these numbers mean for me?
- Has the cancer spread outside of the prostate gland?
- What is the best treatment for the stage of prostate cancer I have?
- If I choose active surveillance, what can I expect? What signs of cancer should I look out for?
- What are the treatment risks and side effects?
- Is my family at risk for developing prostate cancer? If so, should we get genetic tests?
- Am I at risk for other types of cancer?
- What type of follow-up care do I need after treatment?
- Should I look out for signs of complications?
A note from Cleveland Clinic
Prostate cancer is a common cancer that affects males. Most prostate cancers grow slowly and remain in the prostate gland. For a small number, the disease can be aggressive and spread quickly to other parts of the body. Men with slow-growing prostate cancers may choose active surveillance. With this approach, you can postpone, and sometimes completely forego, treatments. Your healthcare provider can discuss the best treatment option for you based on your Gleason score and Group Grade.
Read Also: What Can You Do To Help An Enlarged Prostate
Bladder And Urinary Troubles
A prostate tumor that has grown significantly in size may start to press on your bladder and urethra. The urethra is the passage the carries urine from your bladder out of your body. If the tumor is pressing on your urethra, you might have trouble passing urine.
One of the common areas for prostate cancer to spread to is the bladder, because the two organs are close. This can cause additional problems with urination and bladder function.
Some symptoms your bladder and urethra are being affected by cancer include:
- urinating more frequently
- getting up in the middle of the night to pee
- having blood in your urine or semen
- feeling like you have to urinate often and not actually passing anything
Its not as common, but prostate cancer can also spread to your bowel. The cancer first spreads to the rectum, which is the part of your bowel closest to the prostate gland.
Symptoms of cancer thats spread to the bowels include:
- stomach pain
How Prostate Cancer Is Diagnosed And Staged
Cancer staging helps you and your doctor understand how advanced your cancer is and how much it has spread at the time of diagnosis. Knowing your cancer stage also helps your doctor determine the best treatment options for you and estimate your chance of survival.
The most widely used staging system for cancer is the TNM system that classifies cancer from stage 1 to stage 4.
TNM stands for:
- Tumor: the size and extent of the tumor
- Nodes: the number or extent of nearby lymph node involvement
- Metastasis: whether cancer has spread to distant sites in the body
The TNM scale is used for many types of cancer. When a doctor uses it to determine your prostate cancer stage, theyll consider several other factors as well, including:
- grade groups
Recommended Reading: Alternative Cures For Prostate Cancer
What Are The Five Stages Of Prostate Cancer
The Gleason grading system grades prostate cancer from 1 to 5. According to cells appearances under a microscope, this system grades the most common and second most common patterns of cells in a tissue sample collected via biopsy.
- Grade 1: The cells appear like normal prostate cells.
- Grades 2-4: Cells that score the lower look closest to normal and are suggestive of less aggressive cancer. Those that score higher look the furthest from normal and will probably grow faster.
- Grade 5: Most cells look vastly different from normal.
Depending on the Gleason score, the American Joint Committee on Cancer has classified prostate cancer into four stages.
Stage I cancer:
- This stage is known as localized cancer because the cancer has been found in only one part of the prostate .
- Stage I cancers cannot be felt during a digital rectal exam or seen with imaging tests.
- If the prostate-specific antigen is less than 10, it is most likely slow growing.
Stage II cancer:
- This stage of cancer is still localized but is more advanced than stage I.
- In stage II, the cells are less normal than stage I and may grow more rapidly.
- Stage IIA means that the cancer is found only on one side of the prostate, whereas stage IIB means that the cancer is found in both sides of the prostate.
Stage III cancer:
Stage IV cancer:
To summarize:
What Causes Prostate Cancer
Experts arent sure why some cells in the prostate gland become cancerous . Genetics appear to play a role. For example:
- Youre two to three times more likely to get prostate cancer if your father, brother or son has the disease.
- Inherited mutated breast cancer genes and other gene mutations contribute to a small number of prostate cancers.
Recommended Reading: Prostate Health Foods To Eat And Foods To Avoid
Expert Review And References
- American Cancer Society. Prostate Cancer Early Detection, Diagnosis, and Staging. 2019: .
- Garnick MB . Harvard Medical School 2015 Annual Report on Prostate Diseases. 2015.
- Hermanns T, Kuk C, Zlotta AR. Clinical presentation, diagnosis and staging. Nargund VH, Raghavan D, Sandler HM . Urological Oncology. Springer 2015: 40: 697-718.
- Logothetis CJ, Kim J, Davis J, Kuban D, Mathew P, Aparicio A. Neoplasms of the prostate. Hong WK, Bast RC Jr, Hait WN, et al . Holland Frei Cancer Medicine. 8th ed. People’s Medical Publishing House 2010: 94: 1228-1254.
- PDQ® Adult Treatment Editorial Board. Prostate Cancer Treatment Patient Version. Bethesda, MD: National Cancer Institute 2020: .
- PDQ® Adult Treatment Editorial Board. Prostate Cancer Treatment Health Professional Version. Bethesda, MD: National Cancer Institute 2020: .
How Is Stage Ii Prostate Cancer Treated
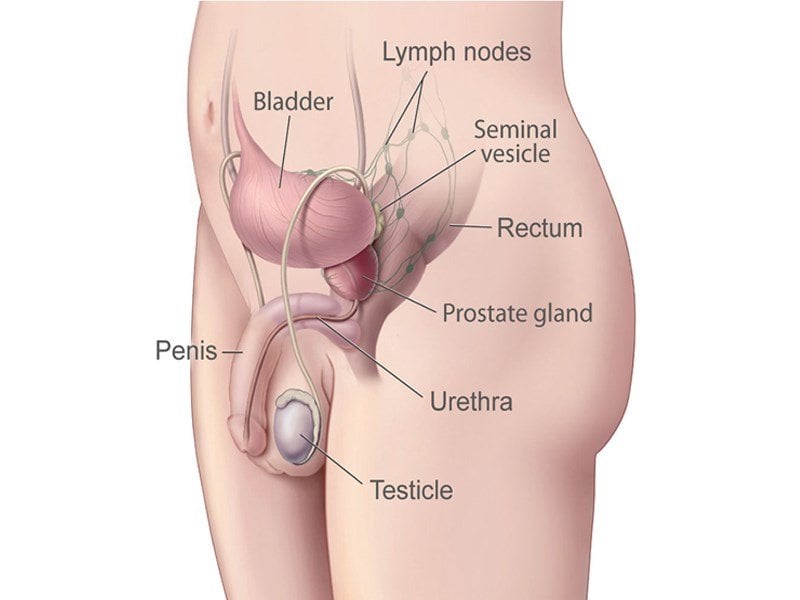
In stage II of prostate cancer, the cancer is small and is confined to the prostate gland and the growth and spread may be slow and it may never show symptoms. The course of action depends on the age of the patient and their overall health and if they can withstand the treatment. The following are the treatment methods generally preferred for stage I prostate treatment:
Active surveillance:
Because this cancer type grows very slowly, men may often not require any treatment immediately if not throughout their lifetime. Active surveillance is a method of monitoring the cancer closely regularly. PSA blood test, DRE , prostate biopsies may be done once in six months or so. If the results show signs of the cancer spreading, the treatment options are reviewed to eliminate the cancer.
External beam radiation:
It is a type of radiation therapy, a treatment method that involves use of high beams of X rays to kill cancerous cells. In external beam radiation therapy, also called EBRT, beams of radiation are focused on the prostate gland from a machine outside the body and it is used to treat the early stages of cancer.Read more about radiation therapy of prostate cancer here.
Brachytherapy:
Radical prostatectomy:
Also Check: Side Effects Of Having Your Prostate Removed
How Does Hormone Therapy Work Against Prostate Cancer
Early in their development, prostate cancers need androgens to grow. Hormone therapies, which are treatments that decrease androgen levels or block androgen action, can inhibit the growth of such prostate cancers, which are therefore called castration sensitive, androgen dependent, or androgen sensitive.
Most prostate cancers eventually stop responding to hormone therapy and become castration resistant. That is, they continue to grow even when androgen levels in the body are extremely low or undetectable. In the past, these tumors were also called hormone resistant, androgen independent, or hormone refractory however, these terms are rarely used now because the tumors are not truly independent of androgens for their growth. In fact, some newer hormone therapies have become available that can be used to treat tumors that have become castration resistant.
Dont Miss: Perineural Tumor
Learn More About Prostate Cancer Care At Rcca
If youve been diagnosed with prostate cancer or are concerned about potential symptoms, contact RCCA today. Our team of cancer care specialists will assess the stage of your cancer using the latest diagnostic methods and work with you to design a fully individualized care plan that includes advanced treatment options, the potential for clinical trials, and support that addresses physical and emotional well-being. To speak with a representative right away, please call .
Don’t Miss: Effects Of Radiation Therapy For Prostate Cancer
The Number Staging System
There are a few different systems used for staging prostate cancer. A simplified number staging system is described below.
- Stage 1 The tumour is contained in the prostate. The tumour is too small to be felt when a doctor does a rectal examination or to be seen on a scan.
- Stage 2 The tumour is still contained in the prostate, but your doctor can feel it when they do a rectal examination.
- Stage 3 The tumour has started to break through the outer capsule of the prostate and may be in the nearby tubes that produce semen .
- Stage 4 The tumour has spread outside the prostate. It may have spread to areas such as the bladder or back passage . Or it may have spread further, for example to the bones.
Using the numbered staging system described above:
- stage 4 is known as advanced prostate cancer.
See also
The grade of a cancer gives an idea of how quickly the cancer might grow or spread. A doctor decides the grade of the cancer by how the cancer cells look under the microscope.
Doctors look at the grade of the cancer to help them plan your treatment.
Gleason is the most commonly used grading system for prostate cancer.
How To Make The Right Treatment Decision
Current expert guidelines for treatment of localized prostate carcinoma recommend potentially curative therapy for patients whose life expectancy is at least 10 years., Patients with limited life expectancy are more likely to die from health conditions other than prostate cancer. Men with a life expectancy of more than 10 years are more likely to die from progressive prostate cancer. This 10-year rule enjoys broad acceptance among urologists and radiation oncologists.,
Conservative management proved to be an acceptable treatment option for men with low-grade Gleason scores, clinically localized disease, and life expectancies of less than 10 years. Increasing age was described as a risk factor for receiving inadequate treatment for prostate cancer. Thus, older men have been shown to receive potentially curative therapy less often than younger men., Radical prostatectomy is preferred treatment in men younger than 70 years, whereas radiation therapy is applied predominantly in patients older than 70 years. Conservative therapy such as watchful waiting or androgen deprivation by luteinizing hormone-releasing hormone analogs is preferentially applied in men older than 80 years. Watchful waiting or hormonal therapy is used to treat 82% of men older than 80 years.
Don’t Miss: How To Effectively Stimulate Prostate
Living With Prostate Cancer
As prostate cancer usually progresses very slowly, you can live for decades without symptoms or needing treatment.
Nevertheless, it can have an effect on your life. As well as causing physical problems such as erectile dysfunction and urinary incontinence, a diagnosis of prostate cancer can understandably make you feel anxious or depressed.
You may find it beneficial to talk about the condition with your family, friends, a family doctor and other men with prostate cancer.
Financial support is also available if prostate cancer reduces your ability to work.
Read more about living with prostate cancer
Diagnosis With The Tnm System
When using the TNM System, a patient’s PSA and Gleason scores are usually considered. Using the TNM system Stage 2 prostate cancer can be:
Stage 2a: prostate cancer cells are confined to one lobe, the PSA is less than 10 and the Gleason score 6 or less.
Stage 2b: prostate cancer cells are found in both lobes, or, cancer cells are found in one lobe and the PSA score is equal to or greater than 20, or, the Gleason score is equal to or greater than 8.
The main difference between the Stage 1 grade and Stage 2a grade is that at Stage 2a the PSA and/or Gleason score is higher. Whilst there are there are typically more prostate cancer cells at stage 2, they are still confined to the prostate gland and have not spread.
Don’t Miss: Can You Remove Your Prostate
Diagnosing Stage 2 Prostate Cancer
A stage 2 prostate cancer diagnosis can only be made after a number of tests have been given. Such tests may include:
A Needle Biopsy : a needle is inserted into the seminal vesicles, which are glands connected to the prostate, and a sample of fluid is taken. This sample is then analyzed using a microscope. If a certain level of cancerous cells are found and the cancer is still localized to the prostate, a diagnosis of second stage prostate cancer may be made.
Imaging Tests: MRI or CT scans determine whether tumors are present and the cancer has spread.
Digital Rectal Examination: a finger is inserted in the rectum to feel for any abnormalities of the prostate area.
PSA Test: prostate-specific antigen is a protein created in the prostate gland and found in the blood. Higher levels of PSA may indicate prostate cancer .
Gleason Test: the Gleason grading system assesses how aggressive a cancer is. The arrangement of cancer cells are examined underneath a microscope and patterns of cells are graded.
After the relevant tests have been taken, prostate cancer can be staged using a four stage system.
Currently, there are two main systems used to stage prostate cancer. The TNM system uses four categories 1-4 and the Whitmore-Jewett system uses four categories: A-D.