Does Untreated Clinical Gleason 6 Disease Cause Symptoms Or Death
Several studies that examined the natural history of untreated prostate cancer diagnosed in the prePSA screening era have suggested that men with Gleason 6 cancers are at risk for prostate cancerspecific mortality beyond 10 years of follow-up. The majority of the Gleason 6 disease was T1a/b disease, which was identified at the time of transurethral resection of the prostate for benign disease. Today, it is extremely rare to diagnose T1a/b disease because fewer TURPs are performed and those undergoing TURP have been prescreened with PSA testing. The results of the natural history studies in the PSA screening era are also problematic because many of the cases were likely misclassified at the outset because of the aforementioned limitations attributable to the random-systematic tissue sampling guided by TRUS.
With reported median follow-up ranging from 22 to 82 months, current active surveillance cohorts remain immature at this time, and longer follow-up will be necessary to draw definitive conclusions. Thus far, cancer-specific survival among these cohorts has been > 97%, and there are no data to suggest inferior outcomes after delayed radical therapy, as compared with immediate therapy.
A Roundtable Discussion With Brian F Chapin Md Jonathan I Epstein Md And Maha Hussain Md Facp Fasco
Physician-Patient Communication Oncologist counsels patient about options for treatment of prostate cancer. Photo courtesy of Thinkstock.
Prior to ASCOs 2016 endorsement of the Cancer Care Ontario guideline on active surveillance in the management of localized prostate cancer,1 most menover 90%diagnosed with low-risk localized disease were treated with active therapy.2 Today, about 50% of American men with low-risk disease opt for active surveillance instead of therapy. In Sweden, nearly 80% of men with low-risk prostate cancer undergo surveillance rather than treatment.3
This year, approximately 165,000 men in the United States will be diagnosed with prostate cancer,4 and half of those men will have low-risk tumors that pathologists rate as Gleason 6 disease. Changes to the Gleason score grading system in 2014 by the International Society of Urological Pathology classified Gleason 6 as grade 1, putting the cancer in the very lowrisk category.
Strong evidence suggests that Gleason 6 disease, when not associated with higher-grade cancer, almost never develops into aggressive cancer requiring treatment. Thus, many patients with Gleason 6 cancer are able to sidestep therapy, such as surgery and radiation therapy, and its attendant side effects, including sexual, urinary, and bowel dysfunction, for active surveillance, which is increasingly being adopted as the standard of care for men with a Gleason 6 score.
Defining Gleason 6 Cancer
Managing Localized Prostate Cancer
What Does It Mean If In Addition To Cancer My Biopsy Report Also Says Acute Inflammation Or Chronic Inflammation
Inflammation of the prostate is called prostatitis. Most cases of prostatitis reported on a biopsy are not caused by infection and do not need to be treated. In some cases, inflammation may increase you PSA level, but it is not linked to prostate cancer. The finding of prostatitis on a biopsy of someone with cancer does not affect their prognosis or the way the cancer is treated.
Also Check: Does Fish Oil Cause Prostate Cancer
Read Also: Blood In Urine After Radiation For Prostate Cancer
Risk Of Progression Of Prostate Cancer
Prostate cancer can also be classified based on the risk of recurrence . For this assessment, that can impact your choice of therapeutic approach, we take into account your clinical stage, PSA level, and Gleason score.
Low risk
Your cancer may be at low risk of spreading if:
- Your PSA level is less than 10 ng/mL
- You Gleason score is 6 or less
- Your cancer is stage T1 or T2a
Medium risk
Your cancer may be at medium risk of spreading if:
- Your PSA level is between 10 and 20 ng/mL
- Your Gleason score is 7
- Your cancer is stage T2b
High risk
Your cancer may be at high risk of spreading if:
- Your PSA level is higher than 20 ng/mL
- Your Gleason score is 8, 9 or 10
- Your cancer is stage T2c, T3 or T4
Survival For All Stages Of Prostate Cancer
Generally for men with prostate cancer in England:
- more than 95 out of 100 will survive their cancer for 1 year or more
- more than 85 out of 100 will survive their cancer for 5 years or more
- almost 80 out of 100 will survive their cancer for 10 years or more
Survival of prostate cancer is also reported in Scotland and Northern Ireland. But it is difficult to compare survival between these countries because of differences in the way the information is collected.
Cancer survival by stage at diagnosis for England, 2019Office for National Statistics
These statistics are for net survival. Net survival estimates the number of people who survive their cancer rather than calculating the number of people diagnosed with cancer who are still alive. In other words, it is the survival of cancer patients after taking into account the background mortality that they would have experienced if they had not had cancer.
Don’t Miss: What Size Of Prostate Requires Surgery
What Do The Results Mean
A higher Gleason score indicates more aggressive prostate cancer. Typically, lower scores suggest a less aggressive cancer.
In most cases, scores range between 610. Doctors do not often use biopsy samples that score 1 or 2, as they are not usually the predominant areas of the cancer.
A Gleason score of 6 tends to be the lowest possible score. A doctor will describe prostate cancer with a score of 6 as being well differentiated, or low grade. This means that the cancer is more likely to have a slower rate of growth.
Scores in the 810 region are poorly differentiated, or high grade. In these cases, the cancer is likely to spread and grow quickly. The growth rates of cancers with a score of 9 or 10 are likely to be twice as high as those of a cancer with a score of 8.
A score of 7 can be broken down in two ways:
This distinction indicates how aggressive the tumor is. Scores of 3 + 4 typically have a good outlook. A score of 4 + 3 is more likely to grow and spread than the 3 + 4 score, but less likely to grow and spread than a score of 8.
Some people receive multiple Gleason scores. This is because the grade may vary between samples of the same tumor or between two or more tumors.
In these cases, doctors are likely to use the higher score as the guide for treatment.
The Gleason score is an important tool for doctors when deciding on the best course of treatment. However, additional factors and grouping systems can assist them in making this decision.
What Is A Grade Group
In 2014, the International Society of Urological Pathology released supplementary guidance and a revised prostate cancer grading system, called the Grade Groups.
The Grade Group system is simpler, with just five grades, 1 through 5.
*Risk Groups are defined by the Grade Group of the cancer and other measures, including PSA, clinical tumor stage , PSA density, and number of positive biopsy cores.
Many hospitals report both the Gleason score and the Grade Group, but there may be hospitals that still report only the old Gleason system.
You May Like: How To Avoid Prostate Cancer
Read Also: Disadvantages Of Brachytherapy For Prostate Cancer
The Ajcc Tnm Staging System
A staging system is a standard way for the cancer care team to describe how far a cancer has spread. The most widely used staging system for prostate cancer is the AJCC TNM system, which was most recently updated in 2018.
The TNM system for prostate cancer is based on 5 key pieces of information:
- The extent of the main tumor *
- Whether the cancer has spread to nearby lymph nodes
- Whether the cancer has spread to other parts of the body
- The PSA level at the time of diagnosis
- The Grade Group , which is a measure of how likely the cancer is to grow and spread quickly. This is determined by the results of the prostate biopsy .
*There are 2 types of T categories for prostate cancer:
- The clinical T category is your doctors best estimate of the extent of your disease, based on the results of the physical exam and prostate biopsy, and any imaging tests you have had.
- If you have surgery to remove your prostate, your doctors can also determine the pathologic T category . The pathologic T is likely to be more accurate than the clinical T, as it is done after all of your prostate has been examined in the lab.
Numbers or letters after T, N, and M provide more details about each of these factors. Higher numbers mean the cancer is more advanced. Once the T, N, and M categories have been determined, this information is combined in a process called stage grouping to get the overall stage of the cancer.
How Do I Know The Gleason Grade Is Accurate
Assigning the correct Gleason score is a skill just like any other that is developed through experience and practice. It is often prudent to have the biopsy material referred for a second opinion at a reference center to confirm the accuracy of the initial Gleason score that was assigned.
References:
Also Check: Prostate Specific Antigen Normal Level
Active Surveillance Testing Schedule
Medical experts offer various recommendations regarding frequency of testing and when to start treatment during active surveillance. The American Society of Clinical Oncology recommends the following periodic evaluations while under active surveillance for prostate cancer:
-
PSA testing every three to six months
-
A digital rectal exam at least once a year
-
A prostate biopsy at least every two to five years
If test results or symptoms indicate the cancer is progressing, treatment is recommended with the intention of curing the disease.
What Is A Normal Gleason Score For Prostate Cancer
Your Gleason score doesn’t rank potential ranges like ranges set for elevated PSA tests. Instead, providers break Gleason scores into three categories:
- Gleason 6 or lower: The cells look similar to healthy cells, which is called well differentiated.
- Gleason 7: The cells look somewhat similar to healthy cells, which is called moderately differentiated.
- Gleason 8, 9 or 10: The cells look very different from healthy cells, which is called poorly differentiated or undifferentiated.
What are grade groups?
Healthcare providers established grade groups to clarify the Gleason score system. Those grade groups are:
- Grade Group 1 = Gleason 6 .
- Grade Group 2 = Gleason 3+4=7.
- Grade Group 3 = Gleason 4+3=7.
- Grade Group 4 = Gleason 8.
- Grade Group 5 = Gleason 9-10.
Read Also: Final Stages Of Metastatic Prostate Cancer
Stages Of Prostate Cancer
|
Any T, any N, M1 Any Grade Group Any PSA |
The cancer might or might not be growing into tissues near the prostate and might or might not have spread to nearby lymph nodes . It has spread to other parts of the body, such as distant lymph nodes, bones, or other organs . The Grade Group can be any value, and the PSA can be any value. |
Prostate cancer staging can be complex. If you have any questions about your stage, please ask someone on your cancer care team to explain it to you in a way you understand.
While the stage of a prostate cancer can help give an idea of how serious the cancer is likely to be, doctors are now looking for other ways to tell how likely a prostate cancer is to grow and spread, which might also help determine a mans best treatment options.
What Is A Gleason Score
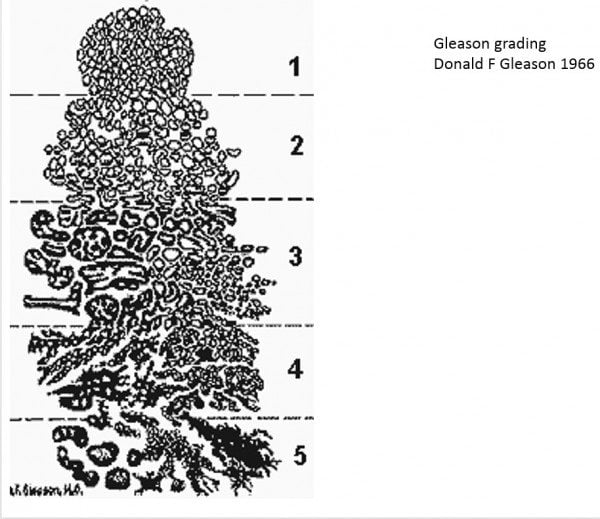
After a prostate biopsy, a pathologist looks at each sample under a microscope to see how closely they resemble normal prostate tissue and grade them on a scale of 1 to 5. Your Gleason score represents the two most common scores for tissue found in your biopsy. Because pathologists tend to only flag samples that are grade 3 or higher, the lowest score for prostate cancer is Gleason 6.
You May Like: Prostate Cancer Psa Level 200
Movement Builds To Classify Gleason 6 Prostate Lesions As Nonmalignant
In prostate cancer, as in life, you roll the dice.
In craps, 3+3 is called a “hard six.” It’s hard because you can only win if you repeat with a combination of 3+3. Any other sixes you roll — 4+2, 5+1 — are losers.
Gleason 3+3 is a hard six in prostate cancer. It is the lowest grade cancer in the traditional Gleason scoring system. Still, to the eye of a pathologist, a Gleason 6 looks like a malignancy.
Now, a few experts are questioning whether this hard six is a cancer at all. Some urologists see a Gleason 6 as a noncancerous growth that has the potential to be invasive, but most likely will never spread to other organs or end up killing a man.
To a patient like me, who has been on active surveillance for 10 years, a Gleason 6 can create a big medical fuss lasting years with regular prostate-specific antigen blood tests, digital rectal exams , biopsies, and MRIs. It can cause “anxious surveillance” that prompts them to drop AS and undergo unnecessary radical prostatectomy, which poses a potential risk of impotence and urinary incontinence.
The Gleason 6 diagnosis can yield polar opposite recommendations from urologists. Ten years ago, I found this to be the case in the matter of a day.
On December 14, 2010, a local urologist recommended I undergo a radical prostatectomy within the week. When asked, he said he didn’t support active AS, then a relatively new approach for monitoring low-grade prostate cancer.
‘The right thing to do’
Mixed reactions
Understanding Your Pathology Report: Prostate Cancer
When your prostate was biopsied, the samples taken were studied under the microscope by a specialized doctor with many years of training called a pathologist. The pathologist sends your doctor a report that gives a diagnosis for each sample taken. Information in this report will be used to help manage your care. The questions and answers that follow are meant to help you understand medical language you might find in the pathology report from your prostate biopsy.
Also Check: How To Cure Prostate Enlargement
How Is Active Surveillance Done
Although the protocol can vary, recommendations for active surveillance generally call for routine PSA tests and prostate biopsies to check for any indication that the cancer might be growing.
For example, patients at Montefiore Health System in New York City get a PSA test every 36 months, at least initially, and an MRI-guided biopsy a year after diagnosis, said Kara Watts, M.D., a urologist at the hospital who specializes in treating prostate cancer but was not involved in the study.
After the initial PSA tests and biopsy, how often they are performed depends largely on the patients particular situation, Dr. Watts explained.
We have a flexible protocol, particularly for people at both ends of the spectrum, she continued. For a man in his 70s and a life expectancy of 510 years , she said, additional PSA tests or biopsies may only be conducted every few years or only if he has symptoms. An otherwise healthy man in his 50s, on the other hand, will usually continue to have PSA tests and MRI-guided biopsies on a schedule similar to the initial protocol.
At the NIH Clinical Center, where Dr. Parnes sees patients, in addition to routine PSA testing, MRI-guided biopsies are used to help inform decisions around whether to pursue active surveillance and as part of the surveillance protocol.
Your Cancer Care Team
People with cancer should be cared for by a multidisciplinary team . This is a team of specialists who work together to provide the best care and treatment.
The team often consists of specialist cancer surgeons, oncologists , radiologists, pathologists, radiographers and specialist nurses.
Other members may include physiotherapists, dietitians and occupational therapists. You may also have access to clinical psychology support.
When deciding what treatment is best for you, your doctors will consider:
- the type and size of the cancer
- what grade it is
- whether the cancer has spread to other parts of your body
Also Check: Can I Get Cancer If My Husband Has Prostate Cancer
What Does It Mean
A Gleason score of 6 is low grade, 7 is intermediate grade, and a score of 8 to 10 is high grade cancer.
Get More Information
Its also important to know whether any cells rated at Gleason grade 5 are present, even in just a small amount, and most pathologists will report this. Having any Gleason grade 5 in your biopsy or prostate puts you at a higher risk of recurrence.
But because many prostate cancer cases are extremely slow-growing, the Gleason system didnt necessarily do a good job of communicating the risks for these cases. Patients with scores of 6 and 7 didnt have a clear picture of the nature of their particular cancer.
What Does It Mean To Have A Gleason Score Of 6 Or 7 Or 8
The lowest Gleason Score of a cancer found on a prostate biopsy is 6. These cancers may be called well-differentiated or low-grade and are likely to be less aggressive – they tend to grow and spread slowly.
Cancers with Gleason Scores of 8 to 10 may be called poorly differentiated or high grade. These cancers tend to be aggressive, meaning they are likely to grow and spread more quickly.
Cancers with a Gleason Score of 7 may be called moderately differentiated or intermediate grade. The rate at which they grow and spread tends to be in between the other 2.
Don’t Miss: What Doctor Does Prostate Exams
Biopsy Gleason Score Underestimates Disease Grade And Extent
On the basis of the intermediate end points of pathologic grade and stage, biopsy Gleason score underestimates both grade and extent of disease. Among men at a median age of 58 years who had at least a 10-core prostate biopsy, 36% of Gleason score 5 to 6 tumors were upgraded at radical prostatectomy if tertiary patterns were considered, and 25% were if tertiary patterns were not considered.20 The rate of upgrading was 35% for Gleason scores 5 to 6 on biopsy to Gleason score 7 at radical prostatectomy when studies that had evaluated at least 100 patient cases since 1992 were included.20
In addition to upgrading, men who are thought to harbor Gleason score 6 on biopsy may have more extensive nonorgan-confined disease. In a study evaluating men who met different criteria for enrollment in active surveillance, 70% to 80%, depending on inclusion criteria, were organ confined and Gleason score 6 on pathologic review of radical prostatectomy specimens.21 Furthermore, among men chosen for active surveillance based on a Gleason score 6 and treated surgically after a median of 1.3 years after enrollment, 80% had organ-confined disease.22 Thus, one could argue that if one in three to one in five men thought to harbor Gleason score 6 tumors actually have high-grade or nonorgan-confined disease, assigning a noncancer moniker to these low-grade cancers would disadvantage a substantial proportion of men by delaying curative therapy.