What Are The Warning Signs Of Prostate Cancer
Risk factors for prostate cancer include age, family history, race, and obesity. You may be at higher risk for prostate cancer if you are over age 50, have a family history of prostate cancer, are overweight, or if you are a Black man. See your doctor if you have any of these symptoms:
- Trouble passing urine
Sex After Surgery To The Prostate Gland
When your prostate gland is removed, you will still make sperm, but it wonât come out through your penis. It will be absorbed back into the body. You may also have problems with erections or lose interest in sex after prostate surgery. Although you may feel embarrassed, doctors who deal with prostate cancer are very used to talking about these issues and will be able to give you advice. There are treatments that can help with this.
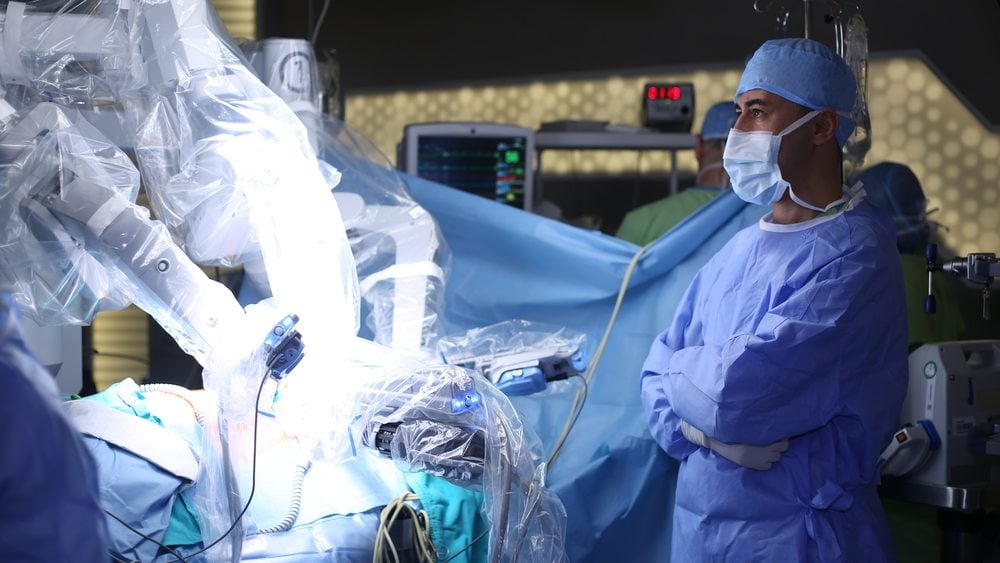
Robotic Prostate Surgery Details
Using the advanced surgical system, miniaturized robotic instruments are passed through several small keyhole incisions in the patients abdomen to allow the surgeon to remove the prostate and nearby tissues with great precision. This is much less invasive than a conventional radical retropubic prostatectomy, which involves an abdominal incision that extends from the belly button to the pubic bone.
During robotic-assisted radical prostatectomy, a three-dimensional endoscope and image processing equipment are used to provide a magnified view of delicate structures surrounding the prostate gland , allowing optimal preservation of these vital structures. The prostate is eventually removed through one of the keyhole incisions.
For most of the surgery, the surgeon is seated at a computer console and manipulates tiny wristed instruments that offer a range of motion far greater than the human wrist. The surgery is performed without the surgeon’s hands entering the patients body cavity.
Also Check: Is Asparagus Good For Prostate Cancer
Prostate Cancer Treatment Begins With Your Primary Physician
In most cases once youve been diagnosed with prostate cancer, your primary care physician and/or urologist will assist you with the necessary tests required before prostate surgery. This should be done approximately four weeks before surgery. If you have any questions regarding pre-operative tests please email us or call at .
About Your Prostate Surgery
A radical prostatectomy is a surgery to remove your entire prostate gland and seminal vesicles. Some of the lymph nodes in your pelvis are removed as well. This is done to prevent cancer from spreading from your prostate to other parts of your body.
A radical prostatectomy can be done in 1 of 2 ways. One way is through an open incision , which is called an open prostatectomy. Another way is to use a laparoscope, which is a tube-like instrument with a camera. Your surgeon will talk with you about the best surgery option for you.
Open prostatectomy
In an open prostatectomy, your surgeon will make an incision that goes from your pubic bone towards your belly button . Theyll remove the pelvic lymph nodes first, followed by the prostate gland, and then the structures next to it.
Figure 2. Open prostatectomy incisions
Laparoscopic or robotic-assisted prostatectomy
During a laparoscopic or robotic-assisted prostatectomy, your surgeon will make several small incisions in your abdomen . Theyll insert a laparoscope into 1 of the incisions and use gas to expand your abdomen. Surgical instruments will be inserted into the other incisions to remove the prostate. Some surgeons at MSK are specially trained to use a robotic device to assist with this procedure.
Figure 3. Laparoscopic or robotic-assisted prostatectomy incisions
Read Also: How Do They Scrape The Prostate
Will I Be Incontinent
Some patients have full urinary control as soon as the catheter is removed. Most patients experience some urinary leakage, which clears up in an average of three weeks but can take as long as 18 months. Small incontinence pads may be worn during this time to absorb any leaking urine and protect your clothing. For one out of 20 men, leakage may persist longer or even be permanent.
We define incontinence as needing more than two pads a day, says Dr. Mohler. Four out of five men wont need any pads at all. One in five will need one to two mini pads per day. One in 100 will end up needing more than two pads per day. This has a devastating effect on quality of life for these men. We dont fully understand why this happens, and we cannot predict who will have this experience. Strengthening the pelvic floor muscles with Kegel exercises before and after your operation may help you avoid or recover from problems with urinary control.
Removal Of The Catheter
Your catheter will be removed by the clinic nurse at Urology Care Wellington 7-14 days after surgery. This is straightforward. You will be given an antibiotic tablet at the time of catheter removal. Afterward, you will be monitored by the nurse to make sure that you are able to pass urine. She will check your wounds are healing and will discuss the use of pads and pelvic floor exercises.
Most patients have some incontinence when the catheter is taken out and most are pad-free three months after surgery. Over nine out of ten are pad-free after a year. We recommend that you start the pelvic floor exercises as soon as your catheter is removed and repeat them every day.
To be prepared for your catheter removal and any temporary urine leakage, you should ensure that you have your own supply of pads at home prior to attending for catheter removal. Bring two pads to your appointment for catheter removal.
Dont Miss: Fiducial Marker Placement For Prostate Cancer
Don’t Miss: Can Psa Test Detect Prostate Cancer
Life After Treatment: Alan Weiners Story
When Alan Weiner found out he had prostate cancer, it was a huge and frightening emotional bomb blast.
The New York native was diagnosed in February 2014 at age 69. After seeking out opinions from various doctors, Weiner underwent robotic prostatectomy in April at Mount Sinai Hospital in New York.
Because of the emotional toll his diagnosis took, Weiner says he found a support group that helped him through that uncertain time in his life. I joined Gildas Club after surgery, but if I had known about it, I would have attended sessions prior to deciding treatment, he says. I found a friend who went through the process and was understanding of my anxieties, fears, and projections.
I never thought that the emotional aspects of this would be so difficult to deal with, Weiner adds. I never believed that the mortality rate of prostate cancer was very low, and I believed that I would be the one who would not make it. I now know that my fears and negative thinking were things most men go through, however.
Today, Weiner goes for routine checkups, and two years after his initial diagnosis, his PSA level is undetectable. He deals with persistent sexual dysfunction, but the bladder control issues he first experienced after his surgery have resolved.
Postoperative Care After Prostate Surgery
After a healthy operation and discharge, there are some rules that you must follow. There is a risk of bleeding for the first several months after surgery. Therefore, there are some points to take into consideration. The length of the recovery period after prostate cancer surgery varies depending on some conditions. There are factors such as the type of surgery, the stage of disease, and the patientâs health status. However, overall recovery time is short.
Also Check: What Does An Enlarged Prostate Indicate
You May Like: Extreme Fatigue After Prostate Removal
Control Of The Lateral Pedicles And The Veil Of Aphrodite
The lateral pedicles at the prostate vesical junction are controlled using Hem-o-lock clips and/or bipolar coagulation. The clips are applied close to the prostate, and the pedicle is divided between them . Once the dissection enters the plane between the prostatic fascia medially and the levator fascia laterally, electrocautery is avoided and the anterior nerve-sparing dissection proceeds using sharp cutting with scissors and blunt dissection using the grasper . This dissection proceeds distally to the puboprostatic ligaments.
Several authors have also advocated a completely cautery-free or athermal dissection of the lateral pedicles to avoid any inadvertent damage to the neurovascular bundle. This can be achieved with laparoscopic bulldog clamps and oversewing of the neurovascular bundle for hemostasis. Although results of this technique have not been validated in large series, minimizing the use of cautery or other thermal hemostatic instruments during dissection near the neurovascular bundle seems prudent.
What Are The Types Of Radical Prostatectomy
Your surgeon will choose among several types of radical prostatectomy:
- Open radical prostatectomy: During this traditional type of surgery, your surgeon makes a vertical incision between your belly button and pubic bone. Your surgeon inserts tools through the incision to remove the prostate and surrounding tissue.
- Robot radical prostatectomy: Your surgeon makes several small incisions or one single incision across your abdomen. During the surgery, your surgeon operates state-of-the-art robotic controls outside your body. They can see the surgical area with a magnified view on a 3D screen.
You May Like: What Not To Eat For Enlarged Prostate
How Will Prostate Surgery Affect My Sex Life
Experienced robotic surgeons like Dr. David Samadi dont open the endopelvic fascia during surgery, which spares the rick of damage to nerve bundles that control sexual function. The recovery of the function, however, is not immediate and you should not feel discouraged if weeks or even a few months after surgery you experience erectile dysfunction. It is not an indication of long-term damage.
One major change that you will notice in your sex life is the absence of sperm. Having no prostate, the body will not produce semen during the orgasm. The sperm cells will be simply reabsorbed by the body them. This is not harmful and you shouldnt be worried about it. Plenty of men deal with the problem with the help of medication that improves erectile dysfunction.
What Are The Benefits To Patients
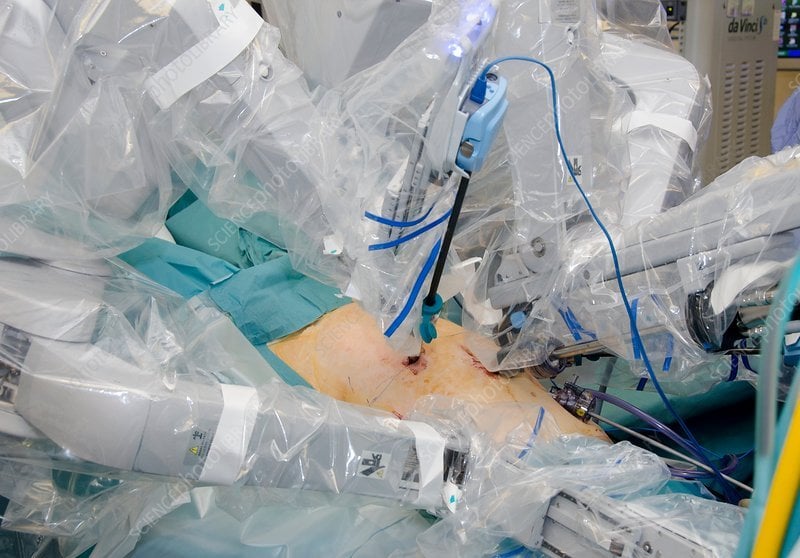
Robotics procedures, and minimally invasive surgeries in general, involve smaller incisions than traditional open surgeries, which reduces blood loss and postoperative recovery times. Patients typically experience significantly less pain and blood loss than in conventional open incision procedures. Patients also tend to enjoy quicker recovery times. Traditional open surgery can require several days of hospitalization and recovery time can last several months. While every case is unique, the return to normal, everyday activities following robotic-assisted surgery can occur in as little as two to three weeks.
You May Like: Prostate Cancer Recovery Time After Surgery
Open Or Laparoscopic Radical Prostatectomy
In the more traditional approach to prostatectomy, called anopen prostatectomy, the surgeon operates through a single long skin incision to remove the prostate and nearby tissues. This type of surgery is done less often than in the past.
In a laparoscopic prostatectomy, the surgeon makes several smaller incisions and uses special long surgical tools to remove the prostate. The surgeon either holds the tools directly, or uses a control panel to precisely move robotic arms that hold the tools. This approach to prostatectomy has become more common in recent years. If done by experienced surgeons, the laparoscopic radical prostatectomy can give results similar to the open approach.
What Is Robotic Prostate Cancer Surgery
Of the available comprehensive treatment options, UCA is proud to offer robotic prostate cancer surgery to patients with prostate cancer. As a surgical treatment option, the radical prostatectomy procedure removes the entire prostate gland. This can be performed by laparoscopic or robotic techniques. When open prostate surgery is performed, the prostate gland is removed through a larger incision in the lower portion of the abdomen. Laparoscopic prostate surgery involves small incisions, around the size of a keyhole, which are used for inserting a lighted viewing instrument into the pelvic region and allows the surgeon to examine and remove the prostate without a large, cumbersome abdominal incision.
Also Check: Radiation Dose For Prostate Cancer
Prostate Surgery Recovery Timeline
Prostate surgery recovery varies from person to person depending on how their body heals naturally and how severe the condition was prior to surgery. Here are some tips to help you through your recovery.
Prostatectomy typically requires general anesthesia and a hospital stay of 1 to 4 days. Your physician will have you walk around the day of or the day after your procedure. You may also be instructed to do little exercises while you are in the bed. All prostate cancer patients will be discharged from the hospital with a urinary catheter in place. A catheter is a thin flexible tube that is usually left in your bladder for 1 to 2 weeks to help drain your urine. Your doctor will give you specific guidelines about how to care for your catheter at home. Bladder control may be difficult for a few months after the catheter is removed. Some males will need a urinary catheter for 5 to 10 days after surgery.
Refrain from driving for 1 week after your prostate surgery. Do not drive until your catheter is removed. Also, be aware that you should not drive on prescribed pain medications unless a doctor says its ok. After one week, it should be safe to resume driving and begin most daily activities.
Less Time Under Anesthesia With Open Prostatectomy
An open prostatectomy, however, is a much shorter surgery than the robotic procedure, which means patients spend less time under anesthesia. Length of anesthesia for an open prostatectomy is 2 to 3 hours, compared to 4 to 7 hours for a robotic prostatectomy.
In several measures, there is no demonstrated difference between open and robotic prostatectomy. The risk of blood transfusion for an open prostatectomy is less than 1 percent, and fewer than 1 percent of patients have wound complications. Post-operative pain on the morning following surgery is typically 2 on a 10-point scale. The patients length of stay in the hospital is 1½ to 2 days. Approximately 85 percent of patients regain excellent urinary control, and three-quarters retain sexual potency.
While all precautions are taken to reduce the likelihood of complications, no surgical treatment is completely without risk. Potential complications of open and robotic prostatectomies include infection, bleeding requiring blood transfusion, urinary incontinence, erectile dysfunction and injury to adjacent organs.
You May Like: What Foods Can Prevent Prostate Cancer
Don’t Miss: How Big Is A Normal Prostate
Urinary Problems After Surgery
Leaking urine
Most men cant control their bladder properly when their catheter is first removed. This is because surgery can damage the muscles and nerves that control when you urinate.You might just leak a few drops if you exercise, cough or sneeze . Or you might leak more and need to wear absorbent pads, especially in the weeks after your surgery.Leaking urine usually improves with time. Most men start to see an improvement one to six months after surgery. Some men leak urine for a year or more and others never fully recover, but there are things that can help and ways you can manage it.
Difficulty urinating
A few men may find it difficult to urinate after surgery . This can be caused by scarring around the opening of the bladder or the urethra .Some men find they suddenly and painfully cant urinate. This is called acute urine retention and it needs treating quickly to prevent further problems. If this happens, call your doctor or nurse, or go to your nearest accident and emergency department.
Watch Paul’s story for one man’s experience of managing urinary problems after surgery below.
Sexual problems after surgery
Erection problems
Change in penis size and shape
Changes to orgasm
The seminal vesicles, which make some of the fluid in semen, are removed during surgery. This means you wont ejaculate any more. You may have a dry orgasm instead where you feel the sensation of orgasm but dont ejaculate. This may feel different to the orgasms youre used to.
What Happens Before Radical Prostatectomy
Before radical prostatectomy, your provider will ask you about your health history. Youll also need to tell your provider what drugs and vitamins you take. You may need to stop taking some of your medications a few days before your surgery, especially drugs that cause blood thinning.
Your hospital will give you specific instructions, including how long before your surgery to stop eating and drinking.
To check your health before your procedure, you also may need:
- Blood tests.
- Prostate ultrasound and biopsy.
Don’t Miss: Best Food For Prostate Problems
What Can I Expect Before And After Robotic Prostatectomy
If after consulting with Dr. Engel, becoming educated on the topic of prostate cancer, potentially seeking other opinions, and being presented all options, a patient opts for robotic prostatectomy, he will then be taken extensively through what to expect. Dr. Engel currently performs robotic surgery exclusively at George Washington University Hospital, and a date and time will be scheduled for surgery there. The patient will generally be urged to see his internist for a pre-operative physical, although this can also be accomplished at the hospital itself. Tests to rule out spread of cancer such as a bone scan and CT scan, looking for spread to bones and lymph nodes, may be performed in higher risk cases. The patient will be given detailed instructions regarding a bowel preparation regimen and the patient must follow this strictly. The purpose of the bowel prep is not only to create more space in the abdomen, but also for safety in the very unlikely event that there is an inadvertent injury to the intestine or rectum during the surgery. If this occurs, a bowel prep will likely keep this from being a life threatening problem.
Development Of The Extraperitoneal Space
This step is performed using a 30° upward-looking lens. A transverse peritoneal incision is made extending from the left to the right medial umbilical ligament and extended in an inverted U-shaped manner to the level of the vasa on either side. The vasa can also be divided at this point to aid in bladder mobility. The extraperitoneal space is developed after the medial and median umbilical ligaments are transected, allowing the bladder, prostate, and bowel to drop posterior and the remainder of the operation to be performed extraperitoneally . Some authors fill the bladder to help identify the planes of dissection and to aid in dropping the bladder posteriorly.
A 0° lens is used for optimum visualization, and 1:3 scaling is used for lymphadenectomy. Lymphadenectomy is performed at the surgeons discretion if the preoperative serum prostate-specific antigen value exceeds 10 ng/mL, the biopsy Gleason score is greater than 6, or more than 50% of the biopsy cores are positive for cancer. The anatomic boundaries of the limited bilateral pelvic nodes dissection include the iliac artery superiorly, the obturator nerve inferiorly, the iliac bifurcation cranially, and the obturator fossa caudally. The nodal package is sent for frozen-section analysis only if the nodes appear grossly enlarged.
Also Check: Prostate Cancer Signs Of Dying