Artemis Fusion Guided Biopsy: Targeted Painless Accurate
Prostate cancer can only be definitively diagnosed by means of a needle biopsy for laboratory analysis. Imaging alone cannot provide the cellular and genetic information we need to formulate a treatment plan. In fact, The Scionti Prostate Centers position is that it is unethical to put a man through treatment for prostate cancer without a needle biopsy to confirm and characterize the prostate cancer.
Many men fear the traditional TRUS guided biopsy that takes 12-14 needles. It is inaccurate up to 51% of the time and cannot accurately identify all the cancerous regions of the prostate gland. Our Center offers a painless targeted biopsy using advanced MRI fusion imaging. This has been referred to as a Smart Biopsy. Confirming the true nature of your cancer can be accomplished by selectively sampling the areas revealed by 3D MRI prostate mapping. Artemis® technology makes this possible.
The Scionti Prostate Center utilizes ARTEMIS technology to perform MRI-to-ultrasound precision fusion guided biopsy.We believe that a Smart targeted biopsy more precisely identifies the size, location and stage of a prostate cancer.
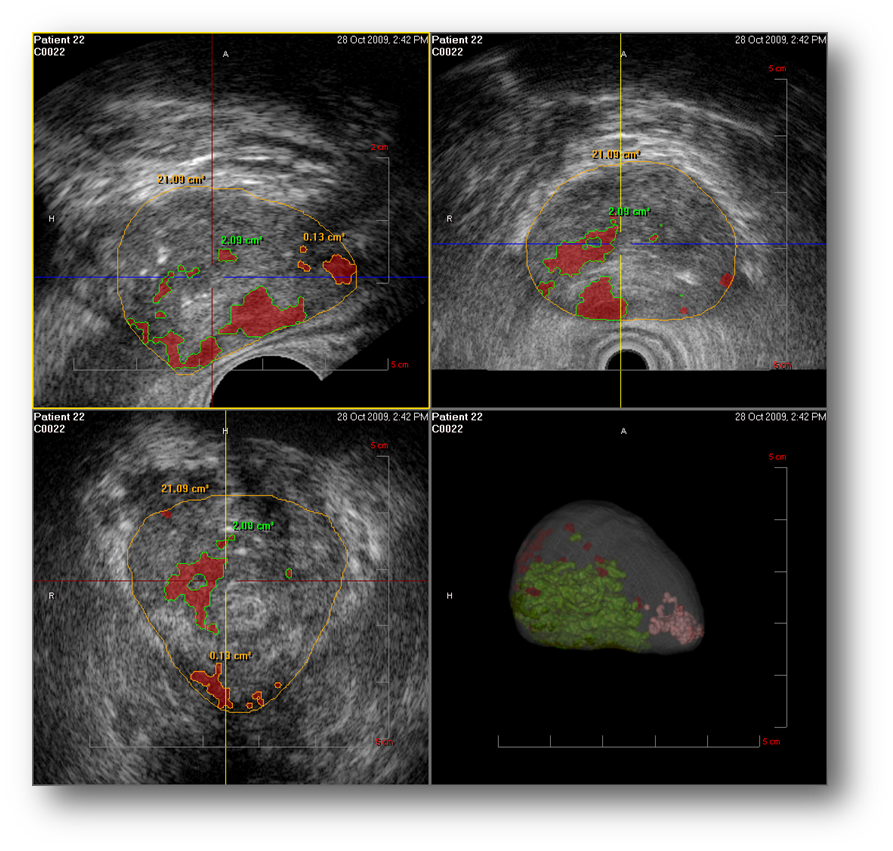
This figure illustrates the MRI-to-ultrasound fusion process.Ultrasound images on the left of the diagram are fused or superimposed on a model of the prostate made from MRI images.Biopsies can be directed to the MRI abnormalities.
What Is A Biopsy
A biopsy is a procedure that removes a sample of tissue or cells for study and are most commonly used to look for cancer.
Prostate biopsies are done with a biopsy needle that can be positioned with the assistance of ultrasound images to get samples for testing.
Your doctor might decide you need a prostate biopsy based on the results of a blood test that measures your level of PSA . A high PSA result might point to cancer, but there are other things such as non-cancerous enlargement or infection that cause PSA to rise. Tests that measure derivatives of PSA such as OPKO 4k and Prostate Health Index may be more accurate than PSA in assessing your risk for having a cancer that needs treatment.
Advanced Magnetic Resonance Mapping Targets Cancer
Using a cutting-edge technique for prostate cancer diagnosis and management, our team at University Hospitals uses MRI mapping to identify the exact location of suspicious tissue. We use images from the MRI to distinguish abnormal tissue from normal tissue. This allows our physicians to more accurately identify prostate cancer tumors and lesions, while also tracking their growth.
Although historically believed that MRI machines couldnt detect cancerous tissue, we now know that MRI images accurately identify aggressive cancers. So, with this knowledge, UH physicians developed the non-invasive fingerprinting technique to map the prostate and help distinguish normal from abnormal prostate tissue.
This breakthrough procedure lets UH physicians also monitor the prostate without making men go through unnecessary biopsies or other invasive examinations. As part of our active surveillance treatment, our team is able to monitor the growth of the tumor and determine if more interventional prostate cancer treatment is needed.
Future benefits may be even brighter: University Hospitals has been awarded a $5 million grant from the National Institutes of Health to further develop MRI mapping and the use of artificial intelligence to predict the likelihood of a cancer diagnosis.
Recommended Reading: Best Scan For Prostate Cancer
How Does It Work
An MRI-guided prostate biopsy occurs in an MRI-positive prostate lesion.
In other words, if there is no highly suspicious lesion in an MRI, theres no reason to spend extra money on a fusion biopsy.
With that in mind, the indications of this type of biopsy include :
- Patients who had previous transrectal ultrasound biopsies with a negative result but the suspicion is still very high.
- Patients with a diagnosis of prostate cancer under active surveillance.
After receiving the MRI image, doctors create a prebiopsy MRI map. They use a navigation feature that provides real-time feedback to guide needle location, the optimal patient position, and more.
The doctor may choose between a transperineal or transrectal approach depending on the prostate lesion.
The doctor will usually recommend the former if the patient is susceptible to infections or had a history of .
Fusion-guided biopsy uses a medical imaging software that works by:
Robotically Assisted Mr Imagingguided Biopsy
Robotic technology is currently undergoing evaluation for use in guiding prostate interventions and may increase the accuracy of needle placement in the prostate gland. All robotic components are constructed of nonmagnetic and dielectric materials for MR compatibility. These components are designed to accept as input the high-resolution anatomic and functional information provided by the MR imaging system and to be fully operational in the MR imaging suite.
Until recently, none of these systems was commercially available. The first commercially available robotically assisted MR imagingguided system was evaluated in a cadaver study , in which it was used to guide prostate interventions performed with a transgluteal approach. Preliminary results show that the use of this type of system has potential for improving prostate interventions .
You May Like: Psa In Bph And Prostate Cancer
The Day Of The Biopsy
The morning of the exam, give yourself a Fleet enema, which is available over the counter and follow the instructions on the packaging. The enema helps to clean out the rectum and to minimize the risk of infection.
You may eat a light breakfast and a light lunch before your biopsy, and you should take your usual medications, except for the above-mentioned blood thinners if applicable.
If you have undergone a recent artificial joint replacement you might need to take additional antibiotics about 1-2 hours prior to the biopsy. Please notify your Urologist if you have a recent history of such procedure, or if you usually take antibiotics before e.g. dental procedures.
What Happens During An Mri
These are done in the outpatient procedure area. Antibiotics will be given to reduce the risk of infection from the biopsy. Your doctor will be using the MRI and ultrasound images to watch where the biopsy needles are going. You may feel some discomfort or mild pain when the ultrasound probe is inserted into the rectum. Local anesthesia is used to ease the discomfort.
You May Like: Prostate What Does It Do
What Is A Biopsy And How Effective Is It
A needle biopsy is the only way to diagnose prostate cancer when it is suspected. But there are problems with the method most commonly used, called transrectal ultrasound guided biopsy. These problems often lead to inaccurate diagnosis.
For the last two decades, TRUS biopsy has been used to diagnose prostate malignancy. It is actually a blind and random procedure. Specific prostate tumors, especially very small ones, cannot be identified because ultrasound cannot visually detect specific cancer sites. Therefore, it is blind to tumors. In addition, TRUS biopsies tend to target the peripheral aspects of the gland and are likely to miss 30-40% of prostate cancer located in the anterior, midline transition zone, or apex. This is called sampling error. To attempt to overcome it, TRUS biopsies typically average 12-14 needles saturation biopsies use as many as 24 needles. The more needles used, the greater the risk of discomfort, infection, and urinary or sexual side effects while tumors continued to be missed. No other type of tumor cancer is biopsied this way!
Preparation For The Biopsy
You cannot take aspirin or other blood thinners, such as Plavix, Eliquis, Brilinta, Pradaxa, Coumadin, Warfarin, Ibuprofen, Naproxen, Aleeve, Advil, Celebrex, Ecotrin, and many others for several days prior to your scheduled biopsy. If you take any of these or other anticoagulants please discuss this with your Urologist beforehand. It might be necessary that you also consult with your Cardiologist prior to stopping.
Read Also: What Are The Symptoms Of Prostate Cancer Men’s Health
Mri/ultrasound Fusion Guided Biopsy For Prostate Cancer
How we detect prostate cancer has changed little in the past 30 years. University of Iowa urologists and Holden Comprehensive Cancer Center experts now offer a new technology to help improve the accuracy of prostate cancer biopsies.
MRI/Ultrasound fusion guided biopsy combines a specialized magnetic resonance imaging scan with an ultrasound image to help urologists precisely target the area of the prostate that needs to be biopsied. This approach allows our doctors to ensure they sample the exact site in the prostate where there is concern for cancer.
Koelis Technology For Fusion Biopsy
For over a decade KOELIS® has assisted urologists and radiologists from around the world in their routine clinical practice providing the latest technology for personalized prostate cancer.
We propose precise real-time 3D transrectal ultrasound fusion-guided transperinal and transrectal prostate biopsy against conventional and random systematic biopsy to increase sampling quality with KOELIS Trinity®. In a simple process and device, KOELIS Trinity® cartographer is a powerful diagnostic tool to plan, implement, review and control a personalized care solution. It creates a detailed and personalized map of the patients prostate showing accurate core distribution since our image-based cartographer is equipped with the Organ-Based Tracking® technology. Without changing the usual clinical practices, this technique brings an increased quality control over biopsy localizations. A precise, individual prostate biopsy mapping is a value for the accurate diagnosis and the further management of each patient.
Health innovation as a passion
At KOELIS®, we innovate every day in collaboration with world-renowned universities and hospitals to offer physicians new advancements in imaging and a greater field of view in order to bring personalized answers to every patient, in the respect of their quality of life.
Do you have questions about our precision fusion technology? Find the common inquiries or contact us !
To locate a clinic equipped with our solutions: Discover our interactive map.
Read Also: How To Reach Your Prostate
Mri Guided Prostate Biopsy For Prostate Cancer Diagnosis: Now Available At University Hospitals
University Hospitals offers a prostate biopsy procedure guided by magnetic resonance imaging technology. This leading-edge diagnostic tool for prostate cancer is much more efficient than a traditional biopsy and causes less discomfort. In some cases, you can receive a diagnosis and treatment plan in as little as a day.
Benefits Of Mri/us Fusion Guided Biopsy:
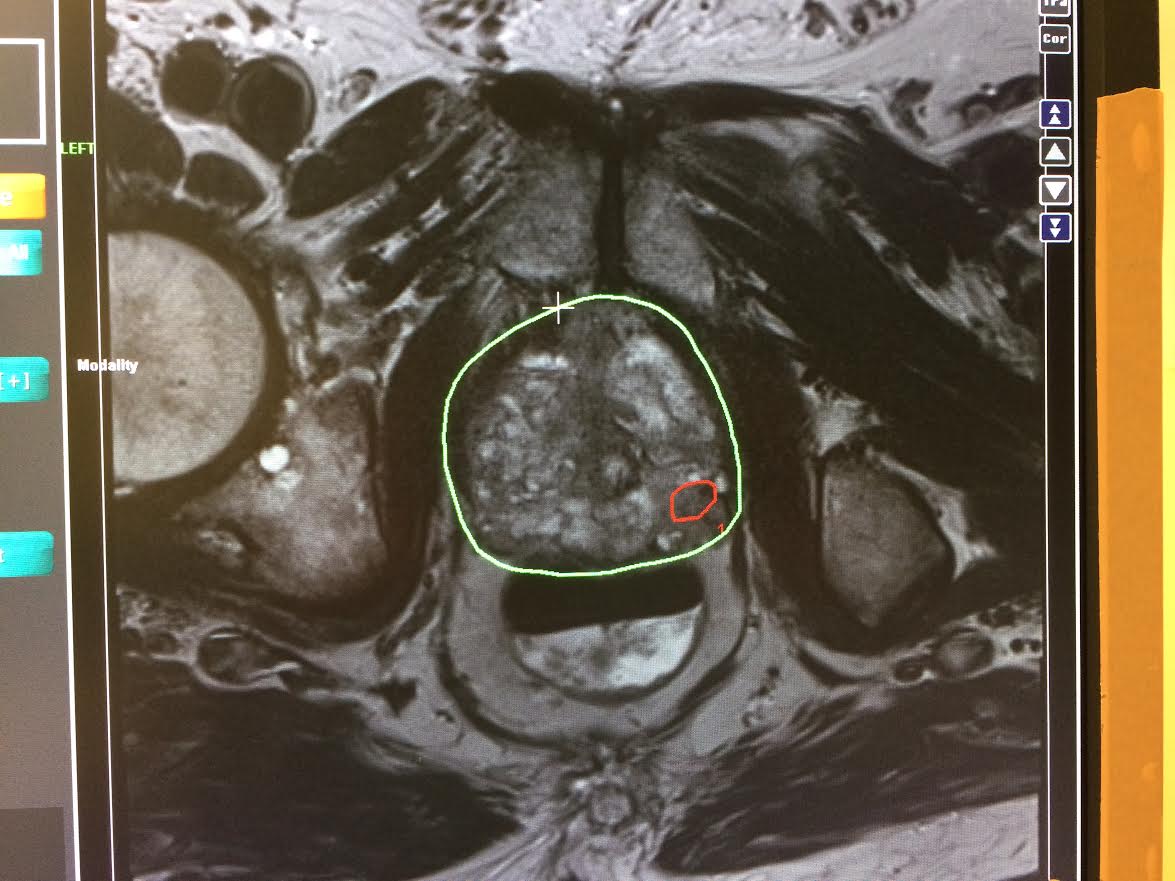
- Identifies and locates hidden tumors missed by traditional biopsies
- Enhances visualization of tumors within the prostate, detailing exact size and location of suspicious tissue and tumors
- 3D map of the prostate and tumor allows for targeted biopsies and improved sampling for a more accurate diagnosis.
- Fusion of live 3D Ultrasound and MRI images provide more accurate staging, diagnosis and individualized cancer treatment and management plan
- The system provides the ability to retrieve a record of previous biopsy sites to allow the urologist to go back to the exact area of a previous biopsy site
While MRI and MRI/US Fusion Guided Biopsy may offer benefit in a few scenarios, it is not appropriate for all men. Those who would potentially benefit, generally fall into the following categories:
Prostate MRI and MRI/US Fusion Guided Biopsies are the most advanced techniques available to screen and stage prostate cancer in the appropriate situations. Although a prostate MRI or MRI/US Fusion Guided Biopsy is not appropriate for all men, if you or a loved one are concerned about the risk of developing prostate cancer, we encourage you to talk to your Urologist about these tests to determine if they are right for you.
To learn more about these procedures and about Dayton Physicians Network Urology please call 937-293-1622.
Were here for you, leading with the latest technology.
You May Like: Mayo Clinic For Prostate Cancer
What Are The Benefits
- This technique allows our specialists to find hidden tumors that may be missed by other prostate biopsies.
- We can perform targeted biopsies using sophisticated MRI/ultrasound fused images to focus on the worrisome areas directly.
- The technology, which has proven to be very useful for men with previous negative biopsies, may also help detect aggressive cancers in patients who have not had a previous biopsy.
- It may reduce the number of biopsies you need.
Talk to your doctor or your urologist if you want to learn more about the prostate MRI fusion biopsy. Or call for the Urology department for an appointment with Dr. Chad Tracy.
% Less Detection Of Insignificant Cancer 3 Times Less Biopsy Core: Less Complication And Side Effects Mri/us Fusion Cancer Detection Rate
PRECISION study : MRI-Targeted or standard Biopsy for Prostate-Cancer Diagnosis
V.Kasivisvanathanet al. May 2018
For this reason:
- In cases of negative results, the hypothesis of cancer cannot be ruled out.
- In cases of low-positive results, suspicion of more aggressive cancer may remain.
Conventional Biopsy : Possible results
25% of cases Biopsy misses the tumor
Fortuitous reaching of non significant cancer
Underestimation of tumors size
Delaying the diagnosis, under- or overestimating the aggressiveness of the disease and, ultimately, failing to provide the best possible care for the patient.
However, the evolution of medical imaging techniques together with advances in fusion technologies have changed the landscape where practices are concerned.
In technical terms, targeted biopsies are made possible by the fusion of ultrasound images of the prostate with MRI scans or PET sequences, in real time during the procedures.
Recommended Reading: How Is Prostate Test Done
Targeted Prostate Biopsy: What You Should Know
Targeted biopsy is being used at UCLA to diagnose prostate cancer. Targeted biopsy refers to using advanced imaging techniques to identify areas of the prostate suspicious for cancer, and then directly biopsying them. The traditional method of biopsy uses ultrasound imaging, with which tumors are hard to see. With targeted prostate biopsy, systematic sampling of prostate tissue is performed. The new method employs sophisticated MRI technology, developed at UCLA, to visualize prostate cancer, and fusion of the MR images with real-time ultrasound using the specialized biopsy equipment. The result is a 10-20-minute procedure, done in the clinic under local anesthesia, that is much more accurate at finding significant prostate cancer in men.
What Gets Stored In A Cookie
This site stores nothing other than an automatically generated session ID in the cookie no other information is captured.
In general, only the information that you provide, or the choices you make while visiting a web site, can be stored in a cookie. For example, the site cannot determine your email name unless you choose to type it. Allowing a website to create a cookie does not give that or any other site access to the rest of your computer, and only the site that created the cookie can read it.
Read Also: What Is The Treatment For Prostate Cancer That Has Spread
The Groundbreaking Technology Includes:
The PROMAP-MR combines 3D ultrasound and MRI to produce an accurate 3D mapping of biopsy samples within multimodal images.
The PROMAP-US combines full 3D ultrasound and automatic organ tracking to create, visualize and memorize a 3D map of target lesions and biopsy samples.
How 3D Ultrasound/MRI Fusion Biopsy Works
- Creates a 3D map of the prostate.
- Identifies suspicious lesions or targets on MRI.
- A specially trained urologist overlays 3D MRI and 3D ultrasound images in order to get a precise picture and location of suspicious areas of the prostate .
- Accurately guides the biopsy needle into the target lesion. Uniform random biopsies of other areas of the prostate may also be performed, depending upon the clinical circumstances.
- The computer creates a record of the exact location of each biopsy, which is then stored and available for future use.
Studies show that computer-assisted 3D Ultrasound/MRI Fusion Biopsy provides a more precise way to identify clinically significant prostate cancers. This allows patients access to unique technology that will significantly improve their clinical outcomes.
Who is a Candidate?
Several groups of patients can take advantage of this diagnostic tool including:
Talk to your doctor about the 3D Ultrasound/MRI Fusion Biopsy to see if you are a candidate for this advanced diagnostic procedure for prostate cancer.
Contact Us
What Is Mri With Transrectal Ultrasound Fusion
Prostate cancer has a new standard of care in MRI-guided fusion biopsy with transrectal ultrasound. While a prostate biopsy has been the only way to get a definitive diagnosis of prostate cancer, it has only been working if cancer cells are identified in the sample tissue. But in some cases, such as when the tumor occurs at the top surface of the prostate or other unusual locations, a biopsy may not give a correct diagnosis. For instance, the standard TRUS guided biopsy in which tissue samples are collected from the prostate in a systematic pattern gives a negative result with tumors located in unusual areas of the prostate. About 15-20 percent of tumor locations can be missed by the biopsy needle.
Don’t Miss: Prostate Cancer Gene Test Helps Patients Decide On Treatment
The Sperling Prostate Center Advantage
Our philosophy is to match the treatment with the disease. Our BlueLaser 3T mpMRI-Guided Biopsy is the most responsible and accurate way to know your disease before making a treatment decision. We help patients avoid the risk of under-treating aggressive disease, or over-treating insignificant disease that can safely be monitored. We pride ourselves on having attained international recognition for excellence in real-time MRI-guided prostate cancer diagnosis.
If BlueLaser 3T mpMRI detects cancer, a biopsy is essential because prostate cancer may not show early symptoms, though certain warning signs indicate increased prostate cancer risk:
- An elevated or rising PSA blood test result
- An abnormal digital rectal exam
- A family history of prostate cancer or breast cancer
- Being of African-American descent
- Exposure to certain cancer-causing toxins, e.g. Vietnam vets exposed to Agent Orange
- In later stages, prostate cancer may show symptoms such as urinary difficulties, blood in urine, pelvic or back pain, and bone pain. See a doctor if any of these symptoms occur.