Are Prostate Problems Always A Sign Of Prostate Cancer
Not all growths in the prostate are cancerous, and not all prostate problems indicate cancer. Other conditions that cause similar prostate cancer symptoms include:
- Benign prostatic hyperplasia : At some point, almost every man will develop benign prostatic hyperplasia . This condition enlarges the prostate gland but doesnt increase cancer risk. The swollen gland squeezes the urethra and blocks the flow of semen and urine. Medications, and sometimes surgery, can help.
- Prostatitis: Men younger than 50 are more prone to prostatitis, inflammation and swelling of the prostate gland. Bacterial infections are often the cause. Treatments include antibiotics or other medications.
What Causes Prostate Cancer
Experts arent sure why some cells in the prostate gland become cancerous . Genetics appear to play a role. For example:
- Youre two to three times more likely to get prostate cancer if your father, brother or son has the disease.
- Inherited mutated breast cancer genes and other gene mutations contribute to a small number of prostate cancers.
Three Helpful Upcoming Webinars
Three upcoming webinars deal with the diagnosis and work-up of clinically significant forms of localized prostate cancer handling anxiety and related issues for men on active surveillance and whether AS is appropriate for African Americans and others of African ethnicity. See below for details.
On Wednesday, June 30, at 7:00 to 8:30 pm Eastern, the Cancer Support Community and Prostate Cancer International will be presenting a webinar on the diagnosis and work-up of men with clinically significant forms of prostate cancer . The featured speaker will be Prof. Eric Klein, MD, of the Cleveland Clinic. He will be addressing current and potential new ways to properly identify such patients among the previously undiagnosed and among men progressing on active surveillance.
You will be able to take advantage of this educational webinar in three ways:
- You can participate actively in this live ZOOM meeting if you .
- After the meeting, we will be posting a full recording of the meeting on YouTube at this link.
On Saturday, June 26, at 12:00 to 1:30 pm Eastern, Active Surveillance Patients International is presenting a webinar on mood and anxiety issues and how they may impact decisions about starting and staying on active surveillance for relatively favorable risk form of localized prostate cancer. The featured speaker will be Alan J. Hsu, MD, a board-certified psychiatrist who works at Moores Cancer Center, UC San Diego Health, in San Diego.
Read Also: How To Get Rid Of Prostate Stones
Ethics Approval And Consent To Participate
PBCG data were collected following IRB approval at UT Health San Antonio, Memorial Sloan Kettering Cancer Center, Mayo Clinic, University of Zurich, VA Durham, VA Caribbean Healthcare System San Juan, P.R., VA Durham, San Raffaele Hospital, Sunnybrook Health Systems, University of California San Francisco, Hamburg University Hospital. Analyses on anonymized data for this study were approved by the Technical University of Munich Ethics Commission. Consent was waived for all data collection, which involved only record extraction of standard clinical care elements. For detailed family history collected at the Durham VA written consent was obtained by all participants as required for a local study prior to this study.
What Happens If My Biopsies Comes Back Negative
Just because your biopsies are negative, does not mean that you do not have cancer in your prostate. You need to be seen on a regular basis for digital rectal examination and PSA testing. If there is significant change in your PSA, we may suggest repeat biopsies. The average risk of finding cancer in a repeat biopsy following a benign diagnosis is about 18%.
Recommended Reading: Best Bike Seat For Prostate
Outcome Measurements And Statistical Analysis
We used multinomial logistic regression to estimate the risks of high-grade prostate cancer on biopsy based on clinical characteristics, including age, prostate-specific antigen, digital rectal exam, African ancestry, first-degree family history, and prior negative biopsy. We compared the PBCG model to the PCPTRC using internal cross-validation and external validation on the European cohorts.
What Are Prostate Cancer Treatment Side Effects
Some prostate cancer treatments can affect the bladder, erectile nerves and sphincter muscle, which controls urination. Potential problems include:
- Incontinence: Some men experience urinary incontinence. You may leak urine when you cough or laugh, or you may feel an urgent need to use the bathroom even when your bladder isnt full. This problem can improve over the first six to 12 months without treatment.
- Erectile dysfunction : Surgery, radiation and other treatments can damage the erectile nerves and affect your ability to get or maintain an erection. Some men regain erectile function within a year or two . In the meantime, medications like sildenafil or tadalafil can help by increasing blood flow to the penis.
- Infertility: Treatments can affect your ability to produce or ejaculate sperm, resulting in male infertility. If you think you might want children in the future, you can preserve sperm in a sperm bank before you start treatments. After treatments, you may undergo sperm extraction. This procedure involves removing sperm directly from testicular tissue and implanting it into a womans uterus.
You May Like: What Is Prostate Specific Antigen
How Is Prostate Cancer Diagnosed
Screenings are the most effective way to catch prostate cancer early. If you are at average cancer risk, youll probably have your first prostate screening at age 55. Your healthcare provider may start testing earlier if you have a family history of the disease or are Black. Screening is generally stopped after age 70, but may be continued in certain circumstances.
Screening tests for prostate cancer include:
- Digital rectal exam: Your provider inserts a gloved, lubricated finger into the rectum and feels the prostate gland, which sits in front of the rectum. Bumps or hard areas could indicate cancer.
- Prostate-specific antigen blood test: The prostate gland makes a protein called protein-specific antigen . Elevated PSA levels may indicate cancer. Levels also rise if you have BPH or prostatitis.
- Biopsy: A needle biopsy to sample tissue for cancer cells is the only sure way to diagnose prostate cancer. During an MRI-guided prostate biopsy, magnetic resonance imaging technology provides detailed images of the prostate.
What Is Biopsy And How Is It Done
Once we find an abnormal area in the prostate on ultrasound, we need to remove small pieces of prostate for pathological examination called prostate biopsy.
While the ultrasound probe is in the rectum, a biopsy needle is inserted through the probe and under the ultrasound guidance, biopsies are performed. Six to twelve tine pieces of tissue are taken from the prostate. These pieces of prostate tissue are then sent to a Laboratory where a pathologist who is an expert in prostate cancer examined these pieces under the microscope to determine.
- Whether cancer is present
- Evaluate microscopic features of cancer
- Whether suspicious lesions are present
- Or the biopsy is negative for cancer
- Whether inflammation is present
Recommended Reading: Aggressive Prostate Cancer Survival Rates
What Questions Should I Ask My Healthcare Provider
If you have prostate cancer, you may want to ask your healthcare provider:
- Why did I get prostate cancer?
- What is my Gleason score? What is my Grade Group? What do these numbers mean for me?
- Has the cancer spread outside of the prostate gland?
- What is the best treatment for the stage of prostate cancer I have?
- If I choose active surveillance, what can I expect? What signs of cancer should I look out for?
- What are the treatment risks and side effects?
- Is my family at risk for developing prostate cancer? If so, should we get genetic tests?
- Am I at risk for other types of cancer?
- What type of follow-up care do I need after treatment?
- Should I look out for signs of complications?
A note from Cleveland Clinic
Prostate cancer is a common cancer that affects males. Most prostate cancers grow slowly and remain in the prostate gland. For a small number, the disease can be aggressive and spread quickly to other parts of the body. Men with slow-growing prostate cancers may choose active surveillance. With this approach, you can postpone, and sometimes completely forego, treatments. Your healthcare provider can discuss the best treatment option for you based on your Gleason score and Group Grade.
The Prostate Cancer Risk Calculators
Risk Calculator 1 the general health calculator is a starting point, looking at family history, age and any medical problems with urination.
Risk Calculator 2 the PSA risk calculator looks at the levels of prostate specific antigen in patients blood to help predict whether further investigation is required.
Risk calculator 3 and 4 the urologist risk calculator using data from DRE, TRUS and/or MRI and providing probabilities based on traditional Gleason grading or with inclusion of cribriform growth for the definition of clinically significant prostate cancer.
The option of calculating probabilities based on a definition of clinically significant prostate cancer including information on cribriform growth and intraductal carcinoma is currently available for the risk calculators without MRI information.
See table below for difference in definition of clinically significant prostate cancer
| Indolent prostate cancer | ||
|---|---|---|
| Gleason score 3+3 | Gleason 3+4 of higher or clinical stage > T2B | |
| Cribriform risk calculator 3/4 | GG1 or GG2 without cribriform growth or intraductal carcinoma | GG2 with cribriform or intra ductal carcinoma or GG3 or higher |
Nowadays these risk calculators are combined into one decision tree and thus can be used for men that have not been previously biopsied but also for men that have been screened previously and had a prostate biopsy with a benign result. In addition, if available, there is an option to include the result of an MRI .
You May Like: Prostate Cancer Self Exam How Often
Information About Calculator Input
Prostate Specific Antigen Level
This is the result, in nanograms per mililiter, of the PSA blood test. PSA has to be between 2 and 50 .
Family History of Prostate Cancer
Choose Yes if a father, brother, or son had prostate cancer.
Digital Rectal Examination
Digital Rectal Examination is a test performed by a health care professional in which a gloved finger is placed in the rectum to feel the surface of the prostate. It is normal if the prostate is smooth and soft. It is abnormal if an area of firmness or a nodule is noted.
Prior Prostate Biopsy
What Is Transrectal Ultrasound
Transrectal ultrasound is the examination of prostate using a machine called ultrasound. We insert a finger like probe into the rectum to examine the prostate. Ultrasound creates a picture of prostate using high-frequency sound waves. These sound waves come out of the probe and are transmitted through body tissues. The sound waves then bounce off the tissue and return to the probe. These returning sound waves are called echoes and are translated and recorded into photographic images. Transrectal Ultrasonography provides excellent visualization of the prostate and abnormalities that may be present in the prostate. We can also easily guide the biopsy needle under ultrasound guidance into the prostate where cancer is suspected.
The ultrasound machines in our offices are capable of doing color doppler studies and three dimensional reconstruction of the gland. Usually there is increased blood flow within the cancerous lesion or adjacent to the lesion and color doppler helps us precisely guide the biopsy needle into the lesion for accurate biopsy.
Transrectal ultrasonography is also used to estimate the prostate volume accurately to calculate PSA density.
Transrectal ultrasonography also provides images sensitive enough to defect capsular involvement and extention of cancer into the seminal vesicles .
Recommended Reading: Best Scan For Prostate Cancer
What Are The Symptoms Of Prostate Cancer
Early-stage prostate cancer rarely causes symptoms. These problems may occur as the disease progresses:
- Frequent, sometimes urgent, need to urinate, especially at night.
- Weak urine flow or flow that starts and stops.
- Painful urination .
- Painful ejaculation and erectile dysfunction .
- Blood in semen or urine.
- Lower back pain, hip pain and chest pain.
- Leg or feet numbness.
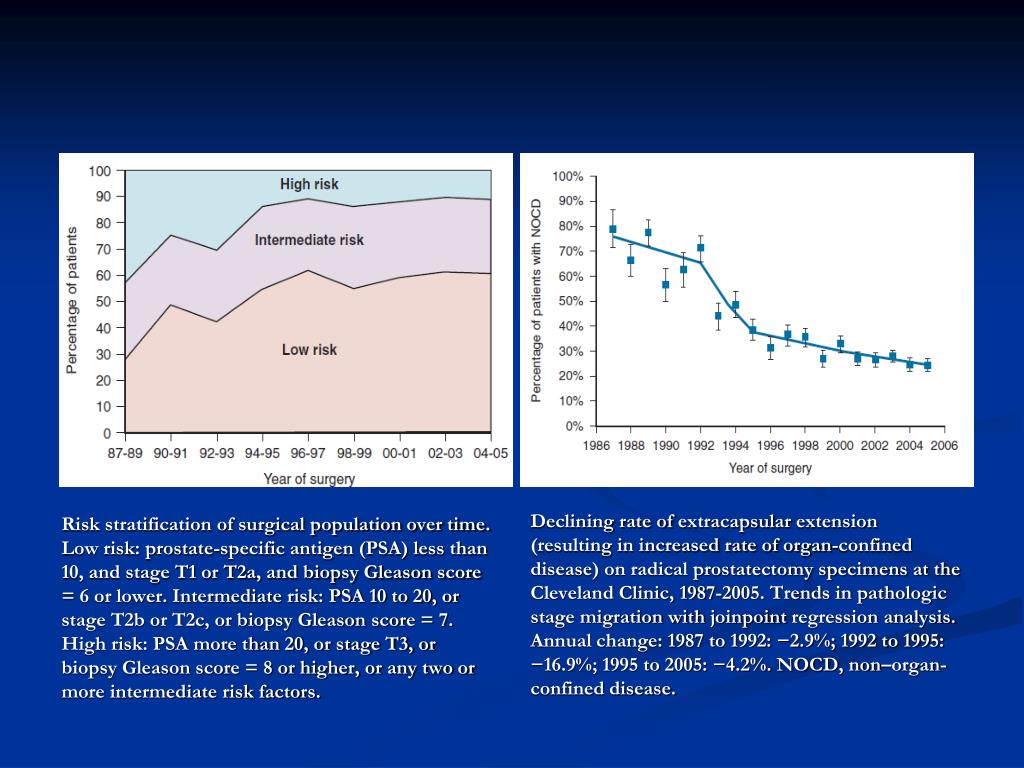
Risk Of Dying Of Prostate Cancer In Men With A Rising Psa After Radical Prostatectomy
This nomogram can be used by patients to estimate the risk of dying of prostate cancer if their cancer recurs, signaled by a rising PSA, after radical prostatectomy. The nomogram predicts the likelihood, in a man initially treated with surgery, that he will die of prostate cancer five, ten, and 15 years from the time his PSA begins to rise.
Read Also: Foods To Avoid With Prostate Issues
Evaluating The Prostate Cancer Prevention Trial High Grade Prostate Cancer Risk Calculator In 10 International Biopsy Cohorts: Results From The Prostate Biopsy Collaborative Group
- World Journal of Urology . Feb2014, Vol. 32 Issue 1, p185-191. 7p.
- Ankerst, Donna Boeck, Andreas Freedland, Stephen Stephen Jones, J. Cronin, Angel Roobol, Monique Hugosson, Jonas Kattan, Michael Klein, Eric Hamdy, Freddie Neal, David Donovan, Jenny Parekh, Dipen Klocker, Helmut Horninger, Wolfgang Benchikh, Amine Salama, Gilles Villers, Arnauld Moreira, Daniel Schröder, Fritz
For access to this entire article and additional high quality information, please check with your college/university library, local public library, or affiliated institution.
Important User Information: Remote access to EBSCO’s databases is permitted to patrons of subscribing institutions accessing from remote locations for personal, non-commercial use. However, remote access to EBSCO’s databases from non-subscribing institutions is not allowed if the purpose of the use is for commercial gain through cost reduction or avoidance for a non-subscribing institution.
When To Consider Genetic Counseling For Prostate Cancer
Experts recommend that men with a family history suggesting an increased risk of prostate cancer engage in shared decision-making with their physicians about genetic counseling and testing. Genetic testing can educate you about your inherited risk of prostate cancer, and it also can inform your family members that they may have genetic mutations that increase their cancer risk. Here are 7 factors that warrant a referral to a certified genetic counselor:
Journal of Clinical Oncology, Feb. 1, 2018).
This article originally appeared in Cleveland Clinic Mens Health Advisor.
Recommended Reading: Foods That Shrink Your Prostate
What Are The Stages Of Prostate Cancer
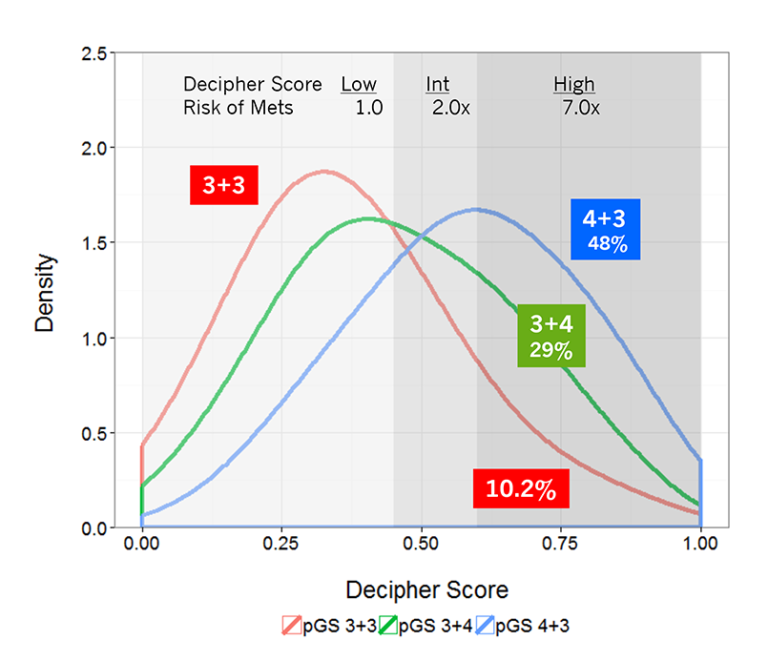
Your healthcare provider uses the Gleason score and Grade Groups to stage prostate cancer based on its projected aggressiveness. To get this information, the pathologist:
- Assigns a grade to each type of cell in your sample. Cells are graded on a scale of three to five . Samples that test in the one to two range are considered normal tissue.
- Adds together the two most common grades to get your Gleason score .
- Uses the Gleason score to place you into a Grade Group ranging from one to five. A Gleason score of six puts you in Grade Group 1 . A score of nine or higher puts you in Grade Group five . Samples with a higher portion of more aggressive cells receive a higher Grade Group.
Prostate Cancer Prevention Trial Risk Calculator Version 20
Disclaimer
The original Prostate Cancer Prevention Trial Prostate Cancer Risk Calculator posted in 2006 was developed based upon 5519 men in the placebo group of the Prostate Cancer Prevention Trial. All of these 5519 men initially had a prostate-specific antigen value less than or equal to 3.0 ng/ml and were followed for seven years with annual PSA and digital rectal examination . If PSA exceeded 4.0 ng/ml or if an abnormal DRE was noted, a biopsy was recommended. After seven years, all men were recommended to have a prostate biopsy, regardless of PSA or DRE findings. PSA, family history, DRE findings, and history of a prior negative prostate biopsy provided independent predictive value to the calculation of risk of a biopsy that showed presence of cancer.
The results of the PCPTRC may not apply to different groups of individuals. As about 80% of men had a prostate biopsy with six cores, if more than six cores are obtained at biopsy, a greater risk of cancer may be expected. Most men in this study were white and results may be different with other ethnicities or races. The calculator is in principle only applicable to men under the following restrictions:
- Age 55 or older
- No previous diagnosis of prostate cancer
- DRE and PSA results less than 1 year old
Don’t Miss: Vitamin D3 For Prostate Health
How Common Is Prostate Cancer
About one in nine men will receive a prostate cancer diagnosis during his lifetime. Prostate cancer is second only to skin cancer as the most common cancer affecting males. Close to 200,000 American men receive a diagnosis of prostate cancer every year. There are many successful treatments and some men dont need treatment at all. Still, approximately 33,000 men die from the disease every year.
What Is Prostate Intraepithelial Neoplasia Or Atypical Or Suspicious Cells On Biopsy
In about 10% of prostate needle biopsy reports, the pathologist will tell us that the final diagnosis is neither benign nor malignant. They describe this condition as
- High Grade Intraepithelial Neoplasia
- A premalignant condition
- Biopsy should be repeated soon
- 25% risk of cancer on repeat biopsy
- Low Grade Intraepithelial Neoplasia
- Repeat biopsy is not indicated unless there is a rise in PSA
- Atypia
Read Also: Castration Resistant Prostate Cancer Treatment
When Prostate Cancer Risk Is All In The Family
Your familial risk of prostate cancer is greatest if you have a first-degree relative who had the disease, especially if they were diagnosed at a relatively young age. Having multiple first degree relatives with prostate cancer also increases risk. Having multiple second-degree relatives and third-degree relatives adds to the risk, Carroll explains. Its more concerning when we see all cancers on one side of the family, in one blood line, she adds.
In one study, researchers found that men with a brother who had prostate cancer were more than twice as likely as men in the general population to be diagnosed with the disease themselves, and they faced nearly twice the risk of developing aggressive prostate cancer by age 75. Also, men with both a father and brother who had prostate cancer faced about a threefold greater risk of prostate cancer and developing aggressive disease by age 75 compared with the general population.