How Will Prostate Surgery Affect My Sex Life
Experienced robotic surgeons like Dr. David Samadi dont open the endopelvic fascia during surgery, which spares the rick of damage to nerve bundles that control sexual function. The recovery of the function, however, is not immediate and you should not feel discouraged if weeks or even a few months after surgery you experience erectile dysfunction. It is not an indication of long-term damage.
One major change that you will notice in your sex life is the absence of sperm. Having no prostate, the body will not produce semen during the orgasm. The sperm cells will be simply reabsorbed by the body them. This is not harmful and you shouldnt be worried about it. Plenty of men deal with the problem with the help of medication that improves erectile dysfunction.
Can Prostate Surgery Affect Penis Size Or Sensitivity
Prostate surgery is very unlikely to affect penis size. The only likely case this would occur if an individual underwent surgery for ED after prostate surgery. Implants will often cause a slight shortening of the penis.
Sensitivity, however, is an issue. In order to allow men to urinate, they have to operate on the prostate.
Its right next to the bundle of nerves that relay the sensation to the brain, causing a lot of the physical pleasure that men experience during sex.
It used to be the case that a prostatectomy would almost always damage those nerves, causing a permanent decrease or even loss of sensation. It would often be 8 months to a year before men reported any sense of sexual desire after the surgery.
However, nerve-sparing surgeries, particularly robotic prostatectomies, can avoid that nerve group far more effectively.
Its never a guarantee, but a majority of men who have undergone a nerve-sparing procedure can expect to regain the majority of the sexual desire and sensation they had before the operation.
For less-involved surgeries, men can expect to regain their sexual function a lot sooner. TURPs, ReZum, Aquablation or various other novel surgeries are all less likely to damage nerves and have faster recovery periods.
Dont Miss: Does Cialis Shrink The Prostate
What Happens After Urethral Sling Surgery
Patients usually recover from this surgery quickly. It’s best to limit demanding activities for approximately six weeks after surgery to avoid having the sling loosen before healing is complete.
After surgery, there may be swelling that makes it difficult to urinate. You’ll have a catheter coming out of the urethra for two to three days. After this, the catheter is removed and just about everyone is able to void on their own. In rare cases, the catheter may have to be reinserted for a few days or up to a week if you cannot urinate.
After the swelling goes down, youll gradually be able to urinate on your own and empty your bladder. However, your normal urination pattern may not return for a few weeks.
The majority of men who’ve had this procedure have been cured of their urinary incontinence and no longer use pads. The others usually improve to the point where they don’t use as many pads as they were before.
Last reviewed by a Cleveland Clinic medical professional on 10/31/2020.
References
Also Check: Foods That Irritate The Prostate
How Do Doctors Perform Prostate Removal
During prostate removal the prostate gland and some tissue around the gland, including the seminal vesicles, are removed. A prostatectomy takes about two hours and is performed under general anesthesia.
There are two approaches used for a prostatectomy:
- Robotic surgery
- Minimally invasive procedure with faster recovery time
- Uses smaller incisions and robotic technology
The surgical process is as follows:
- The doctor will make a small incision to gain access to the prostate
- The prostate is removed
- The bladder is reconnected to the urethra
- A catheter is connected to the bladder to allow urine to drain while the area heals
Prostate Removal: 8 Things To Know
Recommended Reading: Blood In Urine After Radiation For Prostate Cancer
What Changes Do I Need To Make To My Diet
Discuss your post-surgery diet with your doctor as you will probably want to avoid or at least minimize issues such as constipation. The lack of exercise, the medication, even the stress, might affect your bowel functions. Your diet will be focused on eating more vegetables, fruits, grains and avoiding meat, especially the red one, pasta, alcohol, fast-food, sugar and processed desserts.
Also Check: What Is Perineural Invasion In Prostate Cancer
What Are Pelvic Floor Exercises And Can Improve Erection Quality
As we age, we lose muscle tone throughout your body. That includes the muscles that men need to maintain erections. However, there are physical exercises men can do to reduce erectile dysfunction. The best ones are known as pelvic floor exercises or kegels.
Those muscles are the core of how your body maintains blood flow to the penis and therefore keeps erections strong.
They put pressure on the veins in your penis, preventing blood from flowing back into the rest of your body. If they arent strong enough then even if you can get an erection, you wont be able to keep it.
The process starts with identifying the muscles you need to activate. Thats best achieved by lying down with knees bent and feet flat on the floor. Thats when you breathe out and squeeze your pelvic floor muscles for 3 seconds.
Its important that you identify the right group, at the base of your buttocks, on either side of your perineum. It can be easy to mistake other muscles, such as the legs or stomach for the pelvic floor.
Once you are confident you have the right muscle group, then doing the exercises in a seated or standing position three times a day can firm and strengthen the muscles, with a likely improvement within four to six weeks.
Some men find that after the initial strengthening that options like Pilates become appealing as not only are there many exercises which improve the pelvic floor, but they can improve overall posture and strength.
Also Check: What Is The Definition Of Prostate Gland
Also Check: Hdr Brachytherapy Prostate Cancer Side Effects
What Is An Artificial Urinary Sphincter And How Does It Help With Urinary Incontinence
An artificial urinary sphincter can help men who have moderate to severe urinary incontinence due to poorly functioning muscle or sphincter valve after prostate cancer surgery.
The AUS has three parts:
- An inflatable cuff that is placed around the upper urethra. The cuff closes off the urethra to prevent leakage of urine.
- A pump that is inserted into the scrotum. It’s completely on the inside and not visible, and the pump controls the opening and closing of the cuff.
- A small pressure-regulating balloon that is placed in the abdomen, under the muscles. The balloon maintains fluid under pressure within the urethral cuff to pressurize the system and hold urine back.
If you have this surgery, youll press on the pump when you feel the need to pee. This opens the cuff to allow urine to pass. When youre done peeing, the cuff automatically closes again on its own.
The AUS procedure provides a very good and satisfactory result in 90% of cases. Risks are uncommon and include:
- Failure of the device .
- Erosion of the cuff into the urethra.
- Infection.
All of these would require additional surgery.
Side Effects From Radiation
Urinary symptoms from radiation treatment for prostate cancer are different from those caused by prostate surgery. Its more like a urinary tract infection-increased urgency and frequency, and men may some have bleeding or pain when they urinate, Calvaresi said. These problems often go away once treatment is complete.
Radiation also may cause bowel changes, such as constipation, loose stools or both. These can be managed by over-the-counter medication. Men may also see some blood in their stool during treatment-if so, let your health care provider know about this.
Men undergoing radiation are likely to have ED, but not immediately. It slowly sets in after radiation treatment, Calvaresi said. Treatments for radiation-related ED are the same as ED caused by prostate cancer surgery.
Read Also: What Are The Grades Of Prostate Cancer
Why The Procedure Is Performed
Radical prostatectomy is most often done when the cancer has not spread beyond the prostate gland. This is called localized prostate cancer.
Your doctor may recommend one treatment for you because of what is known about your type of cancer and your risk factors. Or, your doctor may talk with you about other treatments that could be good for your cancer. These treatments may be used instead of surgery or after surgery has been performed.
Factors to consider when choosing a type of surgery include your age and other medical problems. This surgery is often done on healthy men who are expected to live for 10 or more years after the procedure.
Can You Still Have An Erection If Your Prostate Is Removed
When you have a radical prostatectomy , you have surgery to remove your prostate gland. These nerves, blood vessels, and muscles may be weakened when you have surgery for your prostate cancer. For a period of time after surgery , many men are not able to get an erection . This time is different for each man.
Read Also: Radiation For Metastatic Prostate Cancer
How Bad Is The Pain After Prostate Surgery
The level of pain is lower than that of open prostatectomy, due to smaller incisions. However, you will be administered pain medication both orally and intravenously, through an IV. Make sure you have someone to pick you up from the hospital, as you wont be able to drive right away. Ask your doctor to recommend some pain medication and dosages that you can take from home most common ones are Tylenol or Ibuprofen. Even though the recovery is fast, you should get plenty of rest and not force yourself with lifting weights or exercises in the first few weeks.
Risks Of Prostate Surgery

The risks with any type of radical prostatectomy are much like those of any major surgery. Problems during or shortly after the operation can include:
- Reactions to anesthesia
- Blood clots in the legs or lungs
- Damage to nearby organs
- Infections at the surgery site.
Rarely, part of the intestine might be injured during surgery, which could lead to infections in the abdomen and might require more surgery to fix. Injuries to the intestines are more common with laparoscopic and robotic surgeries than with the open approach.
If lymph nodes are removed, a collection of lymph fluid can form and may need to be drained.
In extremely rare cases, a man can die because of complications of this operation. Your risk depends, in part, on your overall health, your age, and the skill of your surgical team.
Recommended Reading: Prostate Cancer Family History Risk
What You Need To Know About Prostate Surgery
What is prostate surgery for?
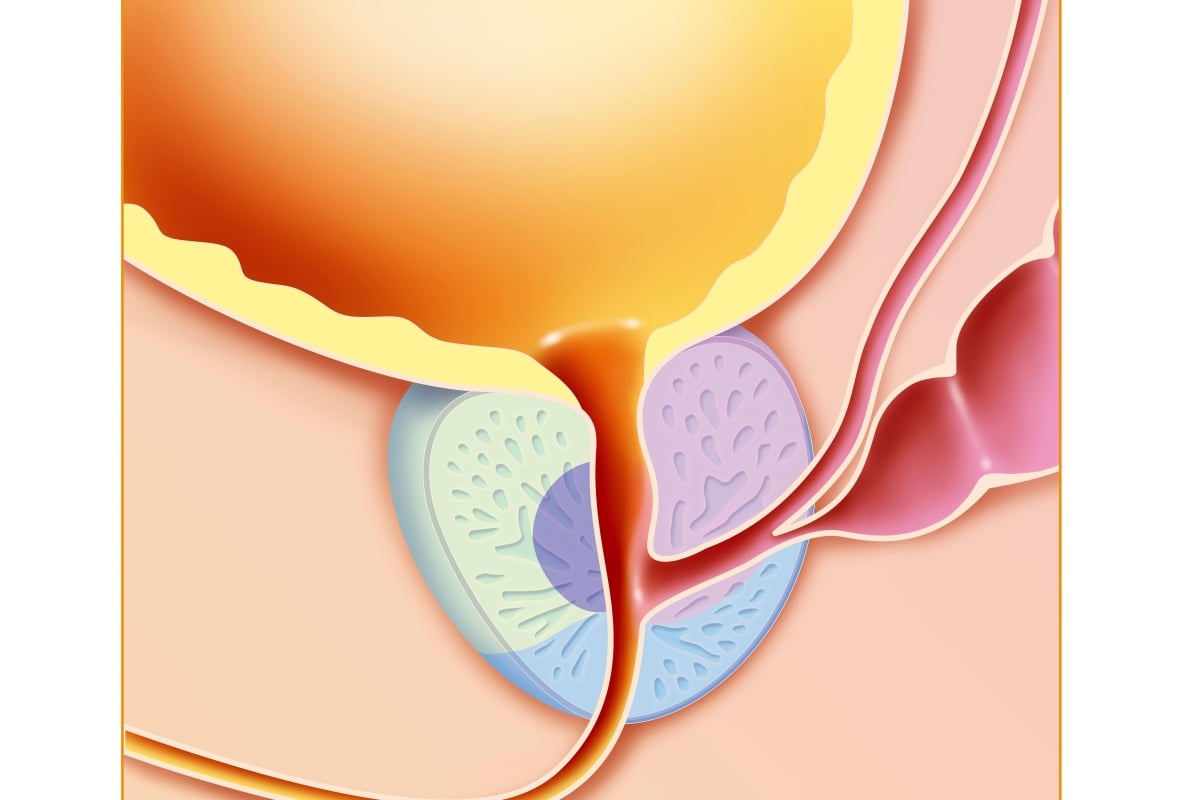
The prostate is a gland located underneath the bladder, in front of the rectum. It plays an important role in the part of the male reproductive system that produces fluids that carry sperm.
Surgery for partial or complete removal of the prostate is called a prostatectomy. The most common causes for prostate surgery are prostate cancer and an enlarged prostate, or benign prostatic hyperplasia .
Pretreatment education is the first step to making a decisions about your treatment. All types of prostate surgery can be done with general anesthesia, which puts you to sleep, or spinal anesthesia, which numbs the lower half of your body.
Your doctor will recommend a type of anesthesia based on your situation.
The goal of your surgery is to:
- cure your condition
- maintain the ability to have erections
- minimize side effects
- minimize pain before, during, and after surgery
Read on to learn more about the types of surgery, risks, and recovery.
The goal of prostate surgery also depends on your condition. For example, the goal of prostate cancer surgery is to remove cancerous tissue. The goal of BPH surgery is to remove prostate tissue and restore the normal flow of urine.
Side Effects Of Prostate Surgery
The major possible side effects of radical prostatectomy are urinary incontinence and erectile dysfunction . These side effects can also occur with other forms of prostate cancer treatment.
Urinary incontinence: You may not be able to control your urine or you may have leakage or dribbling. Being incontinent can affect you not only physically but emotionally and socially as well. These are the major types of incontinence:
- Men with stress incontinence might leak urine when they cough, laugh, sneeze, or exercise. Stress incontinence is the most common type after prostate surgery. It’s usually caused by problems with the valve that keeps urine in the bladder . Prostate cancer treatments can damage this valve or the nerves that keep the valve working.
- Men with overflow incontinence have trouble emptying their bladder. They take a long time to urinate and have a dribbling stream with little force. Overflow incontinence is usually caused by blockage or narrowing of the bladder outlet by scar tissue.
- Men with urge incontinencehave a sudden need to urinate. This happens when the bladder becomes too sensitive to stretching as it fills with urine.
- Rarely after surgery, men lose all ability to control their urine. This is called continuous incontinence.
After surgery for prostate cancer, normal bladder control usually returns within several weeks or months. This recovery usually occurs slowly over time.
There are several options for treating erectile dysfunction:
Recommended Reading: What Does An Mri Of The Prostate Show
How Long After Prostate Surgery Does Impotence Last
While ED is common right after prostate surgery, you may regain sexual function after some time. This may range from several months to 2 years . Also, remember that ED can be treated. By working with your doctor, you will be able to recover from prostate surgery and find an effective ED treatment that is right for you.
How Is Urinary Incontinence After Prostate Surgery Treated
If you find youre having issues with mild to moderate leakage after surgery, your healthcare provider might suggest starting with noninvasive therapies like medications or physical therapy exercises for the pelvic floor muscles. These treatments may also cut down on the number of times that you have to get up each night to pee.
These methods can sometimes help men who have mild to moderate leakage. Men who have persistent leakage or a more severe problem may need surgery if they do not want to continue to use pads.
Also Check: How Long Can You Live With Gleason 7 Prostate Cancer
What Can I As A Partner Expect
One of the effects of prostate cancer treatment is erectile dysfunction or impotence. This means that your partner may not be able to have erections that are hard enough for him to have sex with you or that he may not be interested in sex because of the medicine he is taking to treat his prostate cancer. This affects not only the man, but you, too, as his intimate partner. If you are the partner of a man with erectile dysfunction, it can be difficult to cope with changes in your sexual relationship. Sometimes men struggle to come to terms with changes in their body image or their ability to perform sexually. This can sometimes result in him staying away from intimate situations where he may feel under pressure to make love. As a partner you may feel rejected by what seems like a lack of sexual interest or intimacy. This may not have anything to do with his feelings for you, but is a result of his cancer treatment. Erectile dysfunction can be difficult for both of you. You may want to reassure your partner that:
- Sex is not as important as long as he is healthy and that he is no less of a man to you
- You will work through it with him
- You understand his feelings
- He is important to you
It may help if you explain to your partner how important nonsexual touching and intimacy such as kissing and cuddling is to you.
Open Radical Prostatectomy Vs Minimally Invasive Radical Prostatectomy
In 2003, only 9.2% of radical prostatectomies were done using a minimally invasive procedure. By 2007, that number had jumped to 43.2%. In 2009, researchers in Boston reported on a study that compared outcomes, benefits, and complications of open surgery vs. minimally invasive surgery:
- No difference was found in deaths or in the need for additional cancer therapy between the two approaches.
- The median hospital stay was two days for minimally invasive surgery and three days for open surgery.
- 2.7% of men having laparoscopic surgery required a blood transfusion compared with 20.8% of men having open surgery.
- There was more anastomotic stricture — narrowing of the suture where internal body parts are rejoined — for open surgery than for minimally invasive surgery .
- There were fewer respiratory complications with minimally invasive surgery than with open surgery .
- There were lower rates of incontinence and erectile dysfunction with open surgery. The overall rate was 4.7% for laparoscopic surgery and 2.1% for open surgery.
Also Check: Fiducial Markers For Prostate Cancer