Imaging Tests For Prostate Cancer
Imaging tests use x-rays, magnetic fields, sound waves, or radioactive substances to create pictures of the inside of your body. One or more imaging tests might be used:
- To look for cancer in the prostate
- To help the doctor see the prostate during certain procedures
- To look for spread of prostate cancer to other parts of the body
Which tests you might need will depend on the situation. For example, a prostate biopsy is typically done with transrectal ultrasound and/or MRI to help guide the biopsy. If you are found to have prostate cancer, you might need imaging tests of other parts of your body to look for possible cancer spread.
The imaging tests used most often to look for prostate cancer spread include:
Choice Of Biopsy Procedure
There are two classical procedures for the Biopsy. They are called Transperineal and Transrectal. The second of these is used far more often than the first one as it is easier to perform. A device is inserted into the rectum and the prostate tissue samples are obtained by firing a needle through the rectum wall and into the prostate gland. Unfortunately, in a small number of cases about 1 in 50 material from the rectum mixes with the prostate tissue and can cause severe side effects, leading to the patient having to be treated in an Intensive Care Unit. Indeed, rarely, death can result.
However, if the patient chooses the Transperineal biopsy, the samples are taken through the Perineum, and this does not result in any dangerous transfer of tissue to the prostate gland.
You should discuss this with your Urologist. In my case, as this procedure came early on, and I did not have sufficient knowledge, my biopsy was by means of the Transrectal Procedure. However, fortunately I have had no negative symptoms from my biopsy.
What Do You Say To Patients Diagnosed With Prostate Cancer
Something I say to my patients a lot is that, in treating prostate cancer, we end up trying to extend your quantity of life at the cost of your quality of life. And so, at some point, if the quantity is extended a lot, and we can minimize the effect on quality, that makes sense, but the equation is different for every man. How much decrease in quality of life are you willing to accept if were going to extend your life?
Realistically, a lot of guys who are 70 dont have any sexual function anyway, so thats not a huge loss for them. As men get older theres definitely an increased chance of having erectile dysfunction the guys who have sexual function over 70 are very keen on preserving it. Even for the guys who dont have good sexual function, who are on Viagra, for them its often even more important to preserve what sexual function they have.
Also Check: How Successful Is Radiation Therapy For Prostate Cancer
What Is A Digital Rectal Exam
The most common way for doctors to check on the health of your prostate is with a DRE. Its a fairly quick and simple procedure.
For the exam, youll bend at the waist while standing or lie on your side with your knees bent toward your chest.
Your doctor will lubricate a gloved finger and gently place it inside your rectum. Theyll press one hand on your prostate, and their other hand will feel your pelvic area. It should only take a few moments.
You may experience momentary discomfort. You may also feel the urge to urinate, especially if your prostate is enlarged or inflamed.
Your doctor will be able to tell you if your prostate seems to be a normal size and shape. In general, a DRE has no risks.
What Will I Experience During And After The Procedure
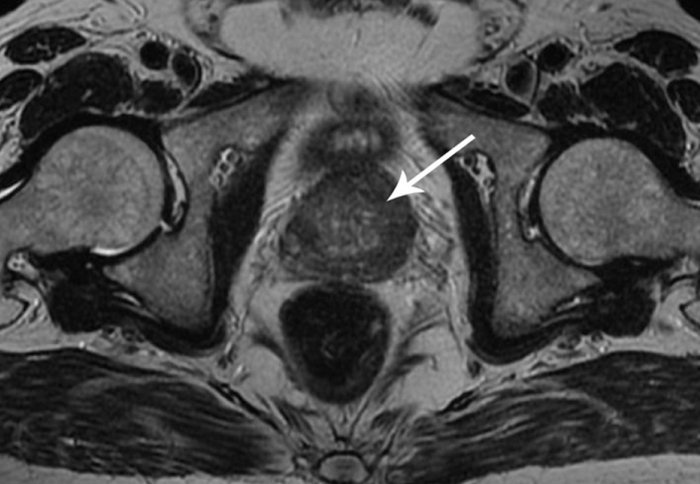
Most MRI exams are painless. However, some patients find it uncomfortable to remain still. Others may feel closed-in while in the MRI scanner. The scanner can be noisy. Sedation may be arranged for anxious patients, but fewer than one in 20 require it.
You may feel pressure while the doctor inserts the endorectal coil into your rectum. This is similar to that experienced during a digital rectal exam.
It is normal for the area of your body being imaged to feel slightly warm, but if it bothers you, notify the radiologist or technologist. It is important that you remain perfectly still while the images are being recorded, which is typically only a few seconds to a few minutes at a time. For some types of exams, you may be asked to hold your breath. You will know when images are being recorded because you will hear tapping or thumping sounds when the coils that generate the radiofrequency pulses are activated. You will be able to relax between imaging sequences, but will be asked to maintain your position as much as possible.
You will usually be alone in the exam room during the MRI procedure. However, the technologist will be able to see, hear and speak with you at all times using a two-way intercom. Many MRI centers allow a friend or parent to stay in the room as long as they are also screened for safety in the magnetic environment.
Recommended Reading: Icd 10 Code For Prostate Cancer
Use In Men Already Diagnosed With Prostate Cancer
The PSA test can also be useful if you have already been diagnosed with prostate cancer.
- In men just diagnosed with prostate cancer, the PSA level can be used together with physical exam results and tumor grade to help decide if other tests are needed.
- The PSA level is used to help determine the stage of your cancer. This can affect your treatment options, since some treatments are not likely to be helpful if the cancer has spread to other parts of the body.
- PSA tests are often an important part of determining how well treatment is working, as well as in watching for a possible recurrence of the cancer after treatment .
Study Shows Mri Can Help Detect Prostate Cancer More Accurately
The January 2017 study looked at the effect of using an MP-MRI earlier in the prostate cancer screening process. MP-MRI uses the same machine as other MRI imaging, but differs in that it uses multiple, specific imaging sequences to make a diagnosis instead of one essential MRI sequence.
In the study, patients with an elevated PSA level underwent a MP-MRI before having a biopsy. The investigators then performed a standard TRUS biopsy on the patients, as well as a comprehensive template biopsy under anesthesia. This template biopsy was used as the gold standard for which to compare the performance of standard biopsy versus the MRI findings.
The results were fairly dramatic. The study found that 27 percent of patients did not have MRI findings that would warrant a biopsy. Thanks to the MP-MRI, one in four men would avoid an unnecessary biopsy. For the patients who did need a biopsy, the MRI-guided biopsy found 93 percent of aggressive cancers, compared with just 48 percent when the biopsy was done at random.
Read Also: What Is A Good Psa Reading For Prostate
How We Screen For Prostate Cancer Now
Most prostate cancers are first detected when a patient is found to have an elevated prostate-specific antigen , which is a blood test used for prostate cancer screening. The prostate is a walnut-sized gland that produces the fluid in semen. PSA is a protein made in the prostate, and elevated levels often are found in men with prostate cancer.
There has been some controversy about when men should get PSA tests, but we follow the guidelines of the American Urological Association, which recommend patients and their doctors discuss the test at age:
- 55-69 for men at average risk
- 40-54 for men at higher risk for prostate cancer, such as black men and men with a family history of prostate cancer
- 70 and older for men in excellent health with a 10- to 15-year life expectancy
While a PSA test can give us a clue that something may be wrong, it isnt fool-proof. For example, the test can be elevated in patients who have benign enlargement of their prostate or prostatic inflammation. In such cases, the abnormal PSA test can lead to an unnecessary biopsy.
If your PSA levels are elevated, well likely perform a transrectal ultrasound-guided prostate biopsy to gather small samples of the prostate to examine in the lab. We use a transrectal ultrasound to visualize the prostate. Then we insert a small needle into the gland to remove about 12 samples from different parts of the prostate.
When Can I Expect The Results Of My Prostate Mri
The time that it takes your doctor to receive a written report on the test or procedure you have had will vary, depending on:
- the urgency with which the result is needed
- whether more information is needed from your doctor before the examination can be interpreted by the radiologist
- whether you have had previous X-rays or other medical imaging that need to be compared with this new test or procedure
- how the report is conveyed from the practice or hospital to your doctor .
Please feel free to ask the private practice, clinic or hospital where you are having your test or procedure when your doctor is likely to have the written report.
It is important that you discuss the results with the doctor who referred you, either in person or on the telephone, so that they can explain what the results mean for you.
Also Check: Prostate Cancer Treatments Covered By Medicare
Also Check: Radium 223 Treatment For Prostate Cancer
How To Tell If Your Cancer Has Metastasized
Prostate cancer metastasis may be suspected if you have specific symptoms such as new lower back pain or elevated liver enzymes. These may be signs your cancer has spread to your spine or your liver, respectively. If your prostate-specific antigen levels continue to rise despite treatment, especially if they are rising particularly fast, this may be a sign that cancer is metastasizing somewhere in your body.
Can Mri Detect Cancer
MRI scans can help medical professionals detect cancer. And whole-body magnetic resonance imaging has become available to the general public to screen for potential cancer.
If you find out early that you have a tumor or cancer, you can start treatment earlier, giving you a head start and improving your prognosis. This way, you also avoid more costly cancer treatment.
Oncologists use whole-body MRI more often to manage treatment for patients whose cancer is likely to metastasize to bone marrow, such as prostate and breast cancers. Oncologists and radiologists also use WB-MRI in lymphoma follow-up because of its superior diagnostics compared to positron emission tomography.
As an imaging tool, WB-MRI minimizes ionizing radiation exposure.
Read Also: Living With Metastatic Prostate Cancer
How Should I Prepare
The Night Before:
Avoid caffeine for 24 hours prior to the MRI. Do not have sexual relations 48 hours prior to your test. Sometimes, your physician would like you to wait 6 weeks after having a prostate biopsy to have a prostate MRI, this will ensure that the images are very clear.
Communicate with your technologist!
How long does an MRI take?The MRI takes around 45 minutes. Please be aware that you must hold still for the exam. Any motion causes the images to be blurry, which can reduce the detail of the images. If you have severe pain, you may want to discuss with your doctor about taking pain medication prior to the test so that you can hold still for the MRI. If you are claustrophobic or do not like smaller spaces, you may want to discuss with your doctor medication to help relax you during the MRI.
What does the equipment look like?
Medical History And Physical Exam
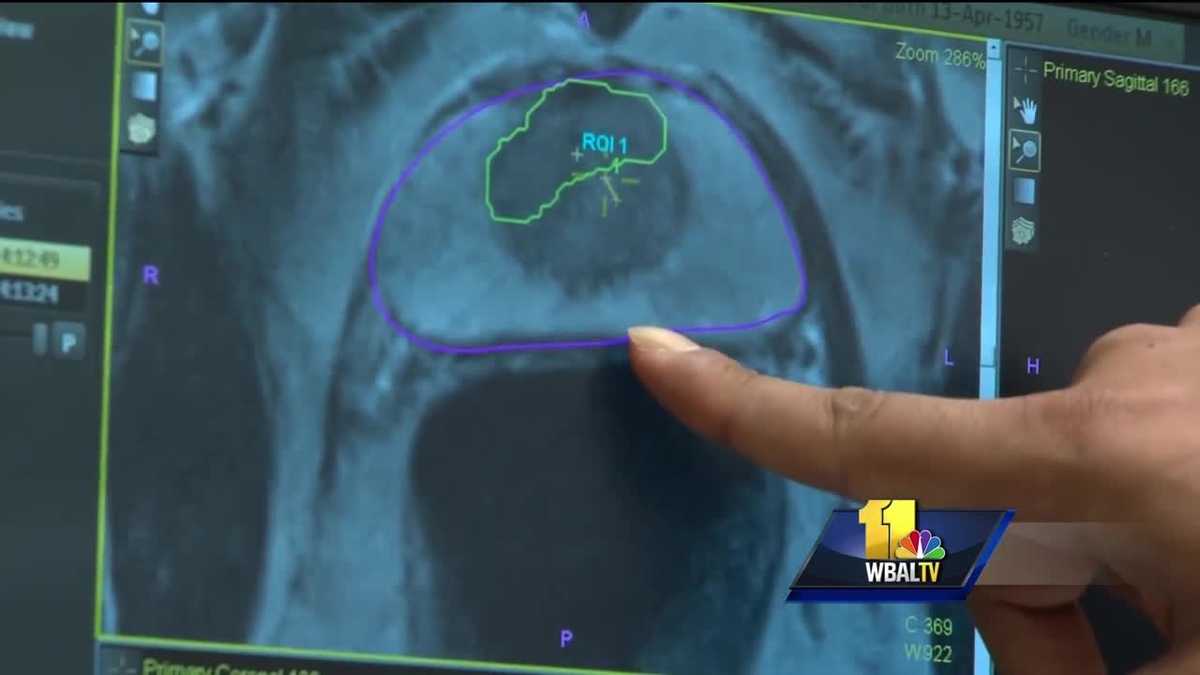
If your doctor suspects you might have prostate cancer, you will be asked about symptoms you are having, such as any urinary or sexual problems, and how long you have had them. You might also be asked about possible risk factors, including your family history.
Your doctor will also examine you. This might include a digital rectal exam , during which the doctor inserts a gloved, lubricated finger into your rectum to feel for any bumps or hard areas on the prostate that might be cancer. If you do have cancer, the DRE can sometimes help tell if its only on one side of the prostate, if its on both sides, or if its likely to have spread beyond the prostate to nearby tissues. Your doctor may also examine other areas of your body.
After the exam, your doctor might then order some tests.
Read Also: Chinese Medicine For Prostate Cancer
Preparing For Your Mri Scan
Before you go to your appointment, or when you arrive, you fill in a safety checklist. This asks about:
- any operations youve had
- whether you have any metal implants or other metals in your body
An MRI scan uses strong magnetism which could affect any metal in your body. This includes:
- pacemakers or an implantable defibrillator
- surgical clips, pins or plates
- cochlear implants
- metal fragments anywhere in your body for example from an injury, dental fillings and bridges
You can still have an MRI scan if you have some metals in your body, but your doctor and radiographer decide if its safe for you. Tell the scanner staff about any metals in your body.
Some people feel claustrophobic or closed in when theyre having an MRI scan. Contact the department before your test if youre likely to feel like this. The hospital staff can take extra care to make sure youre comfortable and that you understand whats going on. Your doctor can give you medicine to help you relax if you need to.
The radiographers let you know whether you need to empty your bowels of any poo or gas before having the scan. In some departments you might be given an enema. An enema is a liquid filled pouch that has a nozzle that you can put into your back passage and it helps to empty your bowels.
Role Of Mri In Screening For Prostate Cancer
The concept of screening a population for the purpose of finding a malignancy in its earliest stages of development, which could then allow selective, efficacious, and cost-effective treatment, is inherently attractive to patients and their physicians.
Population-based screening for prostate cancer has historically relied on prostate specific antigen blood testing and digital rectal examination . Injudicious screening of populations unlikely to benefit from diagnosis, adherence to monolithic PSA normal values to guide recommendations for prostate biopsy, and poor decision making by patients and physicians regarding treatment of disease of low malignant potential lead to concerns about the value of PSA-based screening.
The conclusions of the U.S. Prostate, Lung, Colorectal and Ovarian Cancer Screening Trial have been called into question based on high contamination rates for PSA screening in the control arm of the study.31 The European Randomized Study of Screening for Prostate Cancer has shown an increasing absolute risk reduction in prostate cancer mortality with increasing length of follow-up.32 In response to these results the United States Preventive Services Task Force has revised its negative recommendations regarding PSA screening.33 The current recommendation of the AUA is that men 5569 years of age should discuss with their physicians the relative risks and harms associated with PSA-based screening.34
Key Point
Read Also: What Is Malignant Neoplasm Of Prostate
What Is Colorectal Cancer
Colorectal cancer is a disease in which abnormal cells in the colon or rectum divide uncontrollably, ultimately forming a malignanttumor.
Parts of the colon. Drawing of the front of the abdomen that shows the four sections of the colon: the ascending colon, the transverse colon, the descending colon, and the sigmoid colon. Also shown are the small intestine, the cecum, and the rectum. The cecum, colon, rectum, and anal canal make up the large intestine. The cecum, ascending colon, and transverse colon make up the upper, or proximal, colon the descending colon and sigmoid colon make up the lower, or distal, colon.
Most colorectal cancers begin as a growth, or lesion, in the tissue that lines the inner surface of the colon or rectum. Lesions may appear as raised polyps, or, less commonly, they may appear flat or slightly indented. Raised polyps may be attached to the inner surface of the colon or rectum with a stalk , or they may grow along the surface without a stalk .
Colorectal polyps are common in people older than 50 years of age, and most do not become cancer. However, a certain type of polyp known as an adenoma is more likely to become a cancer.
Colorectal cancer is the third most common type of non-skin cancer in both men and women . It is the second leading cause of cancer death in the United States after lung cancer. In 2021, an estimated 149,500 people in the United States will be diagnosed with colorectal cancer and 52,980 people will die from it .
Less Than Half Of Men Get Colon Cancer Tests
Data came from a 2002 national phone survey of more than 22,000 men aged 50 and older.
About 61% of the men had stayed current with the PSA tests or a digital rectal exam to screen for prostate cancer. But only 48% had followed colorectal cancer screening guidelines for fecal occult blood test, sigmoidoscopy, or colonoscopy.
That means that a third of men who were good about getting PSA tests didnt make the same effort with colon cancer screening, the study explains.
Older men and black men were more likely to follow colon cancer testing guidelines. Health insurance, bigger paychecks, and higher education levels also helped.
Adherence to prostate cancer screening had the biggest influence on whether men underwent colon cancer screening. Men who adhered to prostate cancer screening were two to three times more likely to have had a colon cancer screening.
Hispanic men, smokers, and those who reported general good health were less likely to follow colon cancer screening guidelines, says the study, which appears in Februarys Journal of the American College of Surgeons.
The study was conducted by the University of Michigans Ruth Carlos, MD, MS, and colleagues.
Show Sources
Journal of the American College of Surgeons
Also Check: What Is Pae Prostate Procedure