What Is Prostate Cancer Screening
The diagnosis of prostate cancer usually follows a biopsy prompted by a significantly elevated initial PSA level, an increase in PSA levels over time, or an abnormal digital rectal examination. According to JAMA, patients with a prostate cancer history benefit from extended PSA monitoring. Elevated PSA levels may help determine when to go in for a prostate MRI and hopefully avoid unnecessary or repeat prostate biopsies.
The American Journal of Mens Health reports that prostate cancer diagnosis occurs most often in men older than 50. Other factors influencing the rate of prostate cancer are ethnicity and family history. Screening is vital because localized prostate cancer sometimes causes no symptoms or warning signs.
What New Biopsy Techniques Are Out There
Research is developing on other biopsy techniques that use MRIs. In this technique, doctors combine real-time ultrasound imaging with MRI data to guide a biopsy. A recent study published in the Journal of the American Medical Association that concludes using MRI with ultrasound produces better biopsy results1. This method aims to give a more accurate biopsy result while minimizing side effects including infection, bleeding, and potential damage to the urethra or nerves causing temporary incontinence and/or erectile dysfunction.
For men who have had a negative biopsy, there is a new test called ProMark. This helps to predict whether the next biopsy will also be negative, potentially cutting down on the number of biopsies a man will have to go through.
What Will Happen During A Prostate Biopsy
- You may need to lie on your side with your knees pulled up toward your chest. Numbing cream or gel may be put into your rectum or injected near your prostate. You may instead be given general anesthesia to keep you asleep and free from pain during the procedure. A biopsy sample may be taken through your rectum, urethra, or perineum. The perineum is the area between your scrotum and rectum. Most of the time, biopsy samples are taken through the rectum.
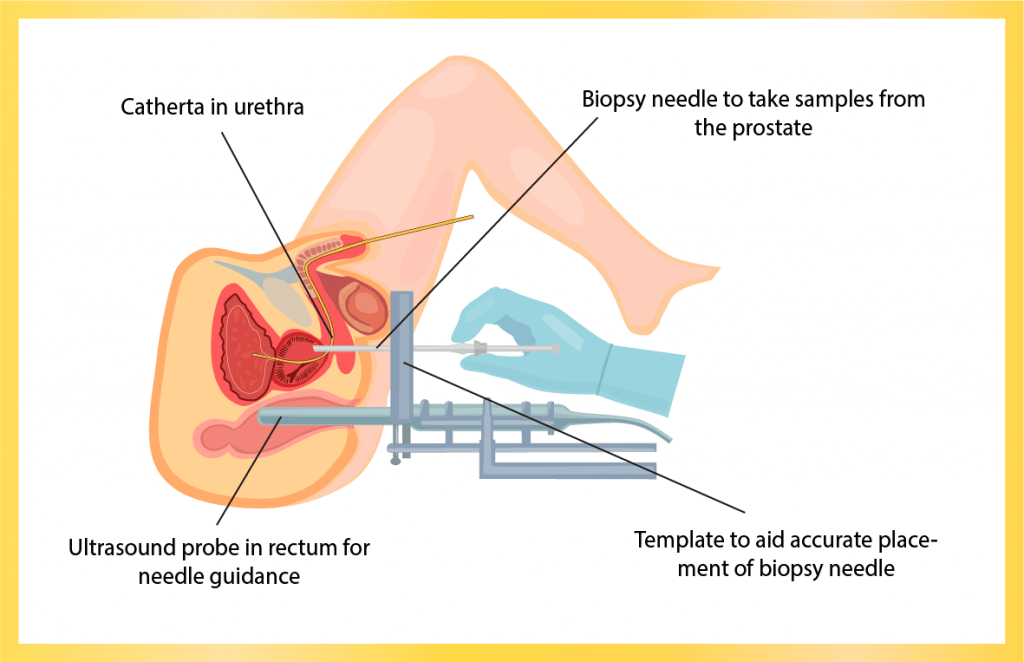
- Your healthcare provider may insert a small ultrasound probe into your rectum. The ultrasound shows pictures of your prostate on a monitor, and is used to help guide the biopsy needle. Your provider may instead use MRI pictures to guide the placement. He or she will push the biopsy needle through the wall of your rectum and into your prostate gland.
- Your provider will remove 6 to 12 samples of tissue from several areas of your prostate gland. The samples will be sent to a lab and tested for cancer.
You May Like: When To Start Prostate Screening
What Abnormal Results Mean
A positive biopsy result means that cancer cells have been found. The lab will give the cells a grade called a Gleason score. This helps predict how fast the cancer will grow. Your doctor will talk to you about your treatment options.
The biopsy may also show cells that look abnormal, but may or may not be cancer. Your provider will talk with you about what steps to take. You may need another biopsy.
Transrectal Biopsy Of The Prostate
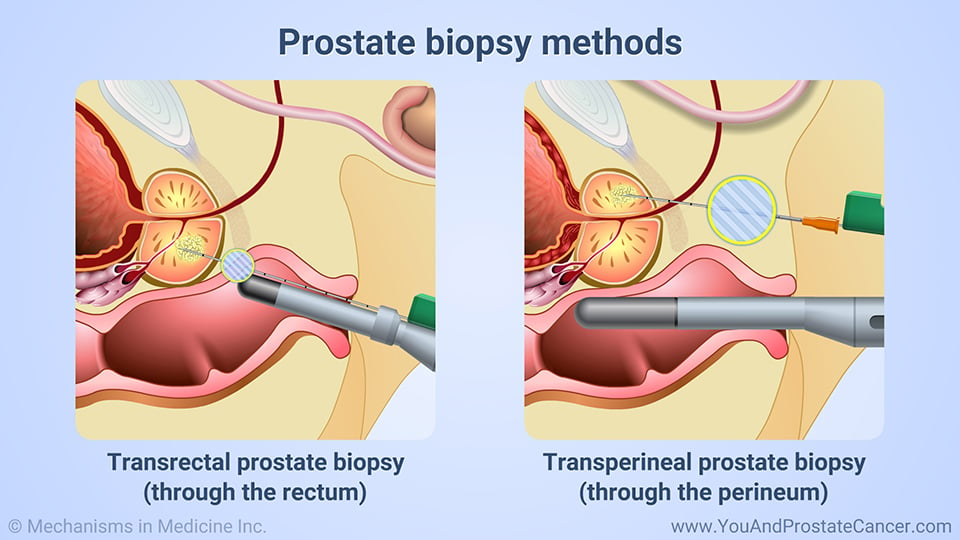
Today this procedure is usually carried out in the office of an experienced physician such as a urologist. However, it can also be carried out in a hospital or a day surgery center. It is commonly carried out with the accompanying use of a local anesthetic, but always ask the urologist if he or she is going to give you an anesthetic: prostate biopsy can quite often be painful without it.
The patient is asked to lie in one of several possible positions. The physician normally uses a special prostate biopsy gun to drive ultra-fine biopsy needles through the wall of the rectum and into the prostate. This gun is used in combination with a transrectal ultrasound probe, which enables the doctor to see where the biopsy needles are being placed into the prostate. Each hollow needle will remove a fine cylindrical core of prostate tissue in about a second.
This entire procedure, properly called transrectal ultrasound-guided prostate biopsy or TRUS-guided biopsy is usually completed in about 20 minutes, from start to finish.
The Number of Cores Removed
Many different theories exist as to the best way to sample the prostate so as to find any cancer that may be present. There are no absolute prostate biopsy guidelines. In general, however, an experienced physician will seek to take prostate biopsy specimens as follows:
Recommended Reading: Is Stage 3 Prostate Cancer Curable
How Doctors Determine Whether To Recommend A Prostate Biopsy
No two patients are alike, and a urologist needs to take many variables into account before recommending a prostate biopsy, including a patients:
- Age and life expectancy
- Comorbidities
- Change in PSA values across time.
The decision of whether to undergo a prostate biopsy should be determined after an individual conversation with your doctor during which he or she presents you with the big picture of your situation.
Compare, for example, the case of two 50-year-old men: One of them has been diagnosed with heart failure and is in poor overall health. The other has no pre-existing health conditions. I probably wouldnt advise a prostate biopsy for the 50-year-old with heart failure because prostate cancer is unlikely to cause his death within the next five years.
But I would recommend that the healthy 50-year-old get a prostate biopsy, because even if his cancer isnt aggressive right now, missing a prostate cancer diagnosis may result in his death from the disease in 15 years. In his case, it would be better to risk the prostate biopsy to catch the cancer early and improve his chances of long-term survival.
What Are The Risks Of A Prostate Biopsy
You may bleed more than expected or get an infection in your urinary tract or prostate gland. The infection may spread to your blood and the rest of your body. Your bladder may not empty completely when you urinate. You may need a catheter to help empty your bladder for a short period of time. Cancer cells may be missed during your biopsy procedure. You may need another prostate biopsy to check for cancer again.
You May Like: How Old Can You Be To Get Prostate Cancer
Genetic Testing For Some Men With Prostate Cancer
Some doctors now recommend that some men with prostate cancer be tested to look for certain inherited gene changes. This includes men in whom a family cancer syndrome is suspected, as well as men with prostate cancer that has certain high-risk features or that has spread to other parts of the body. Talk to your doctor about the possible pros, cons, and limitations of such testing.
The Test Is Often Not Needed
Most men with high PSAs dont have prostate cancer. Their high PSAs might be due to:
- An enlarged prostate gland.
- Recent sexual activity.
- A recent, long bike ride.
Up to 25% of men with high PSAs may have prostate cancer, depending on age and PSA level. But most of these cancers do not cause problems. It is common for older men to have some cancer cells in their prostate glands. These cancers are usually slow to grow. They are not likely to spread beyond the prostate. They usually dont cause symptoms, or death.
Studies show that routine PSA tests of 1,000 men ages 55 to 69 prevent one prostate cancer death. But the PSA also has risks.
Also Check: Can Prostate Cancer Cause Dizziness
Additional Tests That May Aid Prostate Cancer Diagnosis
There are few other diagnostic tools or tests, which can be performed before you have a prostate biopsy, that may help your physician gather more information about your specific case. These procedures may help determine the likelihood of the presence of cancer and its aggressiveness and increase the accuracy of a biopsy when performed. Those tests include:
4Kscore blood test is a molecular test that helps predict the likelihood and risk of a patient having aggressive prostate cancer. If you’re a patient whose PSA values are borderline for a prostate biopsy or you have a condition that could be aggravated by a biopsy, your physician may use this test before to help determine whether you should get a biopsy or a repeat biopsy.
Urine sample testlooks for biomarkers that may indicate the presence of prostate cancer cells in a patient’s body. This test may also be helpful when trying to determine whether a patient should be rebiopsied or not.
Multiparametric MRI
The use of multiparametric MRI imaging of the prostate gland before a biopsy has been a game changer in prostate cancer diagnosis, increasing the accuracy of biopsies over standard biopsies. The mpMRI doesn’t replace the standard biopsy, but by improving its accuracy, it may help decrease the number of biopsies needed.
The mpMRI has a higher resolution than a standard prostate ultrasound. This increases the ability to see suspicious lesions in the prostate, providing additional targets for the biopsy to sample.
Is A Prostatebiopsy Painful
A prostate biopsy is a surgical procedure, and what people feel after is very similar to what people feel after surgery. After any surgical procedure and when the anesthesia wears off, people feel pain. They need to use anti-inflammatory drugs to manage their symptoms, and the intensity is variable. You have people who manage their pain efficiently and others who are significantly affected by the symptom. Something similar happens after a prostate biopsy.
Anesthesia is not always used in a transrectal ultrasonography-guided biopsy. So, it might be a good idea to ask your doctor if hes going to use anesthesia or not. Certain studies show that theres no significant difference in pain symptoms with and without anesthesia. Others mention that anesthesia reduces the sensation of pain significantly. Due to diverging studies, anesthesia use is not explicitly written in the protocol, and some doctors prefer not to use it. However, it is essential to achieve adequate pain management in this procedure in any way or another. Ask your doctor what will be the method he will use to manage pain .
Don’t Miss: Best Prostate Over The Counter Medicine
Q: I Had Gleason Score 4+3 In One Area Of My Prostate And 3+4 In Another Is This Common
A: Yes. It is very common for men to have different Gleason scores in different areas of the prostate.
Its critical to personally research Prostate Cancer treatment options to make an informed decision that is best for you and your family. And, with few exceptions, your first treatment gives you the best chance for success.
Alternatives To A Prostatebiopsy
When you need a prostate biopsy to complete the diagnosis and the Gleason score, no other diagnostic tool has the same value. However, there is a gray zone, in which doctors are not sure if the patient has prostate cancer or not. Many patients in this gray zone undergo a prostate biopsy that could be avoided by considering other options.
Depending on your case, one of these alternatives could rule out the suspicion of prostate cancer and disregard the need for a prostate biopsy:
- Advanced PSA test measures such as PSA density or PSA velocity, especially in patients with known benign prostatic hyperplasia
- A prostate MRI scan to see a more detailed picture of the prostate
- Additional prostate markers such as PCA3, T2:ERG, and the MIPS prostate score
- Watchful waiting, which is recommended for some patients in the gray zone
Read Also: Prostate Cancer In Older Men
Prepare For The Immediate Complications
A prostate biopsy usually has the primary complication of bleeding. You can see blood in the urine, in the stool, or in your semen. Also, you may feel pain in your pelvic floor for up to one week. You need to understand before the procedure why this happens. That way, you will be able to tell when the bleeding is too much. Be sure to ask your doctor what to expect in your case.
Use In Men Who Might Have Prostate Cancer
The PSA blood test is used mainly to screen for prostate cancer in men without symptoms. Its also one of the first tests done in men who have symptoms that might be caused by prostate cancer.
PSA in the blood is measured in units called nanograms per milliliter . The chance of having prostate cancer goes up as the PSA level goes up, but there is no set cutoff point that can tell for sure if a man does or doesnt have prostate cancer. Many doctors use a PSA cutoff point of 4 ng/mL or higher when deciding if a man might need further testing, while others might recommend it starting at a lower level, such as 2.5 or 3.
- Most men without prostate cancer have PSA levels under 4 ng/mL of blood. Still, a level below 4 is not a guarantee that a man doesnt have cancer.
- Men with a PSA level between 4 and 10 have about a 1 in 4 chance of having prostate cancer.
- If the PSA is more than 10, the chance of having prostate cancer is over 50%.
If your PSA level is high, you might need further tests to look for prostate cancer.
To learn more about how the PSA test is used to look for cancer, including factors that can affect PSA levels, special types of PSA tests, and what the next steps might be if you have an abnormal PSA level, see Screening Tests for Prostate Cancer.
Recommended Reading: Digital Examination Of The Prostate
Isnt A Psa Test Enough
The prostate specific antigen test is a common screening test for prostate cancer. PSA is a protein that comes from the prostate gland. The test measures the amount of PSA in your blood. Its a simple blood test, and for some men, it turns out to be a lifesaver.
On the other hand, its value as a diagnostic tool is fairly limited. High PSA levels may be a sign of prostate cancer, but its not enough to diagnose the disease with certainty. Thats because there are other reasons your PSA levels could be high, including urinary tract infection and inflammation of the prostate.
Read more: PSA levels and prostate cancer staging »
Also, a single abnormally high PSA test result cant tell you if the high level is temporary or rising over time.
Low PSA levels cannot definitively rule out prostate cancer, either. The fact is that PSA tests can result in both false positives and false negatives.
PSA tests can be useful during and after treatment for prostate cancer. Rising PSA levels may signal that treatment is not effective or there is a recurrence of the cancer. If your PSA levels are decreasing, your current treatment is probably doing its job.
Controversies And Misconceptions Surrounding Prostate Biopsies
The PSA test measures the levels of PSA proteins in the body, and when it was first developed, it was quickly implemented by many physicians as a screening test for prostate cancer. The thought was that since PSA proteins are only produced by the prostate, elevated levels could be an indication of prostate cancer. As a result, most men with an abnormal PSA test underwent a prostate biopsy.
The increase in biopsies resulted in the number of advanced, untreatable prostate cancers decreasing significantly because more prostate cancers were caught earlier, when the disease is easier to treat. But the problem with many patients being diagnosed sooner was that some patients were being aggressively treated when they should have been monitored instead.
Though many in the field of urology believe it was flawed, a controversial study attempted to assess the benefits of the PSA test as a screening tool for prostate cancer, and its results led to the recommendation that most men shouldn’t get the test because it didnt appear to improve mortality rates from prostate cancer. This, combined with growing awareness that many cases of prostate cancer were being treated unnecessarily or prematurely, led to a reduction in prostate biopsies. This controversy led to a reduction in prostate cancer screening and an increase in the number of diagnoses of advanced prostate cancer.
Also Check: 10 Early Warning Signs Of Prostate Cancer
Prostate Biopsy Specimens: Ask For Meticulous Labeling
The way that prostate biopsy samples are handled varies among hospitals. The samples, or “cores,” are put onto glass slides to be examined under a microscope for signs of cancer. Find out if the physician doing the biopsy will place each core in a separate, labeled container. If cancer is discovered, its location in the prostate gland can affect decisions about further testing and possible treatment.
Individual labeling of biopsy cores is more expensive, and not all hospitals provide this level of service. “If all of the samples from the right and left side of the prostate gland are processed together, as opposed to individually, consider having the biopsy done elsewhere,” Dr. Garnick says.
What Will I Experience During And After The Biopsy
If you receive IV contrast for the MRI-guided procedure, you may feel coolness and a flushing sensation for a minute or two when the contrast material is injected. The intravenous needle may cause you some discomfort when it is inserted and you may experience some bruising once it is removed.
Rarely, patients may experience side effects from the MR contrast material, including nausea and local pain, hives, itchy eyes or other reactions. If you experience allergic symptoms, a radiologist or other physician will be available for immediate assistance.
When the ultrasound probe or endorectal coil is inserted into the rectum, you will feel pressure and may have some temporary discomfort.
You will hear a clicking noise when the biopsy needle samples the prostate, and you may feel a stinging or burning sensation in the area.
Some patients find it uncomfortable to remain still during MR imaging. Others experience a sense of being closed-in . Therefore, sedation can be arranged for those patients who anticipate anxiety.
If you feel heating on your skin at any time during MR imaging, the MR technician should be notified so that they can perform a closer examination of the area.
Some patients experience a small amount of bleeding from the rectum or perineum immediately after the biopsy procedure. If this occurs, it will cease with gentle pressure.
You may feel pain and discomfort in the area of the prostate for a day or two after the biopsy, particularly when you are seated.
You May Like: What Is The Best Over The Counter Prostate Supplement