Pni And Clinical Outcomes
During postoperative follow-up 14.9% of our population developed a biochemical progression while 5.9% progressed radiologically with no deaths. PNI positivity was significantly correlated with biochemical progression . In comparison to those without PNI, cases with PNI had a higher rate of biochemical relapse , radiological progression and local recurrence , while lymph-node or distant progression rates were low and independent of PNI status . Moreover, in PNI positive cases the percentage of biochemical progression increased if PNI was multifocal versus unifocal . Kaplan-Meier survival analysis showed that mean biochemical progression free survival was significantly lower in cases with PNI when compared with those without PNI . On the contrary, no significant differences in terms of mean radiological progression free survival were found according to PNI status . In the intermediate risk class, but not in the low and high risk classes , PNI was able to predict cases with lower mean biochemical progression free survival when compared to cases without PNI. In particular, within the intermediate risk class, cases with multifocal PNI showed significantly lower mean biochemical progression free survival when compared to cases without PNI .
Table 3Figure 2Figure 3
What Does It Mean If In Addition To Cancer My Biopsy Report Also Mentions Acute Inflammation Or Chronic Inflammation
Inflammation of the prostate is called prostatitis. Most cases of prostatitis reported on biopsy are not caused by infection and do not need to be treated. In some cases, inflammation may increase your PSA level, but it is not linked to prostate cancer. The finding of prostatitis on a biopsy of someone with prostate cancer does not affect their prognosis or the way the cancer is treated.
Correlation Among Pni Incidence And Clinical Parameters
Clinical parameters such as age, body mass index and preoperative PSA were not significantly different between cases with and without PNI . Additionally, the distribution of risk classes did not significantly differ with regard to PNI status . Pearson correlation analysis showed no significant correlation between PNI status and risk classes or mpMRI PI-RADS score distribution . There were a higher percentage of PI-RADS 45 cases which was independent of PNI status .
Table 2
Also Check: Hifu For Prostate Cancer Treatment
The Analysis Of Npy And Chromogranin Expression
Benign prostate and PCa cells showed NPY expression . As regards BP, only luminal cells were characterized by membrane apical expression and, rarely, weak cytoplasmic staining, with the negativity of basal cells . Cancer glands were characterized by both cytoplasmic and membrane staining with different intensity. Neuroendocrine cells in BP and PCa were NPY-positive, but the strongest staining was observed in case of autonomic nerve ganglia . Other compounds of the tumor stroma were negative. In 65.75% the staining was non-homogeneous. The results of immunostaining are presented in Table 3. We checked if the parameters of cancer innervation depended on NPY expression. The average of ND in PCa and the periphery was the same . However, a tendency towards lower ND was noted in the peripheral tumor area of PCa in tumors with a high NPY expression . In some cases NPY expression was higher in the peripheral area or in the proximity of the nerves. A high NPY expression in PNI area occurred more commonly in NPY-positive than NPY-negative cases . No correlation occurred between NPY and tumor stage , EPE , Grade Group , and ERG .
Table 3 The summary of chromogranin and NPY expression results.
Prognostic Significance Of Pni In Prostate Cancer
PNI is often associated with adverse clinicopathological parameters like Gleason score, prostate-specific antigen levels, or extraprostatic extension . As discussed for molecules and pathways involved in PNI, many studies also focus on the prognostic relevance of PNI. However, its significance as an independent predictive factor in PCa is still controversial. Several systematic reviews and meta-analyses suggest that PNI is, in fact, a significant prognostic factor for biochemical recurrence of localized PCa . A meta-analysis of 19 studies with a total of 13,412 patients showed a 1.4- or 1.2-fold increased risk of BCR in patients with PNI after radical prostatectomy or radiotherapy, respectively . Similar results, i.e., a significant adverse association of biopsy PNI with BCR-free survival, were also reported in other meta-analyses with smaller patient cohorts . However, systematic assessment of PNIs clinical significance is complicated by inconsistent PNI definition and substantial variation in PNI reporting. Therefore, despite the plethora of existing studies, the overall prognostic value of PNI remains unclear. The following paragraphs will highlight some of the problems identified within PNI studies and offer suggestions to increase comparability and thus improve clinical relevance.
Read Also: What’s Good For Prostate Problems
The Morphological Analysis Of Innervation
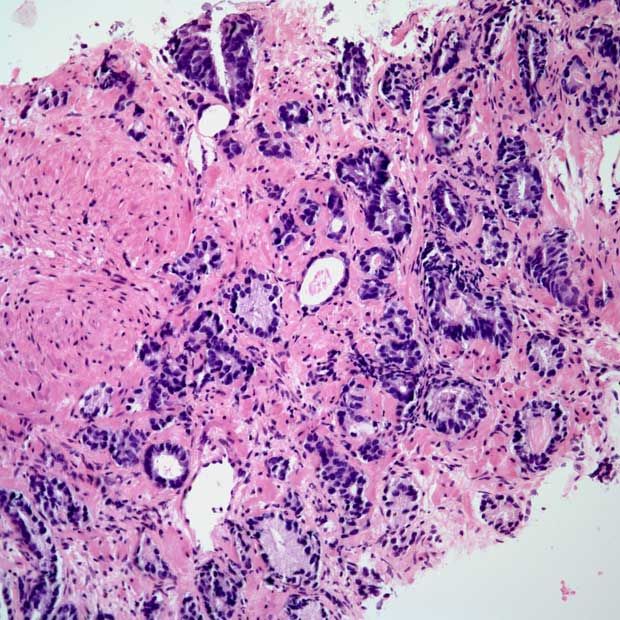
Figure 1 The morphology of perineural invasion and axonogenesis in PCa and the benign prostate. Different forms of perineural invasion and small nerves within the cancerous infiltration . Multiple axons and small nerves within the stroma of the benign prostate . Axons within the neoplastic infiltrate located in the stroma and surrounding cancer cells , . High neural density in the surrounding benign prostate with axons growing into the cancer tissue of high Gleason score PCa .
Figure 2 NPY, chromogranin, and ERG expression and perineural invasion in prostate cancer. Cytoplasmic-membranous NPY expression in neoplastic glands. Strong expression score . 200x Heterogenous intermediate NPY expression score and membranous apical immunostaining within the preexistent prostate glands . Chromogranin a strongly positive scattered single cell pattern . A high level of neuroendocrine differentiation within PCa . Nuclear ERG expression with diverse intensity within the cancer cells, positive endothelial cells, and immunonegative benign prostatic glands . A histological section of prostate cancer with focal perineural invasion and other invisible neural components of the microenvironment .
Slide Preparation And Digitization
The biopsy cores were formalin-fixed, stained with hematoxylin and eosin and mounted on glass slides. Histologic assessment was undertaken by the study pathologist , and pathological features including cancer grade and PNI were entered into a database. We then randomly selected 1427 participants from which we retrieved 8803 biopsy cores. The selection was stratified by grade to include a larger sample of high-grade cancers and also included all cases containing PNI . From these, we randomly assigned 20% of the subjects to a test set to evaluate PNI. The remaining 80% of subjects were used for developing and training the AI system.
Fig. 1
You May Like: Is Cialis Good For Enlarged Prostate
Data Extraction And Study Quality
The data of the eligible studies were extracted independently by two investigators . Any discrepancies were resolved by discussion with a third reviewer . The following data were extracted from the included studies: first author, year of publication, country, recruitment period, sample size, patients age, preoperative PSA level, Gleason score, pathological stage, positive percentage of PNI, definition of BCR, follow-up time and the HR of PNI for BCR. When the study provided the results of both the multivariate and univariate outcomes, we chose the multivariate model. The quality of the eligible studies was evaluated according to the Newcastle-Ottawa scale , which include 3 domains with 8 items. Studies with scores of 7 or more stars were considered high- quality studies.
Perineural Invasion And Risk Of Lethal Prostate Cancer
*Corresponding Author:
Note: M. Fiorentino and L.A. Mucci share senior authorship of this article.
Corresponding Author:
Cancer Epidemiol Biomarkers Prev
Piotr Zareba, Richard Flavin, Masis Isikbay, Jennifer R. Rider, Travis A. Gerke, Stephen Finn, Andreas Pettersson, Francesca Giunchi, Robert H. Unger, Alex M. Tinianow, Swen-Olof Andersson, Ove Andrén, Katja Fall, Michelangelo Fiorentino, Lorelei A. Mucci on behalf of the Transdisciplinary Prostate Cancer Partnership , Perineural Invasion and Risk of Lethal Prostate Cancer. Cancer Epidemiol Biomarkers Prev 1 May 2017 26 : 719726.
You May Like: Is Asparagus Good For Prostate Cancer
Is A Gleason 7 Capable Of Spreading
As explained by Dr. Klotz, whether or not a mans PSA levels increased fast was directly related to the quantity of Gleason 7 cancer present in the prostate. He predicts that when the research participants become older and are monitored for a longer period of time, a few more may get metastatic cancer.
Cox Regression Analysis For Pni Independent Prognostic Value
Cox regression analysis to identify predictors of biochemical progression in our population is displayed in Table 4. Univariate analysis had shown that PNI was a significant predictor of biochemical progression with a 2.33-fold higher risk when compared with cases without PNI . Other significant predictors of biochemical progression at univariate analysis were pathological stage, risk class, ISUP grading and surgical margins status. At multivariate analysis, after adjusting for pathological stage, grading and surgical margins, PNI was no longer a statistically significant predictor of biochemical progression .
Table 4
Also Check: 20 Year Survival Rate Prostate Cancer
Perineural Invasion Associated With Increased Cancer
Beard. IJROBP 2006 66:403
The significance of PNI with respect to prognosis after surgery has been inconsistently demonstrated, with some investigators showing a clear risk of upstaging, upgrading, or adverse outcomes in their PNI+ patients, and others showing no effect whatsoever. There is less information on the association between outcomes after RT and PNI, but theavailable data suggest that PNI is associated with unfavorable outcomes after RT. Previously, an unfavorable outcome was defined as freedom from PSA failure. To the best of our knowledge, this is the first report demonstrating a survival decrement in the PNI+ patient population. However, the results must be viewed as preliminary, given the small number of events, relatively short follow-up, and retrospective nature of the analysis.
Purpose: To identify an association between perineural invasion and cancer-specific survival in patients with prostate cancer after standard-dose external beam radiation therapy .
Results: At a median follow-up of 4.5 years, 84 patients have died, 15 of 84 from prostate cancer. PNI was the only significant predictor of prostate cancer-specific mortality after RT . The estimated prostate cancerspecific mortality was 14% at 8 years for PNI+ patients vs. 5% for PNI patients .
The Analysis Of Erg Expression

A total of 47.95% of studied PCa cases were ERG-positive . The analysis of ND in correlation with ERG status revealed that the mean of ND PGP 9.5 in the ERG+ group was higher than in ERG- group , but ND TH was similar in PCa . PNI was present four times more commonly in ERG-positive tumors than in ERG-negative ones . ERG positivity was associated with EPE , but it was not correlated with Grade Group , age , or angio- and lymphatic invasion .
Also Check: Gleason 8 Prostate Cancer Treatment
How Important Is The Gleason Score
The Gleason score is very important in predicting the behavior of a prostate cancer and determining the best treatment options. Still, other factors are also important, such as:
- The blood PSA level
- How much of each core is made up of cancer
- The number of cores that contain cancer
- Whether cancer was found in both sides of the prostate
- Whether the cancer has spread outside the prostate
Can The Gleason Score On My Biopsy Really Tell What The Cancer Grade Is In The Entire Prostate
Because prostate biopsies are tissue samples from different areas of the prostate, the Gleason score on biopsy usually reflects your cancers true grade. However, in about 1 out of 5 cases the biopsy grade is lower than the true grade because the biopsy misses a higher grade area of the cancer. It can work the other way, too, with the true grade of the tumor being lower than what is seen on the biopsy.
You May Like: Proton Treatment For Prostate Cancer
What Does It Mean When There Are Different Core Samples With Different Gleason Scores
Cores may be samples from different areas of the same tumor or different tumors in the prostate. Because the grade may vary within the same tumor or between different tumors, different samples taken from your prostate may have different Gleason scores. Typically, the highest Gleason score will be the one used by your doctor for predicting your prognosis and deciding on treatment options.
Perineural Invasion Linked With Prostate Cancer Bone Metastasis
Perineural invasion was a significant predictor of increased risk for bone metastases in men with prostate cancer who had suspicion for bone metastases after a whole-body bone scan.
Perineural invasion was a significant predictor of increased risk for bone metastases in men with prostate cancer who had suspicion for bone metastases after a whole-body bone scan , according to the results of a review in Prostate.
According to the review, clinicians currently have few factors that help to predict recurrence, prognosis or bone metastasis in men with prostate cancer. In addition to Gleason score, some research has suggested that PNI in the prostate specimen may indicate metastasis of the disease.
In this study, Seyfettin Ciftci, MD, of the Sivas Numune State Hospital, Sivas, Turkey, and colleagues reviewed data from 633 men with prostate cancer diagnosed with transrectal ultrasound guided prostate biopsy who underwent WBBS between 2008 and 2014. All men underwent WBBS and those whose scans returned suspicion for bone metastasis had a follow-up MRI.
Our results showed that PNI in the TRUS-Bx specimens is the most powerful predictive histopathological feature for bone metastasis, by increasing the risk of bone metastasis 11-fold in NCCN bone scan indicated patients, wrote the authors.
Patients positive for PNI had an 11-fold increased risk for bone metastases compared with men who were negative for PNI.
Related Content:
Also Check: Medication To Treat Prostate Cancer
Classification Of Perineural Invasion
PNI refers to a rare type of contiguous spread of neoplastic cells from their primary site along the potential space between or beneath the layers of perineurium . It is defined as âtumor in close proximity to nerve and involving at least 33% of its circumference or tumor cells within any of the three layers of the nerve sheath .â1 It was first described in 1952 by Dr. Frederick Mohs and Dr. Theodore Lathrop as âsilentâ extensions along the nerve sheath.2 Even though this phenomenon is frequently discussed in patients with primary head and neck malignancies, it is well defined in malignancies of the pancreas, prostate, and colorectum.3â8Perineural invasion can be broadly divided into two main categories based on the patientâs clinical presentation:
- â¢
-
Microscopic perineural invasion is the asymptomatic type where diagnosis is made on surveillance imaging, biopsy, or autopsy.
- â¢
-
Clinical perineural invasion is the symptomatic type .9,10
Another approach to their classification is to differentiate between the type and caliber of nerve that is involved:
- â¢
-
Perineural invasion is used to describe involvement of small, unnamed nerves around a tumor.
- â¢
-
Perineural spread is the term used when there is evidence of invasion and spread along a larger, named nerve or cranial nerves.11
Although both can result in symptoms, PNS is generally considered to be more aggressive and frequently presents with neuropathy of the affected nerve.12,13
After A Prostatectomy Why Does Psa Rise
The cancer cells may have spread outside of your prostate prior to your surgery. A few cancer cells might have survived the procedure if any were accidentally removed during the procedure. In the future, the cells may begin to divide. Your doctor may monitor your recovery after a prostatectomy by ordering periodic PSA tests.
Recommended Reading: Foods To Avoid When You Have Prostate Cancer
Chemokines Cytokines And Related Pathways
Plenty of studies have shown that various chemokines and cytokines play important roles in PNI. Chemokines released by nerves induce cancer cell migration and invasion towards nerves, indicating the significance of tumor-nerve interaction in PNI. For instance, CC-chemokine ligand 2 , well-known as an inflammatory chemokine, has been shown to promote the progression of many cancers, including PCa . The signaling axis of CCL2 and its receptor CC-chemokine receptor 2 facilitates PNI in PCa too. It has been reported that CCR2 expression in cancer cells accelerates PNI in the in vitro tumor-nerve co-culture invasion assays. Such effect was found to be significantly suppressed when the neurons were harvested from CCL2 knockout mice. Therefore, the nerve-released CCL2 interacts with cancer cell CCR2 to promote PNI and this CCR2-mediated signaling links to the MAPK and Akt pathway activity . Many other chemokines are also reported to be highly expressed in PNI tissue. They might have close connections with the development of PNI, such as CXCL12 and its receptor CXCR4 , CX3CL1 and the receptor CX3CR1 , and CXCL16 . However, a more detailed chemokine regulation network remains to be delineated.
Correlation Among Pni Incidence And Pathological Parameters
Presence of PNI was significantly correlated with unfavorable pathological parameters such as higher T stage and grade. In particular the percentage of localized PC at surgery without PNI was 81.4% vs. 39.6% in cases with PNI, whereas the percentage of extracapsular PC was 18.6% when PNI was absent versus 60.4% when it was present . The percentage of ISUP 1 PC was 52.3% in PNI negative specimens compared to 18.3% in PNI positive specimens . The percentage of positive surgical margins was slightly but not significantly higher in PNI positive than in PNI negative cases . In PNI positive cases, the distribution of pathological staging and ISUP grading did not vary according to the uni- or multifocality of PNI . Pearson correlation analysis showed a significant correlation between PNI status and pathological stage or ISUP grading .
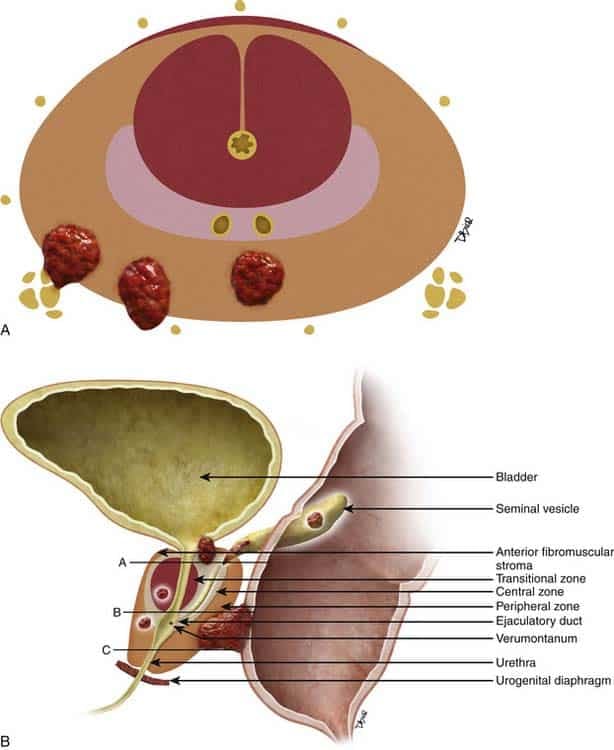
Figure 1
Read Also: How Big Is A Normal Prostate
The Initial Causes Perineural Invasion Prostate Cancer Treatment Radiation Or Surgery
One of the first symptoms of prostate issues is pain or tenderness in the groin or lower back. This can be the result of a noncancerous condition called enlarged prostatic tissue, or it could be an infection of the bladder. In either case, its important to see a doctor as soon as possible. If youre suffering from prostate pain, you may want to consider reducing your caffeine intake.
Another symptom of a potentially enlarged prostate is difficulty starting a stream of urine, leaking, or dribbling. These symptoms are not serious, but theyre still alarming. Most men put up with an enlarged prostate for years before seeking medical attention, but they typically seek treatment as soon as they notice symptoms. Even if you dont have symptoms, its worth getting checked to determine if you have any prostate issues.
If you experience nightly bathroom runs, you may be experiencing an enlarged prostate. You may be having difficulty starting a stream of urine, or you may even be dribbling or leaking during the day. These problems arent life-threatening, but can become a nuisance. You should not ignore these signs and seek treatment as soon as you notice them. If you feel any of these symptoms, you should consult a doctor.