Swelling Bruising Or Tenderness Of The Scrotum
Symptoms generally resolve on their own within three to five days. Oral anti-inflammatory medications such as ibuprofen are usually sufficient for pain relief, if necessary. You should avoid hot tubs and Jacuzzis for at least two to three days after the procedure. Postpone bike riding until the tenderness is gone.
Read Also: How To Have A Prostate Orgasim
Testosterone And Prostate Cancer What You Should Know
What is the relationship between testosterone and prostate cancer? Does testosterone stimulate the growth of prostate cancer? Lets answer the many questions surrounding the association between mens hormones and prostate cancer.
Starting with probably the single most common question that has been weighing on the minds of many scientists and medical professionals for decades:
Prostate Cancer Information: Prostate Cancer Hormone Therapy
Prostate cancer hormone therapy is the systemic ablation of the bodys testosterone which, for a period of time, will slow or stop the growth and spread of prostate cancer. Hormone therapy may also be called androgen deprivation or androgen ablation.
The Role of Hormones in Prostate Cancer The male sex hormone, testosterone, causes the growth of the prostate gland and other sex organs in the developing male. Even as men pass through the age of puberty, testosterone continues to contribute to the growth of the organ. Testosterone will fuel the growth of any prostatic cell: the chemical cannot discriminate between the receptors of healthy tissue and cancerous tissue. Prostate cancer hormone therapy removes the chemical that feeds cells and can stop or slow the growth and spread of the tumor.
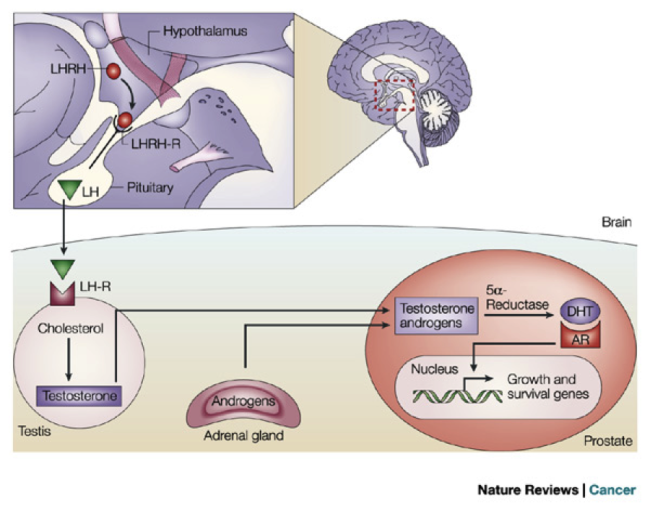
Where does Testosterone Come From? A chemical sequence in the brain signals the testicles, which make 90% of the bodys hormones, to begin production. A structure in the brain called the hypothalamus continually monitors the blood stream for adequate levels of testosterone. If these levels drop, the hypothalamus releases a chemical called GnRH or LHRH . GnRH acts as a messenger and travels to the pituitary gland where it plugs into designated receptors.
How is Hormone Therapy Administered? There are four basic methods androgen deprivation: castration, estrogen, anti androgens, and combine androgen blockade.
Don’t Miss: Prostate Specific Antigen Psa Screen
The Saturation Model And Its Proposed Mechanisms
A new paradigm gaining momentum to replace the traditional testosterone dependent theory has been termed the saturation model . According to this model, testosterone and its intracellular metabolite 5-DHT are critical for the growth of prostate tissue, but are in excess at physiologic concentrations. The theory maintains that serum testosterone concentration has limited ability to stimulate prostate growth. A hypothesized saturation point occurs at near-castrate levels where the low androgen concentration would be rate-limiting in prostate tissue proliferation . The saturation model is supported by evidence derived from both animal and human studies. In rats, the half-maximal prostate growth occurs at approximately 36 ng/dL, which correlates to near-castrate levels of testosterone . In human prostate tissue, the AR has been reported to become saturated at approximately 120 ng/dL in vitro, and 240 ng/dL in vivo . A 6-month study of TRT in men with LOH revealed that despite administration of exogenous testosterone, which substantially increased serum testosterone, there was no increase in testosterone or DHT within the prostate itself . This has led some to believe that a mechanism of the saturation model could be a lack of prostatic uptake of exogenous testosterone protecting the prostate from large serum androgens changes.
Hormone Therapy For Prostate Cancer
Jump to a section
Hormone therapy is also called androgen suppression therapy. The goal is to reduce levels of male hormones, called androgens, in the body, or to stop them from fueling prostate cancer cells.
Androgens stimulate prostate cancer cells to grow. The main androgens in the body are testosterone and dihydrotestosterone . Most androgen is made by the testicles, but the adrenal glands as well as the prostate cancer itself, can also make a fair amount. Lowering androgen levels or stopping them from getting into prostate cancer cells often makes prostate cancers shrink or grow more slowly for a time. But hormone therapy alone does not cure prostate cancer.
Recommended Reading: Soy Milk And Prostate Cancer
What Are The Risks Of Testosterone Therapy
A relatively small number of men experience immediate side effects of testosterone treatment, such as acne, disturbed breathing while sleeping, breast swelling or tenderness, or swelling in the ankles. Doctors also watch out for high red blood cell counts, which could increase the risk of clotting.
Men on long-term using forms of testosterone therapy long term appear to have a higher risk of cardiovascular problems, like heart attacks, strokes, and deaths from heart disease. For example, in 2010, researchers halted the Testosterone in Older Men study when early results showed that men on testosterone replacement therapy had noticeably more heart problems. “In older men, theoretical cardiac side effects become a little more immediate,” Dr. Pallais says.
Some physicians also have a lingering concern that testosterone therapy could stimulate the growth of prostate cancer cells. As with the hypothetical cardiac risks, the evidence is mixed. But because prostate cancer is so common, doctors tend to be leery of prescribing testosterone to men who may be at risk.
So, keep risks in mind when considering testosterone therapy or other therapies . “I frequently discourage it, particularly if the man has borderline levels,” Dr. Pallais says.
The Truth About Testosterone Replacement Therapy And Prostate Cancer
Many men with low testosterone find themselves apprehensive about undergoing testosterone replacement therapy . The commonly held theory is that high levels of testosterone stimulate the growth of prostate cancer.
New findings show that TRT has very little impact on the growth of prostate cancer or the elevation of PSA levels and may change the way you think about the efficacy of testosterone in cancer treatment.
Also Check: What Surgery Is Done For Enlarged Prostate
Surgery To Remove The Testicles
Surgery to remove your testicles isnt a common way of lowering the amount of testosterone you produce.
You usually only have surgery to remove your testicles if you need your testosterone reduced urgently. For example if your cancer has spread to your bones and is pressing on your spinal cord, your doctors might want to reduce the amount of testosterone quickly.
Your doctors might also suggest surgery as an option if you dont want to have injections or tablets.
What Are Male Sex Hormones
Hormones are substances that are made by glands in the body. Hormones circulate in the bloodstream and control the actions of certain cells or organs.
Androgens are a class of hormones that control the development and maintenance of male characteristics. The most abundant androgens in men are testosterone and dihydrotestosterone .
Androgens are required for normal growth and function of the prostate, a gland in the male reproductive system that helps make semen. Androgens are also necessary for prostate cancers to grow. Androgens promote the growth of both normal and cancerous prostate cells by binding to and activating the androgen receptor, a protein that is expressed in prostate cells . Once activated, the androgen receptor stimulates the expression of specific genes that cause prostate cells to grow .
Almost all testosterone is produced in the testicles a small amount is produced by the adrenal glands. Although prostate cells do not normally make testosterone, some prostate cancer cells acquire the ability to do so .
Read Also: Best Prostate Supplement Beta Sitosterol
Treating Prostate Cancer With Hormone Therapy
Hormone therapy, also known as androgen deprivation therapy , has long been the backbone of treatment for metastatic prostate cancer.
The male sex hormone testosterone is known to stimulate the growth of prostate cancer cells.
Hormone therapy, depending on the form, reduces this effect by either decreasing the bodys production of testosterone or blocking testosterone from binding to cancer cells.
There are several scenarios in which hormone therapy is typically used:
- When prostate cancer has spread too far to be cured by surgery or radiation, or has recurred after surgical or radiation treatment
- As an initial treatment for patients who are at higher risk of recurrence after treatment, such as those with a high PSA level or a high Gleason score
- For patients who have a high PSA level following surgery or radiation, even if they have no evidence of disease. Not all doctors, however, agree with this approach
Obesity & Physical Activity
I think it comes as no surprise that obesity is very well linked to advanced and aggressive prostate cancer 14,15. One possible reason for this is due to altered hormone and metabolic profiles. Elevated insulin, due to the insulin resistance associated with obesity can promote prostate cancer growth. Furthermore, in obesity we note an elevation in oestradiol levels, which can encourage prostate cancer growth 16. Exercise can naturally decrease the risk of prostate and other cancers 1.
Lets expand on the point regarding Oestradiol What role do your sex hormones play?
Don’t Miss: Where Does Prostate Cancer Commonly Metastasize To
How Are Treatments Administered
GnRH agonists are either injected or placed as small implants under the skin. Anti-androgens are taken as a pill once per day. Degarelix is given as an injection. A chemotherapy drug called docetaxel is sometimes used in combination with these hormone therapies.
Zytiga is taken by mouth once per day in combination with a steroid called prednisone.
Surgery to remove the testicles can be done as an outpatient procedure. You should be able to go home a few hours after an orchiectomy.
Confusion About Testosterone Therapy And Prostate Cancer
One of the most commonly cited side effects for hormone replacement therapy as a cure to low testosterone in men is an increased risk of prostate cancer. However, much like with the Million Woman Study that linked HRT and breast cancer, the evidence corroborating this belief is dated and likely false. In fact, according to some modern research, low testosterone is actually a risk factor FOR types of male cancer.
The origins of the theory that testosterone replacement increased the risk of prostate cancer go back to research done at the University of Chicago in the 1940s by a group led by urologist Charles Huggins. Based on experiments performed first on dogs and then on humans, Huggins group concluded that prostate cancer was androgen dependent when testosterone levels were high, the cancer worsened, but when the levels were lowered, the cancer shrank. Huggins theory led to surgical castration removal of the testicles becoming the standard treatment for prostate cancer because of the resultant drop in testosterone. Huggins was awarded a Nobel Prize in 1966 for these contributions to medical research.
So if youre a man who suspects he may have low testosterone, and are considering hormone replacement therapy, you can rest easy. HRT wont give you prostate cancer in fact, it might help prevent it.
Don’t Miss: What Doctor Treats Prostate Cancer
Does T Level Influence Survival Following Adt
Controversy previously existed regarding the clinical significance of circulating androgens following treatment with GnRH agonists. There is evidence that very low levels of T and its metabolites may elicit prostate cancer progression. Although the treatment is controversial, some experts believe that MAB achieves superior survival over GnRH agonists alone. It is unclear whether this modest observed survival advantage is attributable to prevention of the T flare or T escape, or suppression of adrenal androgens. There is new evidence that prostate cancers themselves are capable of synthesizing endogenous T. A recent clinical study showing that treatment with a CYP17 inhibitor such as abiraterone, either alone or with glucocorticoids, resulted in significant antitumor activity in patients with androgen independent progression both who had and had not received chemotherapy.
How May Changing Prostate Cancer Screening Guidelines Impact Use Of Adt
PSA is the most utilized biomarker for diagnosing prostate cancer. It is a serine protease inhibitor that was discovered and purified in 1979. Thirteen years later, two large studies reported the utility of using PSA screening for prostate cancer., In one study, approximately 15% of men of 1249 over the age of 50 years were found to have an elevated PSA, defined by a serum level > 4.0 ng/mL. Prostate cancer was diagnosed in slightly more than 30% of men with an elevated PSA. Soon thereafter, PSA screening gained widespread acceptance in the United States. According to Zeliadt and colleagues, it has been estimated that approximately 50% of the male US population between the ages of 55 and 74 years undergo PSA screening over a 6- to 7-month period.
The European Randomized Study of Screening for Prostate Cancer had less contamination than the PLCO study because a smaller proportion of men in the unscreened cohort underwent screening prior to randomization or during the study. The median follow-up was 9 years. Overall, prostate cancer mortality was reduced by 20%. Upon correcting for contamination, PSA screening decreased prostate cancer mortality by 31% in actually screened patients.
Don’t Miss: Does Prostate Cancer Make You Tired
Complications Of Hormonal Therapy
E. David Crawford, MD, Professor of Surgery and Radiation Oncology, Head of the Section of Urologic Oncology at the University of Colorado, and Chairman of the 16th International Prostate Cancer Update, provided an excellent overview of complications of hormonal therapy and their treatment. He began this discussion by outlining not only the benefits but also the complications of androgen deprivation, the latter including osteoporosis, hot flushes, gastrointestinal side effects, anemia, gynecomastia, sarcopenia, central nervous system effects, change in body weight, sexual dysfunction, loss of bone density, and increased risk of bone fracture and hot flushes .
Dont Miss: Does Enlarged Prostate Cause Constipation
How To Screen For Prostate Cancer
Weve talked a lot about causes of prostate cancer, but not on the methods used to screen for it, other than monitoring PSA.
A raised PSA level is about 3ng/mL or higher in men aged 50 +. But, having elevated PSA can also be due to an enlarged prostate, prostatitis , or a urinary infection.
Further follow up checks are warranted using digital rectal examination , particularly if youre over 45 where the risk of prostate cancer increases dramatically. This will involve having a finger inserted into your prostate by a doctor or nurse. Dont worry, lubricant and a glove are used its a short assessment. You MUST get a DRE if youre over 45 dont be afraid of it. Prostate cancer is much, much worse than a DRE.
If you are over 40 years old and on Testosterone Replacement Therapy, The BSSM guidelines recommend an annual DRE, alongside regular monitoring of your PSA.
To really confirm prostate cancer, an MRI is the gold standard. In addition to this, core needle biopsies may be performed, which involve taking small samples of the prostate. The cells are then looked at under a microscope. Please dont worry if you ever need this done, it only causes some brief discomfort and is generally painless as local anaesthetic is used and the biopsy instrument is designed to not cause any pain. This combined procedure will provide a highly accurate assessment of whether you have prostate cancer, or not.
Recommended Reading: How Old Can You Be To Get Prostate Cancer
Early Versus Delayed Treatment
For men who need hormone therapy, such as men whose PSA levels are rising after surgery or radiation or men with advanced prostate cancer who dont yet have symptoms, its not always clear when it is best to start hormone treatment. Some doctors think that hormone therapy works better if its started as soon as possible, even if a man feels well and is not having any symptoms. Some studies have shown that hormone treatment may slow the disease down and perhaps even help men live longer.
But not all doctors agree with this approach. Some are waiting for more evidence of benefit. They feel that because of the side effects of hormone therapy and the chance that the cancer could become resistant to therapy sooner, treatment shouldnt be started until a man has symptoms from the cancer. This issue is being studied.
Adverse Effects Of Adt
T suppression is associated with bone loss, which may also be influenced by other factors such as obesity, age, and sedentary lifestyle. Moreover, ADT and attendant bone demineralization is associated with an increased risk of skeletal fracture. Skeletal fractures are of particular concern, given their documented correlation with decreased overall survival in men with prostate cancer.
The morbidities of ADT should be considered in the context of the existing comorbidities of the patient when choosing palliative ADT. As per the AUA guidelines, ADT may be used for the palliation of symptomatic patients with more extensive or poorly differentiated tumors, whose life expectancy is too short to benefit from treatment with curative intent. When making treatment decisions about ADT, physicians and patients should discuss and review existing guidelines for lifestyle modifications, and the increased risk of adverse effects such as osteoporosis, fracture risks, obesity, alteration in lipids, diabetes and cardiovascular disease., Patients should be monitored with periodic follow-up evaluations including assessment of blood pressure, lipid profile, and glucose level. Patients with cardiac disease should receive appropriate secondary preventive measures as recommended by existing guidelines.,
Also Check: Is Prostate Cancer Genetically Inherited
Do Gnrh Agonists Have Unique Properties
Heyns and colleagues compared T suppression in 140 and 137 men receiving monthly leuprolide acetate versus triptorelin pamoate, respectively. The primary endpoint of the trial was the percentage of men whose serum T declined and remained at or below castration level during the 9-month treatment duration. The probability of maintenance of castration T levels is shown at monthly intervals throughout the 9-month study . A Kaplan-Meier survival analysis for the maintenance of castration levels measured 3.75 mg triptorelin pamoate or 7.5 mg leuprolide. The cumulative maintenance of castration levels were 96% and 91% for triptorelin pamoate and leuprolide, respectively . In this study, a greater proportion of men maintained medical castration with triptorelin pamoate at 29 days.
The maintenance of castration in men treated with triptorelin pamoate, 3.75 mg , or leuprolide acetate, 7.5 mg , for 9 months . Reproduced with permission from Heyns CF et al.
Mean serum testosterone levels were analyzed every 28 days in 277 men receiving androgen deprivation with either leuprolide acetate or triptorelin pamoate. These levels fell below the predefined levels for medical castration at 29 days and 57 days for 91% and 98% of subjects in the triptorelin pamoate group and 99% and 97% of the subjects in the leuprolide group. Although the mean difference was significant between the groups at 29 days, it was not significant at 57 days. Reproduced with permission from Heyns CF et al.