Guidelines For Radiotherapy Of Prostate Cancer
Department of Radiation Oncology, Beijing Hospital, National Center of Gerontology Institute of Geriatric Medicine, Chinese Academy of Medical Sciences, Beijing, P. R. China
Correspondence
Gaofeng Li, Department of Radiation Oncology, Beijing Hospital, National Center of Gerontology, Institute of Geriatric Medicine, Chinese Academy of Medical Sciences, Beijing, P. R. China.
Yexiong Li
State Key Laboratory of Molecular Oncology and Department of Radiation Oncology, National Cancer Center/Cancer Hospital, Chinese Academy of Medical Sciences and Peking Union Medical College , Beijing, P. R. China
Qiuzi Zhong
Department of Radiation Oncology, Beijing Hospital, National Center of Gerontology Institute of Geriatric Medicine, Chinese Academy of Medical Sciences, Beijing, P. R. China
Liru He
Department of Radiation Oncology, State Key Laboratory of Oncology in South China, Collaborative Innovation Center for Cancer Medicine, Sun Yat-sen University Cancer Center, Guangzhou, 510060 P. R. China
Chunmei Li
Department of Radiation Oncology, Beijing Hospital, National Center of Gerontology Institute of Geriatric Medicine, Chinese Academy of Medical Sciences, Beijing, P. R. China
Ming Liu
Department of Urology, Beijing Hospital, National Center of Gerontology, Institute of Geriatric Medicine, Chinese Academy of Medical Sciences, Beijing, P. R. China
Yueping Liu
Xuan Wang
Hui Zhu
Correspondence
Yexiong Li
Qiuzi Zhong
Liru He
Chunmei Li
Ming Liu
Yueping Liu
Xuan Wang
What Types Of Hormone Therapy Are Used For Prostate Cancer
Hormone therapy for prostate cancer can block the production or use of androgens . Currently available treatments can do so in several ways:
- reducing androgen production by the testicles
- blocking the action of androgens throughout the body
- block androgen production throughout the body
Androgen production in men. Drawing shows that testosterone production is regulated by luteinizing hormone and luteinizing hormone-releasing hormone . The hypothalamus releases LHRH, which stimulates the release of LH from the pituitary gland. LH acts on specific cells in the testes to produce the majority of testosterone in the body. Most of the remaining androgens are produced by the adrenal glands. Androgens are taken up by prostate cells, where they either bind to the androgen receptor directly or are converted to dihydrotestosterone , which has a greater binding affinity for the androgen receptor than testosterone.
Treatments that reduce androgen production by the testicles are the most commonly used hormone therapies for prostate cancer and the first type of hormone therapy that most men with prostate cancer receive. This form of hormone therapy includes:
Treatments that block the action of androgens in the body are typically used when ADT stops working. Such treatments include:
Treatments that block the production of androgens throughout the body include:
Study Process And Results
Researchers working at 10 hospitals in Spain enrolled 355 men with newly diagnosed prostate cancer that was still confined to the prostate and seminal vesicles . The men were divided into two groups: one group received a short course of hormonal therapy lasting four months, and the other group was treated for a longer duration of 24 months. All the patients were also treated with high-dose radiation.
After 10 years, only men who had been diagnosed initially with high-risk prostate cancer benefited from the long-term treatments. Specifically, 67.2% of these men avoided subsequent increases in prostate-specific antigen that signified worsening cancer. By contrast, 53.7% of men with high-risk cancer who received four months of hormonal therapy avoided similar PSA increases. Importantly, 78.5% of high-risk men who had long-term hormonal therapy were still alive after 10 years, compared to 67% of high-risk men treated with hormonal therapy for four months.
Among men with intermediate-risk prostate cancer, the duration of hormonal therapy made little difference. Just four men with intermediate-risk cancer developed worsening cancer that had spread to other sites in the body. Two came from the short-term treatment group, and two from the group that received hormonal therapy for 24 months. And after 10 years, none of the intermediate-risk patients had died from prostate cancer, regardless of how long the hormonal therapy treatments lasted.
Recommended Reading: Fiducial Markers For Prostate Cancer
What Happens To The Prostate After Radiation
The prostate gland will end up having a lot of scar tissue. It will shrink in size to about half its original weight within a couple years after finishing radiation. The urethra passes through the canter of the prostate gland like the hole of a doughnut. Sometimes this passage can widen, other times it can shrink after radiation. In summary, the prostate gland is heavily damaged from radiation and does not work normally afterwards.
High Dose Stereotactic Body Radiotherapy
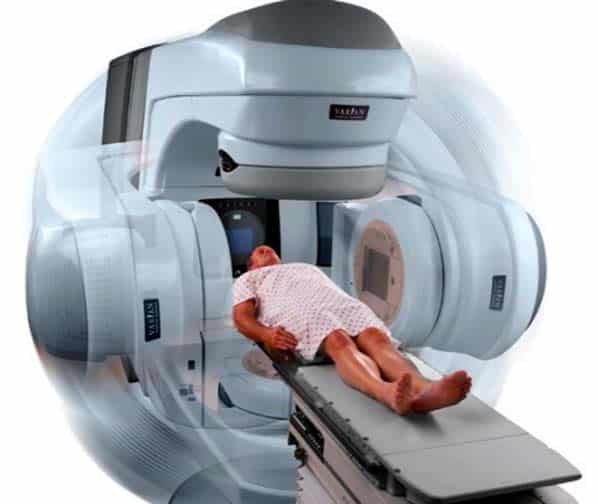
High dose stereotactic body radiotherapy treatment of men with newly diagnosed prostate cancer appears to result in shorter treatment times, less severe toxicity and excellent cancer control rates.1-6
Although prostate cancer generally responds well to radiation therapy, the possibility of radiation exposure to healthy tissue in the genitourinary and gastrointestinal systems can be of concern. SBRT is an advanced technique that precisely targets high doses of radiation to the cancer in a small number fractions, simultaneously avoiding surrounding tissue and reducing toxicity to non-cancerous cells.
Men with early stage prostate cancer can currently be treated with surgical prostatectomy, brachytherapy or external beam radiation therapy . SBRT, a form of EBRT condenses the radiation treatment for prostate cancer into as few as four to five sessions . The technique has become the standard of care for many non-surgical lung cancer patients, as it limits exposure to the heart and surrounding lungs. When treating tumors in the prostate, SBRT avoids the adjacent bladder, sex organs and rectum.
You May Like: Final Stages Of Prostate Cancer Life Expectancy
Read Also: How Do Doctors Check For Prostate Cancer
How Prostate Cancer Staging And Risk Group Affect Treatment Options
Your treatment choices are determined by several factors, including your cancers stage, aggressiveness and assigned risk stratification . Your age and current general health condition may also affect your choices.
Prostate cancer staging
Prostate cancer staging determines whether the cancer is confined to the prostate gland or whether theres evidence of metastasis, meaning its spread to other areas of the body.
Tools and methods to determine staging may include the prostate-specific antigen test, the digital rectal examination , the Gleason score and the American Joint Committee on Cancer TNM system, which provides information on the tumor, lymph node involvement and metastasis of a cancer. Imaging tests, such as a PET/CT scan, may also help determine your cancers stage.
The four stages of prostate cancer are subdivided into more precise categories, but we generally refer to three groups that indicate how far the cancer has spread:
- Localized: Theres no indication that the cancer has spread beyond the prostate.
- Regional: Theres evidence of cancer cells in nearby lymph nodes or tissue.
- Distant: Theres evidence the cancer has spread to other organs or body parts farther from the prostate.
Almost 90 percent of prostate cancers are diagnosed at the localized or regional stage. The five-year relative survival rate for men diagnosed with prostate cancer at these stages is nearly 100 percent.
Prostate cancer risk assessment
Treatment guidelines for prostate cancer
When Is Brachytherapy Alone The Right Choice
For some patients with disease that is confined to the prostate and not too aggressive , brachytherapy alone is a good option. It is also convenient for the patient as it is done in an outpatient setting and most people can get back to work within a few days.
But brachytherapy is not right for everyone. For some patients with less-aggressive disease, a watch-and-wait approach would be preferred. At MSK, our philosophy is that when the disease is caught very early, it is very appropriate to do active surveillance and hold off on treatment.
This philosophy applies to patients with a low PSA level, or nonaggressive disease as reflected by a Gleason score of 6 with evidence of cancer in only a few of the biopsy samples and no evidence from the MRI of a significant amount of disease. There are also very select patients with Gleason 7 disease who may be candidates for active surveillance.
You May Like: What Is An Enlarged Prostate Mean
Who Remained Prostate Cancer Free
Intermediate Risk patients experience a wider range of results and approaches due to the risk of disease beyond the prostate. When selecting a course of action, consultations are recommended with a urologist or surgeon, radiation oncologist and medical oncologist. Different treatments have different results and side effects. It is important to understand the potential impact each treatment can have on your quality of life after treatment.
Intermediate Risk patients are at a higher risk for cancer relapse or recurrence than Low Risk patients. That means patients in this risk group are more likely to have their cancer return following initial treatment, which may require additional treatment. To understand how effective the treatment or combination of treatments, are in keeping patients in remission, Doctors perform periodic monitoring or testing PSA levels, following treatment. It is very unlikely that the cancer will ever return, if you remain in remission for 10-15 years after prostate cancer treatment. Click on Get the Study, to obtain your copy of Foundations work. Share this Study with your Doctor as you select your treatment plan.
Intermediate Risk is any of the following:
PSA greater than 10 less than 20
Gleason Score is 7
How to Use the Graph
About the Data
Prostate Cancer Risk Groups
Prostate cancer can be categorised into one of 5 risk groups in the Cambridge Prognostic Group .
Doctors will look at the Grade Group , prostate specific antigen level and tumour stage to decide which CPG group the prostate cancer is.
The risk group of the cancer will help determine which types of treatments will be necessary.
If prostate cancer is diagnosed at an early stage, the chances of survival are generally good.
Recommended Reading: How Many Radiation Treatments Are Needed For Prostate Cancer
Possible Side Effects Of Ebrt
Some of the side effects from EBRT are the same as those from surgery, while others are different.
Bowel problems: Radiation can irritate the rectum and cause a condition called radiation proctitis. This can lead to diarrhea, sometimes with blood in the stool, and rectal leakage. Most of these problems go away over time, but in rare cases normal bowel function does not return. To help lessen bowel problems, you may be told to follow a special diet during radiation therapy to help limit bowel movement during treatment. Sometimes a balloon-like device or gel is put between the rectum and the prostate before treatment to act like a spacer to lessen the amount of radiation that reaches the rectum.
Urinary problems: Radiation can irritate the bladder and lead to a condition called radiation cystitis. You might need to urinate more often, have a burning sensation while you urinate, and/or find blood in your urine. Urinary problems usually improve over time, but in some men they never go away.
Some men develop urinary incontinence after treatment, which means they cant control their urine or have leakage or dribbling. As described in the surgery section, there are different levels and types of incontinence. Overall, this side effect occurs less often with radiation therapy than after surgery. The risk is low at first, but it goes up each year for several years after treatment.
Are Surgery And Radiation Therapy Ever Used Together
In some cases, your care team may use both surgery and radiation therapy as part of your prostate cancer treatment plan. Typically, radiation therapy is delivered after surgery to target remaining cancer cells or that came back. However, in some situations, doctors may recommend radiation therapy first to kill cancer cells in tissues near the prostate gland before performing the prostatectomy.
Also Check: Signs Of Prostate Cancer In Dogs
Does Msk Offer Proton Therapy For Prostate Cancer
Some men with prostate cancer may choose to receive another form of external-beam radiation therapy called proton therapy. Proton therapy can deliver a high radiation dose to the prostate while lowering the radiation dose to normal surrounding tissue. It is unclear if there is any advantage to proton therapy compared with IMRT. We are now studying how these approaches compare in terms of side effects and outcomes at the New York Proton Center. These efforts are being led by radiation oncologist Daniel Gorovets.
Radiation Therapy For Prostate Cancer
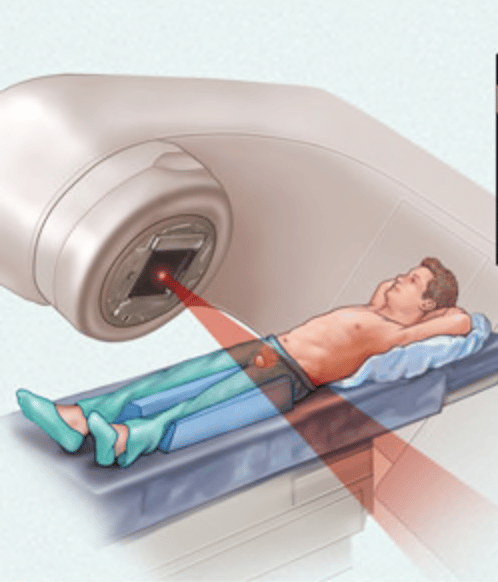
Radiation therapy uses high-energy rays or particles to kill cancer cells. Depending on the stage of the prostate cancer and other factors, radiation therapy might be used:
- As the first treatment for cancer that is still just in the prostate gland and is low grade. Cure rates for men with these types of cancers are about the same as those for men treated with radical prostatectomy.
- As part of the first treatment for cancers that have grown outside the prostate gland and into nearby tissues.
- If the cancer is not removed completely or comes back in the area of the prostate after surgery.
- If the cancer is advanced, to help keep the cancer under control for as long as possible and to help prevent or relieve symptoms.
Also Check: How Do They Check Your Prostate For Cancer
Role Of The Funding Source
This is an independent academic study supported by an unrestricted educational grant from Astellas. The authors performed the protocol design, data analysis, interpretation, and preparation of this report. Data analysis was performed by an independent statistician . All authors had access to the study data. All decisions relating to the manuscript writing and content were made jointly by the authors, including the final decision to submit it for publication.
Matching Treatment For Favorable Risk Prostate Cancer
Today, the majority of PCa cases are diagnosed early thanks to PSA screening coupled with noninvasive multiparametric MRI tumor detection. It therefore makes sense that for those with Gleason 3+3 and some with Gleason 3+4, the conditions are favorable for a successful minimalist approach to managing the disease, including treatment and AS. These are considered favorable low-risk and favorable intermediate-risk prostate cancers. When carefully diagnosed and qualified, these patients may safely hold off on such aggressive radical treatments provided they protect themselves by adhering to monitoring protocols.
Recommended Reading: Prostate Cancer And Radiation Seeds
Video: What Is Radiation Therapy
Watch this short video to learn more about radiation therapy.
A/Prof Ian Vela, Urologic Oncologist, Princess Alexandra Hospital, Queensland University of Technology, and Urocology, QLD A/Prof Arun Azad, Medical Oncologist, Urological Cancers, Peter MacCallum Cancer Centre, VIC A/Prof Nicholas Brook, Consultant Urological Surgeon, Royal Adelaide Hospital and A/Prof Surgery, The University of Adelaide, SA Peter Greaves, Consumer Graham Henry, Consumer Clin Prof Nat Lenzo, Nuclear Physician and Specialist in Internal Medicine, Group Clinical Director, GenesisCare Theranostics, and Notre Dame University Australia, WA Henry McGregor, Mens Health Physiotherapist, Adelaide Mens Health Physio, SA Jessica Medd, Senior Clinical Psychologist, Department of Urology, Concord Repatriation General Hospital, NSW Dr Tom Shakespeare, Director, Radiation Oncology, Coffs Harbour, Port Macquarie and Lismore Public Hospitals, NSW A/Prof David Smith, Senior Research Fellow, Daffodil Centre, Cancer Council NSW Allison Turner, Prostate Cancer Specialist Nurse , Canberra Region Cancer Centre, Canberra Hospital, ACT Maria Veale, 13 11 20 Consultant, Cancer Council QLD Michael Walkden, Consumer Prof Scott Williams, Radiation Oncology Lead, Urology Tumour Stream, Peter MacCallum Cancer Centre, and Professor of Oncology, Sir Peter MacCallum Department of Oncology, The University of Melbourne, VIC.
View the Cancer Council NSW editorial policy.
Physical Emotional And Social Effects Of Cancer
Cancer and its treatment cause physical symptoms and side effects, as well as emotional, social, and financial effects. Managing all of these effects is called palliative care or supportive care. It is an important part of your care that is included along with treatments intended to slow, stop, or eliminate the cancer.
Palliative care focuses on improving how you feel during treatment by managing symptoms and supporting patients and their families with other, non-medical needs. Any person, regardless of age or type and stage of cancer, may receive this type of care. And it often works best when it is started right after a cancer diagnosis. People who receive palliative care along with treatment for the cancer often have less severe symptoms, better quality of life, and report that they are more satisfied with treatment.
Palliative treatments vary widely and often include medication, nutritional changes, relaxation techniques, emotional and spiritual support, and other therapies. You may also receive palliative treatments similar to those meant to get rid of the cancer, such as chemotherapy, surgery, or radiation therapy.
Learn more about the importance of tracking side effects in another part of this guide. Learn more about palliative care in a separate section of this website.
You May Like: Small Cell Carcinoma Of The Prostate Survival
Remission And The Chance Of Recurrence
A remission is when cancer cannot be detected in the body and there are no symptoms. This may also be called having no evidence of disease or NED.
A remission can be temporary or permanent. This uncertainty causes many people to worry that the cancer will come back. Although there are treatments to help prevent a recurrence, such as hormonal therapy and radiation therapy, it is important to talk with your doctor about the possibility of the cancer returning. There are tools your doctor can use, called nomograms, to estimate someone’s risk of recurrence. Understanding your risk of recurrence and the treatment options may help you feel more prepared if the cancer does return. Learn more about coping with the fear of recurrence.
In general, following surgery or radiation therapy, the PSA level in the blood usually drops. If the PSA level starts to rise again, it may be a sign that the cancer has come back. If the cancer returns after the original treatment, it is called recurrent cancer.
When this occurs, a new cycle of testing will begin again to learn as much as possible about the recurrence, including where the recurrence is located. The cancer may come back in the prostate , in the tissues or lymph nodes near the prostate , or in another part of the body, such as the bones, lungs, or liver . Sometimes the doctor cannot find a tumor even though the PSA level has increased. This is known as a PSA recurrence or biochemical recurrence.