Locally Advanced Prostate Cancer
In the UK, locally advanced prostate cancers account for 40% of prostate cancers at presentation. These include carcinomas where one or two acini have penetrated through the prostatic capsule to those invading adjacent structures including the trigone of the bladder, the rectum, the urethra, and the pelvic side wall. Therapeutic options include external beam radiotherapy , androgen ablation alone, or active monitoring.
What Is Advanced Prostate Cancer
When prostate cancer spreads beyond the prostate or returns after treatment, it is often called advanced prostate cancer.
Prostate cancer is often grouped into four stages, with stages III and IV being more advanced prostate cancer.
- Early Stage | Stages I & II: The tumor has not spread beyond the prostate.
- Locally Advanced | Stage III: Cancer has spread outside the prostate but only to nearby tissues.
- Advanced | Stage IV: Cancer has spread outside the prostate to other parts such as the lymph nodes, bones, liver or lungs.
When an early stage prostate cancer is found, it may be treated or placed on surveillance . Advanced prostate cancer is not curable, but there are many ways to treat it. Treatment can help slow advanced prostate cancer progression.
There are several types of advanced prostate cancer, including:
Biochemical Recurrence
With biochemical recurrence, the prostate-specific antigen level has risen after treatment using surgery or radiation, with no other sign of cancer.
Castration-Resistant Prostate Cancer
Non-Metastatic Castration-Resistant Prostate Cancer
Prostate cancer that no longer responds to hormone treatment and is only found in the prostate. This is found by a rise in the PSA level, while the testosterone level stays low. Imaging tests do not show signs the cancer has spread.
Metastatic Prostate Cancer
- Lymph nodes outside the pelvis
- Bones
- Other organs, such as liver or lungs
Metastatic Hormone-Sensitive Prostate Cancer
External Beam Radiotherapy And Androgen Ablation
For men receiving EBRT for T34 disease long term adjuvant androgen ablation after radiation offers a significant improvement in both metastatic and biochemical relapse rates when compared with short course androgen ablation given immediately before and during radiotherapy. This has translated into improvements in disease-free survival and overall survival at three years in one study, although in other trials this survival advantage was confined to poorly differentiated tumours only.
Androgen ablation involves chemical or surgical orchidectomy. However, reduced libido and increased fatigue are often associated with both these treatments. Non-steroidal antiandrogen monotherapy with bicalutamide 150 mg for T34 disease, compared with luteinising hormone releasing hormone agonists has been evaluated in a number of studies. No significant difference has been seen between the two types of drug in terms of overall survival and time to progression, although significant improvements in sexual interest and physical capacity were reported with bicalutamide.
For asymptomatic patients over 70 years old with low grade disease, active monitoring may be a favoured option. Although a significant survival advantage in favour of immediate hormonal therapy was initially demonstrated in a Medical Research Council study, subsequent follow up has shown much less of a survival difference and thus the potential benefits and side effects of early treatment warrant a full patient discussion.
Don’t Miss: What Fruit Is Good For Prostate Cancer
Radiation Therapy In Metastatic Disease
In a study of men with newly diagnosed metastatic prostate cancer, treatment with prostate radiation and ADT led to substantially longer survival compared with treatment with ADT alone. In the study, which included 6,382 men, combination therapy yield superior median survival and 5-year overall survival .
In patients with metastatic prostate cancer, radiation is also applied for palliative purposes. It is used in patients with castration-resistant prostate cancer with painful bone metastases, in patients at risk for fracture, and in patients with impending spinal cord compression.
A meta-analysis of the use of radioisotopes to relieve pain from bone metastases found that over 1-6 months, pain may be reduced without an increase in analgesic use however, severe effects such as leukocytopenia and thrombocytopenia frequently surface.
Radium-223 dichloride , formerly alpharadin, is an alpha particleemitting radioactive therapeutic agent that was approved by the FDA in 2013 for use in men with CRPC, symptomatic bone metastases, and no known visceral metastatic disease. Approval was based on the multinational ALSYMPCA trial , which is the first randomized phase III trial to demonstrate improved survival of CRPC with a bone-seeking radioisotope.
Biochemical Recurrence Without Metastatic Disease After Exhaustion Of Local Treatment Options
Biochemical recurrence is defined as a rise in PSA to 0.2 ng/mL and a confirmatory value of 0.2 ng/mL or greater following radical prostatectomy, or a rise of 2ng/mL or more above the nadir PSA after radiation therapy. Not all men who have a rising PSA will develop metastases, and for that reason not all such men require treatment. The risk of metastases and death depend on the patients Gleason score, the length of time between the nadir PSA and the onset of the PSAs rise, and the PSA doubling time.
Patients who have PSA failure following radical prostatectomy and have no evidence of metastatic disease have the options of watchful waiting, radiation therapy, or hormone ablation as salvage therapy. Similarly, patients who have PSA failure following radiation therapy have the following options:
- Watchful waiting
- Cryotherapy
- Hormone ablation
The pretreatment Gleason score, clinical stage, PSA level, and percentage of positive core biopsy results have been found to be reliable predictors of failure following local therapy. Unfortunately, no means of identifying recurrences limited to the pelvis is reliable. Although a Gleason grade of 7 or less is associated with a better prognosis than a grade of 8 or more, the survival likelihood associated with a rise in the PSA level is greater if the rise occurs more than 2 years after local treatment than if it occurs less than 2 years afterward.
Also Check: Prostate Cancer With Normal Psa
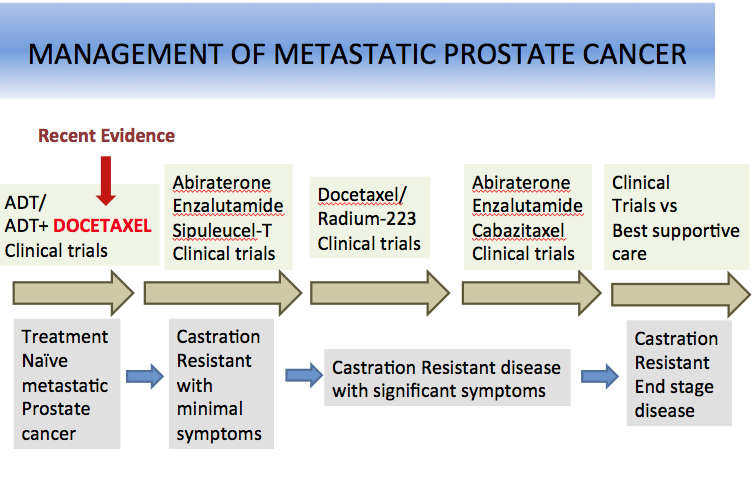
Management Of Advanced And Metastatic Disease
AUA/ASTRO/SUO guidelines on advanced prostate cancer separate management considerations into the following four disease states, which encompass the entire continuum of advanced prostate cancer :
These disease states are defined by the following:
- Primary tumor status
- Presence or absence of distant disease on imaging
- Testosterone levels
- Prior chemotherapy exposure
Multidisciplinary Nature Of Treatment In Todays Advanced Prostate Cancer Care Paradigm
As the therapeutic landscape evolves to include increasingly complex combinations of systemic therapies with or without local therapies, advances in imaging, and germline and somatic genetic testing, treating men with advanced prostate cancer is increasingly one that must embrace multidisciplinary management approaches. Team members should include urologists, medical oncologists, and radiation oncologists at a minimum when supporting treatment decisions for advanced disease. Additional specialists may also include genitourinary pathology, genetic counseling, palliative care, and holistic specialists, as appropriate, in addition to primary care. Best practices must also include clinicians comfortable describing the use of germline and somatic genetic testing, and when advanced imaging techniques could be optimally used or avoided. Radiologists and nuclear medicine specialists are valuable in helping to accurately interpret scans. Palliative care team members may also play a key role when treating men with symptomatic metastatic disease. Palliative care itself is an interdisciplinary, holistic approach to managing an advanced disease such as prostate cancer with a guarded prognosis. It can include controlling symptoms that are physical, psychological, spiritual, and social. The goal of palliation is to prevent and relieve suffering and to support the best possible QOL for the patient and family.
Don’t Miss: Where Can I Get A Free Prostate Exam
Psa Levels In Metastatic Prostate Cancer
As part of your ongoing treatment, your care team will regularly test your PSA levels. PSA stands for prostate-specific antigen, which can be high in men who have prostate cancer. PSA tests are used not only for the initial cancer diagnosis but also to observe the advancement of the disease over time.
Generally, PSA levels are higher in men with metastatic prostate cancer. However, in rare cases, its possible to have a low PSA even if you have metastatic disease. For these patients, disease progression is better measured in other ways, such as through imaging tests and biomarker tools.
What Treatments Are Available
If you have advanced prostate cancer, treatment wont cure your cancer. But it can help keep it under control and manage any symptoms.
If youve just been diagnosed with advanced prostate cancer, you may be offered the following treatments:
- chemotherapy with hormone therapy
- clinical trials.
Research has found that having radiotherapy together with one of the main treatments listed above can help some men with advanced prostate cancer to live longer. But radiotherapy isnt suitable for all men with advanced prostate cancer.
If you live in Scotland, you may also be offered a type of hormone therapy called abiraterone acetate together with standard hormone therapy. In the rest of the UK, abiraterone is currently only given to men with advanced prostate cancer that has stopped responding to other types of hormone therapy. The National Institute for Health and Care Excellence is currently deciding whether to make it available for men who have just been diagnosed with advanced prostate cancer.
Before you start treatment
Before you start any treatment, make sure you have all the information you need. Its important to think about how you would cope with the possible side effects. Speak to your doctor or nurse about this.
It can help to write down any questions you want to ask at your next appointment. It may also help to take someone with you, such as your partner, a family member or friend.
If you have any questions, speak to our Specialist Nurses.
Read Also: What Medicine Is Good For Enlarged Prostate
Addition Of Other Therapies In The Hormone
Docetaxel
As in many other malignancies, we have learned that combination therapy at the outset of treatment improves long-term disease control and survival outcomes. Both docetaxel and abiraterone acetate in the hormone-sensitive setting have demonstrated a survival benefit when added to standard ADT . Based on these data, most providers should offer, or at least consider, additional therapies to treat patients at this stage. Certainly in a frail patient population, one must continue to assess the overall fitness of a patient. Any patient already thought of as fit should be offered unaltered therapy. Those found to be vulnerable or frail could be considered based on the ability to reverse at-risk conditions.
Abiraterone acetate and prednisone
The patients enrolled in the LATITUDE and STAMPEDE-abiraterone trials were generally older , with ECOG scores of 02 compared with the CHAARTED and STAMPEDE-chemotherapy cohorts. Of note, patients being treated with abiraterone must take a low-dose corticosteroid to avoid mineralocorticoid excess, which results from alteration of adrenal function. In addition, patients may not have the means to pay for this costly agent, since older patients usually have a fixed income. Overall, there is little need for dose interruptions or reductions of abiraterone, and it should be considered for a broad group of older patients with newly diagnosed metastatic hormone-sensitive prostate cancer.
Biochemical Recurrence After Locoregional Treatment
Biochemical recurrence can occur as PSA recurrence after definitive local treatment or as PSA persistence after definitive treatment. Per the National Comprehensive Cancer Network definition, persistence is the failure of PSA to become undetectable after surgery, whereas the European Association of Urology definition is PSA > 1.0 ng/mL within 4 to 8 weeks after surgery and has consistently been associated with poor oncological outcomes . Risk factors for PSA persistence include higher pre-operative PSA levels, advanced pathological T stage and International Society of Urological Pathology grade, positive surgical margins, and pathologic node-positive status . Therefore, it is essential to use effective imaging for staging workup in order to help identify these patients. Currently, there is a prospective study that aims to assess whether PSMA PET/CT should replace conventional imaging for the initial staging of patients with high-risk features .
After confirming BCR, imaging is used to assess for the presence of local or distant disease. However, conventional imaging modalities are limited by low sensitivity. For instance, both scintigraphy and 18-F sodium fluoride PET imaging visualize osteoblastic activity and thus do not indicate the full extent of disease activity or volume. Given these limitations, other tracers have been developed to more accurately characterize BCR.
You May Like: Malignant Prostate Cancer Survival Rate
Lutetium Lu 177 Vipivotide Tetraxetan
Lutetium Lu 177 vipivotide tetraxetan is indicated for the treatment of men with prostate-specific membrane antigen -positive, metastatic castration-resistant prostate cancer who have been treated with androgen receptor pathway inhibition and taxane-based chemotherapy. It is a radioligand therapeutic agent. The active moiety is the radionuclide lutetium-177, which is linked to a moiety that binds to PSMA, a transmembrane protein expressed in prostate cancer, including mCRPC. Upon binding to PSMA-expressing cells, the lutetium-177 delivers beta-minus radiation to the cells, as well as to surrounding cells, inducing DNA damage that can lead to cell death.
Approval was based on the phase 3 VISION trial. Compared with patients receiving standard care , patients who received lutetium Lu 177 vipivotide tetraxetan plus standard care had significantly prolonged imaging-based progression-free survival and overall survival .
Justification For A New Guideline
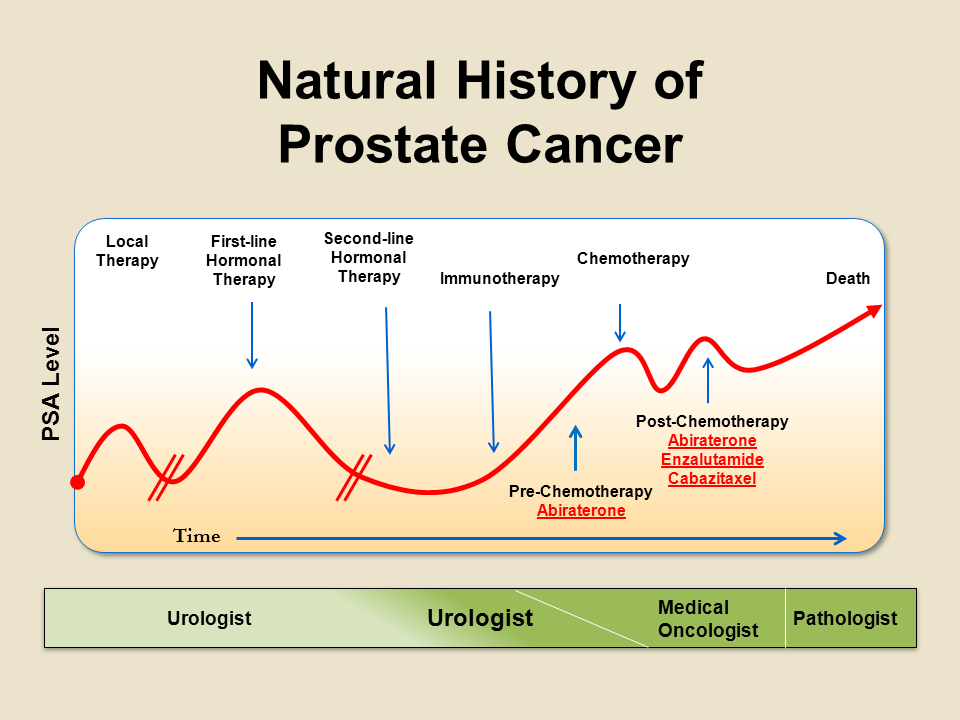
Clinicians treating men with advanced prostate cancer are challenged with the rapidly evolving prostate cancer landscape given the approval of new classes of agents for use in various prostate cancer disease states. The increasing complexity of advanced prostate cancer management underscores the need for the current clinical practice guideline, developed to provide a rational basis for treatment of patients with advanced disease, based on currently available published data. To assist in clinical decision-making, guideline recommendations are furnished according to disease state across the entire continuum of advanced prostate cancer.
You May Like: How Is Prostate Removal Performed
Are There Any Lifestyle Changes I Should Consider While In Treatment For Metastatic Prostate Cancer
The most important thing you can do is to stay physically active and strong. This includes following a heart-healthy diet and exercising.
Cardiovascular exercise is the most important. The degree, or intensity and duration, of cardio exercise depends on the individual person.
Several studies have pointed to a link between obesity and aggressive prostate cancer, although the mechanism is still being worked out.
Weight loss is generally encouraged if youre overweight, but excessive or unintentional weight loss can be a sign of disease progression and should be discussed with your doctor.
Finally, if youre a smoker, stop! If youre finding it hard to quit, ask your doctor about products and medications that might help you.
What Is My Outlook
If youre diagnosed with advanced prostate cancer, you may want to know how well your treatment is likely to control your cancer and for how long it will control it. This is sometimes called your outlook or prognosis. But not all men will want to know this.
While it isnt possible to cure advanced prostate cancer, treatments can help keep it under control, often for several years. Treatments will also help manage any symptoms, such as pain.
No one can tell you exactly what your outlook will be, as it will depend on many things such as where the cancer has spread to, how quickly it has spread, and how well you respond to treatment. Some men may not respond well to one treatment, but may respond better to another. And when your first treatment stops working, there are other treatments available to help keep the cancer under control for longer. Speak to your doctor about your own situation and any questions or concerns you have.
Also Check: What Foods Can Prevent Prostate Cancer
How Will My Cancer Be Monitored
Your doctor will talk to you about how often you should have check-ups. At some hospitals, you may not have many appointments at the hospital itself. Instead, you may talk to your doctor or nurse over the telephone. You might hear this called self-management.
You will have regular PSA tests. This is often a useful way to check how well your treatment is working. Youll also have regular blood tests to see whether your cancer is affecting other parts of your body, such as your liver, kidneys or bones.
You might have more scans to see how your cancer is responding to treatment and whether your cancer is spreading.
Your doctor or nurse will also ask you how youre feeling and if you have any symptoms, such as pain or tiredness. This will help them understand how youre responding to treatment and how to manage any symptoms. Let them know if you have any side effects from your treatment. There are usually ways to manage these.
Determination Of Evidence Strength
Based on assessments of the domains described above, the methodology team graded the strength of evidence for each intervention as high, moderate, low, or very low. Randomized controlled trials of interventions start as âhighâ strength of evidence and are graded down based on the presence and severity of shortcomings in each domain. A âhighâ grade indicates high confidence that the evidence reflects the true effect and that further research is very unlikely to change confidence in the estimate of effect. A âmoderateâ grade indicates moderate confidence that the evidence reflects the true effect and further research may change the estimate. A âlowâ grade indicates low confidence that the evidence reflects the true effect and further research is likely to change the confidence in the estimate of effect and could increase the confidence in the estimate. A âvery lowâ grade indicates evidence either is unavailable or is too limited to permit any conclusion due to extreme study limitations, inconsistency, imprecision, or reporting bias.
The AUA employs a three-tiered strength of evidence system to underpin evidence-based guideline statements. In short, high certainty by GRADE translates to AUA A-category strength of evidence, moderate to B, and both low and very low to C.
| Table 1: Strength of Evidence Definitions | |
|---|---|
| AUA Strength of Evidence Category | GRADE Certainty Rating |
Don’t Miss: How Does A Doctor Test For Prostate Cancer