Understanding Your Pathology Report: Prostate Cancer
When your prostate was biopsied, the samples taken were studied under the microscope by a specialized doctor with many years of training called a pathologist. The pathologist sends your doctor a report that gives a diagnosis for each sample taken. Information in this report will be used to help manage your care. The questions and answers that follow are meant to help you understand medical language you might find in the pathology report from your prostate biopsy.
Staging Of Prostate Cancer
The stage of a cancer describes its size and how far it has spread. The results of your tests help your doctors decide on the stage and plan your treatment.
We understand that waiting to know the stage and grade of your cancer can be a worrying time. Weâre here if you need someone to talk to. You can:
Macmillan is also here to support you. If you would like to talk, you can:
Nomograms Predict Survival Advantages Of Gleason Score 3+4 Over 4+3 For Prostate Cancer: A Seer
- 1Department of Urology, The First Affiliated Hospital of Chongqing Medical University, Chongqing, China
- 2Department of Respiratory and Critical Care Medicine, The First Affiliated Hospital of Chongqing Medical University, Chongqing, China
Background: Different proportions of Gleason pattern 3 and Gleason pattern 4 lead to various prognosis of prostate cancer with Gleason score 7. The objective of this study was to compare the survival outcomes of Gleason score 3+4 and 4+3 based on data from the Surveillance, Epidemiology, and End Results cancer registry database, and to investigate independent prognosis-associated factors and develop nomograms for predicting survival in Gleason score 7 prostate cancer patients.
Methods: A retrospective study was conducted on 69,116 cases diagnosed as prostate adenocarcinoma with Gleason score 7 between 2004 and 2009. Prognosis-associated factors were evaluated using univariate and multivariate Cox regression analysis, and a 1:1 ratio paired cohort by propensity score matching with the statistical software IBM SPSS, to evaluate prognostic differences between Gleason score 3+4 and 4+3. The primary cohort was randomly divided into training set and validation set . Based on the independent factors of prognosis, nomograms for prognosis were established by the training group and validated by the validation group using R version 3.5.0.
You May Like: Natural Treatment For Enlarged Prostate
Prostate Cancer Stages And Other Ways To Assess Risk
After a man is diagnosed with prostate cancer, doctors will try to figure out if it has spread, and if so, how far. This process is called staging. The stage of a prostate cancer describes how much cancer is in the body. It helps determine how serious the cancer is and how best to treat it. Doctors also use a cancerâs stage when talking about survival statistics.
The stage is based on tests described in Tests to Diagnose and Stage Prostate Cancer, including the blood PSA level and prostate biopsy results.
Also Check: Prostate Cancer Stage 7 Treatment
Can A Positive Prostate Biopsy Be Wrong
And it becomes even more difficult when those tools contradict each other. Finding high levels of PSA, a protein made in the prostate gland, in a man’s bloodstream can indicate prostate cancer. However, PSA testing has a 15 percent false-positive rate, which means the test may detect cancer that isn’t present.
You May Like: What Is The Best Over The Counter Prostate Supplement
What Is A Normal Gleason Score For Prostate Cancer
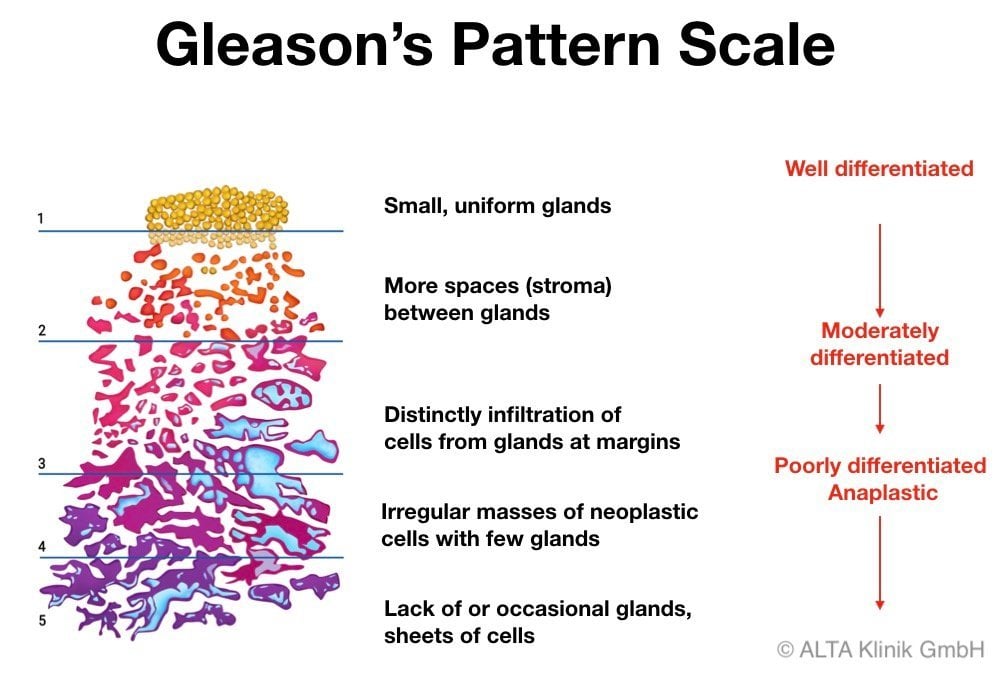
Your Gleason score doesn’t rank potential ranges like ranges set for elevated PSA tests. Instead, providers break Gleason scores into three categories:
- Gleason 6 or lower: The cells look similar to healthy cells, which is called well differentiated.
- Gleason 7: The cells look somewhat similar to healthy cells, which is called moderately differentiated.
- Gleason 8, 9 or 10: The cells look very different from healthy cells, which is called poorly differentiated or undifferentiated.
What are grade groups?
Healthcare providers established grade groups to clarify the Gleason score system. Those grade groups are:
- Grade Group 1 = Gleason 6 .
- Grade Group 2 = Gleason 3+4=7.
- Grade Group 3 = Gleason 4+3=7.
- Grade Group 4 = Gleason 8.
- Grade Group 5 = Gleason 9-10.
How Do Doctors Find Out Your Grade Group
The pathologist grades each sample of prostate cancer cells from 3 to 5 based on how quickly they are likely to grow or how aggressive the cells look. You may hear this score being called the Gleason grade.
Doctors then work out an overall Gleason score by adding together the 2 most common Gleason grades. So for example, if the most common Gleason grade is 3, and the second most common is 4, then the overall Gleason score is 7. Or they might write the scores separately as 3 + 4 = 7. This combined score is now called the Grade Group.
There are 5 Grade Groups. Grade Group 1 is the least aggressive and Grade Group 5 is the most aggressive.
This is how the Gleason score and Grade Groups match up and what it means:
| Gleason score |
|---|
Don’t Miss: What Kind Of Pain Does Prostate Cancer Cause
What Is A Gleason Score
If you have prostate cancer, your Gleason score is one factor healthcare providers consider to develop your treatment plan.
Your score reflects what providers learned about your cancer after examining tissue samples from your prostate cancer biopsy. They looked for patterns of normal and abnormal cells, noting where your cells look more like cancerous cells and where they look more like healthy cells.
Then they graded each piece of the pattern on a 3 to 5 scale. Pattern pieces with cancer cells that look like healthy cells were graded low. Pieces with cancer cells that don’t look like healthy cells get high grades.
Providers add those scores to set an overall Gleason score between 6 and 10. They might refine their analysis by classifying your cells by group, with Gleason scores listed in grade groups 1 to 5.
How Do I Know The Gleason Grade Is Accurate
Assigning the correct Gleason score is a skill just like any other that is developed through experience and practice. It is often prudent to have the biopsy material referred for a second opinion at a reference center to confirm the accuracy of the initial Gleason score that was assigned.
References:
Also Check: Remedios Caseros Para El Cancer De Prostata
Impact Of Percent Gleason Pattern 4 On Active Surveillance
Active surveillance is now common practice for patients with clinically localized, low-volume Gleason score 3+3=6 prostate cancer . In addition, depending on age, comorbidity, PSA level, tumor extent, and patient desire, some Gleason score 3+4=7 tumors, with only focal, low-volume areas of pattern 4 disease, may be appropriate for active surveillance . Therefore, recording the percentage of pattern 4 in the pathology report is clinically relevant in such cases.
Stage Iv Prostate Cancer Prognosis
Prostate cancers detected at the distant stage have an average five-year survival rate of 28 percent, which is much lower than local and regional cancers of the prostate. This average survival rate represents stage IV prostate cancers that have metastasized beyond nearby areas to lymph nodes, organs or bones in other parts of the body.
How We Treat Prostate Cancer
The prognosis for metastatic prostate cancer can be discouraging, but some treatment centerslike the Johns Hopkins Precision Medicine Center of Excellence for Prostate Cancerspecialize in innovative, individualized therapy with the potential to improve outcomes.
Also Check: How Many Men Die Of Prostate Cancer
Don’t Miss: Stage 4 Prostate Cancer In Bones
How Is The Gleason Score Derived
The pathologist looking at the biopsy sample will assign one Gleason grade to the most predominant pattern in your biopsy and a second Gleason grade to the second most predominant pattern. For example: 3 + 4. The two grades will then be added together to determine your Gleason score. Theoretically, Gleason scores range from 2-10. However, since Dr. Gleasons original classification, pathologists almost never assign scores 2-5, and Gleason scores assigned will range from 6 to 10, with 6 being the lowest grade cancer.
You May Like: Is Cialis Good For Enlarged Prostate
The Natural History And Molecular Biology Of Low Grade Prostate Cancer
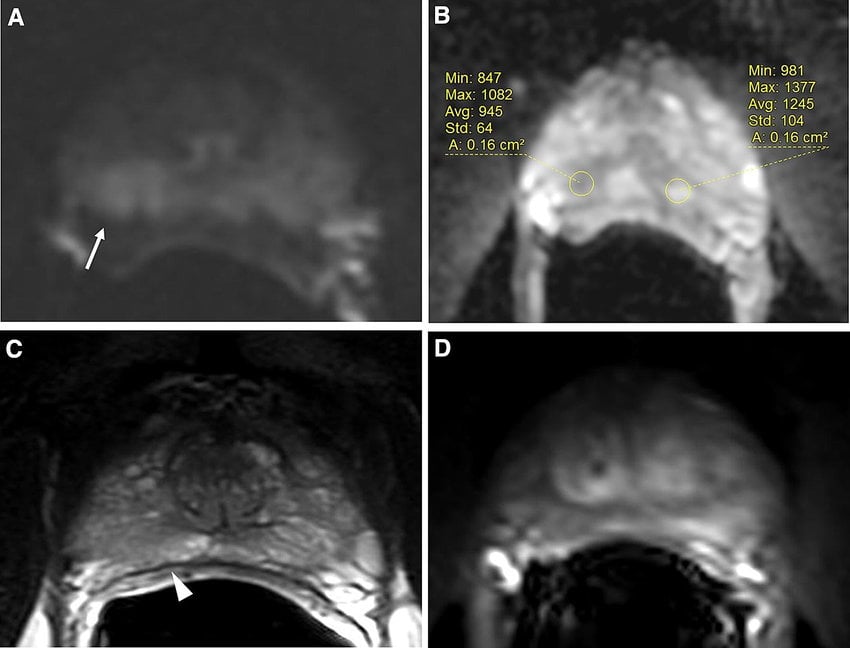
Prostate cancer develops with age in the majority of men, including those from all races and regions. In Caucasians, the chance of harboring prostate cancer is approximately the same as ones age thirty percent of men in their 30s, 40% in their 40s, 80% in their 80s . Most of these are microfoci and low grade, particularly in younger men. The high prevalence of microfocal prostate cancer has been confirmed in autopsy studies of Caucasians, Asians, and other ethnic groups going back more than 50 years. A recent autopsy study in Japanese and Russian men who died of other causes showed that overall 35% of both groups had prostate cancer, and 50% of the cancers in Japanese men aged > 70 were Gleason score 7 or above .
Recommended Reading: Can I Shrink My Prostate
Does Percent Gleason Pattern 4 Stratify The Prognosis Of Patients Undergoing Radical Prostatectomy
Table 1 summarizes the findings in previous studies assessing the impact of percent Gleason pattern 4 in prostate needle biopsy, radical prostatectomy, or both on stratifying patient outcomes.
Table 1
Prior to the recommendation from the ISUP 2014 consensus conference, the relative proportion of high-grade carcinoma in radical prostatectomy specimens was reported to strongly associate with established prognostic factors, such as higher preoperative prostate-specific antigen levels, positive surgical margins, extraprostatic extension, and lymph node metastasis. In a study by Cheng et al. involving 504 men who underwent radical prostatectomy for clinically localized prostate cancer, the rates of 10-year cancer-specific survival were 100%, 85%, and 67% in those with 0% Gleason pattern 4/5, 1â20% Gleason pattern 4/5, and > 20% Gleason pattern 4/5, respectively . Thus, in these 504 patients, the combined percent Gleason patterns 4 and 5 were found to be an independent predictor of cancer-specific survival.
Sauter et al. subsequently assessed a system for integration of both Gleason patterns 4 and 5 into a continuous numerical scale or score . Based on their data from 13,261 prostatectomy specimens and 3,295 matched biopsies, the IQ-Gleason score appeared to represent an efficient approach for combining quantitative Gleason grading and tertiary patterns into a single prognostic variable.
Limitations Of The Gleason Grading System
Although current revisions have improved the Gleason grading system, it continues to have limitations. Recent modifications have made the Gleason grading system much more complex than its original version. This complexity can be confusing for patients and clinicians. Gleason score 6 is now recommended as the lowest grade to be assigned on prostate biopsy. This is counterintuitive in that the Gleason scale ranges from 2 to 10. Patients may assume that a diagnosis of Gleason score 6 on biopsy means their tumor is in the mid-range of aggressiveness rather than having the best prognosis. In addition, many former Gleason score 6 tumors are now reclassified as Gleason score 7 in the modified system. Modern Gleason score 6 tumors have a much better prognosis than reported in the older literature. Studies have shown that virtually no pure Gleason score 6 tumors are associated with disease recurrence after radical prostatectomy and pure Gleason 6 cancer at radical prostatectomy lacks the potential for lymph node metastases . Another problem in the modern Gleason grading system is the lumping of Gleason score 7, as noted above in the NCCN Risk Classification System. Whereas many clinicians consider Gleason score 7 on biopsy to be intermediate risk, multiple studies have shown that Gleason score 4+3=7 demonstrates worse pathological stage and biochemical recurrence rates than 3+4=7 .
Read Also: What Percent Of Prostate Cancer Is Metastatic
Technique Of Focal Therapy
A variety of techniques have been described, all involving the use of directed energy and image guidance. These include high intensity focused ultrasound , MR guided ultrasound, laser ablation, cryosurgical ablation, focal photodynamic therapy, electroporation, various forms of radiation. Ultimately, which of these therapies becomes widely used will be a reflection of precision of treatment, morbidity, cost, and availability and convenience. The principles and methods used with these directed energies have been described previously. The experience with these technologies used for focal therapy is summarized in the table below, in chronological order.
Most of the focal therapy data lacks robust endpoints. In most published studies, follow-up biopsies were usually not systematic, and in most studies the majority of patients were not biopsied. This is a potential source of bias, in that PSA and MRI may misidentify as responders some patients with residual disease. In patients having a biopsy, the rate of positive biopsies ranged from 14% to 50% . Further, most authors only biopsied the treated area. Biopsies of the untreated area were selective based on mpMRI.
What Does It Mean If In Addition To Cancer My Biopsy Report Also Says Acute Inflammation Or Chronic Inflammation
Inflammation of the prostate is called prostatitis. Most cases of prostatitis reported on a biopsy are not caused by infection and do not need to be treated. In some cases, inflammation may increase you PSA level, but it is not linked to prostate cancer. The finding of prostatitis on a biopsy of someone with cancer does not affect their prognosis or the way the cancer is treated.
Recommended Reading: How Do They Test For Prostate Cancer
What Is A Bad Gleason Score For Prostate Cancer
Gleason scores aren’t good or bad, per se. They predict how quickly your prostate cancer might grow. Tumors with higher Gleason scores are likely to grow quickly. And Gleason scores aren’t the only factors healthcare providers consider when creating your treatment plan.
What other factors do healthcare providers consider?
Providers consider the results of other tests and additional biopsy information. For example, when you had your biopsy, your healthcare provider obtained several samples or cores from your prostate. They checked how many cores contained cancer and whether most of the cells in the cores were cancerous cells.
Other factors may include:
The Number Staging System
There are a few different systems used for staging prostate cancer. A simplified number staging system is described below.
- Stage 1 The tumour is contained in the prostate. The tumour is too small to be felt when a doctor does a rectal examination or to be seen on a scan.
- Stage 2 The tumour is still contained in the prostate, but your doctor can feel it when they do a rectal examination.
- Stage 3 The tumour has started to break through the outer capsule of the prostate and may be in the nearby tubes that produce semen .
- Stage 4 The tumour has spread outside the prostate. It may have spread to areas such as the bladder or back passage . Or it may have spread further, for example to the bones.
Using the numbered staging system described above:
- stage 4 is known as advanced prostate cancer.
See also
The grade of a cancer gives an idea of how quickly the cancer might grow or spread. A doctor decides the grade of the cancer by how the cancer cells look under the microscope.
Doctors look at the grade of the cancer to help them plan your treatment.
Gleason is the most commonly used grading system for prostate cancer.
Read Also: Remedios Caseros Para Desinflamar La Prostata
Do Gleason Scores Change
Asked by: Lavon Hamill
The decrease in proportion of high Gleason score cancers, however, was due to higher rates of low-grade disease diagnosis as a result of PSA screening. The researchers show that the shift in Gleason score proportions over time is not likely due to changes in the age at diagnosis.
Active Surveillance And Focal Therapy For Low

Laurence Klotz
Division of Urology, Sunnybrook Health Sciences Centre, University of Toronto, Canada
Correspondence to:
Keywords: Active surveillance focal therapy low risk prostate cancer minimally invasive conservative management biomarkers
Submitted Jun 01, 2015. Accepted for publication Jun 05, 2015.
doi: 10.3978/j.issn.2223-4683.2015.06.03
Recommended Reading: Stereotactic Body Radiotherapy For Prostate Cancer
What Is The Gleason Score
The Gleason grading system estimates the aggressiveness of the cancer by assigning a pattern to the cancer cells depending on their appearance under the microscope. A number from 1 to 5 is used as a measure of how aggressive the cancer looks under the microscope.
- If the cancerous tissue looks much like normal prostate tissue, a grade of 1 is assigned.
- If the cancer cells and their growth patterns look very abnormal, a grade of 5 is assigned.
- Grades 2 through 4 have features in between these extremes.
The most common type of prostate biopsy is a core needle biopsy. For this procedure, the doctor inserts a thin, hollow needle into the prostate gland. When the needle is pulled out it removes a small cylinder of prostate tissue called a core. This is typically repeated several times to sample different areas of the prostate.
Since multiple core biopsy samples are evaluated and prostate cancers in a single patient often have areas with different grades the pathologist assigns two grades to the examined prostate tissue. The first grade is the most common pattern seen after review of all the biopsy specimens and the 2nd grade is assigned to the next most common pattern.
Tertiary Grade On Needle Core Biopsy
In contrast to the original Gleason grading system, it is now recommended that on a needle core biopsy both the most common and highest grade are added together for the Gleason score . For example, if there is 60 % Gleason pattern 3, 35 % Gleason pattern 4, and 5 % Gleason pattern 5, the Gleason score would be 3+5=8. Needle core biopsy is an imperfect, non-targeted, random sampling of the prostate gland. Thus any amount of high-grade tumor sampled on needle biopsy most likely indicates a more significant amount of high-grade tumor within the prostate. In all specimens, in the setting of high-grade cancer, one should not report a lower grade if it occupies less than 5 % of the total tumor. For example, if there is 98 % Gleason pattern 4 and 2 % Gleason pattern 3, the Gleason score would be reported as 4+4=8 .
Read Also: Procedure To Check For Prostate Cancer