When Should I Call My Healthcare Provider
If youre 50 and you havent had your first prostate exam yet, call your healthcare provider to set up an appointment. If youre at higher risk, such as if you’re Black or prostate cancer runs in your family, you should have your first prostate exam by age 45.
Furthermore, if you develop symptoms of urinary tract obstruction, schedule a visit with your provider right away. This may indicate an enlarged prostate, benign prostatic hyperplasia or a urinary tract infection.
A note from Cleveland Clinic
Most people are understandably apprehensive about their first prostate exam. Learning all you can about the process can help abate any fears or uncertainties you have. Talk to your healthcare provider about your screening options. A prostate exam is the first step in the early detection of prostate cancer and early detection is key to successful treatment.
Last reviewed by a Cleveland Clinic medical professional on 04/04/2022.
References
Diagnostic Radiologic Procedure And Ultraviolet Light Exposure
The radiation generated from X-ray, CT and nuclear imaging is ionizing radiation that penetrates the tissue to reveal the bodyâs internal organs. However, ionizing radiation can damage DNA, and although cells repair most of the damage, sometimes small area may remain altered consequently leading to DNA mutations that may contribute to cancer development years down the road. The first study investigating the connection between low-dose ionization radiation from diagnostic X-ray procedures and risk for prostate cancer reported that exposure to a hip/pelvic X-ray significantly increased prostate cancer risk independently of other known risk factors such as family history of cancer . However, unless men were exposed to high doses of radiation during cancer treatment in youth, any increase in the risk for cancer due to medical radiation appears to be slight. Considering that the increase in high-dose imaging has occurred only since 1980 and the effects of radiation damage typically take many years to appear, this may explain the weak association between ionizing radiation and prostate cancer risk observed thus far.
Finally, exposure to solar UV radiation is inversely associated with both the incidence and mortality of prostate cancer . The biological explanation of this fact is based on the synthesis and physiological actions of vitamin D .
What Causes Early Onset Cancer
Itâs not yet clear why younger men get prostate cancer.
There seems to be a link between your genes and early onset prostate cancer. Researchers need to do more studies to see if things like obesity, physical activity, HPV infection, and exposure to things in the environment like cancer-causing agents play a role.
Don’t Miss: Seminal Vesicle Prostate Cancer Survival
What Questions Should I Ask My Healthcare Provider
If you have prostate cancer, you may want to ask your healthcare provider:
- Why did I get prostate cancer?
- What is my Gleason score? What is my Grade Group? What do these numbers mean for me?
- Has the cancer spread outside of the prostate gland?
- What is the best treatment for the stage of prostate cancer I have?
- If I choose active surveillance, what can I expect? What signs of cancer should I look out for?
- What are the treatment risks and side effects?
- Is my family at risk for developing prostate cancer? If so, should we get genetic tests?
- Am I at risk for other types of cancer?
- What type of follow-up care do I need after treatment?
- Should I look out for signs of complications?
A note from Cleveland Clinic
Prostate cancer is a common cancer that affects males. Most prostate cancers grow slowly and remain in the prostate gland. For a small number, the disease can be aggressive and spread quickly to other parts of the body. Men with slow-growing prostate cancers may choose active surveillance. With this approach, you can postpone, and sometimes completely forego, treatments. Your healthcare provider can discuss the best treatment option for you based on your Gleason score and Group Grade.
Family History And Genetics
Your family history is information about any health problems that have affected your family. Families have many common factors, such as their genes, environment and lifestyle. Together, these factors can help suggest if you are more likely to get some health conditions.
Inside every cell in our body is a set of instructions called genes. These are passed down from our parents. Genes control how the body grows, works and what it looks like. If something goes wrong with one or more genes , it can sometimes cause cancer.
Is prostate cancer hereditary?
If people in your family have prostate cancer or breast cancer, it might increase your own risk of getting prostate cancer. This is because you may have inherited the same faulty genes.
My father had prostate cancer. What are my risks?
- You are two and a half times more likely to get prostate cancer if your father or brother has had it, compared to a man who has no relatives with prostate cancer.
- Your chance of getting prostate cancer may be even greater if your father or brother was under 60 when he was diagnosed, or if you have more than one close relative with prostate cancer.
- Your risk of getting prostate cancer may also be higher if your mother or sister has had breast cancer.
Do you have a family history of prostate cancer?
If you’re over 45 and your father or brother has had prostate cancer, you may want to talk to your GP. Our Specialist Nurses can also help you understand your hereditary risk of prostate cancer.
Read Also: Non Invasive Prostate Cancer Test
Prostate Cancer In Australia What Do The Numbers Tell Us
HomeNews & MediaNewsProstate cancer in Australia what do the numbers tell us?
05 January 2022
The Australian Institute of Health and Welfare recently released the latest figures on prostate cancer incidence, mortality, and survival in Australia.
The trends over time are different to the trends we see for many other types of cancer, including a decreasing number of diagnoses since 2009, when cases peaked in Australia. In that year, 22,157 cases were diagnosed, compared to 18,110 cases expected to be diagnosed in 2021. With an ageing and increasing population, we might ordinarily expect to see the number of men diagnosed increase, but this has not been the case.
Why?
According to the AIHW:
Prostate-specific antigen testing and associated changes in guidelines can affect the number of new cases of prostate cancer. PSA testing was introduced in 1987 and is thought to have contributed to the peak in incidence in the 1990s. The PSA threshold at which males were referred for a prostate biopsy was lowered in 2002 and might have contributed to the peak incidence during the mid to late 2000s .
Numbers versus rates
Expressed in charts, this is what the trends look like for prostate cancer incidence and mortality in Australia for the period from 1982 to 2019:
Source:
The improved mortality rate is a key measure of success and is reflected in increasingly higher rates of survival over time:
Incidence
Mortality
Prostate Cancer In Asia
The incidence of prostate cancer in Asian countries has been historically much lower than their Western counterpart, ranging between 4.5 cases per 100,000 persons for South-Central Asia, 10.5 for Eastern Asia and 11.2 for Southeast Asia . Those values could be explained both by a low susceptibility of Asian men to prostate cancer and the lack of a systematic screening program. However, there is evidence that these figures are increasing in several countries . A review by Ha Chung et al., showed a general increase in prostate cancer incidence across China, India, South Korea, Vietnam, Japan, and Singapore . These figures were supported by data from GLOBOCAN 2008 and 2012 . Sim and Cheng noted that in some centres in Japan, the incidence rate rose from 6.3 to 12.7 between 1978 and 1997, while the incidence rates in Singaporean Chinese men increased to 118% within the same period . The lowest incidence reported in Asia was in Shanghai whereas the highest was in the Rizal Province in the Philippines. shows the differences in incidence and mortality across Asia. Studies have also shown that Asian Men living in the United States develop higher risk of prostate cancer than their counterparts living in Asia suggesting that change in lifestyle, and probabaly increased screening, could be the major contributors .
Read Also: What Do You Call A Prostate Doctor
Risk Factors Of Prostate Cancer
- Age
Age is the most significant risk factor for prostate cancer. Your risk increases as you get older. Most men diagnosed with prostate cancer are over 50 years of age. If you are over the age of 50, talk to your GP about the PSA blood test which can indicate if your prostate is healthy or not.
- A family history of cancer
A family history means that you have someone in your family who has cancer. Generally, if you have a father or brother diagnosed with prostate cancer, you are 2 to 3 times more likely to get prostate cancer yourself, compared to the average man.
The risk is much higher for men with several affected relatives, particularly if their relatives were young when the cancer was found. It is always worth knowing about your family history.
- Genes
Several inherited gene changes seem to raise prostate cancer risk, but they probably account for only a small percentage of cases overall. For example, inherited mutations of the BRCA1 or BRCA2 genes raise the risk of breast and ovarian cancers in some families. Mutations in these genes may also increase prostate cancer risk in some men.
- Ethnicity
Prostate cancer is more common in black Caribbean and black African men than in white or Asian men. Asian men have half the risk of white men.
- A previous cancer
What You Should Know About Prostate Cancer
Prostate Cancer is the second most common cancer in men.
The cancer begins when cells in the prostate, a gland found below the bladder and in front of the rectum, begin to grow uncontrollably.
When a male is young, the prostate gland is around the size of a walnut. However, the size of the prostate increases with age.
Most prostate cancer cases grow slowly, allowing for successful treatment options and a low mortality rate. More than two million men in the United States are prostate cancer survivors.
However, the danger comes when men do not recognize their symptoms or delay seeing a doctor.
You May Like: What Is Metastatic Prostate Cancer
Vitamin And Mineral Supplements
Vitamin D
An inverse relationship was observed between sunlight, or UVB exposure, and incidence of prostate cancer , suggesting that vitamin D deficiency might increase prostate cancer risk development . Similarly, discoveries were made by Barnett and Beer who found that people living in âsunnyâ countries were at lower risk of developing secondary solid cancer after melanoma compared to people living in âless sunnyâ countries.
The incidence of prostate cancer in African-American men is twice that of Caucasians, suggesting that race might play a role. There might be a role for vitamin D deficiency in this as UV radiation is blocked in darkly pigmented skin due to high melanin levels and this mechanism inhibits the conversion to vitamin D3 .
Vitamin E
Vitamin E is a vitamin which is fat soluble. Vegetable oils, egg yolks, and nuts are the important dietary sources of vitamin E. Tocopherols present in vitamin E have both potent cellular anti-oxidant with anticancer properties . Studies investigating the relationship between vitamin E and prostate cancer risk have shown contradicting results. The ATBC trial showed that in men who smoked supplementing daily vitamin E was not able to reduce the incidence of prostate cancer . In another large clinical trial , vitamin E supplementation did not show any benefit in 31,000 men with incident prostate cancer .
Selenium
Folate and vitamin B12
What Are The Stages Of Prostate Cancer
Cancer staging is first described using what is called a TNM system. The T refers to a description of the size or extent of the primary, or original, tumor. N describes the presence or absence of, and extent of spread of the cancer to lymph nodes that may be nearby or further from the original tumor. M describes the presence or absence of metastases usually distant areas elsewhere in the body other than regional lymph nodes to which the cancer has spread. Cancers with specific TNM characteristics are then grouped into stages, and the stages are then assigned Roman numerals with the numerals used in increasing order as the extent of the cancer being staged increases or the cancer prognosis worsens. Prognosis is finally reflected by considering the patients PSA score at presentation as well as their Gleason score in assigning a final stage designation.
The American Joint Commission on Cancer system for prostate cancer staging is as follows:
Traditionally, advanced prostate cancer was defined as disease that had widely metastasized beyond the prostate, the surrounding tissue, and the pelvic lymph nodes and was incurable. However, a more contemporary definition includes patients with lower grade disease with an increased risk of progression and/or death from prostate cancer in addition to those with widely metastatic disease.
The National Cancer Institute and the National Comprehensive Cancer Network guidelines on prostate cancer version 2.2017 indicate the following:
Recommended Reading: Prostate Cancer And Radiotherapy Treatment
Should I Poop Before A Prostate Exam
You dont need to change any bathroom habits prior to your appointment. If you feel like you need to poop before your exam, then its fine to do so. But dont worry if you just dont have the urge. The prostate exam shouldnt make you feel like you need to go.
Theres no need to be embarrassed about fecal matter during your prostate exam. Your healthcare provider is experienced in performing this exam and will do everything to ensure your comfort during the process.
Latest Prostate Cancer Data
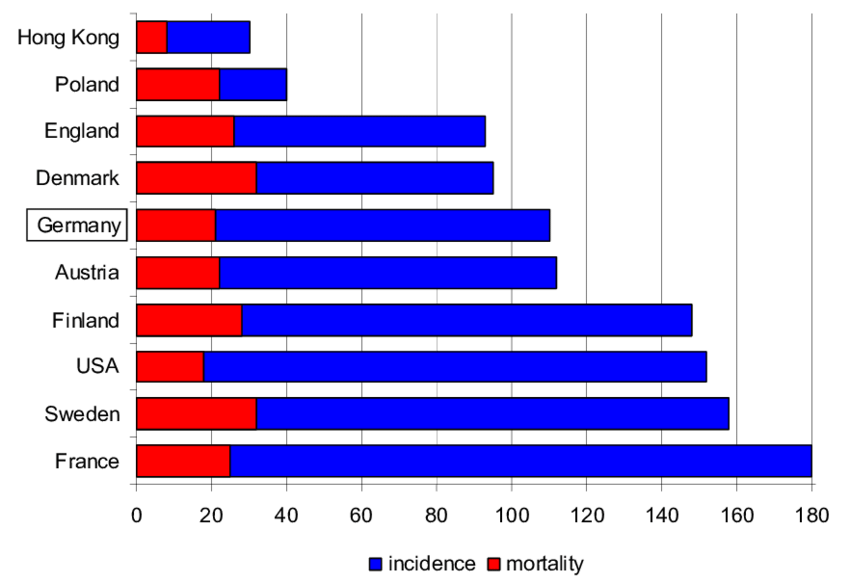
Prostate cancer is the 2nd most commonly occurring cancer in men and the 4th most common cancer overall. There were more than 1.4 million new cases of prostate cancer in 2020.
The 10 countries with the highest rates of prostate cancer and the highest number of deaths from prostate cancer in 2020 are shown in the tables below.
ASR = age-standardised rates. These are a summary measure of the rate of disease that a population would have if it had a standard age structure. Standardisation is necessary when comparing populations that differ with respect to age because age has a powerful influence on the risk of dying from cancer.
You May Like: What Pain Is Associated With Prostate Cancer
Obesity Insulin And Physical Activity
Obesity is linked to advanced and aggressive prostate cancer , and high body mass index is associated with more aggressive disease too and a worse outcome .
The possible explanation is that most of the time obese men present with alteration of circulating levels of metabolic and sex steroid hormones, which are known to be involved in prostate development as well as oncogenesis .
Obesity, particularly when combined with physical inactivity, leads to the development of insulin resistance with reduced glucose uptake. That, in turn, leads to chronically elevated blood levels of insulin. Insulin is a hormone that promotes growth and proliferation, thus is reasonable to add it in the list of risk factors that promote prostate cancer initiation and/or progression . Additionally, adipose cells represent a source of inflammation as well as of macrophages in adipose, which releases inflammatory mediators . Three meta-analyses reported a modest but consistent association between obesity and prostate cancer incidence independently of BMI increase . Data from three national surveys in the US population reported that obesity is associated with more aggressive prostate cancer and higher mortality despite its lower incidence .
Prostate Cancer: A Guide For Aging Men
Prostate cancer is one of the most frequently diagnosed cancers in the world, despite it only being diagnosed in males . In fact, more than 70 percent of men over the age of 80 have some quantity of cancer cells in their prostate.
Its so common that it sometimes doesnt go diagnosed until autopsies are performed, though that doesnt mean the cancer is the cause of death. On the contrary, the overall prognosis for men diagnosed with prostate cancer is as positive as you can get when talking about the dreaded c word. The five-year survival rates for the disease are close to 100 percent, especially when talking about prostate cancer that is caught early on in the processbefore it spreads.
The five-year survival rates for the disease are close to 100 percent, especially when talking about prostate cancer that is caught early on in the processbefore it spreads.
Nevertheless, prostate cancer is serious business, and the best way to handle a diagnosis is to be informed. Lets take a look at the frequency at which its diagnosed, how youre tested for it, how it can affect your daily life, and what we can do to try and prevent the disease.
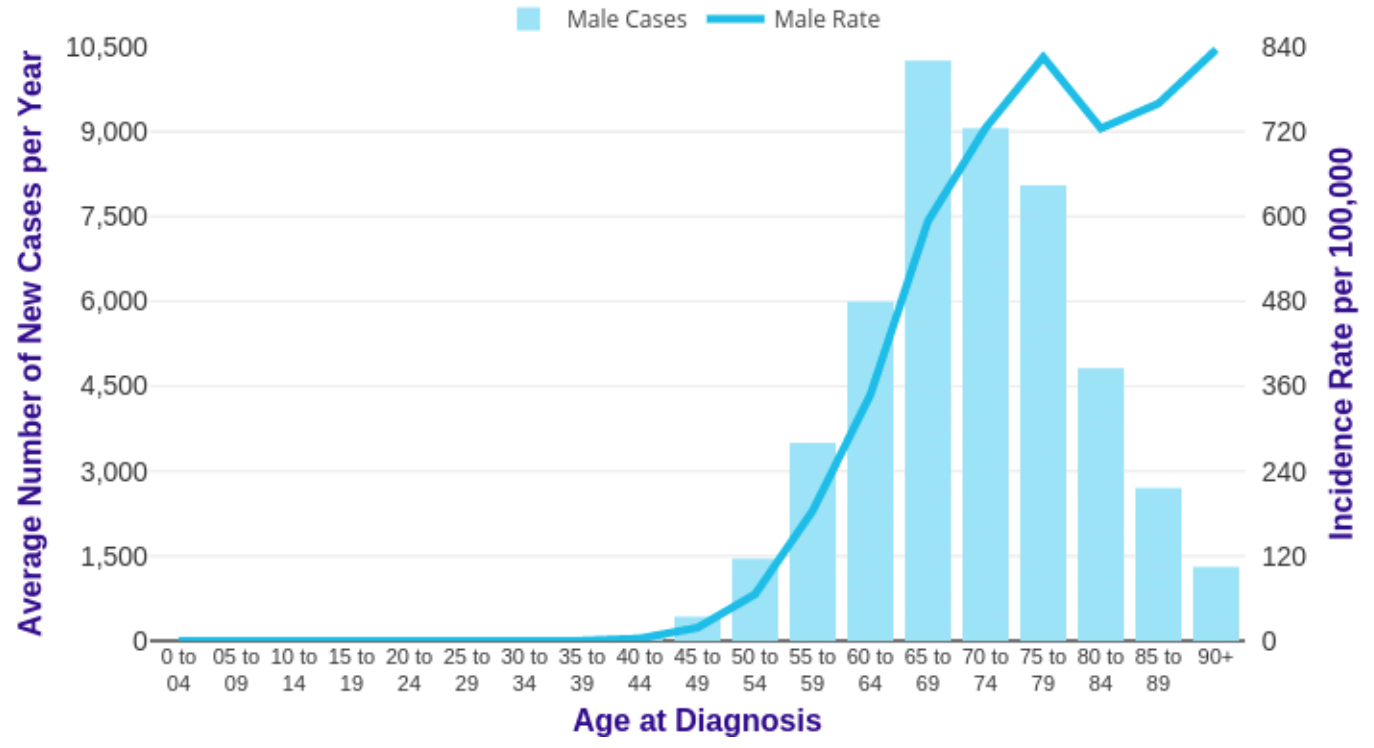
Average Age of Prostate Cancer Diagnosis
Also Check: Dying From Prostate Cancer What To Expect
Family History And Genetic Factors
It is estimated that about 20% of patients with prostate cancer report a family history, which may develop not only because of shared genes but also for a similar pattern of exposure to certain environmental carcinogens and common lifestyle habits . Several studies reported that inherited genetic background is associated with increased risk for prostate cancer, contributing to about 5% of disease risks . Particularly, this risk is increased by several folds when high-penetrance genetic âriskâ alleles are inherited, conversely to more common low-penetrance loci that increase the risk only modestly.
The X chromosome is also believed to have a role in prostate cancer inheritance, because it contains the androgen receptor and because small deletions in Xq26.3-q27.3 region were noted in sporadic and hereditary forms of prostate cancer . More recent studies in 301 hereditary prostate cancer affected families defined a number of other loci that may contribute to hereditary prostate cancer .