What Causes Prostate Cancer And Am I At Risk
Every man is at risk for prostate cancer as he ages. Although prostate cancer can affect younger men, about 6 out of 10 cases are diagnosed in men over the age of 65. The average age of diagnosis is 66. After non-melanoma skin cancer, prostate is the most common cancer diagnosed in men in the United States. The American Cancer Society estimates there will be 248,530 new cases of prostate cancer each year.
Although there are several known risk factors for getting prostate cancer, no one knows exactly why one man gets it and another doesn’t. Some important risk factors for prostate cancer are:
Stage 2 Prostate Cancer
In stage 2, the tumor is still confined to your prostate and hasnt spread to lymph nodes or other parts of your body. A doctor may or may not be able to feel the tumor during a prostate exam, and it may appear on ultrasound imaging. The survival rate is still near 100 percent.
The PSA score for stage 2 is less than 20 ng/mL.
Stage 2 cancer is further divided into three phases depending on the grade group and Gleason scores:
- Grade group: 1
- Gleason score: 6 or less
Correlative Studies Linking Lymph Node Metastasis With The Lymphangiogenic Axis In Human Prostate Cancer
A number of clinical studies have examined the relationship between lymphangiogenesis and prostate cancer lymph node metastasis . These studies produced conflicting results. Although some detected lymphangiogenesis in prostate cancer tissues, which were correlated with lymph node metastasis, others failed to observe such a correlation. Interestingly, most of these studies have observed increased expression of VEGF-C in tumor tissues of prostate cancer patients with lymph node metastasis. The major point of dispute has been whether the increased expression of lymphangiogenic growth factors and their receptors, such as VEGFR-3, in prostate cancer tissues induced lymphangiogenesis for lymph node metastasis, or whether they might facilitate increased invasion of tumor cells into lymphatic vessels. Thus, we will discuss the major findings of each study and attempt to reconcile these conflicting results.
Don’t Miss: How Many Radiation Treatments Are Needed For Prostate Cancer
The Ajcc Tnm Staging System
A staging system is a standard way for the cancer care team to describe how far a cancer has spread. The most widely used staging system for prostate cancer is the AJCC TNM system, which was most recently updated in 2018.
The TNM system for prostate cancer is based on 5 key pieces of information:
- The extent of the main tumor *
- Whether the cancer has spread to nearby lymph nodes
- Whether the cancer has spread to other parts of the body
- The PSA level at the time of diagnosis
- The Grade Group , which is a measure of how likely the cancer is to grow and spread quickly. This is determined by the results of the prostate biopsy .
*There are 2 types of T categories for prostate cancer:
- The clinical T category is your doctors best estimate of the extent of your disease, based on the results of the physical exam and prostate biopsy, and any imaging tests you have had.
- If you have surgery to remove your prostate, your doctors can also determine the pathologic T category . The pathologic T is likely to be more accurate than the clinical T, as it is done after all of your prostate has been examined in the lab.
Numbers or letters after T, N, and M provide more details about each of these factors. Higher numbers mean the cancer is more advanced. Once the T, N, and M categories have been determined, this information is combined in a process called stage grouping to get the overall stage of the cancer.
Cancer That Is Thought To Still Be In Or Around The Prostate
If the cancer is still thought to be just in the area of the prostate, a second attempt to cure it might be possible.
After surgery: If youve had a radical prostatectomy, radiation therapy might be an option, sometimes along with hormone therapy.
After radiation therapy: If your first treatment was radiation, treatment options might include cryotherapy or radical prostatectomy, but when these treatments are done after radiation, they carry a higher risk for side effects such as incontinence. Having radiation therapy again is usually not an option because of the increased potential for serious side effects, although in some cases brachytherapy may be an option as a second treatment after external radiation.
Sometimes it might not be clear exactly where the remaining cancer is in the body. If the only sign of cancer recurrence is a rising PSA level , another option for some men might be active surveillance instead of active treatment. Prostate cancer often grows slowly, so even if it does come back, it might not cause problems for many years, at which time further treatment could then be considered.
Factors such as how quickly the PSA is going up and the original Gleason score of the cancer can help predict how soon the cancer might show up in distant parts of the body and cause problems. If the PSA is going up very quickly, some doctors might recommend that you start treatment even before the cancer can be seen on tests or causes symptoms.
You May Like: What Happens When A Man Has Prostate Cancer
The Role Of Radical Prostatectomy In Management Of Pn+ Pca
Although direct comparison of different trials is a flawed approach, their collective results do provide interesting insights. At the same time as the EORTC was enrolling patients on protocol 30846, the Eastern Cooperative Oncology Group launched a randomized trial of immediate vs deferred ADT in patients who were found to have pathologically involved lymph nodes at the time of RP, but in contrast to the EORTC trial, these patients underwent RP and were randomly assigned to receive immediate, continuous ADT , or to be followed up and receive ADT when clinical recurrence was detected . With a median follow-up of 11.9 years, median overall survival was 13.9 vs 11.3 years in the immediate-ADT and delayed-ADT groups, respectively. In the immediate-ADT group, 41% of patients died of PCa compared with 89% in the delayed-ADT group.
TABLE
Outcomes for Patients Treated With Various Combinations of Androgen Deprivation Therapy and Local Therapies for Lymph NodePositive Prostate Cancer
Understanding Prostate Cancers Progression
To determine the appropriate treatment, doctors need to know how far the cancer has progressed, or its stage. A pathologist, the doctor trained in analyzing cells taken during a prostate biopsy, will provide two starting pointsthe cancers grade and Gleason score.
- Cancer grade: When the pathologist looks at prostate cancer cells, the most common type of cells will get a grade of 3 to 5. The area of cancer cells in the prostate will also be graded. The higher the grade, the more abnormal the cells.
- Gleason score: The two grades will be added together to get a Gleason score. This score tells doctors how likely the cancer is to grow and spread.
After a biopsy confirms prostate cancer, the patient may undergo additional tests to see whether it has spread through the blood or lymph nodes to other parts of the body. These tests are usually imaging studies and may include a bone scan, positron emission tomography scan or computed tomography scan.
Also Check: Do Men Need A Prostate
What Are The Treatments For Prostate Cancer
There are many different ways to treat prostate cancer. For prostate cancer, it is important that you get a second opinion and you will most likely be consulting multiple types of healthcare providers before making a final decision. You should talk to both urologists and radiation oncologists to hear about the benefits and risks of surgery, hormonal therapy and radiation in your particular case. If your prostate cancer has already spread at the time of diagnosis, you will also need a medical oncologist to talk about chemotherapy. The most important thing is to review your options and make a decision that best suits your lifestyle, beliefs and values.
Active Surveillance
Surgery
Surgery is a common form of treatment for men with prostate cancer. Surgery attempts to cure prostate cancer by removing the entire prostate and getting all of the cancer out of the body. An attempt at a surgical cure for prostate cancer is usually done with early stage prostate cancers. However, sometimes surgery will be used to relieve symptoms in advanced stage prostate cancers.
Talk to your surgeon about their complication rates before your operation. With surgery, urinary incontinence and impotence are often most severe right after the operation and generally get better with time. There are things that your providers can recommend to help you with either of these problems. Talk to your urologist about your options.
Radiation
You May Like: Is Zinc Good For Prostate
Gleason Prostate Cancer Score
1960s as a way to measure how aggressive your prostate cancer may be.
A pathologist determines your Gleason score by looking at a biopsy of your prostate tissue under a microscope. They grade the cells in the biopsy on a scale of 1 to 5. Grade 1 cells are healthy prostate, whereas grade 5 cells are highly mutated and dont resemble healthy cells at all.
The pathologist will calculate your Gleason score by adding together the number of the most prevalent type of cell in the sample and the second most prevalent type of cell.
For example, if the most common cell grade in your sample is 4 and the second most common is 4, you would have a score of 8.
A Gleason score of 6 is considered low-grade cancer, 7 is intermediate, and 8 to 10 is high-grade cancer.
Don’t Miss: Can You Have Radiation Twice For Prostate Cancer
Experiments With Tissue Culture & Animal Models Of Prostate Cancer
Experiments with tissue culture and animal models of prostate cancer have revealed the mechanisms of the synthesis of lymphangiogenic growth factors in prostate cancer and their important contribution to lymphangiogenesis in prostate cancer lymph node metastasis.
Signaling pathways for VEGF-C synthesis in prostate cancer
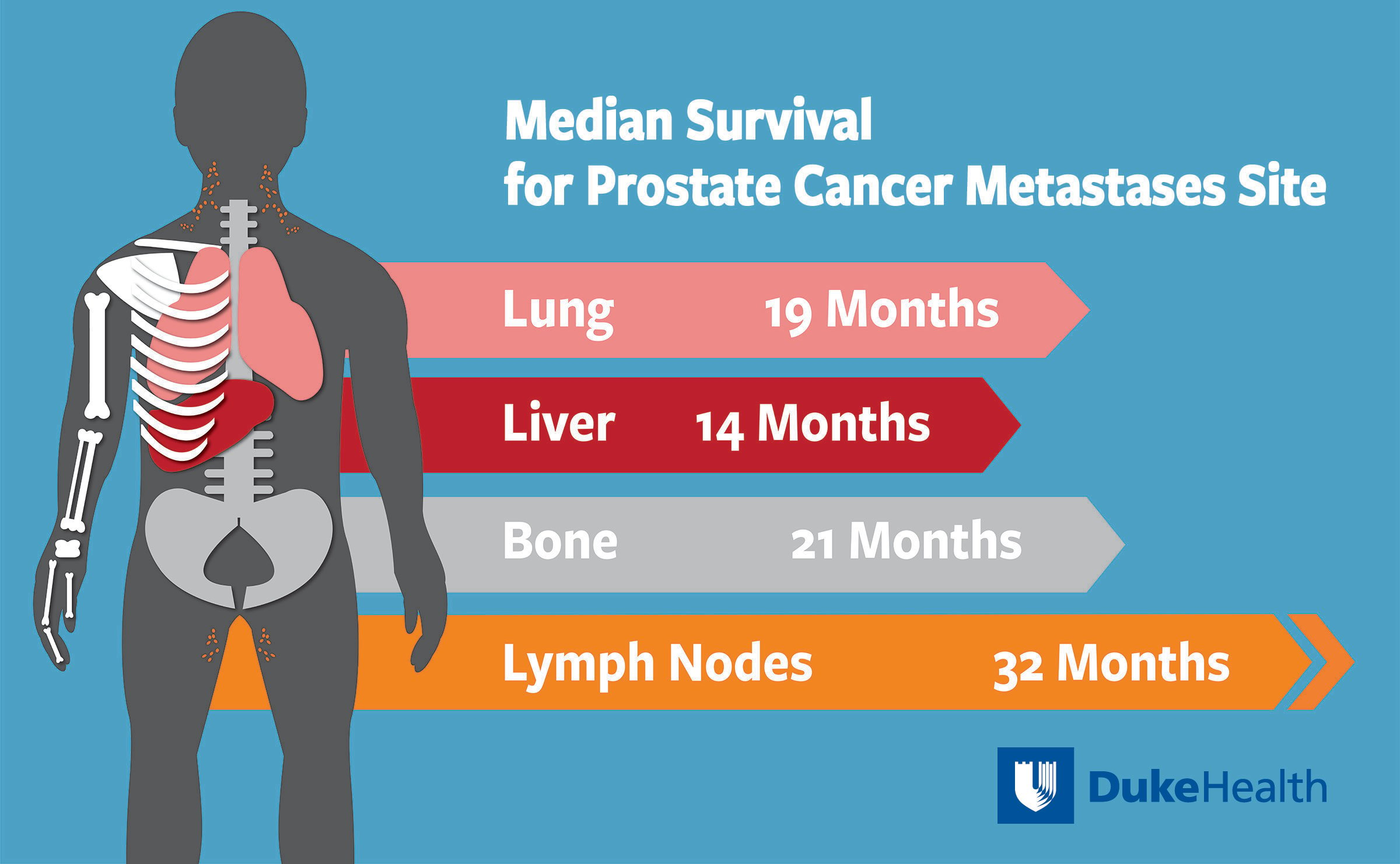
What Does It Mean For Prostate Cancer To Spread
Cancer cells can spread to other parts of the body. If this occurs, doctors say the cancer has metastasized or spread.
Areas of the body to which prostate cancer can spread include:
- the bones
- the lungs
- the lymph nodes, usually those around the pelvis
A doctor will typically recommend imaging scans and tissue samples to test for the presence of cancerous cells.
According to the Prostate Cancer Foundation, age is the biggest contributing factor to the risk for prostate cancer. An estimated 65 percent of all prostate cancers are diagnosed in men older than 65 years of age.
Additional risk factors for prostate cancer include:
- Family history: Men who have a father or brother with prostate cancer are twice as likely to get prostate cancer as men who do not.
- Race: African-American men face the greatest risk of prostate cancer.
- Smoking: A history of smoking is associated with a higher risk of aggressive prostate cancer.
Researchers are also studying a link between diet and increased prostate cancer risk. Diets low in vegetables or high in calcium have been linked to an increased risk of aggressive prostate cancer.
The prostate is very close to the point at which urine drains from the body. As a result, many prostate cancer symptoms affect the urination process. Examples of these symptoms include:
Some of these symptoms are associated with aging and an enlarged prostate. As a result, some men may ignore these symptoms instead of seeking medical attention.
Also Check: How To Get Rid Of Prostatitis
How To Detect Early Signs Of Cancer Of The Lymph Nodes
When cancer cells have spread to the lymph nodes, there are symptoms that will appear. These may include:
- Lymph node swelling or detectable lumps in the neck, under your arm, or in your groin area
- Shortness of breath
- Dizziness
- Body pain
There are patients that will experience all of these symptoms and some that will experience none. Therefore, a follow-up question may be: is cancer of the lymph nodes terminal if there are more symptoms?
The fact is symptoms vary based on where cancer has spread to and how aggressive it is. Its important to identify cancerous growths immediately to prevent their spread to other areas. When isolated to a certain region, the chances of it being terminal are less likely.
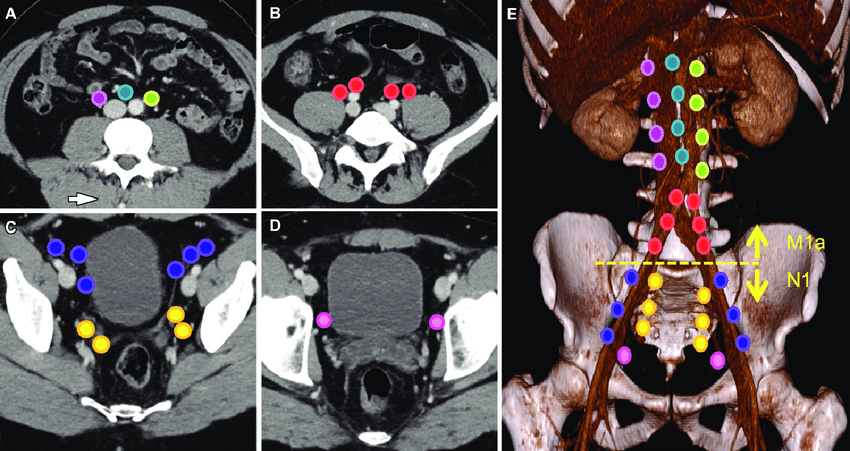
Clinical Lymph Node Metastatic Prostate Cancer
Patients with suspicious lymph nodes at imaging represent approximately 12% of all new PCa diagnosis.2 This rate is likely to increase within the next few years given the greater utilization of advanced preoperative imaging ,3 and a trend towards higher rates of newly diagnosed non-local confined disease observed during the past decade.4 The presence of clinical nodal metastases is associated with detrimental oncologic outcomes. As such, patients with node positive PCa are considered to have stage IV disease based on the National Comprehensive Cancer Network guidelines.6 In these guidelines, no distinction is made between distant metastatic disease and lymph node metastatic disease . Therefore, systemic therapies should be considered in PCa patients with suspicious lymph nodes at diagnosis.7
Also Check: What Is A Good Psa Reading For Prostate
Stage 1 Prostate Cancer
Stage 1 is the least advanced form of prostate cancer. Cancer in this stage is small and hasnt spread past the prostate gland. Its characterized by a PSA of less than 10 ng/mL, a grade group score of 1, and a Gleason score of 6.
Stage 1 prostate cancer has a 5-year survival rate of nearly 100 percent.
What Are The Stages Of Prostate Cancer
Your healthcare provider uses the Gleason score and Grade Groups to stage prostate cancer based on its projected aggressiveness. To get this information, the pathologist:
- Assigns a grade to each type of cell in your sample. Cells are graded on a scale of three to five . Samples that test in the one to two range are considered normal tissue.
- Adds together the two most common grades to get your Gleason score .
- Uses the Gleason score to place you into a Grade Group ranging from one to five. A Gleason score of six puts you in Grade Group 1 . A score of nine or higher puts you in Grade Group five . Samples with a higher portion of more aggressive cells receive a higher Grade Group.
Don’t Miss: What Are The Screening Tests For Prostate Cancer
What Is Cancer Of The Lymph Nodes
When cancer originates in the lymph nodes or other areas of the lymphatic system, its referred to as lymphoma.2 The most common types are hodgkins lymphoma and non-hodgkins lymphoma. In rare instances, theres also a chance for the development of lymphoma of the skin. If youre wondering, Is lymphoma hereditary, we cover this question in our latest blog article.
People with hodgkins lymphoma usually experience enlarged lymph nodes with a small number of Reed-Sternberg cells present surrounded by normal immune cells. With classic hodgkins lymphoma, which accounts for 9 out of 10 cases of this type of cancer, there are four subtypes that may develop.3 These are:
- Nodular sclerosis hodgkins lymphoma is the most common and tends to start in the lymph nodes in the neck or chest. Though it is more prevalent in teens and young adults, it can develop at any age.
- Mixed cellularity hodgkins lymphoma is the second most common subtype and occurs mainly in the lymph nodes found in the upper half of the body. Its mostly detected in people with HIV infection and affects mostly children and the elderly.
- Lymphocyte-rich hodgkins lymphoma is a rarer subtype and usually occurs in the upper half of the body in a few lymph nodes.
- Lymphocyte-depleted hodgkins lymphoma is the rarest subtype of this type of cancer and occurs mainly in older people with HIV infection. Its mostly found in lymph nodes in the stomach, spleen, liver, and/or bone marrow.
What Happens If My Cancer Starts To Grow Again
Your first treatment may help keep your cancer under control. But over time, the cancer may change and it may start to grow again.
You will usually stay on your first type of hormone therapy, even if its not working so well. This is because it will still help to keep the amount of testosterone in your body low. But there are other treatments that you can have alongside your usual treatment, to help control the cancer and manage any symptoms. Other treatments include:
Which treatments are suitable for me?
Which treatments are suitable for you will depend on many things, including your general health, how your cancer responds to treatment, and which treatments youve already had. Talk to your doctor or nurse about your own situation, or speak to our Specialist Nurses.
Read Also: Recovery Time After Green Light Laser Prostate Surgery
Questions To Ask Your Doctor Or Nurse
- What type of hormone therapy are you offering me and why?
- Are there other treatments I can have?
- What are the advantages and disadvantages of my treatment?
- What treatments and support are available to help manage side effects?
- Are there any lifestyle changes that might help me manage my cancer, symptoms, or side effects?
- How often will I have check-ups and what will this involve?
- How will we know if my cancer starts to grow again?
- What other treatments are available if that happens?
- Can I join any clinical trials?
- If I have any questions or get any new symptoms, who should I contact?
Soreness In The Groin
When prostate cancer spreads, its common for cancer cells to go to your lymph nodes and then move to more areas of your body. The lymph nodes are a network of glands that help your body filter fluids and fight infections.
There are several lymph nodes in your groin. These are the ones closest to your prostate, so its common for the cancer to spread to them first. Cancer cells prevent your lymph nodes from draining fluid and working properly. When this happens, your lymph nodes swell. As a result, you might experience pain or soreness in the area.
Recommended Reading: Man To Man Prostate Cancer Support Group