Table 2 What Guides Treatment Recommendations
Both of the situations below involve men diagnosed with a tumor that is small in size , yet who may require quite different treatments, based on their PSA level and Gleason score. Of course, many men have clinical profiles that vary from these two extremes.
Clinical profile Low PSA
Low Gleason score
80% of men with this profile probably have locally confined disease.
It is likely that fewer than 3% will have evidence of cancer in lymph nodes.
Surgery, radiation, or active surveillance . High PSA
High Gleason score
5% of men with this profile probably have locally confined disease.
More than 20% probably have evidence of cancer in the lymph nodes.
Systemic therapy rather than surgery .
Radical prostatectomy . The surgeon removes the prostate and seminal vesicles . In some cases, pelvic lymph nodes are also sampled. This is most often performed through an abdominal incision abdominal surgery may also be done with a laparoscope. A third option is the perineal technique, involving an incision in the area between the scrotum and the anus . The most common side effects are
- impotence
- mild to severe incontinence .
External beam radiation therapy. After a CT scan constructs a three-dimensional picture of the prostate and seminal vesicles, the radiation oncologist directs rays of high-energy radiation at the prostate tumor and sometimes at nearby lymph nodes. The most common side effects are
- impotence
- mild to severe incontinence .
- impotence
- mild to severe incontinence .
Gleason Score For Grading Prostate Cancer
Prostate cancer is also given a grade called a Gleason score. This score is based on how much the cancer looks like healthy tissue when viewed under a microscope. Less aggressive tumors generally look more like healthy tissue. Tumors that are more aggressive are likely to grow and spread to other parts of the body. They look less like healthy tissue.
The Gleason scoring system is the most common prostate cancer grading system used. The pathologist looks at how the cancer cells are arranged in the prostate and assigns a score on a scale of 3 to 5 from 2 different locations. Cancer cells that look similar to healthy cells receive a low score. Cancer cells that look less like healthy cells or look more aggressive receive a higher score. To assign the numbers, the pathologist determines the main pattern of cell growth, which is the area where the cancer is most obvious, and then looks for another area of growth. The doctor then gives each area a score from 3 to 5. The scores are added together to come up with an overall score between 6 and 10.
Gleason scores of 5 or lower are not used. The lowest Gleason score is 6, which is a low-grade cancer. A Gleason score of 7 is a medium-grade cancer, and a score of 8, 9, or 10 is a high-grade cancer. A lower-grade cancer grows more slowly and is less likely to spread than a high-grade cancer.
What Do My Test Results Mean
Your doctor will look at your test results to find out if the cancer has spread and how quickly it might be growing.
How far has my cancer spread?
The stage of your cancer tells you whether it has spread outside the prostate and how far it has spread. You might need scans, such as an MRI, CT or bone scan, to find out the stage of your cancer.
Depending on the results, your cancer may be treated as:
- localised prostate cancer it’s contained inside the prostate
- locally advanced prostate cancer its started to break out of the prostate or has spread to the area just outside it
- advanced prostate cancer its spread from the prostate to other parts of the body.
Is my cancer likely to spread?
Your doctor may talk to you about the risk of your cancer spreading outside the prostate or coming back after treatment.
Your prostate biopsy results will show how aggressive the cancer is in other words, how likely it is to spread outside the prostate. You might hear this called your Gleason grade, Gleason score, or grade group.
To work out your risk, your doctor will look at your PSA level, your Gleason score and the T stage of your cancer.
Low risk
Your cancer may be low risk if:
- your PSA level is less than 10 ng/ml, and
- your Gleason score is 6 or less , and
- the stage of your cancer is T1 to T2a.
Medium risk
Your cancer may be medium risk if:
- your PSA level is between 10 and 20 ng/ml, or
- your Gleason score is 7 , or
- the stage of your cancer is T2b.
High risk
What happens next?
Also Check: What Food Causes Enlarged Prostate
Does Untreated Clinical Gleason 6 Disease Cause Symptoms Or Death
Several studies that examined the natural history of untreated prostate cancer diagnosed in the prePSA screening era have suggested that men with Gleason 6 cancers are at risk for prostate cancerspecific mortality beyond 10 years of follow-up. The majority of the Gleason 6 disease was T1a/b disease, which was identified at the time of transurethral resection of the prostate for benign disease. Today, it is extremely rare to diagnose T1a/b disease because fewer TURPs are performed and those undergoing TURP have been prescreened with PSA testing. The results of the natural history studies in the PSA screening era are also problematic because many of the cases were likely misclassified at the outset because of the aforementioned limitations attributable to the random-systematic tissue sampling guided by TRUS.
With reported median follow-up ranging from 22 to 82 months, current active surveillance cohorts remain immature at this time, and longer follow-up will be necessary to draw definitive conclusions. Thus far, cancer-specific survival among these cohorts has been > 97%, and there are no data to suggest inferior outcomes after delayed radical therapy, as compared with immediate therapy.
What Does It Mean If In Addition To Cancer My Biopsy Report Also Says Acute Inflammation Or Chronic Inflammation

Inflammation of the prostate is called prostatitis. Most cases of prostatitis reported on a biopsy are not caused by infection and do not need to be treated. In some cases, inflammation may increase you PSA level, but it is not linked to prostate cancer. The finding of prostatitis on a biopsy of someone with cancer does not affect their prognosis or the way the cancer is treated.
Read Also: Procedure To Clean Out Prostate
The Gleason 6 Cancer Deception
The all-inclusive prostate cancer label is deceitful by implying that all prostate cancers are equal and have the power to kill rapidly whereas it has been well established that the very common Gleason 6 type of prostate cancer fails to behave as a cancer and, should not be called a cancer.
In fact, Larry Klotz M.D. and others, have shown irrefutably that the Gleason 6 prostate cancer is a not a real cancer at all for two fundamental reasons: no man has died from this disease and, this so-called cancer lacks a number of molecular biological mechanisms normally found in cancerous behaving cells. Furthermore, unlike a typical cancer cell, this cell has a very long doubling time at 475 +/ 56 days so that from mutation to a growth of about 1 cm in diameter takes some 40 years.
Therefore, because the Gleason 6 lacks the hallmarks of a cancer, it is not a health risk, it does not progress to become a health risk, needs no detection and, needs no treatment. The Gleason 6 is a pseudo-cancer mislabeled as a cancer this false cancer tag is a monstrous medical error and public health disaster, inviting legal retribution. Only the 15% or so of the high-grade forms of prostate cancers have the potential to kill and, only they demand detection and treatment.
How Reliable Is Our Detection Of Gleason 6 Disease
Before the PSA screening era began in the late 1980s, prostate cancer was usually diagnosed by directing a biopsy needle into a nodule detected at the time of a digital rectal examination. In most cases, the nodule occupied a significant proportion of the gland. Often, gross extracapsular disease was evident at the time of diagnosis. Low-grade cancers were rarely diagnosed unless they were incidental findings at the time of transurethral prostatectomy for benign disease.
The detection of prostate cancer in the PSA era requires a random biopsy technique because transrectal ultrasonography does not reliably identify the site of clinically significant disease. Therefore, many Gleason 6 cancers identified on biopsy coexist with higher-grade disease missed by random biopsy. Mufarrij et al examined the prostates of 205 and 771 men who met the Epstein or Klotz criteria, respectively, for active surveillance and who underwent radical prostatectomy. By definition, all of these men had Gleason 6 cancers on prostate biopsy. Between 45.9% and 47.2% had Gleason grade 4/5 disease, and 7.8% to 10.9% had evidence of extracapsular extension. The 5-year biochemical-diseasefree survival was estimated to be 83.2% to 92.9% despite curative intervention. Others have confirmed the unreliability of Gleason grading attributable to random biopsy, which remains an essential limitation in assigning men to active surveillance.
Recommended Reading: What Can You Do To Help An Enlarged Prostate
Prostate Cancer Quackery And Money
Much of the medical information and advice dispensed today cannot be trusted as it is heavily influenced by money and, just as Pavlovs dog salivated every time he anticipated a reward, endless financial incentives for healthcare evaluations and treatments generate predictable physician responses.
So it is for prostate cancer management where urologists receive unlimited financial rewards for testing and treatments whether or not they have been scientifically validated or, even necessary. Shamefully, many urologists have lost all connection to the Hippocratic Oath as they are determined to protect the financial windfall from their sham PSA-based screening of healthy males and their ill-founded radical prostatectomy treatment. Especially, when they know full well that the downstream effects from their prostate cancer screening and treatment philosophy fails to extend life and often leaves men with after effects worse than the disease itself.
Surprisingly, the history of medicine is replete with these misguided treatment philosophies that, through academic hubris, paternalism and obedience, gave rise to a herd mentality and consensus medicine. In fact, it is only through consensus medicine that radical surgery for prostate cancer became standard practice and, when perverse financial incentives came along, the focus of prostate cancer management became much less about the patient and much more about the money.
There Are Different Criteria
I have been on active surveillance for ten years, and have had no progression in my disease. My recent MRI and biopsy are the same as in 2009. But, while I have enjoyed those years of living normally, I have also been frequently tested within a formal study group.
With your number of positive cores, you would not be accepted into the AS program at Johns Hopkins, but you would be welcomed into our long-time rival program at Sunnybrook. That is Laurence Koltz research group. You can google him for a lot more information.
I recommend that you get a copy of Dr. Mark Scholz new book The Key to Prostate Cancer. In it, 30 prostate cancer experts describe the treatment, including AS, that they provide for men with different risk levels.
Read Also: How Is Prostate Laser Surgery Performed
Gleason : Is It A Cancer
This important question has significant clinical and public health implications. Unfortunately, there is no simple answer. There are substantial limitations to our ability to accurately risk stratify detected prostate cancers. As a result of random systematic biopsies, Gleason 6 disease often coexists with undetected higher-grade disease. Some argue that this alone justifies labeling Gleason 6 disease as a cancer. We disagree. By extension of this guilt-by-association reasoning, high-grade prostatic intraepithelial neoplasia and atypical small cell acinar proliferation, both of which are known to coexist with undetected cancer, should be labeled as cancers. In fact, we know that many cancers remain undiagnosed owing to a false-negative biopsy that shows only benign prostatic hyperplasia. Is benign prostatic hyperplasia cancer? Where do we draw the line?
What Do The Results Mean
A higher Gleason score indicates more aggressive prostate cancer. Typically, lower scores suggest a less aggressive cancer.
In most cases, scores range between 610. Doctors do not often use biopsy samples that score 1 or 2, as they are not usually the predominant areas of the cancer.
A Gleason score of 6 tends to be the lowest possible score. A doctor will describe prostate cancer with a score of 6 as being well differentiated, or low grade. This means that the cancer is more likely to have a slower rate of growth.
Scores in the 810 region are poorly differentiated, or high grade. In these cases, the cancer is likely to spread and grow quickly. The growth rates of cancers with a score of 9 or 10 are likely to be twice as high as those of a cancer with a score of 8.
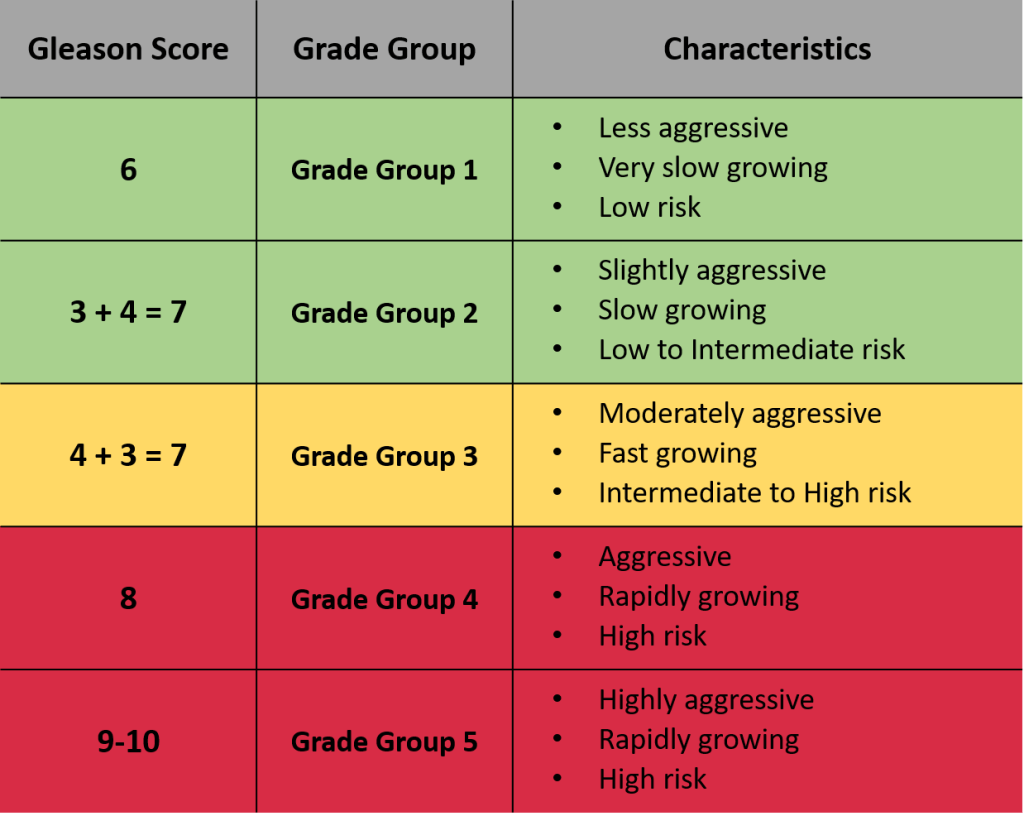
A score of 7 can be broken down in two ways:
- 3 + 4 = 7
- 4 + 3 = 7
This distinction indicates how aggressive the tumor is. Scores of 3 + 4 typically have a good outlook. A score of 4 + 3 is more likely to grow and spread than the 3 + 4 score, but less likely to grow and spread than a score of 8.
Some people receive multiple Gleason scores. This is because the grade may vary between samples of the same tumor or between two or more tumors.
In these cases, doctors are likely to use the higher score as the guide for treatment.
The Gleason score is an important tool for doctors when deciding on the best course of treatment. However, additional factors and grouping systems can assist them in making this decision.
Don’t Miss: Best Over The Counter For Enlarged Prostate
What Does Gleason 6 Mean
A Gleason score of 6 is different from other prostate cancer diagnoses because it means all the biopsy samples are grade 3 . Though the samples dont look like normal tissue, no grade 4 or 5 samples were found.
Gleason 6 prostate tumors are:
- Small
- Confined to the prostate
- Not causing any symptoms
There are changes at the cellular level, but the prostate cancer is likely slow-growing and has a low-risk of metastasizing, or spreading to other areas of the body.
This knowledge allows your doctor to monitor you and see how your tumor changes over time.
What Does It Mean If In Addition To Cancer My Biopsy Report Also Mentions Acute Inflammation Or Chronic Inflammation
Inflammation of the prostate is called prostatitis. Most cases of prostatitis reported on biopsy are not caused by infection and do not need to be treated. In some cases, inflammation may increase your PSA level, but it is not linked to prostate cancer. The finding of prostatitis on a biopsy of someone with prostate cancer does not affect their prognosis or the way the cancer is treated.
Also Check: City Of Hope Prostate Cancer Clinical Trials
Active Surveillance For Prostate Cancer
If diagnosed with localized prostate cancer , disease management can take many forms, depending on the risk category of disease. Patients with low-grade, slow-growing tumors confined to the prostate gland may consider active surveillance. This involves monitoring prostate cancer in its localized stage until your doctor feels that further treatment is needed to halt the disease at a curable stage.
According to the American Society of Clinical Oncology, patients with low-risk, low-grade disease can consider active surveillance. It may also be an option for patients with a Gleason score of 7. Patients within these categories may choose to postpone prostate cancer treatment because of its associated risks and side effects.
The Following Is A Duplicate Of One That I Posted Here: Http: //csncancerorg/node/305388
. . . People here know me as an outspoken advocate for CK and against surgery of any kind. I was treated w/CK 6 years ago . You can troll the forum for my many comments on this point. Here are the highlights of what you need to consider:
1) CK currently is the most precise method of delivering radiation externally to treat prostate cancer. Accuracy at the sub-mm level in 360 degrees and can also account for organ/body movement on the fly during treatment. Nothing is better. Accuracy minimizes the risk of collateral tissue damage to almost nil, which means almost no risk of ED, incontinence and bleeding. Treatment is given in 3-4 doses w/in a week time w/no need to take off time from work or other activities.
2) IMRT is the most common form of external radiation now used. Available everythere. Much better accuracy than before but no where near as good as CK. So, it comes with a slightly higher risk of collateral tissue damage resulting in ED, incontienence and bleeding. Unless things have changed, IMRT treatment generally requires 40 treatments — 5 days a week for 8 weeks — to be completed. I think some treatment protocols have been reduce to only 20 but I’m not sure. Still much longer and more disruptive to your life than CK but, if CK is not available, you may have no other choice.
Good luck!
Also Check: How To Avoid Getting Prostate Cancer
How Do I Know The Gleason Grade Is Accurate
Assigning the correct Gleason score is a skill just like any other that is developed through experience and practice. It is often prudent to have the biopsy material referred for a second opinion at a reference center to confirm the accuracy of the initial Gleason score that was assigned.
References: