How Does Hormone Therapy For Prostate Cancer Work
LHRH, or luteinizing-hormone releasing hormone, is one of the key hormones released by the body that initiates the production of testosterone.
LHRH Agonists: One of the most common hormone therapies in prostate cancer involves blocking the release of LHRH through the use of agonists . LHRH agonists cause a testosterone flare reaction, which is an initial transient rise in testosterone that happens over the first week or two after the first treatment.
LHRH Antagonists: These are a class of medications that can block LHRH from stimulating testosterone production without causing an initial testosterone surge.
Im Worried About All The Side Effects From Prostate Cancer Medications What Can I Do
Carefully review the side effect profile of the different hormone therapy regimens, and discuss with your health care team potential ways to minimize the effects. In the end, its important that you not only understand the value of the therapy in the management of your prostate cancer, but also that you learn how to live your life as best as possible while fighting the disease.
Are Other Tests Needed
A doctor will not generally recommend further treatment after a single PSA test result. They will typically monitor a persons PSA levels over time to see whether they are rising.
PSA testing is only one way to check a persons health after having a prostatectomy. A doctor may use an imaging test to look for a tumor or a growing number of cancer cells.
They are also likely to ask the individual about any possible symptoms that could suggest that prostate cancer has returned.
Don’t Miss: Bowel Problems After Radiotherapy For Prostate Cancer
Standard Treatment Options For Stage Ii Prostate Cancer
Standard treatment options for patients with stage II prostate cancer include the following:
Watchful waiting or active surveillance/active monitoring
Asymptomatic patients of advanced age or with concomitant illness may warrant consideration of careful observation without immediate active treatment. Watch and wait, observation, expectant management, and active surveillance/active monitoring are terms indicating a strategy that does not employ immediate therapy with curative intent. .
Evidence :
Radical prostatectomy
Radical prostatectomy, usually with pelvic lymphadenectomy is the most commonly applied therapy with curative intent. Radical prostatectomy may be difficult after a transurethral resection of the prostate .
Evidence :
Evidence :
Your Cancer Care Team
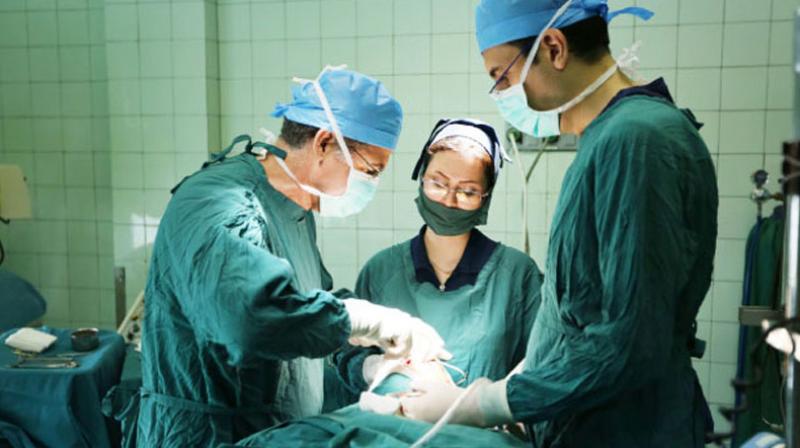
People with cancer should be cared for by a multidisciplinary team . This is a team of specialists who work together to provide the best care and treatment.
The team often consists of specialist cancer surgeons, oncologists , radiologists, pathologists, radiographers and specialist nurses.
Other members may include physiotherapists, dietitians and occupational therapists. You may also have access to clinical psychology support.
When deciding what treatment is best for you, your doctors will consider:
- the type and size of the cancer
- what grade it is
- whether the cancer has spread to other parts of your body
Don’t Miss: Ablation Treatment For Prostate Cancer
Ive Had A Prostatectomy Am I At Risk Of Cancer Returning
Although all forms of cancer are technically a cellular mutation that cannot necessarily be prevented or controlled, there are factors that may increase the risk of prostate cancer recurrence, even after surgery. These include, but are not limited to, the following:
- Stage of Prostate Cancer
- If the prostate cancer was detected in a later stage, or if cancerous tissue or tumor growth is significantly progressed, a prostatectomy may be slightly less effective for the purposes of controlling future susceptibility to recurrence.
Advancing Prostate Cancer Care
At Memorial Sloan Kettering, we tailor multimodal approaches to the individual features of each patients cancer. Radical prostatectomy is a complex procedure that requires a high level of technical precision. We provide state-of-the-art surgical techniques, including minimally invasive robotic and nerve-sparing surgery. Over the past few decades, we have dramatically reduced surgical complications by incorporating imaging test results in surgical plans to ensure the avoidance of other structures and the minimization of the risk of incontinence and erectile dysfunction. Our multidisciplinary prostate cancer team includes radiation oncologists who provide the latest radiotherapy approaches, including image-guided and intensity-modulated radiation therapy, stereotactic radiosurgery, proton therapy, and brachytherapy.
The field of prostate cancer care is evolving rapidly. We continue to explore new ways to improve outcomes and safety and effectiveness through clinical trials, in which we are testing new drugs and drug combinations, surgery and radiation therapy techniques, diagnostic approaches, and strategies for improving quality of life for men undergoing treatment for prostate cancer.
Disclosure: Peter Scardino sits on a clinical advisory board for OPKO Health outside the submitted study he also holds a patent issued by OPKO.
Read Also: Do Men Need A Prostate
Read Also: Prostate Cancer Support Association Of New Mexico
How Is Prostate Cancer Recurrence Treated
Your treatment for prostate cancer relapse will depend on your PSADT and a number of other factors. Some relapses are so low-grade that no treatment at all will be required.
For example, someone with a PSADT of more than 12 months and a PSA level of less than 10 ng/mL may be monitored with repeat PSA tests. Or, relapse may occur in an older person whose life expectancy makes treatment unlikely or unnecessary.
Treatments for prostate cancer relapse may include surgery, radiation, and medication. Keep in mind that the treatment strategy is tailored to the level of relapse: low, intermediate, or high.
It also will depend on whether your initial prostate cancer was treated with surgery or radiation.
Treating Prostate Cancer That Doesnt Go Away Or Comes Back After Treatment
If your prostate-specific antigen blood level or another test shows that your prostate cancer has not been cured or has come back after the initial treatment, further treatment can often still be helpful. Follow-up treatment will depend on where the cancer is thought to be and what treatment you’ve already had. Imaging tests such as CT, MRI, or bone scans may be done to get a better idea about where the cancer is.
Also Check: What Are The Symptoms Of Prostate Cancer Men’s Health
How Is A Recurrence Detected
After prostate cancer treatment, you will go for medical check-ups every few months as determined by your doctor. At each follow-up appointment, your doctor will order a blood test to measure PSA levels. This test helps your doctor detect a cancer recurrence. You will also be examined. New symptoms should be reported to the doctor, as these may prompt other testing.
When PSA test results suggest that the cancer has come back or continued to spread, X-rays or other imaging tests may be done, depending on your situation and symptoms. Your doctor may use a radioactive tracer called Axumin with a PET scan to help detect and localize any recurrent cancer so that it could be biopsied or treated.
Your doctor may also use a new drug called Ga 68 PSMA-11 in the scan which binds to PSMA-positive prostate cancer lesions in the tissues of the body so they can be targeted for treatment.
What Happens If Prostate Cancer Comes Back
The prostate is a small gland about the size of a walnut that helps make seminal fluid. Its intertwined with your urinary tract system, resting below your bladder and surrounding the urethra. As you age, this gland continues to grow, sometimes resulting in benign prostatic hyperplasia. While this growth is normal, cancerous growth is not. Cancer occurs when the cells in your prostate gland begin to grow out of control.
While prostate cancer is common, especially among older men, its got a fairly positive outcome. When caught early and treated, most men survive and continue on with remission after five years. Unfortunately, for a small percentage of men, the cancer returns. To give you some clarity on this situation, heres what happens if prostate cancer comes back.
You May Like: Proton Beam Therapy For Prostate Cancer Locations
Caring For The Catheter
You will be discharged with a Foley catheter, a tube that continuously drains urine from your bladder into a bag and that you will use for seven to 10 days. Before you leave the hospital, your nurse will teach you how to empty and care for your catheter and drainage bag. The catheter works with gravity and should be draining urine at all times, so you have to keep the drainage bag below your bladder at all times, even when you shower. If your urine is not draining, lower the bag and check the connection for kinks or loops. Loops can cause an air lock that prevents drainage. You can also try emptying the bag. Then try briefly disconnecting the catheter from the clear plastic tubing to allow a little air into the system. Your nurse will show you how to do this before your discharge.
To prevent infection, you must keep your catheter clean. This section explains how to clean the catheter, the area around the catheter and the drainage bag. It also explains how to apply your leg bag and secure the catheter to your leg.
We will provide most of the supplies you need to care for your catheter. They include:
- Blue clamp
- StatLock Foley catheter securement device
- Shaving supplies
You should empty the catheter bag when it’s half full. This helps prevent air locks from developing in the tubing.
To apply the leg bag:
Life Expectancy And Localized Prostate Cancer
So how do these treatments affect life expectancy? In one study, researchers in Switzerland examined the treatment and outcomes of 844 men diagnosed with localized prostate cancer. They compared men who had been treated with prostatectomy, radiotherapy and watchful waiting and found that at five years from diagnosis, the type of treatment made little difference to survival. When the researchers went to 10 years from diagnosis, they did find a difference in survival based on treatment, but it was fairly small.
After 10 years, 83 percent of the men who had gotten a prostatectomy were still living, compared to 75 percent who had undergone radiotherapy and 72 percent who took a watchful waiting approach.
Also Check: Can Enlarged Prostate Cause Back And Leg Pain
What Does Psa Velocity Mean
PSA velocity or PSA doubling time, both of which measure the rate at which your PSA rises, can be a very significant factor in determining is the aggressiveness of your cancer. Men with a shorter PSA doubling time or a more rapid PSA velocity after initial therapy tend to have more aggressive disease, and are therefore more likely to need more aggressive therapies. Likewise, men who have recurrence soon after surgery have a higher risk of aggressive disease.
How Prostate Cancer Recurrence Is Detected
Following surgery for prostate cancer removal, the majority of patients will have regular appointments to check in and assess recovery progress with their healthcare provider or preferred oncologist. At each of these visits, your doctor will draw blood to run tests on various levels of biomarkers, hormones, and immunological markers, including PSA. You may also undergo minor physical assessments as part of your post-prostatectomy preventive maintenance care plan.
If prostate specific antigen levels are found to be rising, staying the same as pre-operative quantities, or slowing their rate of decrease in an unexpected way, your provider may suggest imaging tests or an X-ray of the prostate and pelvic area. A few other alternative options for detecting prostate cancer recurrence are available, although some are in the early stages of development or are not yet widely available, so should not be used as a default or go-to option for determining whether metastatic resurgence is a clear and present health risk.
Are you a practicing healthcare provider or oncologist who would like to learn more about alternative options for localized detection of recurrent prostate cancer?
Check out the full infographic here.
You May Like: How To Lower Prostate Cancer Risk
What Is The Life Expectancy After Prostate Removal
. Besides, can you live a long life after prostate cancer?
You can live a long time with prostate cancer, maybe even decades. If you catch and treat it early, you might even be able to cure it.
Secondly, can you still get hard if you have your prostate removed? When you have a radical prostatectomy, you have surgery to remove your prostate gland. These nerves, blood vessels, and muscles may be weakened when you have surgery for your prostate cancer. However, you may find that you cannot have an erection even a year or more after surgery.
Moreover, what happens if you have your prostate removed?
Side effects of prostate surgery. The major possible side effects of radical prostatectomy are urinary incontinence and erectile dysfunction . Men with stress incontinence might leak urine when they cough, laugh, sneeze, or exercise.
Are you ever cured of prostate cancer?
The short answer is yes, prostate cancer can be cured, when detected and treated early. The vast majority of prostate cancer cases are discovered in the early stages, making the tumors more likely to respond to treatment. Treatment doesnt always have to mean surgery or chemotherapy, either.
What To Ask When Your Psa Is Rising After Initial Treatment
For the majority of men, prostate cancer is treatable and curable and does not come back after initial treatment. However, about 25%33% of men with prostate cancer will experience a recurrence of their cancer after surgery or radiation. Some of these men can still be cured with additional treatment, but some men develop a form of prostate cancer that, while not curable, remains TREATABLE for a very long time.
Below is a list of questions to ask when your PSA is rising after initial treatment.
Don’t Miss: What Are The Grades Of Prostate Cancer
Survival Rates For Bladder Cancer
Survival rates can give you an idea of what percentage of people with the same type and stage of cancer are still alive a certain amount of time after they were diagnosed. They cant tell you how long you will live, but they may help give you a better understanding of how likely it is that your treatment will be successful.
Keep in mind that survival rates are estimates and are often based on previous outcomes of large numbers of people who had a specific cancer, but they cant predict what will happen in any particular persons case. These statistics can be confusing and may lead you to have more questions. Talk with your doctor about how these numbers may apply to you, as he or she is familiar with your situation.
Read Also: Prostate Biopsy Cost In Usa
Normal Pelvic Anatomy After Radical Prostatectomy
RP includes total removal of the prostate and seminal vesicles, along with pelvic lymph node dissection. Postradical prostatectomy MRI findings include descent of the bladder which is anastomosed to extra prostatic distal urethra. The vesico-urethral-anastomosis should be visualized as a ring of postoperative fibrosis with low signal intensity on all sequences . Seminal vesicle which are supposed to be removed, may be retained in part with postoperative findings highly variable: 20% of the patients had SV remnants, with similar location of the preoperative SV position, with an additional 38% with fibrotic SV tips .
Figure 1 Postsurgical imaging findings after radical prostatectomy on sagittal and axial T2-weighted imaging: bladder neck descended into the prostatectomy fossa with a more conical shape the VUA anastomosis visualized as a ring of postoperative fibrosis on low signal intensity inferior to the bladder neck. Seminal vesicles which are supposed to be removed in a classical RP demonstrate a low signal intensity , but may be retained in part and can be seen in their presurgical locations with their characteristic tubular structure on T2W .
Don’t Miss: Is Coffee Bad For Your Prostate
Additional Treatment After Surgery
Additional treatment can come with one of two approaches: treatment given as adjuvant therapy , or as salvage therapy . In the modern era, most additional treatment is given as salvage therapy because firstly this spares unnecessary treatment for men who would never experience recurrence, and secondly because the success rates of the two approaches appear to be the same.
Regardless of whether an adjuvant or salvage therapy approach is taken, the main treatment options following biochemical recurrence are:
- Radiotherapy this is the commonest approach. Because scans dont show metastatic deposits until the PSA is more than 0.5 ng/ml and because radiotherapy is more effective when given before this level is reached, the radiotherapy energy is delivered to the prostate bed. This is because we know that this is the commonest site of recurrence in most men, and that 80% of men treated in this way will be cured.
- Active surveillance this is appropriate for a very slowly-rising PSA in an elderly patient who has no symptoms.
- Hormonal therapy in many ways this is the least appealing option as it causes symptoms but does not cure anyone, although it does control the recurrence and lower the PSA.