Im Worried About All The Side Effects From Prostate Cancer Medications What Can I Do
Carefully review the side effect profile of the different hormone therapy regimens, and discuss with your health care team potential ways to minimize the effects. In the end, its important that you not only understand the value of the therapy in the management of your prostate cancer, but also that you learn how to live your life as best as possible while fighting the disease.
Risks Of Prostate Surgery
The risks with any type of radical prostatectomy are much like those of any major surgery. Problems during or shortly after the operation can include:
- Reactions to anesthesia
- Blood clots in the legs or lungs
- Damage to nearby organs
- Infections at the surgery site.
Rarely, part of the intestine might be injured during surgery, which could lead to infections in the abdomen and might require more surgery to fix. Injuries to the intestines are more common with laparoscopic and robotic surgeries than with the open approach.
If lymph nodes are removed, a collection of lymph fluid can form and may need to be drained.
In extremely rare cases, a man can die because of complications of this operation. Your risk depends, in part, on your overall health, your age, and the skill of your surgical team.
The Risk Of Your Cancer Coming Back
For many men with localised or locally advanced prostate cancer, treatment is successful and gets rid of the cancer. But sometimes not all the cancer is successfully treated, or the cancer may have been more advanced than first thought. If this happens, your cancer may come back this is known as recurrent prostate cancer.
One of the aims of your follow-up appointments is to check for any signs that your cancer has come back. If your cancer does come back, there are treatments available that aim to control or get rid of the cancer.
Your doctor cant say for certain whether your cancer will come back. They can only tell you how likely this is.
When your prostate cancer was first diagnosed, your doctor may have talked about the risk of your cancer coming back after treatment. To work out your risk, your doctor will have looked at your PSA level, your Gleason score and the stage of your cancer. If your prostate has been removed, it will have been sent to a laboratory for further tests. This can give a better idea of how aggressive the cancer was and whether it is likely to spread. If you dont know these details, ask your doctor or nurse.
You May Like: How To Prevent Prostate Cancer Naturally
How Is The Treatment Carried Out
NanoKnife involves no knives at all, according to a breakdown of the op by the King Edward VII’s Hospital.
‘The treatment is delivered via a needle puncture through the skin,’ it says.
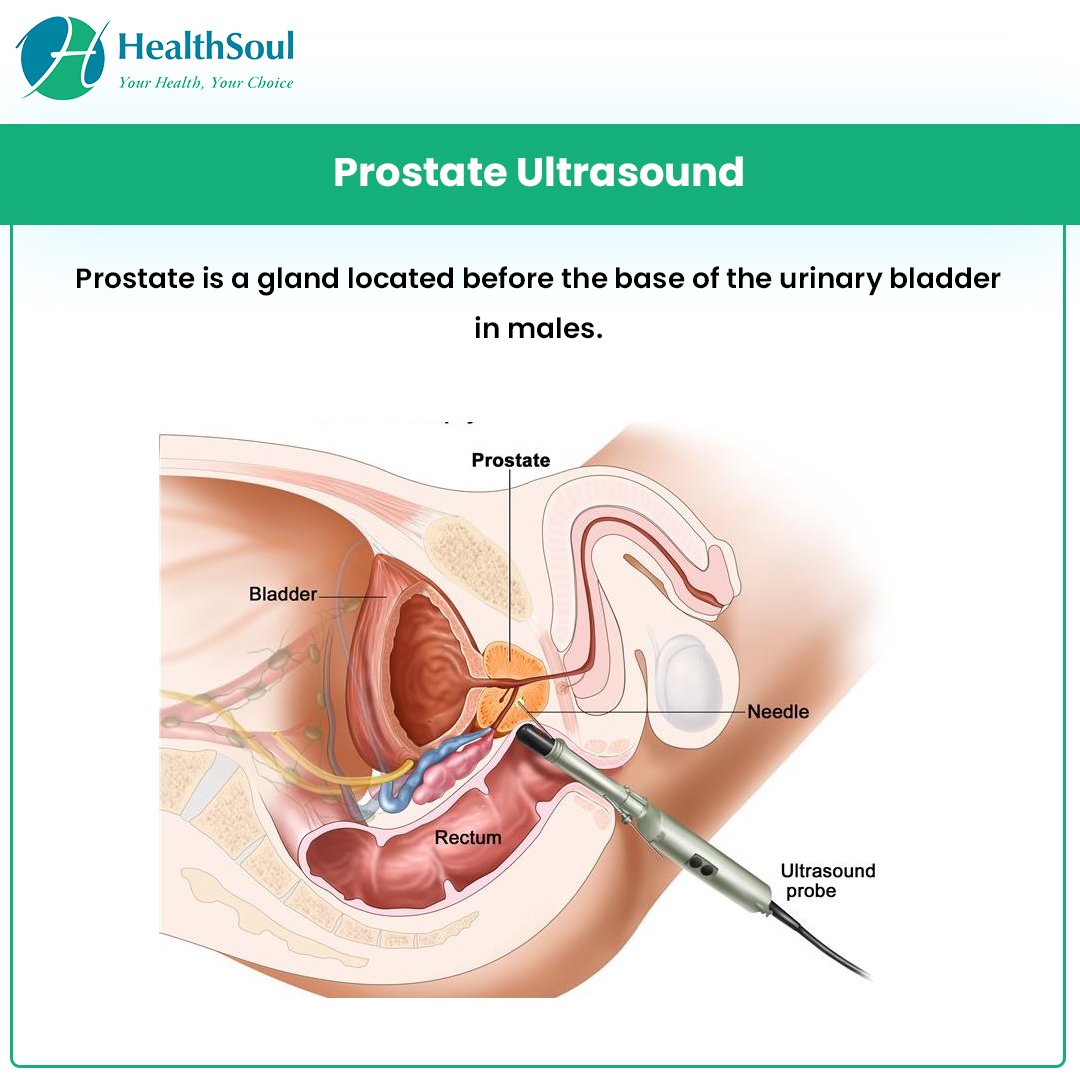
‘Your surgeon will use ultrasound to locate your prostate tumour and then insert up to four needles around it.
‘Then the NanoKnife machine passes an electric current through the needles, damaging the cell membranes of the cancerous cells which then shrink and die.’
Nanoknife is carried out under general anaesthetic and takes around 45 minutes. The procedure is performed as a day case.
Surgeons at University College London Hospital have already used it to treat prostate cancer patients.
And medics have called for bigger trials of the procedure, with it already used for liver and pancreatic cancers.
The process called irreversible electroporation involves sending electrical pulses into tumours which cut open the membrane of the cells.
This targeted style of treatment increases the level of precision while reducing risks to surrounding organs.
It can take less than an hour and patients don’t need to stay in overnight, freeing up valuable time and space in hospitals.
Prostate cancer will affect one in six men across their lifetime as more than 50,000 cases are found every year.
Diagnoses of the disease fell by almost a quarter during the pandemic.
‘It’s an amazing treatment, so quick, and it means we can reach tumours that are beyond where the knife can reach.’
How Prostate Cancer Recurrence Is Detected
Following surgery for prostate cancer removal, the majority of patients will have regular appointments to check in and assess recovery progress with their healthcare provider or preferred oncologist. At each of these visits, your doctor will draw blood to run tests on various levels of biomarkers, hormones, and immunological markers, including PSA. You may also undergo minor physical assessments as part of your post-prostatectomy preventive maintenance care plan.
If prostate specific antigen levels are found to be rising, staying the same as pre-operative quantities, or slowing their rate of decrease in an unexpected way, your provider may suggest imaging tests or an X-ray of the prostate and pelvic area. A few other alternative options for detecting prostate cancer recurrence are available, although some are in the early stages of development or are not yet widely available, so should not be used as a default or go-to option for determining whether metastatic resurgence is a clear and present health risk.
Are you a practicing healthcare provider or oncologist who would like to learn more about alternative options for localized detection of recurrent prostate cancer?
Check out the full infographic here.
Read Also: Doctors Best Comprehensive Prostate Formula
A Primer On Prostate Cancer
Even though prostate cancer is one of the most diagnosed cancers in America, on average men have only a three percent risk of actually dying from the disease. Prostate cancer occurs in the prostate gland, the gland that produces the fluid that makes up semen. Tumors are often slow-growing and highly treatable. However, patients sometimes experience no symptoms until the cancer has spread. Thus, early detection by your doctor is important. Treatments for prostate cancer include: chemotherapy, surgery and radiation.
Its important for you to get your prostate checked. The American Urological Association recommends you discuss the benefits and limitations of these tests with your doctor:
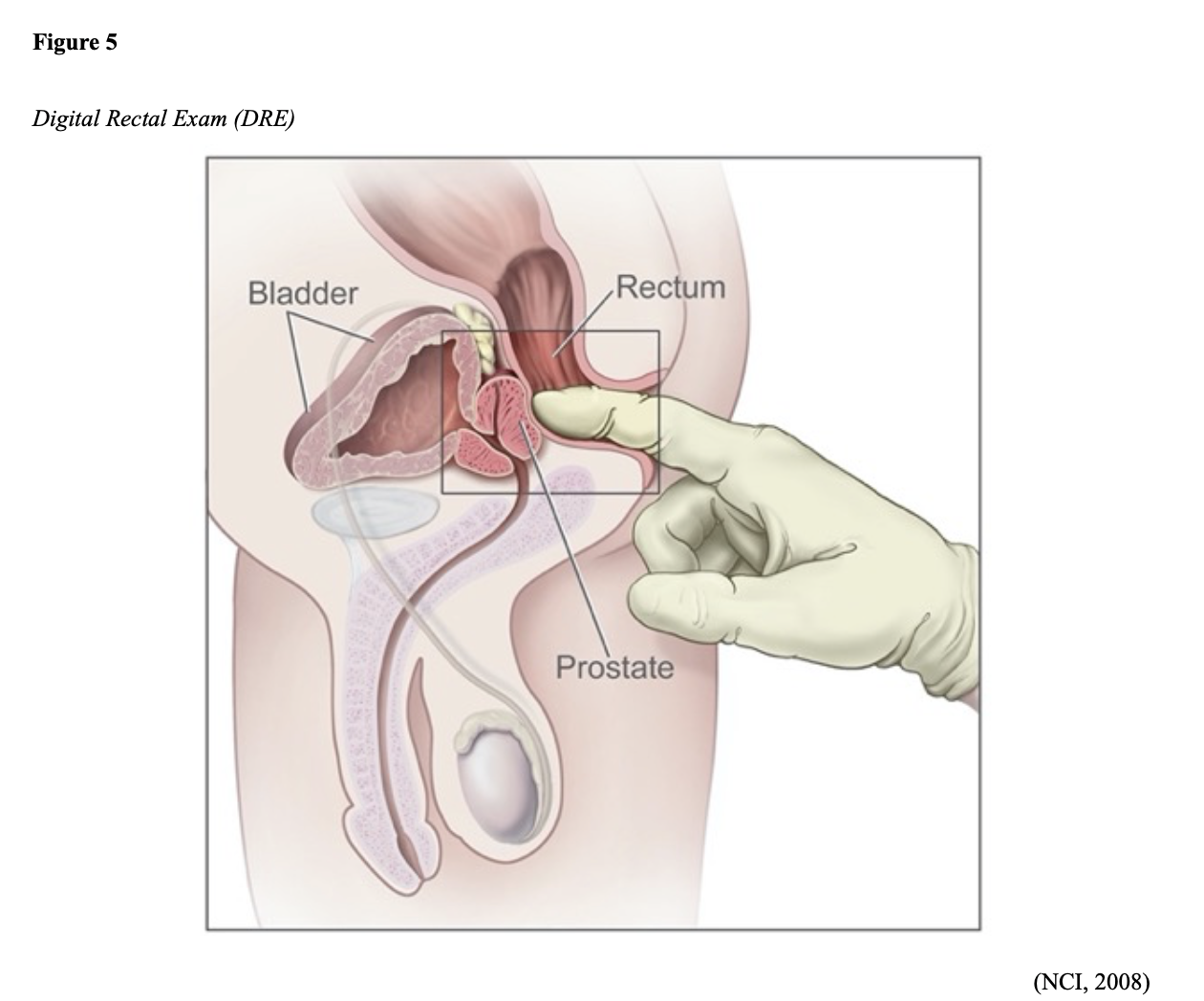
A digital rectal exam once a year after age 40, or earlier if you are having symptoms. Although some men consider this test embarrassing, it is a quick, simple procedure that could save your life.A PSA blood test once a year for men over 50 or earlier for men in high risk groups, such as African-Americans or those with a family history of prostate problems.
If you have a positive DRE or PSA, your doctor may order a biopsy to determine if cancer is involved.
Can I Lower The Risk Of Prostate Cancer Progressing Or Coming Back
If you have prostate cancer, you probably want to know if there are things you can do that might lower your risk of the cancer growing or coming back, such as exercising, eating a certain type of diet, or taking nutritional supplements. While there are some things you can do that might be helpful, more research is needed to know for sure.
Read Also: Best Foods To Eat When You Have Prostate Cancer
Cancer Treatments And Erectile Dysfunction
Following surgery, many men experience erectile dysfunction , but for many, the disruption is temporary. Nerves damaged during surgery may result in erectile dysfunction. A nerve-sparing prostatectomy may reduce the chances of nerve damage. Another factor is the surgeons skill level for performing the nerve-sparing technique, which if done correctly, may improve patients likelihood of retaining erectile function, says Dr. Shelfo.
Prostate cancer may also be treated with various types of radiation therapybrachytherapy, external beam radiation or stereotactic body radiation therapy. Each type of therapy causes somewhat different side effects. About half of all prostate cancer patients who undergo any of these types of radiation therapy are likely to develop erectile dysfunction, according to a 2016 article published in Advances in Radiation Oncology.
When you compare surgery with radiation, both may affect erections, says Dr. Shelfo. Surgery is usually more immediate, and sexual dysfunction has the potential with time to improve. With radiation, erections are usually less affected in the beginning, but over timemonths or, sometimes, yearssexual dysfunction may develop. Both treatments may affect sexual function, resulting in no ejaculate or the ability to attain erections.
Risks Of The Procedure
As with any surgical procedure, certain complications can occur. Somepossible complications of both the retropubic and perineal approaches to RPmay include:
Some risks associated with surgery and anesthesia in general include:
-
Reactions to medications, such as anesthesia
-
Difficulty with breathing
-
Bleeding
-
Infection
One risk associated with the retropubic approach is the potential forrectal injury, causing fecal incontinence or urgency.
There may be other risks depending on your specific medical condition. Besure to discuss any concerns with your doctor prior to the procedure.
Recommended Reading: Pictures Of Prostate Cancer Stages
Transurethral Resection Of The Prostate
This operation is more often used to treat men with non-cancerous enlargement of the prostate called benign prostatic hyperplasia . But it is also sometimes used in men with advanced prostate cancer to help relieve symptoms, such as trouble urinating.
During this operation, the surgeon removes the inner part of the prostate gland that surrounds the urethra . The skin is not cut with this surgery. An instrument called a resectoscope is passed through the tip of the penis into the urethra to the level of the prostate. Once it is in place, either electricity is passed through a wire to heat it or a laser is used to cut or vaporize the tissue. Spinal anesthesia or general anesthesia is used.
The operation usually takes about an hour. After surgery, a catheter is inserted through the penis and into the bladder. It remains in place for about a day to help urine drain while the prostate heals. You can usually leave the hospital after 1 to 2 days and return to normal activities in 1 to 2 weeks.
You will probably have some blood in your urine after surgery.
Other possible side effects from TURP include infection and any risks that come with the type of anesthesia used.
Dr Thompsons Perspective On Testosterone Replacement
What concerns do you have about prescribing testosterone to men who have been successfully treated for prostate cancer?
Obviously, testosterone supplementation has salutary effects for someone who is hypogonadal and suffering from osteoporosis, muscle loss, erectile dysfunction, and other problems. Unquestionably, otherwise healthy men given the choice of being on testosterone or being off testosterone would rather be on it. So, why not prescribe testosterone supplements to men who are hypogonadal and have been treated for prostate cancer?
Well, imagine two men with prostate cancer. The first man had a 12-core biopsy that showed cancer in just a small percentage of one core, cancer that was graded a Gleason 3 + 3. Hes had several prior biopsies, all of which have been negative, and his PSA is 2.5 ng/ml, which is within the normal range. The second mans biopsy shows cancer in every core on the right side of his prostate, graded a Gleason 5 + 4. The cancer can be felt during a digital rectal exam but is confined to the prostate capsule. Both men have undergone treatment.
How does that happen? Testosterone could reactivate existing disease. Or, if the patient had external beam radiation, not all of the tissue becomes fibrotic. Some normal epithelium, the cell layer that lines the prostate, will persist, and that normal epithelium is at risk of becoming cancerous.
Do you have patients who are on testosterone therapy?
So whats your biggest concern?
Recommended Reading: How Do You Know If Prostate Cancer Has Spread
What Factors Increase The Chance Of Cancer Recurrence
The likelihood of metastasis occurring increases with higher grade and stage of the cancer as the more aggressive and developed the cancer is, the higher the chance of it breaking out of the prostate. More specifically:
- High Gleason grades
- High clinical stages
- Positive surgical margins .
However, most prostate cancers are cured with surgery. As an example, using my results from operations performed on over 2,300 men with a variety of stages and grades, 96.3% of operations resulted in full cancer cure. Some combinations of minor prostate cancer had a 100% cancer cure rate, but the higher you go, the lower the full cancer cure rate.
The commonest sites of recurrence of prostate cancer following surgery are:
- the prostate bed 80% of recurrence cases
- lymph nodes 15% of cases
- bones 5% of cases.
Surgically Removing The Prostate Gland
A radical prostatectomy is the surgical removal of your prostate gland. This treatment is an option for curing prostate cancer that has not spread beyond the prostate or has not spread very far.
Like any operation, this surgery carries some risks.
A recent trial showed possible long-term side effects of radical prostatectomy may include an inability to get an erection and urinary incontinence.
Before having any treatment, 67% of men said they could get erections firm enough for intercourse.
When the men who had a radical prostatectomy were asked again after 6 months, this had decreased to 12%. When asked again after 6 years, it had slightly improved to 17%.
For urinary incontinence, 1% of men said they used absorbent pads before having any treatment.
When the men who had a radical prostatectomy were asked again after 6 months, this had increased to 46%. After 6 years, this had improved to 17%.
Out of the men who were actively monitored instead, 4% were using absorbent pads at 6 months and 8% after 6 years.
In extremely rare cases, problems arising after surgery can be fatal.
Its possible that prostate cancer can come back again after treatment. Your doctor should be able to explain the risk of your cancer coming back after treatment, based on things like your PSA level and the stage of your cancer.
After a radical prostatectomy, youll no longer ejaculate during sex. This means you will not be able to have a child through sexual intercourse.
Also Check: What Is C61 Malignant Neoplasm Of Prostate
Understanding The Recurrent Prostate Cancer
Recurrent prostate cancer is when prostate cancer returns after the initial treatment or partial to complete remission has occurred. This is due to the reemergence of surviving prostate cancer cells that have grown large enough to be detected.
Following a prostatectomy, your prostate-specific antigen levels being to decrease. Eventually, they are no longer detectible, which is an indication that prostate cancer is no longer present. However, there is no clear reference for a normal PSA. It differs between men and can be affected by a number of factors. Following your initial prostate cancer treatment, PSA levels should stabilize and be low enough to where theyre not detected on blood tests. In some cases, PSA levels begin to rise again, indicating a need for further tests.
Even if youve had a prostatectomy, prostate cancer can recur in the immediately surrounding tissue, lymph nodes, seminal vesicles, muscles that control urination, the rectum, the wall of the pelvic, or metastasize into lymph nodes and bones further away.
Will Treatment Cause Erectile Dysfunction
When youre sexually excited, nerves cause tissues in your penis to relax, allowing blood to flow into the organ. The nerves that control erection are very delicate. Surgery or radiation for prostate cancer may damage them enough to cause ED. When you have ED, you cant get or keep an erection.
Radical prostatectomy is a surgery to remove the prostate gland. When your surgeon removes the gland, they may damage the nerves and blood vessels that run along it. If theyre damaged enough, you wont be able to get an erection following the procedure.
Today, doctors can do nerve-sparing surgery, which helps prevent permanent ED. Your surgeon can still touch those nerves and blood vessels, causing ED as a temporary side effect. Many men have trouble getting an erection for a few weeks, months, or even years after their procedure.
Radiation therapy also damages blood vessels and the nerves that control erection. Up to half of men who have radiation for prostate cancer experience ED afterward. In some men, this symptom will improve with time. Sometimes radiation side effects dont appear until a few months after the treatment. If ED starts late, it may not be as likely to go away.
A few treatments can help with ED until youre able to have erections on your own again.
Additional treatments include the following:
Dont Miss: Does An Enlarged Prostate Affect A Man Sexually
Don’t Miss: Signs Prostate Cancer Has Spread
Your Emotions And Sex
Your prostate cancer and its treatment wonât just affect your body. Theyâll also have a serious impact on your emotions. Stress and anxiety can trigger your body to make adrenaline, which gets in the way of having sex. The more you worry, the worse the struggle. If youâre in a relationship, your partner will be going through many of the same feelings.
One of the most important things you can do is to talk to your partner. Have an honest conversation about your fears and expectations when it comes to sex. Dont assume they know how you feel. Being open with each other will help you both feel supported and help you work together to make any adjustments that you may need to stay intimate.
Talking with a mental health professional either one-on-one or with your partner can be a powerful way to help manage your emotions. A therapist can also prescribe medications that may ease stress and anxiety. A professional sex therapist can help you and your partner find ways to improve your sex life. It may also be helpful to join a support group where you can talk with others who share your experience.
Prostate Cancer Foundation: Erectile Dysfunction.
UCLA Urology: Prostate Cancer: Dealing with Erectile Dysfunction.
Albaugh, J. Reclaiming Sex & Intimacy After Prostate Cancer: A Guide for Men and Their Partners. Anthony J. Jannetti, Inc., 2012.
Harvard Prostate Knowledge: Achieving orgasm after radical prostatectomy.