Stages Of Prostate Cancer
Most urologists describe the spread and growth of prostate cancer in one of 4 stages. Urologists and treatment providers often use the stage of cancer as a guide when offering prognosis or choosing treatment options. The 4 stages of Prostate cancer are based on a variety of factors, including screening tests such as:
- DRE
- Prostate Biopsies
- Imaging tests from MRI scan, CT scan, bones scan, or transrectal ultrasound
To determine the stage of prostate cancer, most urologists around the world start with the TNM staging system which helps define the different aspects of prostate cancer growth.
- T the T component is used to measure the size & extent of the Tumor
- N the N component is used to measure if and how far the prostate cancer has spread to the Lymph Nodes
- M the M component is used to measure is the prostate cancer has spread to any other organs
After a urologist calculates the TNM components, it will often be combined with the Gleason grading system to determine which stage of prostate cancer the patient is currently in. Prostate cancer survival rates are often based on the actual stage and timing of the diagnosis.
Immunotherapy For Prostate Cancer
Immunotherapy for prostate cancer works by helping a patients own immune system fight back against cancer cells. One immune therapy that has been approved by the FDA is a vaccine called sipuleucel-T , which spurs a patients immune system to attack prostate cancer cells. The vaccine is tailored to match each patients own immune system using the following process:
While sipuleucel-T does not appear to reduce PSA levels or stop prostate cancer growth, it may increase survival in patients with metastatic castration-resistant cancer who show few or no symptoms.
Common side effects of the vaccine include fever, fatigue, chills, back and joint pain, headache and nausea. They are associated with the infusion period and usually only last for a few days.
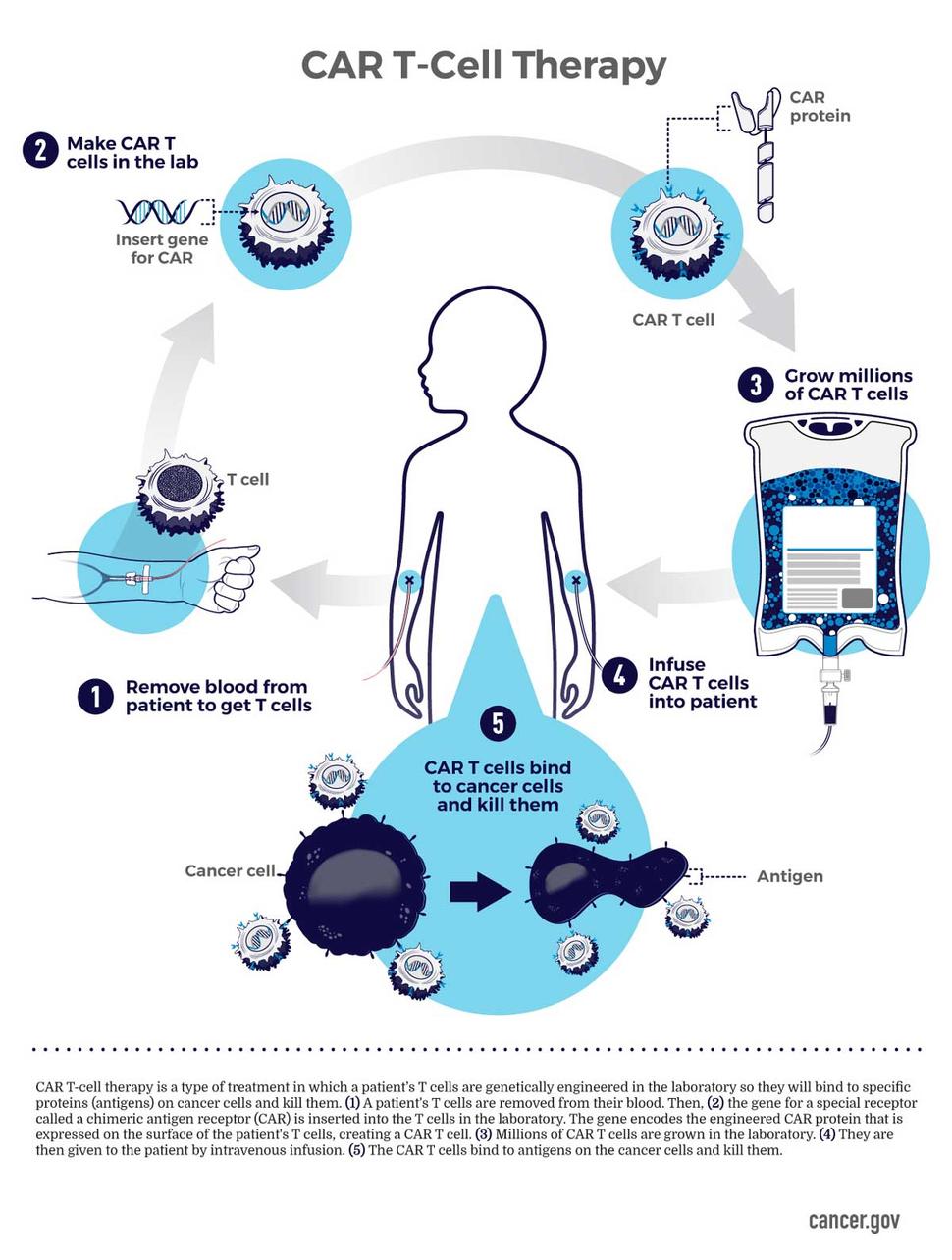
More Than Just Car T Cells: Tils And Tcrs
CAR T cells have garnered the lion’s share of attention when it comes to cellular therapies. But other types of cellular therapies have also shown promise in small clinical trials, including in patients with solid tumors.
One type, known as tumor-infiltrating lymphocytes , uses immune cells that have penetrated the environment in and around the tumor. Researchers at NCI were the first to use TILs to successfully treat patients with advanced cancerinitially in melanoma and later in several other cancers, including cervical cancer. More recently, NCI researchers have developed a technique for identifying TILs that recognize cancer cells with mutations specific to that cancer and identifying people whose cancers are more likely to respond to TIL therapy.
The other type of cellular therapy involves engineering patients’ T cells to express a specific T-cell receptor . Unlike CARs, which use portions of synthetic antibodies that can recognize specific antigens only on the surface of cells, TCRs use naturally occurring receptors that can also recognize antigens that are inside tumor cells.
To date, TCR T cells have been tested in patients with a variety of solid tumors, showing promise in melanoma and sarcoma.
Related Resources
Recommended Reading: Prostate Cancer And Lung Cancer
New Treatment Options Where Few Existed
The initial development of CAR T-cell therapies focused largely on the most common cancer in children, acute lymphoblastic leukemia .
More than 80% of children diagnosed with ALL that arises in B cells, the predominant type of pediatric ALL, will be cured by intensive chemotherapy. But effective treatments have been limited for patients whose cancers return, or relapse, after chemotherapy or a stem-cell transplant.
In 2017, however, a new option appeared, with FDAs approval of tisagenlecleucel , the first CAR T-cell therapy to be approved by the agency, based on clinical trials demonstrating it could eradicate cancer in children with relapsed ALL.
In some cases, CAR T-cell therapy has now been studied long enough that details about the long-term outcomes in children are beginning to emerge.
An NCI-led research team, for example, recently reported on long-term follow-up from children with relapsed ALL who had been treated with CAR T cells as part of a clinical trial. More than half the children went on to receive a potentially curative stem-cell transplant, they found, and approximately 60% of those children were still alive 5 years later without their cancer coming back or the children experiencing any disease-related problems.
The results in lymphoma to date “have been incredibly successful,” Dr. Kochenderfer said, “and CAR T cells become a frequently used therapy for several types of lymphoma.”
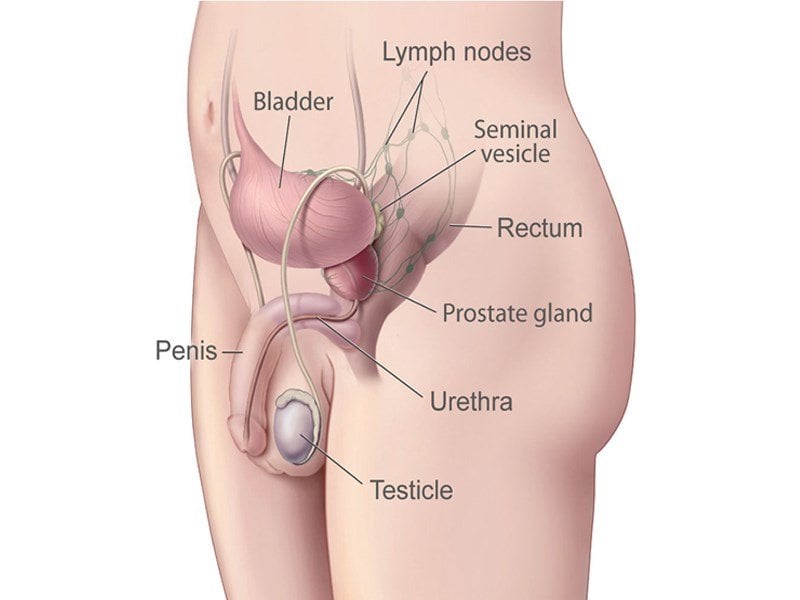
Treatments For Prostate Cancer
If you have prostate cancer, your healthcare team will create a treatment plan just for you. It will be based on your health and specific information about the cancer. When deciding which treatments to offer for prostate cancer, your healthcare team will consider:
- the type and stage of the cancer
- the grade or Gleason score
- prostate-specific antigen levels
- the risk group
- possible side effects of treatments
- your personal preferences
- your overall health and any existing medical conditions
- your age and life expectancy
- whether you have symptoms
Prostate cancer treatments can seriously affect your quality of life and cause side effects such as erectile dysfunction and incontinence . Many prostate cancers grow slowly and cause no symptoms or problems.
You May Like: Alternatives To Surgery For Enlarged Prostate
G Car T Cells Become Exhausted During In Vitro Expansion
During in vitro culture and restimulation, 2G CAR T subset progressively expanded and accumulated up to 6 weeks, the last time point tested. Conversely, 3G CAR T cells strongly reduced their proliferation by week 4 from transduction, with a significant difference in the total CAR T cell yield from day 25 to day 40 . By day 25, furthermore, CD28–4-1BB CAR T cells showed a cell surface profile consistent with exhaustion, including a higher and significant difference in the expression of PD-1 , TIM-3 and LAG-3 , as compared to the 2G CAR T cell population . Moreover, 3G CAR T cells showed higher rates of apoptosis in comparison to the 2G CAR T cell population, likely associated to the induction of the FAS-FASL pathway . In addition, at these late stages of culture 3G CAR T cells produced lower levels of IL-2, TNF-, and IFN- following exposure to PSMA+ cells, as compared with 2G CAR T cells . Together, these phenotypic and functional data demonstrate that 3G CAR T cells become rapidly exhausted and have a limited expansion during in vitro culture, whereas similar effects do not occur in 2G CAR T cells stimulated in the same manner.
T Cell Coinhibition As Immune Evasion Mechanisms In Prostate Cancer
Prostate cancer can escape immune responses via a variety of mechanisms . A prime example is defective antigen presentation. Although tumor cells can theoretically present TAAs with major histocompatibility complex class I molecules, the expression of these MHC molecules and antigen processing machinery are often downregulated, allowing tumors to hide their malignant identity from immune cells. This loss of expression has been noted in some human prostate cancer cell lines and in primary tumor tissues . The immunosuppressive environment surrounding prostate tumors, marked by increased levels of nitric oxide synthase and arginase , the anti-inflammatory cytokines interleukin-10 and transforming growth factor β as well as the infiltration of suppressor cell populations such as FoxP3+ regulatory T cells , also contributes to immune escape.
Recommended Reading: Can Teenagers Get Prostate Cancer
G And 3g Car T Cells Show Comparable Tumor Cell Killing And Cytokine Production Following Exposure To Psma+ Cells
Both the 2G and 3G CAR populations lysed the PSMA-transfected PC3 cells at high levels . Moreover, they efficiently recognized LNCaP cells, a target that naturally harbors the PSMA antigen , while sparing the antigen-negative counterpart . Other than exerting a relevant cytotoxic activity, both generations of CAR-transduced T cells also produced high and comparable levels of IFN-, IL-2, and TNF- in response to PSMA-expressing tumor targets, but not against PSMA negative control cells .
Figure 3 Functional characterization of the 2G and 3G CAR-expressing populations. Lytic activity of the 2G and 3G -CAR expressing populations. Cytotoxicity was analyzed at day 15 post-transduction as target cells, PC3-PSMA, LNCaP, and PC3 were used. Cytokine release upon antigen stimulation. IFN-, IL-2 and TNF-. Cytokine release was evaluated 15 days after T cell infection by stimulating 2G and 3G CAR populations with PC3-PSMA or PC3 cancer cell lines. Negative and positive controls were represented by 2G and 3G CAR T cells treated or not with PMA/Ionomycin. Figures show the mean +/- SD of 3 independent experiments.
Box : Systems For Chimeric Antigen Receptor Gene Transfer Into T Cells
Retroviral and lentiviral vectors: These vectors are currently the most commonly used vectors for transfer of CARs into T cells . It is possible to achieve high and long-lasting CAR expression upon retroviral transduction of proliferating T cells. Although the use of a retroviral vector has induced insertional mutagenesis in hematopoietic stem cells and led to the development of leukemia , such an effect has not been observed in fully differentiated T cells. Lentiviral vectors may be advantageous, since they do not require dividing cells, which could be beneficial in generation of stem-like or young T cells. Although lentiviral gene transfer to quiescent cells is efficient for some cell types, the process is inefficient in inactivated T cells the reason may be lack of low-density-lipoprotein receptors on T cells , which is required for vesicular stomatitis virus glycoprotein -pseudotyped lentivirus cell entry. A measles virus glycoprotein-pseudotyped lentiviral vector has been suggested as an alternative .
You May Like: What Is The Best Prostate Pill
Early Warning Signs Of Prostate Cancer Include:
- Anemia: The patient blood does not have enough hemoglobin due to bone marrow infiltration by the cancerous cells, treatment-related toxic exposure or androgen deprivation
- Severe Abdominal pain: Consistent pressure on organs surrounding the swollen prostate gland causes soreness and pain in the lower abdomen.
- Blood in Semen: Infection or inflammation of the prostate causes blood to appear in the semen
- Hematuria : Cancer in the urinary tract can cause blood to appear in the urine. These symptoms can also appear for patients with kidney failure, kidney cysts or infection in the urinary tract.
- Issues with incontinence or frequent need to urinate: Enlarged prostate glands due to a tumor near the urethra can cause bladder control issues, urine retention issues, incomplete or trouble starting urination and a weak stream of urine.
- Inflammation in Legs: swelling in Legs caused if PC tumors metastasize in the bladder and block urine from the kidneys.
- Frequent Fatigue: This can be caused by traditional chemotherapy or medication based treatments, depression or stress that leads to and lack of appetite.
- Rapid Weight loss: Can be caused by side effects of medical treatments that cause lack of appetite which leads to weight loss.
- Spinal compression or Pain in the Lower Lumbar Spine: Sometimes misdiagnosed as Degenerative Disc Disease, pain in the Lower lumbar or hips can occur when cancer spreads to the bone causing the spinal cord to be compressed leading to pain
Stem Cell Treatment For Prostate Cancer In 2022
To determine eligibility and get exact prices along with day by day treatment outline our oncologists will need to better understand the patients existing needs via recent histological results, Biopsies, blood tests, x-rays or radiology scans from your primary care urologist or oncologist.
If you or a loved one have been diagnosed with prostate cancer, be aware of alternative medical solutions to fight cancer using HSC+ modified immune cells. Take the first step toward treatment by allowing your care to be handled by our team of experts in our advanced facility. We are here to help. To learn more about the safe and effective alternative treatment for Prostate Cancer please contact us today.
Read Also: Prostate Health Foods To Eat And Foods To Avoid
Tumor Immune Escape Due To Heterogeneous Tumor Antigen Expression
To investigate the cytolytic activity of these CAR-Muc1 T cells in a longer co-culture assay we engineered PC3 tumor cells to express GFP and cultured them with either control or transgenic T cells for 3 days. On day 3, residual GFP-positive tumor cells were quantified by flow cytometric analysis. Figure 2a shows that while CAR-Muc1 T cells killed the majority of PC3 cells , decreasing the number of tumor cells from 26.5±1.7E +05 3.2±3.1E +05, CAR-Muc1 T-cell treatment again failed to eliminate all tumor cells . These results were reproduced using a second prostate cancer cell line, DU145. Figure 2c shows that CAR-Muc1 T cells killed the majority of DU145 cells , decreasing the number of tumor cells from 25E + 05 7E +05, again CAR-Muc1 T-cell treatment failed to eliminate all tumor cells.
Increased Risk Of Infection
Some types of CAR T-cell therapy can increase your risk of infection.
In treatment for some leukemias and lymphomas, CAR T-cells are designed to recognise a protein called CD 19. CD 19 is found on the surface of most B cells. B cells are a type of white blood cell and, like T cells, they play an important part in fighting infection.
CAR T-cell therapy that targets the CD 19 protein also destroys the B cells. It kills normal B cells as well as cancerous B cells. This either reduces the number of B cells or destroys them all. This makes it difficult for you to fight infections.
You might need treatment for this side effect. This treatment is called immunoglobulin therapy. It contains antibodies to help you fight infection.
Also Check: High Dose Radiation For Prostate Cancer
Side Effects Of Car T
In general, most patients who receive CAR T-cell therapy do not experience the typical side effects that are associated with chemotherapy, such as nausea, vomiting, and hair loss. However, there are risks of other serious side effects. Because CAR T-cell therapy is given as a one-time infusion , most of the possible complications occur within the first one to two weeks after treatment. They are usually temporary and can be resolved with medication. It is extremely important to communicate with your medical team at Sheba, so our skilled doctors can help to alleviate and manage your side effects.
The most common side effects include:
- Cytokine release syndrome, which involves symptoms that resemble the flu high fever, chills, low blood pressure, muscle or joint pain, shortness of breath, and a fast heart rate. These symptoms can range from mild to severe.
- Neurologic difficulties, such as confusion, tiredness, seizures, agitation, aphasia , encephalopathy , and loss of balance.
- Anemia
- Neutropenia
Who Can Have Car T
CAR T-cell therapy is available for some children with leukaemia and some adults with lymphoma.
This followed decisions by the National Institute for Health and Care Excellence in England in December 2018 and January 2019. And decisions by the Scottish Medicines Consortium in 2019.
Healthcare in Wales and Northern Ireland generally follow NICE guidelines. The following is a summary:
Also Check: Hormone Therapy For Advanced Prostate Cancer
Transurethral Resection Of The Prostate
In most cases, doctors use this procedure to help people with something called benign prostatic hyperplasia , an enlargement of the prostate that isn’t cancer.
People with prostate cancerhave TURP done to ease symptoms like trouble peeing. Doctors don’t use this surgery to try to cure the cancer.
A surgeon removes the inner portion of your prostate gland that surrounds something called the urethra. That’s the tube where the urine leaves your bladder. Then they’ll pass a tool called a resectoscope past the tip of your penis into the urethra. From there, they’ll either send electricity through a wire to heat the area up or use a laser to vaporize or cut tissue.
Children And Young People
CAR T-cell is recommended for those up to the age of 25 who have a type of leukaemia called B cell ALL. It will be used in one of the following situations:
- newly diagnosed children or young people whose leukaemia hasnt gone away with 2 cycles of treatment
- their disease has come back following a stem cell or bone marrow transplant
- their disease has relapsed twice or more
- children and young people whose leukaemia had gone away with treatment, but its come back, and chemotherapy isnt working now
- their disease has come back once but they cant have a stem cell transplant because either they arent well enough, or they dont have a donor
Read Also: Symptoms Of Severe Prostate Cancer
Collecting The T Cells
First, white blood cells are removed from the patients blood using a procedure called leukapheresis. During this procedure, patients usually lie in bed or sit in a reclining chair. Two IV lines are needed because blood is removed through one line, the white blood cells are separated out, and then the blood is put back into the body through the other line. Sometimes a special type of IV line called a central venous catheter is used, which has both IV lines built in.
The patient will need to stay seated or lying down for 2 to 3 hours during the procedure. Sometimes blood calcium levels can drop during leukapheresis, which can cause numbness and tingling or muscle spasms. This can be treated by replacing the calcium, which may be given by mouth or through an IV.