Side Effects Of Radiation Therapy
Compared to earlier radiation methods, these modern techniques reduce the chance of urinary and bowel problems.
With several treatment options available, your doctor will work with you to develop and oversee a treatment plan that precisely addresses your prostate cancer while minimizing the risk to surrounding tissues.
This is why it is important to choose an experienced radiation oncologist who specializes in the management of prostate cancer. High volume centers where practitioners have significant experience and treat large numbers of patients with prostate cancer may be associated with good outcomes and fewer lasting problems related to treatment. The majority of patients who undergo radiation do not have permanent effects on bowel or urinary function, and patients who develop erectile difficulty after these therapies can often be treated successfully with medications such as sildenafil or tadalafil.
Radical Prostatectomy vs. Radiation: How to Compare the Results
Making a decision about prostate cancer treatment is not easy. When considering radiation therapy or radical prostatectomy, one of your top concerns is seeking reassurance that your cancer will be cured following treatment.
Also Check: Va Asbestos And Prostate Cancer
Obesity And Dietary Habits
High-fat intake, the Western diet, obesity, and sedentary behavior are all associated with a higher incidence of prostate cancer. High calcium intake and a diet high in milk products can increase the risk. After being diagnosed with prostate cancer, calcium can increase the risk of aggressive types. On the other hand, whole milk increases the risk of recurrence of prostate cancer. Obese and overweight men are particularly prone to this increase in recurrence. Another dietary risk factor is vitamin D insufficiency. Meat consumption increases cancer risk, while fish consumption lowers the mortality rate.
You May Like: How Do I Know If I Have An Enlarged Prostate
A Paucity Of Practicality Puts Photons Ahead Of Protons
Joseph K. Salama, MD, and Christopher G. Willett, MD
The authors are affiliated with the Department of Radiation Oncology at Duke University in Durham,North Carolina. Dr Salama is an associate professor and Dr Willett is the chairman and a professor.
Since Wilhelm Röntgens discovery of the x-ray in 1895 and its application to the treatment of cancer, advances in technology have led to consistently improved cancer outcomes. Isocentric treatments, computer controlled radiotherapy, megavoltage energy therapy, intensity modulation, volumetric therapy, and image guidance all have significantly advanced the therapeutic index of treatments by improving the chance for appropriate delivery of radiotherapy, while minimizing the exposure of surrounding uninvolved organs.1
Recently, many have advocated proton beam therapy as the next technologic leap forwardone that will further enhance the therapeutic index. Not surprisingly, this enthusiasm has paralleled the establishment of a large number of proton beam therapy centers and a doubling of the number of Medicare beneficiaries receiving proton beam therapy.2 Despite its many theoretical advantages, however, the data do not support a switch to proton therapy at this time.
Potential Advantages of Protons
Planning and Delivery of Radiation
Significant Advances in Photon Therapy
Proton Therapy for Children?
Dosimetric Benefit vs Clinical Benefit
The Issue of Cost
References
You May Like: How Do You Massage Your Prostate
Main Outcomes And Measures
The primary end point was 90-day adverse events associated with unplanned hospitalizations . Secondary end points included Eastern Cooperative Oncology Group performance status decline during treatment, 90-day adverse events of at least CTCAEv4 grade 2 that limit instrumental activities of daily living, and disease-free and overall survival. Data on adverse events and survival were gathered prospectively. Modified Poisson regression models with inverse propensity score weighting were used to model adverse event outcomes, and Cox proportional hazards regression models with weighting were used for survival outcomes. Propensity scores were estimated using an ensemble machine-learning approach.
Dose Escalation Improves Cancer Control
There is currently ample evidence from five randomized controlled trials demonstrating that dose escalation can improve prostate cancerspecific outcomes, particularly for those with intermediate-risk disease based on prostate-specific antigen level, clinical T category, and biopsy Gleason score. The earliest evidence comes from the M.D. Anderson Cancer Center, where 301 patients with T1-T3 disease were randomized to 78 vs 70 Gy . After a median follow-up of 8.7 years, the investigators found that the higher dose improved freedom from biochemical or clinical failure , with the greatest benefit seen in those with an initial PSA greater than 10 ng/mL .
Similarly, a Dutch trial by Peeters et al randomized 669 patients with T1b to T4 prostate cancer to 78 vs 68 Gy and detected an improvement in freedom from failure at 5 years . On subgroup analysis, however, the investigators found that the benefit was limited to patients with intermediate-risk disease.
A study from Ontario randomized 104 patients with intermediate- and high-risk disease to 75 Gy in 6.5 weeks delivered by external-beam radiation therapy plus implant vs 66 Gy in 6.5 weeks by EBRT alone and found that dose escalation reduced biochemical failure .
Finally, Dearnaley et al have published their randomized trial from the British Medical Research Council showing that among men who all received short-course hormonal therapy, treatment with 74 vs 64 Gy resulted in improvements in 5-year outcomes for all patients.
Read Also: Focused Ultrasound Prostate Cancer Treatment
Who Is A Good Candidate
In most cases, you will be a good candidate for proton therapy if you were initially offered radiotherapy as an option. Patients who receive radiotherapy usually have no problems being a candidate for proton treatment. They are usually patients in an early stage or those with localized prostate cancer. It is also useful to keep advanced cancer under control for as long as possible and treat recurrent prostate cancer cases.
However, some patients may not benefit from proton therapy if they have one of these problems :
- In patients with hip replacements, because proton beams often cant reach beyond the prosthesis. In some proton therapy centers, these patients can still get a session when a hip replacement is limited to one side. But bilateral replacement makes it impossible to treat the patient with proton beam therapy.
- In patients with advanced prostate cancer in which treating the pelvic lymph nodes is fundamental. Since proton beam radiation is less likely to reach other tissues than the prostate, it is not applicable when treating surrounding lymph nodes.
- In overweight patients, because the proton beam can only go through a determined depth. This depth depends on the beams energy, and some centers may have a higher energy device that solves the problem.
Proton Therapy Treatment For Prostate Cancer Patients
Proton therapy is a form of radiation treatment for cancer patients. Also called proton beam therapy, proton therapy involves focusing proton particles into a beam, which is then delivered to the cancer cells in a non-surgical procedure. The positively charged particles can be controlled to stop at the tumor site, enabling the cancerous tissues to be destroyed with high levels of radiation without causing damage to nearby healthy tissue and vital organs. Proton therapy is considered more precise than other types of radiation therapy. It is also non-surgical, non-invasive, and has minimal side effects. Proton therapy treatment requires little to no recovery time, and the radiation has very little impact on a patients energy level compared to other cancer treatment options.
Proton therapy exhibits higher success rates in prostate cancer patients.
According to a study published by the University of Florida, prostate cancer patients who received proton therapy treatment were found to be free of cancer progression for five years after their treatment. Patients with low to medium risk prostate cancer experienced a success rate of 99%, while those with high risk prostate cancer experienced a success rate of 76%.
You May Like: Chinese Medicine For Prostate Cancer
You May Like: Where Is The Prostate Cancer
Whats The Procedure Like
Since delivering the protons to the cancer cells is the goal of therapy, a lot of time is spent on positioning your body and adjusting the equipment before each session.
Youll have to remain perfectly still while the proton beam is delivered, but it will only take about 1 to 3 minutes. Its noninvasive, and you wont feel anything. Youll be able to leave right away and continue your normal activities.
Potential Disadvantages Of Proton Therapy
Depending on techniques compared, there may be disadvantages in dose distribution with proton therapy compared with IMRT. For example, Trofimov et al found that IMRT provided better conformality of the high-dose volume to the target than double-scattered proton therapy did. The average conformality index was 2.73 with IMRT and 3.11 with the double-scattered proton therapy plans . Similarly, in a comparison of IMRT to double-scattered proton therapy, Underwood et al found that IMRT provided better high-dose conformality than proton therapy did when evaluating prescription isodose lines. In addition, IMRT provided lower volumes of both rectum- and bladder-receiving doses in the range of V50 to V70 compared with double-scattered proton therapy. This shortfall of double-scattered proton therapy can be eliminated by using IMPT, which is a more refined delivery method of proton particles using PBS. Trofimov et al found that IMPT provided a better conformality index than IMRT did when delivering high-dose radiation therapy to the prostate.
Read Also: Is Asparagus Good For Prostate Cancer
Entrance And Exit Dose Defined
Entrance dose: The dose of radiation that inadvertently makes contact with normal cells before it reaches the cancerous tissue.
Exit dose: Imagine the radiation hitting the tumor, but then continuing on beyond it, taking out normal cells in its path.
The primary difference between proton therapy and Cyberknife is that protons do not have an exit dose, says Dr. Cavanaugh. Both modalities deliver entrance and target dose.
Many insurers have been unimpressed with the differences in outcomes with proton therapy and have declined to pay.
For many patients I prefer HDR brachytherapy to both proton and Cyberknife therapy. HDR stands for high dose rate.
Dont Miss: How Long Does It Take For Prostate Cancer To Spread
Whos A Good Candidate For This Procedure
Anyone who can have radiation therapy can have proton therapy. Proton therapy can be used as primary treatment for early stage prostate cancer or as part of a total treatment plan for prostate cancer. Its also an effective treatment for people who require pelvic radiation therapy after undergoing previous therapies.
Also Check: How Do Doctors Check Prostate Cancer
Trial To Compare Radiation Therapies For Treating Prostate Cancer
MUSC Hollings Cancer Center is enrolling patients in a national clinical trial to help to determine the best, most cost-effective approach for treating prostate cancer through radiation therapy.
The trial, known as the COMPPARE study, will compare the quality of life, side effects and cure rates for prostate cancer patients who are treated with one of two radiation types: photon therapy or proton therapy.
The main difference between the two radiation types is that X-ray beams travel all the way through a patient while protons only travel a certain distance before stopping, allowing them to deliver more concentrated doses of radiation.
Both therapies are currently considered standard of care for treating prostate cancer, and the type of treatment patients receive depends on the facility where theyre receiving treatment, their insurance coverage and their personal preference. Hollings treats patients using photon therapy, which is roughly three times less expensive than proton therapy and has shown to be just as effective as treatment with protons.
The reason we like this trial at Hollings is because it doesnt change our patients course of treatment. They can still choose how they get treated, and theyre able to help future patients determine the best, most cost-effective way to get treated. Dr. David Marshall
How Are They Used
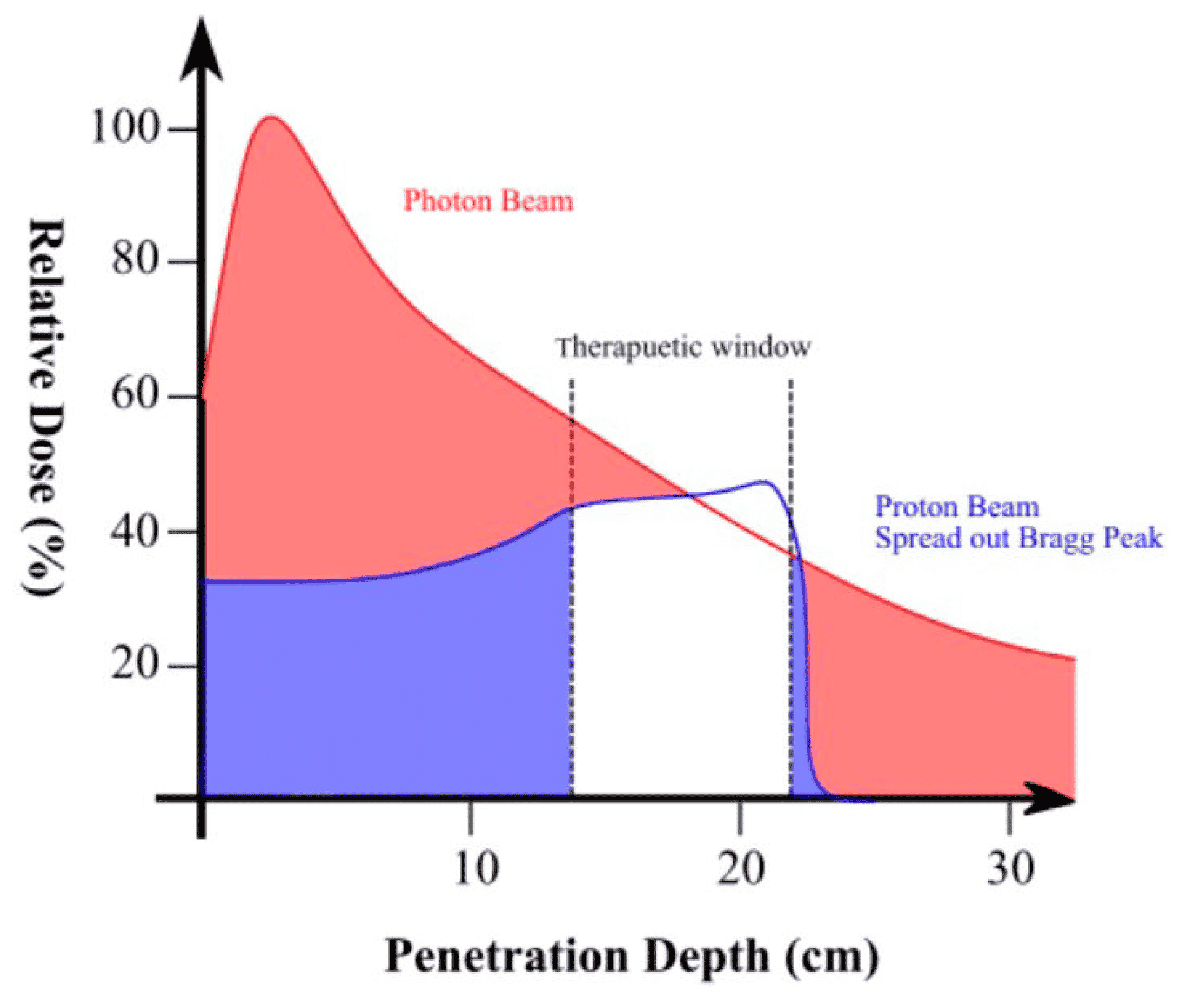
With photon radiation, we can minimize, but are not always able to eliminate, the radiation dose that a neighboring organ receives, says Hani Halabi, MD, Radiation Oncologist at Cancer Treatment Centers of America® , Atlanta.
Advanced technology allows radiation oncologists to better match the size and shape of the tumor and to follow a tumor as it moves while a patient is breathing. But radiation may still affect parts of the body other than the area being treated.
We can modify the beams, change the angles and modify the intensity of the radiation to make the normal organ get less radiation, and keep the radiation exposure to the organ within acceptable and tolerable levels, Dr. Halabi says. But it will not be zero.
Protons have physical mass and can be stopped at a certain depth inside tissue. Without the exit dose, protons improve the sparing of surrounding organs and normal tissues. This offers several potential advantages over photon therapy, including:
- It may result in fewer side effects because less healthy tissue is irritated by the radiation.
- Because of the enhanced ability to spare surrounding organs, proton therapy may allow for higher doses of radiation to be delivered to the cancer compared to photons.
With proton therapy, we can stop the radiation at a certain depth in the body, Dr. Halabi says. This can significantly improve our ability to spare the neighboring organs from receiving radiation.
Recommended Reading: How Long Can One Live With Prostate Cancer
Controversies In The Use Of Protons For Prostate Cancer
Second Malignancy Risk
Because IMRT exposes a greater amount of normal tissue to low-dose radiation than conventional 3D conformal photon therapy, it is believed to be associated with a higher risk of secondary malignancies than conventional photon therapy. For example, Hall et al have estimated based on data from atomic bomb survivors that patients who receive IMRT for prostate cancer would have a secondary malignancy risk of 1.75% at 10 years compared with 1% at 10 years for those who receive conventional photon therapy.
Since protons appear to expose less normal tissue to radiation than IMRT, they might be expected to confer a lower risk of secondary malignancies than IMRT. Miralbell et al assessed the potential influence of improved dose distribution with proton beams compared to photon beams on the incidence of treatment-induced secondary cancers in pediatric oncology. Two children, one with a parameningeal rhabdomyosarcoma and a second with a medulloblastoma, were considered. The investigators found that proton beams have the potential to reduce the incidence of radiation-induced secondary cancers for the rhabdomyosarcoma patient by a factor of > 2 and for the medulloblastoma case by a factor of 8 to 15, compared with either IMRT or conventional x-rays.
Are Protons Cost-Effective?
Which Treatments Are Best In Keeping Men In Remission
Here is your opportunity to compare prostate cancer treatments. Over 129,000 patients underwent PSA monitoring after treatment to see which treatments were most effective at keeping the cancer in remission. The charts show which treatments are more likely to leave patients Prostate Cancer Free, for how many years. Share this data, talk with your Doctor, or multiple Doctors and make an informed decision. Select the treatment option, that is best for you.
Compare Prostate Cancer Treatments by gathering information about your own Prostate Cancer Diagnosis. Your Doctor will provide three elements that describe your prostate cancer. Your PSA, Stage and Gleason Score. These three elements help you determine your risk group. Find and select your Risk Group in the table below. This will take you to the comparing prostate cancer treatments page, where you can select different prostate cancer treatments on an interactive chart and graphically see their effectiveness over time.
The treatments included in this study are Prostate Surgery or Prostatectomy, , Brachytherapy or Seeds, High Dose Rate Radiation, HDR, External Beam Radiation Therapy or EBRT, Androgen Deprivation Therapy, ADT, or Hormone Treatment, Proton Therapy, High-Intensity Focused Ultrasound, HIFU, Cryotherapy, Cryo and Hypo-Fractionated External Beam Radiation Therapy. For more advanced prostate cancer, treatments are combined to increase effectiveness.
Read Also: How Far Up Is The Prostate
Hinged Aluminum Screen Doors
This therapy, also known as radiotherapy, is a cancer treatment procedure that uses high doses of radiation to kill cancerous cells and shrink the tumor as well. At low doses, this procedure is used as an x-ray. This therapy can be internal or external or both form. For externalbeam, a machine that is outside your body aims at the cancerous cells. This is an observational study and the aim is to evaluate the effect of dietary supplements based on Resveratrol, Lycopene, Vitamin C and Anthocyanins in reducing skin toxicity due to external beam radiotherapy in patients affected by breast cancer. 71 patients were enrolled and they were divided in two different groups: a control group of 41 patients.
CLINICAL TREATMENT PLANNING IN EXTERNAL PHOTON BEAM RADIOTHERAPY W. PARKER, H. PATROCINIO Department of Medical Physics, McGill University Health Centre, Montreal, Quebec, Canada 7.1. INTRODUCTION External photon beam radiotherapy is usually carried out with more than one radiationbeam in order to achieve a uniform dose distribution inside the. RadiationTherapy Market – Scope of Report. TMR’s report on the global radiationtherapy market studies the past as well as the current growth trends and opportunities to gain valuable insights of the indicators of the market during the forecast period from 2022 to 2031. The report provides revenue of the global radiationtherapy market for the period 2017-2031, considering 2021 as the base.
3d stl files star wars legion
Proton Therapy For Recurrent Prostate Cancer
For those with a recurrence of prostate cancer, additional radiation therapy with photons can increase the risk of side effects and isnt generally recommendation. In these cases, proton therapy can provide an optimal dose of radiation to your tumor while protecting the healthy tissue surrounding the prostate. This puts radiation back on the table as a treatment option for recurrent prostate cancer.
Don’t Miss: What Pain Is Associated With Prostate Cancer
How Does Proton Therapy Compare With Imrt For Prostate Cancer Treatment Outcomes
UF Health Proton Therapy Institute published in the May 2016 issue of the International Journal of Radiation Oncology Biology Physics a study that reports 5-year outcomes of more than 1,300 prostate cancer patients treated at the Institute from 2006 to 2010. The study shows that proton therapy is a highly effective treatment for low-risk, intermediate-risk and high-risk prostate cancer. It also reports a low rate of serious side effects.
There are no prospective comparative studies for a definitive comparison of proton therapy with IMRT. The following table from the study provides some guidance on patient outcomes following prostate cancer treatment with either proton therapy or IMRT.
We at the University of Florida Health Proton Therapy Institute are fully committed to gaining a better understanding of the impact of utilizing protons to treat prostate cancer. Our published data is based on treatments delivered with well-defined dose levels and toxicity documented by detailed follow-up questions and examinations of our patients. Actual results, reported by patients and their physicians, are utilized in our research studies.
We strongly encourage all prostate patients to become better educated about their disease and the different options for treatment. We likewise encourage patients to take the time and effort to question the data from all sources.
Citations:
Cancer Specialist