The Advantages Of Prostate Mri
MRI allows doctors to better visualize the entire prostate gland. This can help to rule out the need for a biopsy, or if one is needed, it can ensure that biopsies are taken from the most suspicious areasand not just randomly.
At Imaging Healthcare Specialists, our advanced MRI systems provide exceptionally detailed images of soft tissue within the body, such as those of the prostate gland. Combined with our expertise in interpreting prostate MRI exams, this test can help detect or rule out suspected cancer, determine cancer stage, conclude whether the cancer is contained, and help you and your doctor determine an appropriate course of treatment. We can also detect other, non-cancerous diseases of the prostate, such as prostatitis or BPH .
Prostate MRI is safe, accurate and painless, and has been shown to identify cancer in more than 50% of men whose initial biopsy was negative.
Diagnosis Of Prostate Cancer
Check out this factsheet for a summary of the video.
Diagnosis is the process of finding out the cause of a health problem. Diagnosing prostate cancer usually begins with a visit to your family doctor. Your doctor will ask you about any symptoms you have and do a physical exam. Based on this information, your doctor may refer you to a specialist called a urologist or order tests to check for prostate cancer or other health problems. A urologist is a doctor who specializes in treating conditions of the genital and urinary tracts, including the prostate.
The process of diagnosis may seem long and frustrating. Itâs normal to worry, but try to remember that other health conditions can cause similar symptoms as prostate cancer. Itâs important for the healthcare team to rule out other reasons for a health problem before making a diagnosis of prostate cancer.
The following tests are usually used to rule out or diagnose prostate cancer. Many of the same tests used to diagnose cancer are used to find out the stage . Your doctor may also order other tests to check your general health and to help plan your treatment.
Read Also: Finding The Prostate Externally
Prostate Mri Can Help Differentiate Between Harmless And Aggressive Cancers Preventing The Overdiagnosis Of Low
There are two forms of prostate cancer: aggressive and harmless. Fortunately, out of all prostate cancer cases, only a fraction will be aggressive and clinically significant. The majority will never impact the well-being or life expectancy of a patient.
Prostate MRI can help reduce the number of men who are over-diagnosed by 5%.
A prostate MRI scan enables radiologists to better differentiate between aggressive and harmless cancers by providing information about a tumors size, density, and proximity to the bloodstream. One study comparing prostate MRI to biopsy found MRI scans to correctly diagnose 93% of tumors, whereas biopsy correctly diagnosed only 48%. Identifying non-threatening forms of prostate cancer helps decrease the risk of overdiagnosis and overtreatment.
But do keep in mind that MRIs can be complex images for radiologists to interpret. Coupling a prostate MRI with a subspecialty second opinion from a fellowship-trained radiologist can help maximize the advantages and efficacy of the screening. This can be done completely online and is especially recommended for scans that indicate the possibility of aggressive prostate cancer.
CONNECT WITH A SPECIALIST
Take Charge of Your Health
Get a second opinion from a radiology specialist in 3 easy steps.
Also Check: Can A Ct Scan Detect Prostate Cancer
Use In Men Already Diagnosed With Prostate Cancer
The PSA test can also be useful if you have already been diagnosed with prostate cancer.
- In men just diagnosed with prostate cancer, the PSA level can be used together with physical exam results and tumor grade to help decide if other tests are needed.
- The PSA level is used to help determine the stage of your cancer. This can affect your treatment options, since some treatments are not likely to be helpful if the cancer has spread to other parts of the body.
- PSA tests are often an important part of determining how well treatment is working, as well as in watching for a possible recurrence of the cancer after treatment .
How A Prostate Mri Improves Diagnostic Accuracy
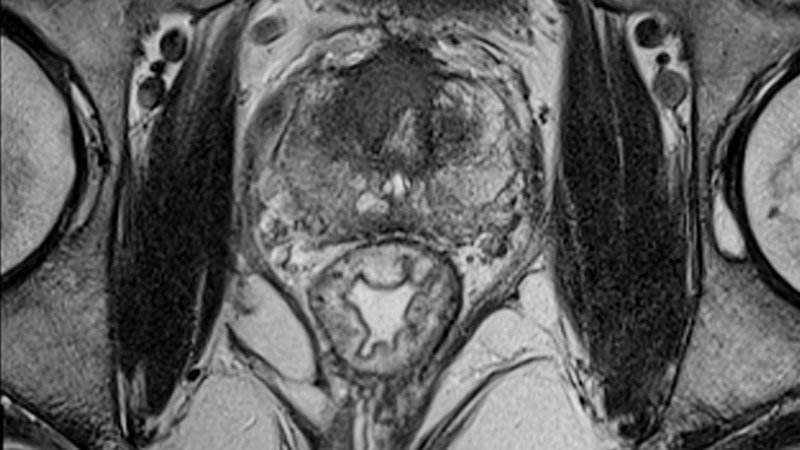
Research indicates MRI scans may be more accurate than other prostate cancer detection methods, especially biopsies.
In one study, tumors were correctly diagnosed in 93% of MRI scans compared to 48% of biopsies. This means a prostate MRI may help avoid unneeded biopsies.
Of the million biopsies performed each year, an estimated 27% are unnecessary.
Avoiding these unnecessary procedures is crucial, as prostate biopsies can cause rectal bleeding, blood in the urine and/or semen, difficulty urinating, and infection. Urinary tract infection is the most common infectious complication of prostate biopsy, occurring in 1 to 11 percent of patients.
Men with elevated PSA levels who want more information about their prostate before undergoing a biopsy can get Ezras Prostate Plus scan, a prostate MRI with contrast. It will indicate with better accuracy where any potential cancer may be prior to undergoing a biopsy.
A study published by JAMA Oncology showed using a prostate MRI could have meant avoiding 38% of biopsies yet still identifying 89% of clinically significant cancers.
As a biopsy involves random tissue samples, it can miss a cancerous region of the prostate. This means MRI results can also help avoid missed diagnoses.
Read Also: What Is The Test For Prostate Cancer
Detection Of Clinically Significant Prostate Cancer
mpMRI is a highly accurate test for the detection of clinically significant prostate cancer. Level one evidence from PROMIS revealed a sensitivity of 93% and negative predictive value of 89%. Comparison of diagnostic performance between studies is hindered by significant heterogeneity in MRI parameters, definition of clinical significance chosen and biopsy route and protocol. Despite this a high sensitivity and negative predictive value are common findings across the summarised reports. Reports of inter reader variation in mpMRI lesion scoring however may impede its timely spread beyond expert centres. Even in such large centre lesser performance has been reported. Johnson and colleagues analysed mpMRI performance in detecting clinically significant prostate cancer using prostatectomy histology as a reference standard and reported a lower sensitivity of 63%, though the post biopsy timing of a majority of their scans likely hindered interpretation.
Table 2Figure 3et al.Figure 4Table 3Figure 5
Mri Does Not Show Every Cancer
MRI of the prostate is best for clinically significant or higher grade cancers which threaten the health and life of the patient. It will at time not show cancers of the prostate however. Those are frequently lower grade cancers but can be higher grade as well. MRI of the prostate does enhance the diagnosis of prostate cancer.
Without the prostate MRI, the urology doctor will blindly biopsy the gland. This will lead to areas which are not sampled. Cancer is therefore more likely to be missed. Prostate MRI will give additional suspicious targets to the urology doctor to biopsy. This will increase the diagnosis of prostate cancer.
Also Check: Life Expectancy Prostate Cancer Gleason 8
Deep Learning And Ai Technology May Help Mri Overcome Human Variability In Identifying Aggressive Prostate Cancer
Prostate cancer manifests as a range of heterogenous cells and tissue in pattern combinations that require experienced genitourinary radiologists trained to identify and classify them on mpMRI studies.1 Distinguishing between low-, intermediate-, and high-risk tumor tissue can be challenging because it is easily impacted by the level of experience of the radiologist on one hand, and the innate variability that exists in human observation and assessment of images on the other.1
Noninvasive mpMRI is an established and important imaging technique that provides high-contrast and high-resolution visualizations of the prostate and pelvic regions essential for detecting and evaluating aggressiveness in prostate tumors.4,5,6 To date, qualitative or semiquantitative assessment criteria used for interpreting mpMRI findings has often produced a range of varying results due to manual input.4,5,6
Determining if a tumor is malignant or benign and classifying its aggressiveness based on imaging exams requires radiologists to have had the opportunity to train by evaluating thousands of mpMRI scans.4,5,6 As a result, interpretation quality can become variable depending on the training of the reader performing the evaluation.4,5,6 One reason for lack of experience is many healthcare facilities do not have the resources to provide the thousands of scans essential for this specialized training.6
Further Testing For Advanced Cancer
If there’s a significant chance the cancer has spread from your prostate to other parts of the body, further tests may be recommended.
These include:
- an MRI scan, CT scan or PET scan these scans build a detailed picture of the inside of your body
- an isotope bone scan, which can tell if the cancer has spread to your bones a small amount of radiation dye is injected into the vein and then collects in parts of the bone where there are any abnormalities
Don’t Miss: What Are The Chances Of Getting Prostate Cancer
Our Ambition For 2020
Since the publication of the PROMIS study in 2017, it has been our ambition to make sure that, by 2020, every man with suspected prostate cancer can get access to a mpMRI scan before a biopsy.
We recognise that mpMRI before biopsy is a complex scanning technique which is why we have worked together with experts and relevant professional bodies to develop resources and guidelines to support healthcare professionals and Hospital Trusts to roll out this technique to a consistent, high-quality standard which delivers the greatest benefit for men.
We also engaged with NICE, the National Institute of Clinical Excellence, to ensure mpMRI before biopsy is recommended in their guidelines as standard practice for suspected prostate cancer diagnosis.
How does mpMRI improve diagnosis?We worked with the MRC Clinical Trials Unit at University College London to produce a series of short films on how mpMRI scans can improve prostate cancer diagnosis.
Imaging And Biopsy Pathways
All men were imaged using a 3T MRI scanner with phased array body coil and spine coil elements for signal detection. The imaging protocol included T2-weighted imaging in three planes, axial diffusion-weighted imaging , and dynamic contrast-enhanced imaging, in accordance with the recommendations from Prostate Imaging Reporting and Data System v2 . Reporting was performed by one of two radiologists with 0.5 and 5 years of experience in reading prostate MRI at the onset of the study. Prior to the study, both radiologists underwent a 2-week training for reading prostate mpMRI, in accordance with PI-RADS, at a high-volume institution. PI-RADS v2 and a standardized reporting template with a maximum of three lesions were used for all reports. Men with negative imaging were referred to a urologist at our outpatient clinic for systematic TRUS. Patients with possible cancer on imaging were randomized to either cognitive targeted TRUS or MRGB. In order to comply with our current clinical practice, the men were referred to a secondary TRUS after MRGB. Randomization and data collection were performed by a web-based randomization and data collection system developed and administered by the Unit of Applied Clinical Research, The Faculty of Medicine and Health Sciences, Norwegian University of Science and Technology.
Read Also: Major Causes Of Prostate Cancer
Prostate Cancer Can Be Hidden Or Normal Gland Can Be Mistaken For Cancer
Prostate MRI is not a perfect test. There are mimics of prostate cancer from normal anatomy. There are also parts of the gland such as the transitional zone which is can be difficult to diagnose cancer. The normal gland in this area of an older man can hide or even mimic cancer. An inflamed gland called prostatitis can sometimes mimic cancer or even hide it.
Prostate MRI may therefore lead to false positive or false negative diagnosis of prostate cancer. Additionally, the biopsy may miss a lesion or result in sampling error of the lesion. The prostate MRI and biopsy may lead to an under-staging of the cancer leading to less aggressive treatment . That is, the grade of the cancer may come back lower then it is.
The experience of the radiology doctor reading the study is also important. The test has many pitfalls and experience certainly helps in a more accurate reading. The quality of the test is also important. Some higher volume centers will have more experience with doing these tests leading to a higher quality of exam.
Prostate MRI improves on the diagnosis of prostate cancer. It is not a perfect test and not every cancer will be diagnosed. Many clinically significant cancers will be diagnosed however. Especially those that threaten health and life. The test will also help target the biopsy to the most suspicious areas.
Multiparametric Mri May Miss Or Underestimate Prostate Cancer Lesions
Multiparametric MRI may not show all prostate cancer lesions or may underestimate their size.
Multiparametric magnetic resonance imaging may miss clinically important lesions in prostate cancer, according to a study published in Radiology.
Researchers from the National Institutes of Health in Bethesda, MD, performed a retrospective single-center study to characterize clinically important prostate cancers missed at MP MR imaging. The study included 100 consecutive patients who had undergone MP MR imaging and subsequent radical prostatectomy. A genitourinary pathologist blinded to MP MR findings outlined prostate cancers on whole-mount pathology slices.
The MP MR images were correlated by two readers who were blinded to histopathology results during prospective reading. Eighty clinically unimportant lesions were excluded from the study. The same two readers then retrospectively reviewed cancers missed at MP MR imaging and assigned a Prostate Imaging Reporting and Data System version 2 score to better understand false-negative lesion characteristics.
The results showed that of the 162 lesions found, 26 were missed and 136 were correctly identified with MP MR imaging. Eight lesions were underestimated for size.
The Gleason scores for the 26 missed lesions were:
3+4 in 17 4+4 in 7 4+5 in 1
Retrospective PI-RADS version 2 scores were:
PI-RADS 1, n = 8
You May Like: What Food Causes Enlarged Prostate
Mri Twice As Likely As Biopsy To Spot Prostate Cancer Research Shows
Finding could bring about change of practice in NHS with potential to save many lives, says charity
Every man with suspected prostate cancer should have an MRI scan, which is twice as likely to identify the presence of dangerous tumours as the invasive biopsy used currently, say doctors.
A major trial, which could influence a change of practice in the NHS, will amount to the biggest leap forward in prostate cancer diagnosis in decades, with the potential to save many lives, Prostate Cancer UK said.
Researchers publishing in the Lancet medical journal have shown that an MRI picks up 93% of aggressive cancers, compared with 48% for a biopsy. The biopsy, which removes a sample of tissue for lab testing, often misses the tumour altogether.
The Prostate MRI Imaging Study , led by researchers at University College London , also showed that more than a quarter of all men with suspected cancer could avoid a biopsy altogether.
MRI scans were shown to be better at ruling out cancer, as well as identifying tumours that are not dangerous because they are slow growing and do not need to be treated. In the trial, the number wrongly diagnosed with a cancer that needed treatment was reduced by 5%.
Some men suffer a life-threatening sepsis a bloodstream infection as a result of the standard transrectal ultrasound-guided biopsy.
What Are The Implications
The higher sensitivity of MP-MRI compared with TRUS-biopsy means that it would miss fewer cases of cancer. Therefore, MP-MRI as a triage test could help guide more targeted biopsies to increase the detection of high risk cancers.
Initial MP-MRI may also prevent unnecessary biopsies and reduce detection of prostate cancers that are at low risk of progression. However, this strategy may miss some cases.
NICE will need to evaluate the cost effectiveness of MP-MRI before it could be recommended as a routine triage step. The technology is already in place in some hospitals, but the costs of widespread introduction and staff training would need to be considered.
Recommended Reading: Surgical Options For Prostate Cancer
Prostate Mri With And Without Contrast
gary37907
Has anyone here had experience with the a Prostate MRI with and without contrast for prostate cancer screening? My internist suggested that I have this rather than biopsy due to possible side effects of needle biopsy. He said that MRI has become pretty accurate in detecting tumors and when it is positive for tumors it can be used as a guide for directing needle biopsy. Mine showed no masses but BPH with medial lobe involvement intruding into the blaldder neck. This all came about because my BPH symptoms got so bad that I was retaining urine in my bladder. MY urologist wanted me to have a biopsy before any BPH surgical procedures because of a history of 3 brothers with prostate cancer. My last PSA was 2.9 but it has gotten up to the low 3âs on several occasions. I donât know what my Uro will do with these results tho I would assume it would mean a go for any procedure I decide to have. Now the hard part is deciding which procedure to get. I am an otherwise healthy 67 year old. I would appreciate some input from those who have knowledge and or experience with the prostate MRI. Thanks Gary
0 likes, 14 replies
Read Also: Fiducial Marker Placement For Prostate Cancer
How Is The Procedure Performed
MRI exams may be done on an outpatient basis.
You will be positioned on the moveable exam table. Straps and bolsters may be used to help you stay still and maintain your position.
Devices that contain coils capable of sending and receiving radio waves may be placed around or next to the area of the body being scanned.
MRI exams generally include multiple runs , some of which may last several minutes.
Your exam may use an endorectal coil. If so, a nurse or doctor will place a disposable cover over the coil. They will lubricate the assembly and insert the coil a short distance into your rectum. After insertion, the doctor inflates the circular balloon that sits around the coil and holds it in place during the exam. When the exam is complete, the doctor deflates the balloon and removes the coil.
If a contrast material is used, a doctor, nurse or technologist will insert an intravenous catheter into a vein in your hand or arm that will be used to inject the contrast material.
You will be placed into the magnet of the MRI unit. The technologist will perform the exam while working at a computer outside of the room.
If a contrast material is used during the exam, it will be injected into the intravenous line after an initial series of scans. More images will be taken during or following the injection.
When the exam is complete, you may be asked to wait while the radiologist checks the images in case more are needed.
Your IV line will be removed after the exam is over.
Recommended Reading: Focal Cryotherapy For Prostate Cancer