Prostate Cancer Survival Rates Are Favorable Overall
Thinking about survival rates for prostate cancer takes a little mental stretching. Keep in mind that most men are around 70 when diagnosed with prostate cancer. Over, say, five years, many of these men will die from other medical problems unrelated to prostate cancer.
To determine the prostate cancer survival rate, these men are subtracted out of the calculations. Counting only the men who are left provides whats called the relative survival rate for prostate cancer.
Taking that into consideration, the relative survival rates for most kinds of prostate cancer are actually pretty good. Remember, were not counting men with prostate cancer who die of other causes:
- 92% of all prostate cancers are found when they are in the early stage, called local or regional. Almost 100% of men who have local or regional prostate cancer will survive more than five years after diagnosis.
- Fewer men have more advanced prostate cancer at the time of diagnosis. Once prostate cancer has spread beyond the prostate, survival rates fall. For men with distant spread of prostate cancer, about one-third will survive for five years after diagnosis.
Many men with prostate cancer actually will live much longer than five years after diagnosis. What about longer-term survival rates? According to the American Society of Clinical Oncology, for men with local or regional prostate cancer:
- the relative 10-year survival rate is 98%
- the relative 15-year survival rate is 96%
International Cancer Imaging Soc Oct 17 Mri In Active Surveillance Of Prostate Cancer J Ftterer
Recently, the origin and function of RJ, such as major royal jelly proteins MRJPs for the development of the larvae , antimicrobial properties , medicinal value , proteins and peptides , the potential applications for cancer treatment , and health aging and longevity have been reported.
To better understand the biochemistry, biological, and pharmaceutical response to health and life benefits of RJ, we update the knowledge from the research advances of the biological activities and pharmaceutical applications of RJ and its bioactive ingredients that are associated with farm animals, micro-organisms, laboratory animals, insects, and clinical trials in humans.
Here, our major focus is on the bioeffects of RJ, such as antimicrobial, antioxidant, anti-inflammatory, wound healing, anti-aging, immunomodulatory, anti-cancer, anti-diabetic, anti-hyperlipidemic, anti-hypertension, hepato-renal protective, neuroprotective, estrogenic, and fertility effects. This evidence 1 cm lesion on prostate a potentially valuable resource for further studies of the health potential properties of RJ for both humans and honeybees.
Better Understanding Of Prostate Cancer
Were using the power of big data, working with partners to analyse and combine data from tens of thousands of men whove been diagnosed and treated for different types and stages of prostate cancer. The aim is to find patterns in when the cancers started, how they developed and how aggressive they are. In the future this could help doctors predict how particular prostate cancers are likely to develop so we can choose the most appropriate treatment for each man.
You May Like: Perineural Tumor
Also Check: Prostate Cancer In Bones And Lungs
Correlation Between Tumor Volume Parameters
In total 549 men underwent 6 biopsies 460 , 7 biopsies and 22 , 8 biopsies. The mean total positive biopsy sample length per patient was 26 mm and the mean total tumor length was 11 mm . The median estimated and calculated tumor percentages were 33% and 33% , respectively. Average estimated tumor percentage strongly correlated with the average calculated tumor percentage . Measured total tumor length moderately correlated with calculated tumor percentage . The median greatest tumor length was 4.5 mm and the median greatest tumor percentage was 50% . Both parameters correlated moderately with calculated tumor percentage . Average tumor percentage of all biopsies correlated moderately with calculated tumor percentage . Since average estimated tumor percentage and calculated tumor percentage were strongly correlated, and estimated tumor percentage is more easily established in daily practice, we excluded average calculated tumor percentage from further analysis.
How Fast Does Prostate Cancer Spread To The Bones
Early detection can catch prostate cancer even before there are any symptoms. Some types of prostate cancer grow very slowly.
There are four main stages of prostate cancer. Within each stage, the cancer is graded based on factors like the size of tumor, prostate-specific antigen level, and other clinical signs.
If the cancer has spread to the bones, its considered to be the most advanced, or stage 4.
Newer lab tests look at the genes inside cancer cells. This can provide more information on how quickly the prostate cancer may progress.
Theres also a grading system known as the Gleason system, which assigns the cancer into a grade group based on how closely it resembles normal tissue.
During the biopsy to diagnose prostate cancer, the cells are closely examined. The more abnormal cells that are in the biopsy sample, the higher the Gleason score and grade group.
When more abnormal cells are present, the cancer is more likely to spread quickly.
Read Also: Prostate Cancer And Lung Cancer
Cancer Staging May Miss Errant Cells
Once a pathologist confirms that cancer is present, the doctor will next determine how far the cancer extends a process known as cancer staging and discuss the implications with you. This is perhaps the most important information of all for you to obtain, as it determines whether the cancer is likely to be curable, or whether it has already spread to additional tissues, making prognosis much worse.
If you were my patient, I would ask you to consider two important points. First, cancer staging actually occurs in two phases: clinical and pathological . Of the two, pathological staging is more accurate.
A second point to understand, however, is that even pathological staging can be inaccurate . A cancer spreads, or metastasizes, once a primary tumor sheds cancer cells that travel elsewhere in the body and establish other tumor sites. Metastasis is a complex process that researchers do not fully understand. What is clear is that this process involves multiple genetic mutations and steps, and that each type of cancer spreads in a unique way.
Diagnostic Criteria For Benign Prostatic Hyperplasia
Nodularity is the hallmark of Benign Prostatic Hyperplasia. In the usual case prostate enlarges up to 100gm and nodular hyperplasia of the prostate originates almost exclusively in the inner aspect of Prostate gland. On cross section, the nodules vary in color and consistency. In nodules that contain mostly glands, tissue is yellow pink with soft consistency and a milky white prostatic fluid oozes out of these areas. In nodules which are composed primarily of fibromuscular area, each nodule is pale gray, tough and does not exclude fluids.
Also Check: What Is Proton Therapy For Prostate Cancer
Are Older Men Undertreated
Schwartz and colleagues reviewed the treatment decisions and factors influencing them in a cohort of men with localized prostate cancer. Age, comorbidity, and Gleason score were found to be independent predictors of suboptimal treatment. It was concluded that most men older than 70 years with moderately or poorly differentiated tumors and no to mild comorbidity were given suboptimal treatment. Most of these men were undertreated, receiving watchful waiting therapy when potentially curative therapy could have been applied. With optimal treatment, clinical outcomes could have been improved.
Thompson and colleagues investigated otherwise healthy octogenarians diagnosed with prostate cancer who underwent radical prostatectomy. At the last follow-up visit, 10 patients had survived more than a decade after surgery, and 3 patients had died within 10 years of surgery. The remaining 6 patients were alive at less than 10 years of follow-up. Seventy-four percent of patients were continent. No patient had died of prostate cancer, and the 10-year, all-cause survival rate was similar to that observed in healthy patients 60 to 79 years old undergoing radical prostatectomy. These findings indicate that careful selection of patients even older than 80 years can achieve satisfactory oncologic and functional outcomes after surgery. It is important to note, however, that the rate of urinary incontinence after surgery exceeds that of younger counterparts.
Prostate Mri And Targeted Biopsy
September 26, 2017PCRI
Multiparametric MRI provides a three-dimensional image of the prostate, giving important information about the cancers location, size, and how aggressive it appears. MP-MRI also greatly increases the confidence that higher-grade cancers are not being overlooked in men on active surveillance. MP-MRI is usually performed without an endorectal coil.
Multiparametric Means Four Scans in One
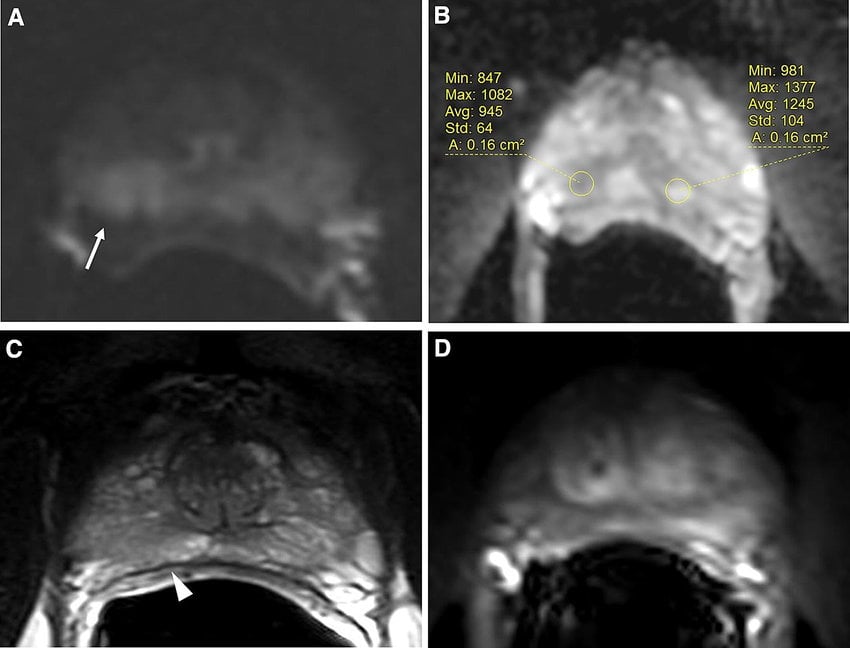
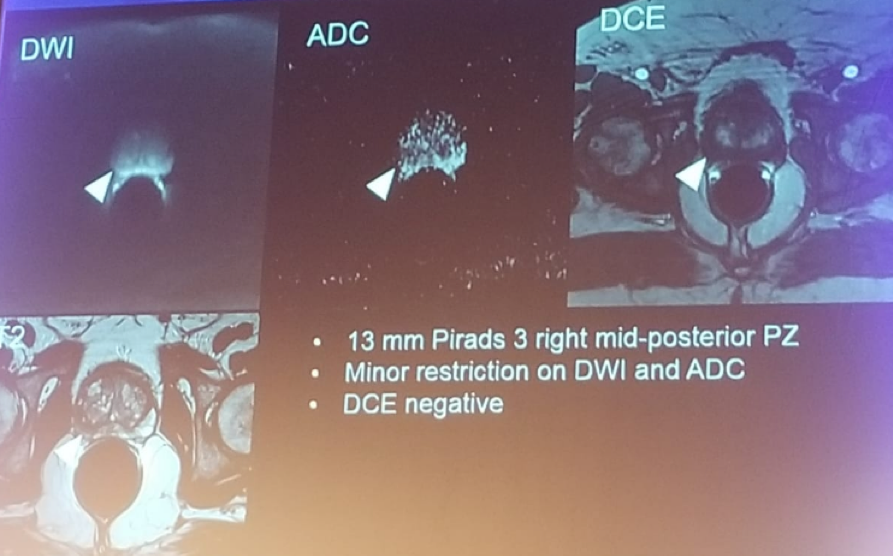
There are four different imaging components to MP-MRI. The first is called T2-weighted, which creates the clearest images and gives the most capsular detail. The second and third parameters are called diffusion-weighted imaging and the apparent-diffusion coefficient . These provide information about the aggressiveness of the tumor. The fourth, called dynamic-contrast enhancement , maps the blood flow of the tumor.
PI-RADS
PI-RADS compiles a score composed of all four parametersT2, DWI/ADC, and DCEon a 1-to-5 scale. Lesions with a score of 4 or 5 are more likely to represent clinically significant prostate cancer . Once MP-MRI detects a suspicious lesion, a targeted biopsy can be performed.
Evaluating Undiagnosed Men with High PSA Levels
MRI for Active Surveillance
The Future of Prostate MRI
Read Also: Vitamin D And Prostate Health
Table 1 Why A Low Psa Does Not Mean You Are Cancer
The Prostate Cancer Prevention Trial included a provision that men randomized to receive placebo undergo a prostate biopsy at the end of the study, even if they had normal PSA levels and digital rectal exams. To their surprise, investigators found that many of these men had prostate cancer in some cases, high-grade prostate cancer.
PSA level 13 *Note: A PSA level over 4.0 ng/ml traditionally triggers a biopsy. Adapted with permission from I.M. Thompson, et al. Prevalence of Prostate Cancer Among Men with a Prostate-Specific Antigen Level 4.0 ng per Milliliter. New England Journal of Medicine, May 27, 2004, Table 2.
This study inadvertently provided evidence not only that prostate cancer occurs more often than once believed, but also that PSA levels may not be a reliable indicator of which cancers are most aggressive. Both findings add weight to the growing consensus that many prostate tumors currently being detected may not need to have been diagnosed or treated in the first place.
Cm Lesion On Prostate 1 Introduction
The derived LOAEC for systemic effects was 32 ppm taking into account the decrease in sperm motility for male mouse exposed to vapour concentrations of 32 ppm and higher concentration levels.
All animals survived to the end of the study. The absolute weights of the liver, right kidney, and thymus of ppm males heart, liver, and right kidney of ppm females and thymus of 62 and ppm females were significantly less than those of the chamber controls.
The relative weights of the heart, right kidney, lung, and right testis of ppm males and the lung of ppm females were significantly greater than those of the chamber controls. Except for a slight 0. Histopathologic changes were noted primarily in the nasal cavity and involved both the respiratory and olfactory epithelium of males and females principally in the 62 or ppm groups.
These lesions included suppurative inflammation, squamous metaplasia of the respiratory epithelium, olfactory epithelial atrophy, and necrosis of the turbinates. Significant olfactory epithelial atrophy was already observed after treatment with 32 ppm.
A NOAEC of 16 ppm for local effects was derived based on the observed nonneoplastic lesions of the mouse nose. The derived LOAEC for systemic effects was 32 ppm taking into account the decrease in the sperm motility for male mouse exposed to vapour concentrations of 32 ppm and higher concentration levels.
Also Check: Prostate Cancer Center Of New Jersey
What Causes A Prostate Nodule
A nodule is a lump or area of hardness under the surface of the prostate. In some cases, a prostate stone, which is similar to a kidney stone, can be felt under the surface. It may seem like a nodule, but its really a tiny formation of calcified minerals. A stone is usually harmless. A true prostate nodule is an abnormal growth of cells that may or may not be cancerous.
Features Of Pin Cells
Basal cellspecific monoclonal antibodies directed against highmolecular weight keratin are used to identify HGPIN cells. Normal prostatic epithelial cells are consistently stained with these antibodies, showing a continuous, intact, circumferential basal cell layer. Cancer cells have lost their receptors for these antibodies.
Basal cell disruption affects 56% of patients with HGPIN and is usually found in glands adjacent to invasive cancer. The degree of disruption correlates with HGPIN. More than one third of the basal cell layer is lost in 52% of foci that contain HGPIN.
In persons with HGPIN and in many with low-grade cancer, the basement membrane that surrounds the prostatic glands remains intact. The expression of collagenase type 4 in PIN and associated cancer cells is abnormally high. The presence of collagenase type 4 and other enzymes is associated with a degradation of the basement membrane, allowing cell invasion into the stroma. Concurrently, the basal cell layer is diminished. This seems to occur primarily at sites of glandular outpouching.
Increased angiogenesis with an increased number of microvessels is associated with the progression of HGPIN to cancer. The microvessels in HGPIN are shorter than those in benign epithelium and have irregular contours and open lumens, an increased number of endothelial cells, and a greater distance from the basement membrane.
Also Check: Can An Enlarged Prostate Cause Constipation
Also Check: Best Cancer Center For Prostate Cancer
What Is A Hypoechoic Lesion
A hypoechoic lesion is an abnormal area that can be seen during an ultrasound examination because it is darker than the surrounding tissue. Such abnormalities can develop anywhere in the body and do not necessarily indicate cancer. Blood tests, biopsies, and further radiological studies may be required to determine the composition of a hypoechoic lesion, sometimes referred to simply as a lesion.
Detecting a Hypoechoic Lesion
During an ultrasound examination, a technician applies a handheld device known as a transducer to the area of the body requiring assessment. The transducer emits high frequency sound waves that are reflected back toward the device when they contact internal structures. A black and white image forms on a monitor, based on the intensity of the echoes. Radiologists call brighter images from highly reflective surfaces hyperechoic while areas that are less reflective appear as darkened regions and are said to be hypoechoic.
Common Hypoechoic Lesions
Gleason Score For Grading Prostate Cancer
Prostate cancer is also given a grade called a Gleason score. This score is based on how much the cancer looks like healthy tissue when viewed under a microscope. Less aggressive tumors generally look more like healthy tissue. Tumors that are more aggressive are likely to grow and spread to other parts of the body. They look less like healthy tissue.
The Gleason scoring system is the most common prostate cancer grading system used. The pathologist looks at how the cancer cells are arranged in the prostate and assigns a score on a scale of 3 to 5 from 2 different locations. Cancer cells that look similar to healthy cells receive a low score. Cancer cells that look less like healthy cells or look more aggressive receive a higher score. To assign the numbers, the pathologist determines the main pattern of cell growth, which is the area where the cancer is most obvious, and then looks for another area of growth. The doctor then gives each area a score from 3 to 5. The scores are added together to come up with an overall score between 6 and 10.
Gleason scores of 5 or lower are not used. The lowest Gleason score is 6, which is a low-grade cancer. A Gleason score of 7 is a medium-grade cancer, and a score of 8, 9, or 10 is a high-grade cancer. A lower-grade cancer grows more slowly and is less likely to spread than a high-grade cancer.
Don’t Miss: Prostate Artery Embolization For Bph
Tests To Diagnose And Stage Prostate Cancer
Most prostate cancers are first found as a result of screening. Early prostate cancers usually dont cause symptoms, but more advanced cancers are sometimes first found because of symptoms they cause.
If prostate cancer is suspected based on results of screening tests or symptoms, tests will be needed to be sure. If youre seeing your primary care doctor, you might be referred to a urologist, a doctor who treats cancers of the genital and urinary tract, including the prostate.
The actual diagnosis of prostate cancer can only be made with a prostate biopsy .
On this page
Read Also: What Is Perineural Invasion In Prostate Cancer
Improvement In Prostate Cancer Diagnostics And Disease Characterisation
Prostate cancer diagnosis has undergone a revolution, as have the accepted paradigms in other areas of medicine, by adding MRI imaging prior to invasive biopsies. Although mpMRI is not a perfect detection tool, it can have sensitivity up to 93% in identifying clinically significant lesions, compared to the 48% sensitivity of TRUS biopsy alone, as shown in the PROMIS study. Allowing the authors to conclude that mpMRI triage might allow 27% of patients to avoid a primary biopsy . The PRECISION study has since shown the advantages of mpMRI-guided biopsies in identifying clinically significant cancer, as opposed to insignificant cancer. The MRI with targeted biopsy arm detected 38% of significant and 9% of insignificant cancers, compared to the standard of care , which detected 26% of clinically significant cancer and 22% of insignificant. Clinically significant cancer was defined as the presence of a single biopsy core indicating disease of Gleason score 3+4 or greater .
Recommended Reading: What Is C61 Malignant Neoplasm Of Prostate