Choosing A Treatment Option
Treatment Options for Localized or Locally Advanced Prostate CancerA man diagnosed with localized or locally advanced prostate cancer has 3 major treatment options: Active Surveillance, surgery, and radiation therapy. For patients whose cancer appears more aggressive, combination treatment may be recommended. For …
Treatments To Help Manage Symptoms
Advanced prostate cancer can cause symptoms, such as bone pain. Speak to your doctor or nurse if you have symptoms there are treatments available to help manage them. The treatments above may help to delay or relieve some symptoms. There are also specific treatments to help manage symptoms you may hear these called palliative treatments. They include:
This is the team of health professionals involved in your care. It is likely to include:
- a specialist nurse
- a chemotherapy nurse
- a diagnostic radiographer
- a therapeutic radiographer
- other health professionals, such as a dietitian or physiotherapist.
Your MDT will meet to discuss your diagnosis and treatment options. You might not meet all the health professionals straight away.
Your main point of contact might be called your key worker. This is usually your clinical nurse specialist , but might be someone else. The key worker will co-ordinate your care and help you get information and support. You may also have close contact with your GP and the practice nurses at your GP surgery.
Treatment Of Patients With Remote Metastases
The aim of treatment is to extend life and to relieve symptoms while ensuring the best possible quality of life. Prognosis is dependent on the metastatic burden , general condition and response to treatment beyond castration.
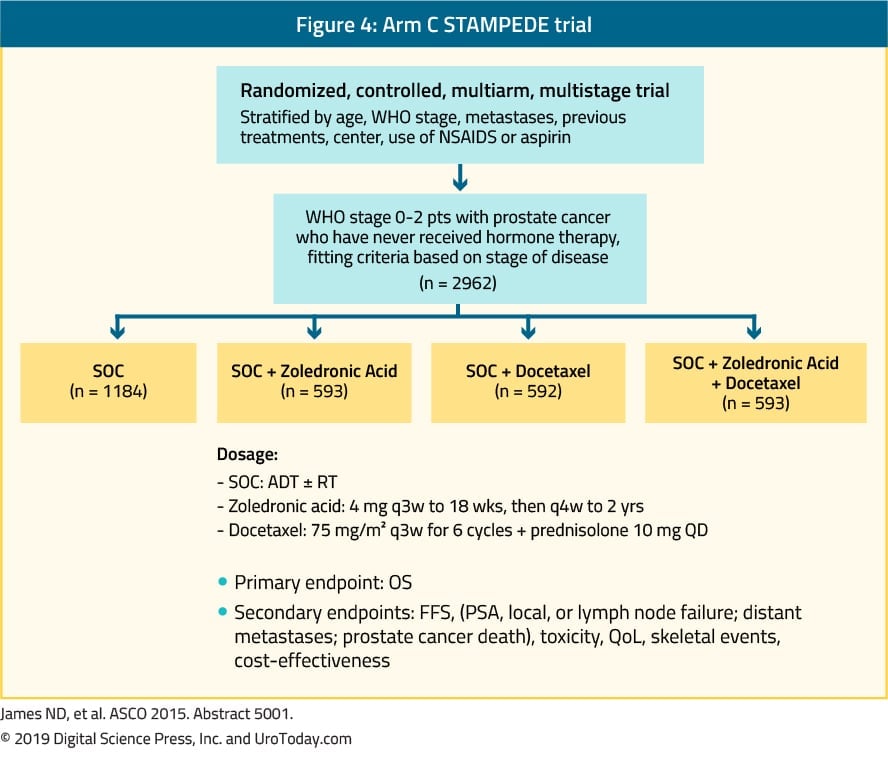
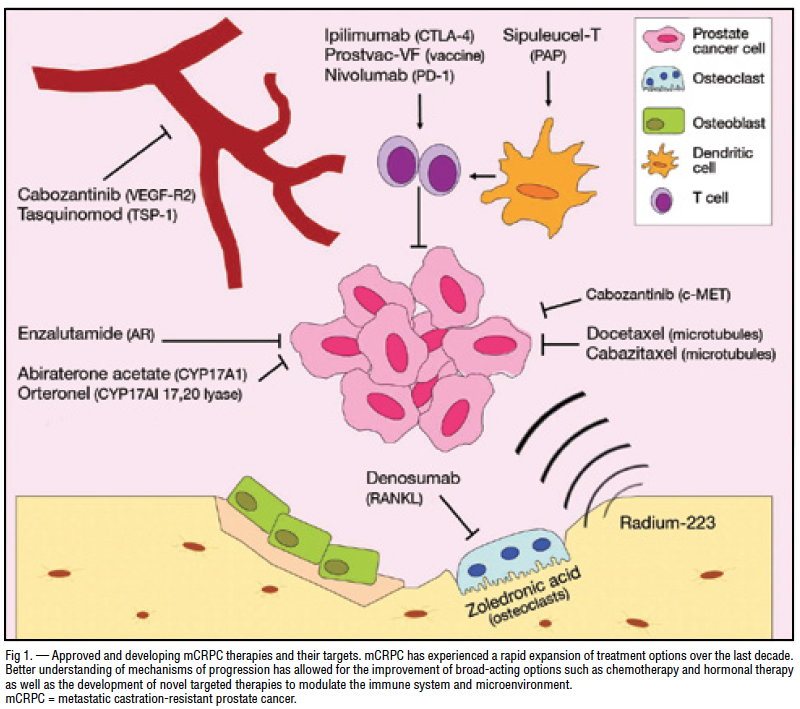
We present two algorithms for the systemic treatment of metastatic prostate cancer: one for the castration-sensitive phase and another for the castration-resistant phase .
Figure 1Figure 2
Recommended Reading: Bipolar Androgen Therapy Prostate Cancer
Treatment Of Local Events
Both the disease and its treatment can give rise to troublesome and serious consequences it is important to take these into account and to inform the patient about them early on.
Skeletal pain can be treated with palliative radiation therapy, steroids and opiates. An MRI examination should be performed promptly upon suspicion of impending spinal cord injury. If confirmed, treatment consists of immediate administration of high dose steroids combined with surgery and/or radiation therapy .
Skeletal-related events may be prevented with zoledronic acid or denosumab . Dosing intervals and when to initiate treatment are poorly defined, but common practice is to administer treatment every three months, beginning when symptomatic skeletal metastases are present. The patient should be examined by a dentist prior to use of zoledronic acid or denosumab, as there is a risk of osteonecrosis in the jaw bone . Calcium and vitamin D supplements should be taken during treatment .
Obstruction of the urinary tract or bowel may be relieved by palliative surgery, drainage or radiation therapy. Surgery, radiation therapy or embolisation may be appropriate in the event of haemorrhage.
Treatments For Prostate Cancer Spread To Bones
If prostate cancer spreads to other parts of the body, it nearly always goes to the bones first. Bone metastasis can be painful and can cause other problems, such as fractures , spinal cord compression , or high blood calcium levels, which can be dangerous or even life threatening.
If the cancer has grown outside the prostate, preventing or slowing the spread of the cancer to the bones is a major goal of treatment. If the cancer has already reached the bones, controlling or relieving pain and other complications is also a very important part of treatment.
Treatments such as hormone therapy, chemotherapy, and vaccines may help with this, but other treatments specifically target bone metastasis and the problems it may cause.
Also Check: Signs Of Prostate Cancer Mayo Clinic
What Else Do People Living With Metastatic Prostate Cancer Need To Know About Their Treatment Options
I cannot stress enough the importance of picking the righttreatment for each individual. Side effects and the expectations for diseaseresponse should be clearly discussed and understood.
Statistically, about one-third of people with metastatic prostate cancer will live more than 5 years. Understanding where your disease is on that continuum can be important for both treatment and lifestyle decisions.
That said, I am consistently amazed by what we as a medical and scientific community can do together. The huge efforts being applied to prostate cancer research hold significant promise for new and better treatment options in the near future.
Dr. Joseph Brito provides general urologic care with a special focus on minimally invasive surgical techniques and urologic oncology. Dr. Brito received his MD from George Washington University School of Medicine and Health Sciences. Dr. Brito completed a residency in urology at Rhode Island Hospital and Alpert Medical School of Brown University and trained at Yale School of Medicine in clinical oncology. Dr. Brito is a member of the American Urological Association.
FEEDBACK:
Intermittent Versus Continuous Therapy
The common complications of androgen deprivation therapy include sexual dysfunction, mood disturbance, change in body composition and osteoporosis.2,3 In view of these adverse effects intermittent dosing has been considered. This is a period of androgen deprivation therapy followed by a break until disease progression, if a good response was attained. The optimal duration of androgen deprivation therapy is fairly arbitrary as the studies have looked into various periods ranging from three months to three years.
In patients with PSA relapse only , intermittent therapy has been shown to be non-inferior to continuous dosing. There was also a better quality of life with intermittent dosing.4
In patients with objective metastases, intermittent androgen deprivation therapy had numerically worse outcomes than continuous treatment, but the study was statistically inconclusive. There was less sexual dysfunction and better mental health in the intermittent group, but this effect disappeared by 15 months when most people were back on continuous treatment.5 If short-term quality of life is important, even at the risk of possible worse survival, intermittent therapy is a reasonable approach.
Read Also: What Is Gleason 9 Prostate Cancer
Adverse Effects Of Androgen Suppression
Surgical and medical castration lead to a number of adverse effects, including the following, that can have a significant impact on a mans quality of life:
- Psychological changes
In addition, in men with prostate cancer receiving ADT, lean body mass decreases significantly after 12-36 months of treatment.
Uncertainty remains about the impact of androgen ablation on cardiovascular morbidity and mortality. However, the combination of weight gain and anemia in men with asymptomatic cardiovascular disease could adversely affect survival in some cases.
The FDA has advised that manufacturers of gonadotropin-releasing hormone agonists, which are approved for palliative treatment of advanced prostate cancer, must add safety warnings about the increased risk of diabetes and certain cardiovascular diseases in men receiving these medications. The FDA notes that although the risk for these complications appears to be low, physicians should evaluate patients for risk factors for these diseases before prescribing these agents.
Patients receiving GnRH agonists should be actively monitored for diabetes and cardiovascular disease and treated when possible. Periodic measurement of fasting glucose, cholesterol, triglycerides, and blood counts should be performed. In addition, the package inserts for all LHRH medications recommend periodically measuring serum testosterone, because levels above 50 ng/dL do occur and may adversely affect long-term survival.
Acute kidney injury
What Treatments Are Available
If you have advanced prostate cancer, treatment wont cure your cancer. But it can help keep it under control and manage any symptoms.
If youve just been diagnosed with advanced prostate cancer, you may be offered the following treatments:
- chemotherapy with hormone therapy
- clinical trials.
Research has found that having radiotherapy together with one of the main treatments listed above can help some men with advanced prostate cancer to live longer. But radiotherapy isnt suitable for all men with advanced prostate cancer.
If you live in Scotland, you may also be offered a type of hormone therapy called abiraterone acetate together with standard hormone therapy. In the rest of the UK, abiraterone is currently only given to men with advanced prostate cancer that has stopped responding to other types of hormone therapy. The National Institute for Health and Care Excellence is currently deciding whether to make it available for men who have just been diagnosed with advanced prostate cancer.
Before you start treatment
Before you start any treatment, make sure you have all the information you need. Its important to think about how you would cope with the possible side effects. Speak to your doctor or nurse about this.
It can help to write down any questions you want to ask at your next appointment. It may also help to take someone with you, such as your partner, a family member or friend.
If you have any questions, speak to our Specialist Nurses.
Read Also: Best Prostate Over The Counter Medicine
What Factors Will My Oncologist Consider When Recommending A Treatment For Metastatic Prostate Cancer
Doctors consider several factors when determining the right treatment for each patient.
First, the disease is staged, usually with imaging like a:
Second, the symptomatic status of the patient is assessed. Somepeople can have significant pain, mobility limitations, or urinary symptoms dueto metastases or local spread.
Third, the sensitivity of the disease to HMT is determined. This is usually done by measuring PSA and testosteronelevels.
Finally, a discussion between the patient and doctor should focus on the goals of care and treatment options available based on the above factors.
What Are Some Of My Options To Manage Those Side Effects
Hot flashes tend to be the most bothersome.
Non-medication strategies like keeping cool drinks with you, dressing comfortably, relaxation techniques, and breathing exercises might be helpful.
Medications, such as megestrol, estrogen therapies, antidepressants, and neuroleptic agents like gabapentin can improve hot flashes but often come with dose-limiting side effects.
Pain, although usually not a side effect of treatment, is managed with non-narcotic or narcotic pain medications. We sometimes have to manage the side effects of pain medication, such as constipation.
Using the mildest medication is always best.
Recommended Reading: Incontinence After Prostate Surgery Mayo Clinic
Radiation Therapy Plus Androgen Ablation Therapy
Androgen ablation has been shown to improve survival in men with localized disease who are treated with external radiation. DAmico et al reported higher overall survival with the combination of radiation therapy and 6 months of ADT in men with intermediate-risk prostate cancer. Median follow-up was 7.6 years.
A study by Jones et al found that for patients with stage T1b, T1c, T2a, or T2b prostate cancer and a PSA level of 20 ng/mL or less, short-term ADT increased overall survival in intermediate-riskbut not low-riskmen. The 10-year rate of overall survival was 62% with combination therapy, versus 57% with radiation therapy alone 10-year disease-specific mortality was 4% and 8%, respectively. In this study, ADT was given for 4 months, starting 2 months before radiation therapy.
In a study by Pisansky et al of 1489 intermediate-risk prostate cancer patients, disease-specific survival was not significantly different whether total androgen suppression was given for 8 weeks or for 28 weeks prior to radiation therapy. Patients in the study were randomized to 8 or 28 weeks of TAS with LHRH agonist, along with a daily nonsteroidal antiandrogen, prior to radiation treatment. This was followed in both groups by an additional 8 weeks of androgen suppression, administered concurrently with radiotherapy.
Taken together, radiation therapy is generally given for 4-36 months, depending on the risk group of the patient.
Biochemical Recurrence Without Metastatic Disease After Exhaustion Of Local Treatment Options
Biochemical recurrence is defined as a rise in PSA to 0.2 ng/mL and a confirmatory value of 0.2 ng/mL or greater following radical prostatectomy, or a rise of 2ng/mL or more above the nadir PSA after radiation therapy. Not all men who have a rising PSA will develop metastases, and for that reason not all such men require treatment. The risk of metastases and death depend on the patients Gleason score, the length of time between the nadir PSA and the onset of the PSAs rise, and the PSA doubling time.
Patients who have PSA failure following radical prostatectomy and have no evidence of metastatic disease have the options of watchful waiting, radiation therapy, or hormone ablation as salvage therapy. Similarly, patients who have PSA failure following radiation therapy have the following options:
- Watchful waiting
- Hormone ablation
The pretreatment Gleason score, clinical stage, PSA level, and percentage of positive core biopsy results have been found to be reliable predictors of failure following local therapy. Unfortunately, no means of identifying recurrences limited to the pelvis is reliable. Although a Gleason grade of 7 or less is associated with a better prognosis than a grade of 8 or more, the survival likelihood associated with a rise in the PSA level is greater if the rise occurs more than 2 years after local treatment than if it occurs less than 2 years afterward.
Don’t Miss: Does Prostate Cancer Come Back
Active Surveillance And Watchful Waiting
If prostate cancer is in an early stage, is growing slowly, and treating the cancer would cause more problems than the disease itself, a doctor may recommend active surveillance or watchful waiting.
Active surveillance. Prostate cancer treatments may seriously affect a person’s quality of life. These treatments can cause side effects, such as erectile dysfunction, which is when someone is unable to get and maintain an erection, and incontinence, which is when a person cannot control their urine flow or bowel function. In addition, many prostate cancers grow slowly and cause no symptoms or problems. For this reason, many people may consider delaying cancer treatment rather than starting treatment right away. This is called active surveillance. During active surveillance, the cancer is closely monitored for signs that it is worsening. If the cancer is found to be worsening, treatment will begin.
ASCO encourages the following testing schedule for active surveillance:
-
A PSA test every 3 to 6 months
-
A DRE at least once every year
-
Another prostate biopsy within 6 to 12 months, then a biopsy at least every 2 to 5 years
Treatment should begin if the results of the tests done during active surveillance show signs of the cancer becoming more aggressive or spreading, if the cancer causes pain, or if the cancer blocks the urinary tract.
Provenge For Advanced Prostate Cancer
Sipuleucel-T is a “vaccine” for advanced prostate cancer that helps prolong survival.
Provenge isn’t your everyday vaccine. It’s an immune therapy created by harvesting immune cells from a patient, genetically engineering them to fight prostate cancer, and then infusing them back into the patient.
It’s approved only for treatment of patients with few or no prostate cancer symptoms whose cancer has spread outside the prostate gland and is no longer responding to hormone therapy.
Once a cancer grows beyond a certain point, the immune system has a hard time fighting it. One reason is that cancer cells look a lot to the immune system like normal cells. Another reason is that tumors may give off signals that manipulate the immune system into leaving them alone.
Provenge bypasses these problems. The treatment first removes a quantity of dendritic cells from a patient’s blood. Dendritic cells show pieces of tumor to immune cells, priming them to attack cells that carry those pieces.
The patient’s doctor ships the cells to Provenge’s manufacturer, Dendreon, which then exposes them to Provenge. Provenge is a molecule made inside genetically engineered insect cells.
Once these cells have been exposed to Provenge, they’re shipped back to the doctor who infuses them back into the patient. This is done three times in one month. The first infusion primes the immune system. The second and third doses spur an anticancer immune response.
Read Also: How Do They Treat Prostate Cancer With Radiation
How Prostate Cancer Is Treated
In cancer care, different types of doctorsincluding medical oncologists, surgeons, and radiation oncologistsoften work together to create an overall treatment plan that may combine different types of treatments to treat the cancer. This is called a multidisciplinary team. Cancer care teams include a variety of other health care professionals, such as palliative care experts, physician assistants, nurse practitioners, oncology nurses, social workers, pharmacists, counselors, dietitians, physical therapists, and others.
The common types of treatments used for prostate cancer are described below. Your care plan may also include treatment for symptoms and side effects, an important part of cancer care.
Treatment options and recommendations depend on several factors, including the type and stage of cancer, possible side effects, and the patients preferences and overall health.
Cancer treatment can affect older adults in different ways. More information on the specific effects of surgery, chemotherapy, and radiation therapy on older patients can be found another section of this website.
Because most prostate cancers are found in the early stages when they are growing slowly, you usually do not have to rush to make treatment decisions. During this time, it is important to talk with your doctor about the risks and benefits of all your treatment options and when treatment should begin. This discussion should also address the current state of the cancer:
Treating Advanced Prostate Cancer
If the cancer has reached an advanced stage, it’s no longer possible to cure it. But it may be possible to slow its progression, prolong your life and relieve symptoms.
Treatment options include:
- hormone treatment
If the cancer has spread to your bones, medicines called bisphosphonates may be used. Bisphosphonates help reduce bone pain and bone loss.
Recommended Reading: How Do You Treat Chronic Prostatitis
Drug Sequencing For Androgen
The availability of the above new agents presents a challenge for physicians and patients, who must decide on the best sequence and timing for each of them. So far, no studies have been done to determine the best approach. Studies in progress are likely to result in some change to the sequencing of these drugs.
As of October 2012, and excluding cost considerations, men with asymptomatic or minimally symptomatic progressive disease can start with immunotherapy using sipuleucel-T. Since no objective responses are expected, patients can then be given abiraterone acetate.
On September 11, 2014 the FDA expanded the approved use of enzalutamide for the treatment of men with late-stage , castrate-resistant prostate cancer prior to receiving chemotherapy. The expanded indication was based on a study in which patients who received enzalutamide reduced the risk of radiographic progression or death by 83% versus placebo, while significantly reducing the risk of death by 29%.
Without formal studies to guide recommendations, either drug may be used next, although enzalutamide does not require prednisone, and for that reason it may be most suitable. Hopefully, studies will be done to determine whether men are better off receiving either enzalutamide or abiraterone first or second. Men showing progression on those drugs should then be offered docetaxel followed by cabazitaxel.
For full discussion, see Metastatic and Advanced Prostate Cancer.