Bipolar Transurethral Resection Of The Prostate Versus Other Technologies
B-TURP has been compared with HoLEP , thulium laser enucleation of the prostate , Eraser laser enucleation of the prostate , B-TUVP , and PKEP . Chen et al. showed similar functional results for B-TURP and HoLEP after 2-yr follow-up in a large RCT including 280 patients, with HoLEP associated with shorter catheterization and hospitalization durations and lower risk of bleeding . Fayad et al., in a smaller study, found no significant differences in postoperative parameters between the two groups .
In a long-term RCT, Zhu et al. showed that PKEP was superior to B-TURP on IPSS reduction and Qmax improvement after 5 yr in patients with prostates > 70 ml, as well as better perioperative outcomes .
Yang et al. reported no difference in functional parameters between ThuLEP and Gyrus-PK B-TURP after a follow-up of 18 mo, but favorable short-term outcomes with ThuLEP . The same conclusions were obtained in favor of ELEP compared with Gyrus-PK B-TURP after 6-mo follow-up .
Olympus TURis and B-TUVP using a button-type vapor-resection electrode were compared by Geavlete et al. in a three-arm RCT, showing better functional results for the TURis arm, as well as fewer postoperative complications .
None of these comparisons was suitable for meta-analysis, and the paucity of the data must lead to cautious interpretation of the results.
What Is An Enlarged Prostate
The prostate is part of a mans reproductive system. This walnut-sized gland sits between the bladder and pelvic floor muscles in front of the rectum. Its job is to produce fluid that mixes with sperm to form semen during ejaculation.
Men typically dont have to think about their prostate until they age. Then it begins to grow, possibly due to changes in hormone production. An enlarged prostate is sometimes called benign prostatic hyperplasia .
As the prostate enlarges, it presses on the urethra, which is the tube that connects to the urinary bladder. Urine flows through the urethra on its way out of the penis. This pressure squeezes and narrows the urethral lumen and can block the flow of urine.
Doctors choose treatments for BPH based on the level of swelling in the prostate, your symptoms, and other factors. The most common treatments are:
- medication to shrink the prostate
- medication to relax the bladder neck and muscle within your prostatic urethra to make urinating easier
- surgery to remove extra prostate tissue
The most common surgery for BPH is TURP. During this procedure, the surgeon inserts a well-lighted scope into the urethra and uses an electrical wire loop to cut and remove excess prostate tissue.
Transurethral Resection Of The Prostate : Home Recovery
Take it easy for the first month or so while you heal after transurethral resection of the prostate. During the first few weeks, you may feel burning when you pass urine. You may also feel like you have to urinate often. These sensations will go away. If your urine becomes bright red, it means that the treated area is bleeding. This may happen on and off for a month or so after a TURP. If this occurs, rest and drink plenty of fluids until the bleeding stops.
Recommended Reading: Prostate And Bladder Cancer Survival Rate
Who Should Receive Transurethral Vaporization
Patients suffering from an enlarged prostate are candidates for a TUVP. Unfortunately, with each pass of the roller, the layer below the vaporized tissue becomes more solid, or coagulated. This coagulated tissue is harder to vaporize — a drawback that makes the procedure more tedious and time-consuming. For this reason, TUVP is best limited to men with small prostates.
- Connect
What Are The Risks
In most cases, TURP is a safe procedure and the risk of serious complications is very small.
However, many men who have a TURP lose the ability to ejaculate semen during sex or masturbation, although they still have physical pleasure from ejaculation . This is known as retrograde ejaculation.
Some men also lose the ability to control their bladder , although this usually passes in a few weeks. In rare cases, it may be persistent and need further treatment.
There’s also a small risk of problems such as erectile dysfunction, difficulties passing urine and urinary tract infections .
You May Like: Prostate Cancer And Kidney Cancer
Transurethral Vaporization Of The Prostate
Transurethral vaporization of the prostate , a technique that employs well-known electrosurgical principles, was introduced approximately 10 years ago . At the moment data about two RCTs with a follow-up of more than five years are available. In a prospective study Hammadeh et al. compared TUVP with conventional TURP and followed their patients for five years . They conclude that TUVP is as effective as standard TURP in the treatment of medium-size prostates. The reintervention and complication rates were comparable and initial improvement could be maintained during a five-year period for most patients who underwent TUVP. Of note, prostate size was rather small with 27 ml resp. 32 ml . The fairly excessive energy application during TUVP , an issue that has been associated with postoperative dysuria, urge incontinence, and erectile dysfunction generated no adverse events. New onset impotence was higher in the TUVP group than in the TURP group but did not reach statistical significance.
These findings are confirmed by van Melick et al., who prospectively randomised men to TUVP or TURP with a mean follow-up of 4.3 years . They demonstrate durable subjective and objective results for patients with LUTS who were treated by TUVP. Again, prostate sizes were noticeably small, averaging 37 ml resp. 35 ml .
Sascha A. Ahyai, … Christian G. Stief, in, 2010
Postoperative Complications And Management
Improvement of technology and refinement of technique has reduced the complication rates of TURP, with contemporary studies demonstrating a 5% risk of reoperation within 5 years and 110% complication rate for TURP performed for BPH . Increasing gland size and pre-operative retention appear to be risk factors for additional procedures .
Bladder neck contracture rates have been fairly consistent over time at around 2% but have occasionally been quoted at much higher rates. Over-fulguration of the bladder neck during the procedure is thought to be causative and patients will generally report worsening urinary flow rates around 6 months from TURP . Office cystoscopy is diagnostic and gentle dilation using sounds or balloon can be tried as first line. After more conservative approaches have failed, endoscopic incision in the OR is generally the next step. We recommend more aggressive incision at this time with the expectation of peri-vesical fat in the lateral incisions.
The larger scope required during TURP may predispose to urethral stricture and a rate of 4.1% was found in an analysis of 34 randomized controlled trials . The scope should be kept well lubricated and movement of the scope within the urethra should be minimized to decrease rates of this complication.
Also Check: Prostate Cancer Erectile Dysfunction Treatment
Incidence Of Treatment Failure
The primary outcome, treatment failure, was defined as any subsequent surgical reintervention or any emergency acute urinary retention event after the initial procedure. The median follow-up time was 2.8 years.
At seven years, the unadjusted cumulative failure rates were 15% for TURP, 14% for PVP, 7% for EEP and 18% for other procedures .
Holmium Laser Enucleation Of The Prostate Versus Bipolar Vaporization Of The Prostate
The safety profile of holmium laser enucleation of the prostate , very similar to that of TURP, together with its excellent long-term postoperative results, and with the fact that the procedure does not depend on prostate size, makes the procedure a very strong competitor for the role of the new gold standard in transurethral surgery for BPH . Unfortunately, at this moment we do not have available any data comparing directly the results of HoLEP with those of bipolar vaporization of the prostate. Perhaps future randomized, prospective trials will address this comparison between two emerging technologies.
You May Like: How Long Does A Prostate Biopsy Take
Intraoperative Complications And Management
Intraoperative bleeding during TURP is common and hemostasis should be maintained through the procedure as an incremental process. If not controlled during the procedure, the sheer volume of small bleeding areas can become overwhelming to the surgeon. A recent analysis of RCTs found that 4.4% of patients required transfusion after TURP , emphasizing the importance of maintaining hemostasis.
Arterial bleeding is characterized by a bright red, pulsatile appearance. A more advanced resectionist may continue to resect areas of arterial bleeding if not yet to the depth of the surgical capsule. The resectionist may just slow the resection over the areas of arterial bleeding in a hope to coagulate the bleeding area with the next resection swipe. This of course improves efficiency of the overall procedure but increases the potential for overwhelming bleeding. Above all else, the resectionist should not move the resection away from a bleeding and exposed artery until it has been controlled. Often arterial bleeding is not completely controlled until the capsule is reached in that area. During the operation, the resecting loop should be placed against the bleeding vessel to tamponade the vessel with the fulguration pedal then pressed as it allows for more selective vaporization. Haphazard coagulation should be discouraged is it can lead to delayed hemorrhage due to sloughing of tissue.
Is Greenlight Laser Pvp Treatment Right For Me
GreenLight Laser PVP is a recent addition to the minimally invasive techniques in the treatment of BPH. The procedure uses the technology of high-powered laser light combined with fiber optics to vaporize the overgrowth of prostate cells quickly and accurately. As the surgeon directs the laser at the prostate, the intense pulses of light emitted from the fiber are absorbed by the blood. Within moments, the temperature of the blood becomes so great it causes the nearby cells to vaporize. GreenLight is being used as an alternative to transurethral resection of the prostate and has been shown to be its equal in terms of effectiveness in an improvement of symptoms. There is growing interest in this technique by patients and practitioners because of its simplicity and efficiency. GreenLight stands alone in its ability to give patients quick symptom relief, ease and comfort of urinary flow, and minimal short-term side effects. This technique is too new for long-term studies to have been completed, but after five years it has been shown to maintain its level of improvement in urinary flow and comfort, and for giving men the quality of life they deserve.
You May Like: Radiation For Recurrent Prostate Cancer
Transurethral Electrovaporization Of The Prostate As An Alternative To Transurethral Resection: A Five
ABSTRACT
INTRODUCTION: The aim of the present study was to compare the safety and efficacy of transurethral electrovaporization of the prostate with conventional transurethral resection of the prostate in the treatment of patients with moderate to severe bladder outlet obstruction due to benign prostatic hyperplasia .
METHODS: Between December 2001 and November 2003, 131 patients presented to the author’s institution with moderate to severe bladder outflow symptoms due to BPH. The patients were randomly assigned to undergo TURP or TUVP . Patients receiving TURP had a significantly larger mean prostate size but were similar in all other evaluated characteristics. Using the hospital database, the author reports the available follow-up results after 1, 2, 3, and 5 years. The International Prostate Symptom Score , uroflowmetry , and postvoid residual volume were used for evaluation. Operative time, catheterization time, hospital stay, and blood tests were also compared.
KEYWORDS: Transurethral electrovaporization of the prostate Transurethral resection of the prostate .
CORRESPONDENCE: Ehab Rifat Tawfiek MD, Department of Urology, El Minia University Hospital, Elminia 16666, Egypt .
INTRODUCTION
Transurethral electrovaporization of the prostate is one of the recent promising alternatives to TURP. It combines tissue removal by vaporization with coagulation, thereby reducing the degree of bleeding.
METHODS
Participants
Evaluation
Surgical Procedures
Data Analysis
RESULTS
Transurethral Resection Of The Prostate
TURP is also a very common surgery for BPH. About 150,000 men in the United States have TURP each year.
After anesthesia, the surgeon inserts a thin, tube-like instrument through the tip of the penis into the urethra. The resectoscope has a light, valves for irrigating fluid, and a thin wire loop. An electrical current is passed along the wire. The surgeon uses the electrified wire to cut away prostate tissue that is blocking the urethra and seal blood vessels. The removed tissue is flushed into the bladder and from there out of the body. You will need to use a catheter for 1 to 2 days after the procedure.
You May Like: What Is Malignant Neoplasm Of Prostate
Benefits Of Button Turp
Button TURP appears to be just as effective as traditional TURP at shrinking the prostate. A few studies have hinted at some advantages of this newer procedure, but there isnt much long-term evidence to prove that its any better than regular TURP.
One theoretical advantage of button TURP is that all the energy stays inside the device. In regular TURP, the electric current can leave the wire and damage tissues around the prostate.
Some studies have found that button TURP reduces complications, like bleeding after surgery. It may also lessen the time men need to use a catheter for irrigation or drainage after surgery. Yet other studies have found no difference in complication rates.
One post-surgery problem button TURP does seem to prevent is a rare but very serious condition called TUR syndrome. During TURP, the surgeon washes out the surgical area with a low sodium solution to keep the area clean. Because this solution can get into the bloodstream in greater amounts through the venous areas of resected prostate tissue, it can cause dilution to a below-normal sodium level in the bloodstream.
In contrast, button TURP uses a saline solution with more sodium in it than what is used in a TURP, which seems to help prevent TUR syndrome. The reduced risk of TUR syndrome allows surgeons to spend more time doing the procedure. This means they can work on larger prostates or perform more complex surgeries with button TURP.
Standard Monopolar Resection Of The Prostate
In 1929, McLean was one of the first authors who studied and presented the principles of electrosurgery . After the introduction of the electrosurgery generator device, developed by Bovie and Cushing, one of its initial applications was the resectoscope, in the 1930s . The resection loop was mounted on an adapted cystoscope and the high frequency electrosurgery generator was able to deliver both cutting and coagulation current.
Despite all of the subsequent technical improvements , the technical principle behind TURP remains the same as 80 years ago, with all of its derived disadvantages, including the use of hypotonic irrigation solutions, which may cause the TURP syndrome .
Recommended Reading: Non Metastatic Castration Resistant Prostate Cancer
Postoperative Complication In Patients
The occurrence of postoperative complications was statistically analyzed . The results showed gross hematuria appeared in 12 BPH patients, hematospermia in 125 cases, dysuria in 36 patients, temporary urinary incontinence in 68 patients, urinary retention in 152 patients, urethral injury in 69 patients, and urinary tract infection in 19 cases. And hematospermia and urinary retention had the highest number of cases. The total cases of recurrence were 384, with an incidence rate of 18.7%.
While You Are Healing
To help prevent problems during the first month after your surgery, follow these tips:
-
Drink plenty of fluids.
-
Dont lift anything over 10 pounds.
-
Avoid sexual activity and strenuous exercise.
-
Avoid straining at stool. If you are constipated, take stool softeners or laxatives for a few days.
-
Talk to your doctor about when you can return to work.
-
Ask your doctor when you can start driving again.
-
Dont sit for more than 60 minutes without getting up.
-
Check with your doctor before taking over-the-counter pain relievers. These include aspirin, ibuprofen, and naproxen.
Also Check: What Is Sbrt For Prostate Cancer
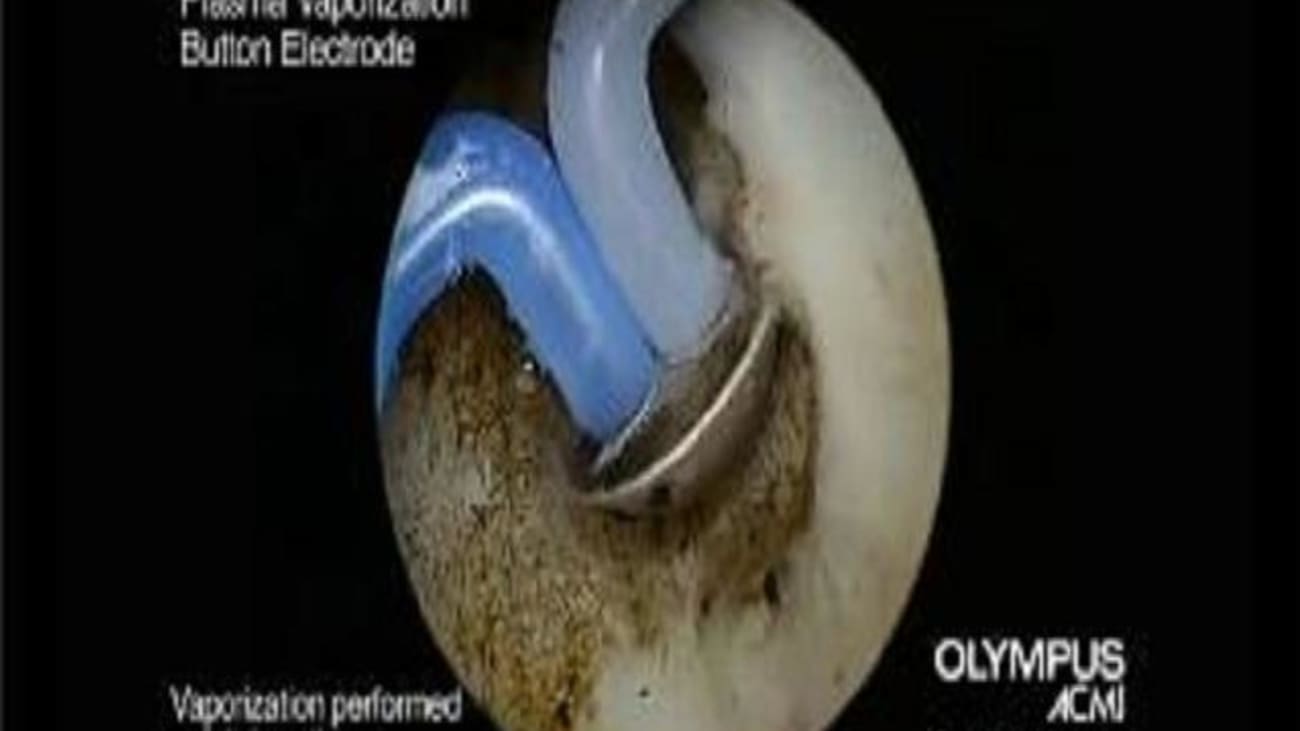
The Plasmabutton Represents The Forefront Of Innovation For The Minimally Invasive Surgical Treatment Of Bph
PlasmaButton vaporization is a completely new surgical option that is now available to doctors for the treatment of benign prostatic hyperplasia. It is an innovative advancement to a conventional TURP in which prostate tissue is removed more gently using low temperature plasma energy. This device is not for use in treating prostate cancer.
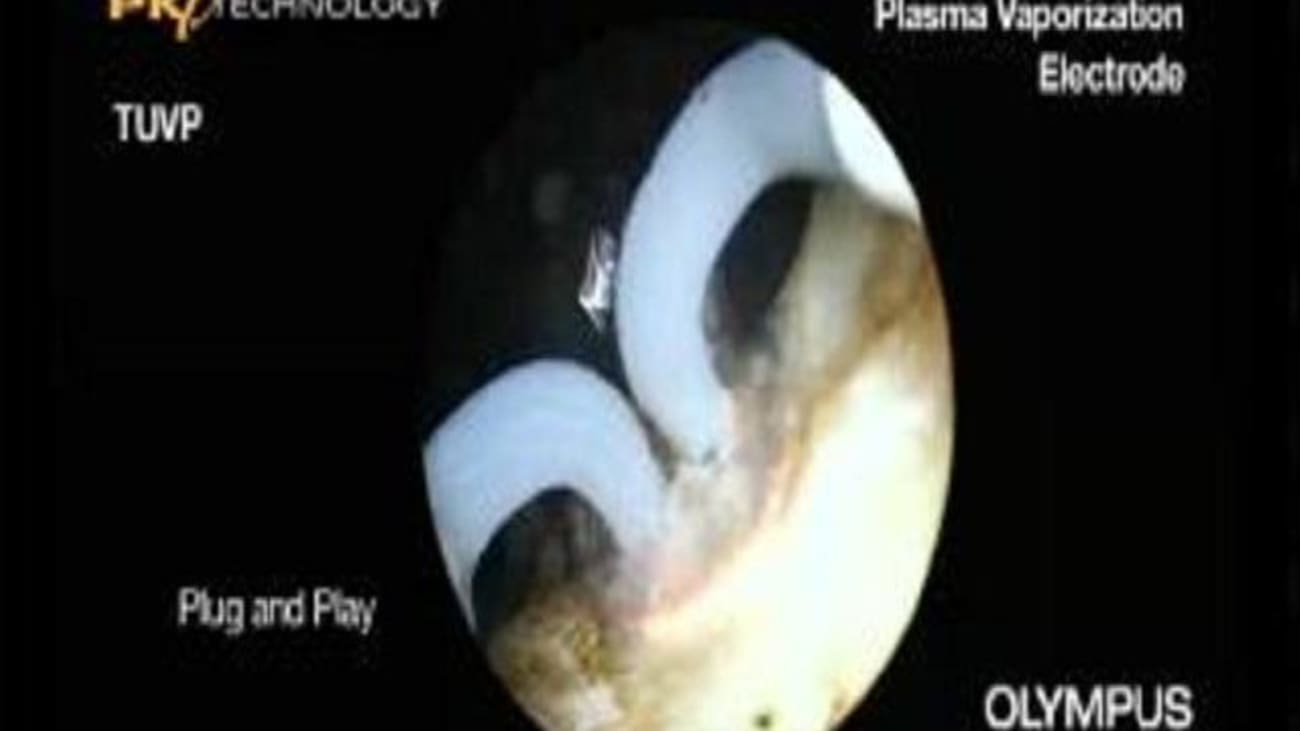
As opposed to the conventional TURP, this new procedure does not cut and shave off tissue with a loop or burn it away with a laser, but gently vaporizes the tissue with a small button-shaped electrode. Using low-voltage energy, a plasma field is created that coats the half-spherical shaped button. Tissue in contact with this plasma field is vaporized. The surgeon uses a unique hovering technique so there is virtually no direct contact needed between the Button and tissue. This advanced Button not only vaporizes the enlarged tissue, it also coagulates the remaining healthy tissue and leaves behind a smooth surface. Bleeding during and after surgery can be minimized from the start encouraging a rapid healing process.
Clinical Benefits:
- Virtually bloodless vaporization of the prostate
- Short catheterization time
- Reduced risk of obturator nerve stimulation
- No risk of hyponatremia
- Less bleeding .
Who Are Good Candiates For Pvp
Good candidates for PVP include men with small- to moderate-sized prostates and those with too many medical problems for more-invasive surgery. Men with weak hearts are also good candidates because there is no blood loss. So are men who want to limit anesthesia. Men with a higher risk of bleeding, such as those taking blood-thinning medications, may also be good candidates for PVP.
Transurethral Resection of the Prostate Medical Illustration Copyright © 2015
Don’t Miss: Focused Ultrasound For Prostate Cancer
Transurethral Vaporizationresection Of The Prostate Versus Standard Transurethral Prostatectomy: Comparative Changes In Histopathological Features Of The Resected Specimens
Log in to MyKarger to check if you already have access to this content.
Buy a Karger Article Bundle and profit from a discount!
If you would like to redeem your KAB credit, please log in.
Save over 20%
- Unlimited fulltext viewing Of this article
- Organize, annotate And mark up articles
- Printing And downloading restrictions apply
For eJournal Archive and eJournal Backfiles information please contact Karger service
The final prices may differ from the prices shown due to specifics of VAT rules.