What Can Affect My Outlook
No one can tell you exactly what will happen. How prostate cancer affects you will depend on many things.
- Your stage Whether your cancer is localised, locally advanced, or advanced.
- Your Gleason score or grade group The higher your Gleason score, the more aggressive the cancer, and the more likely it is to spread.
- Your treatment options You may be able to have treatment aimed at getting rid of the cancer. Or you may be able to have treatment to keep the cancer under control. Read more about choosing your treatment.
- Your health If you have other health problems, you may have fewer treatment options. And you may be more likely to die from another condition, such as heart disease.
- Your PSA level After youve been diagnosed, PSA tests are a good way of monitoring your prostate cancer and seeing how youre responding to treatment.
- How successful your treatment is Your treatment may be successful at getting rid of your cancer or keeping it under control. But for some men, treatment may not work as well as expected.
Risk Of Progression Of Prostate Cancer
Prostate cancer can also be classified based on the risk of recurrence . For this assessment, that can impact your choice of therapeutic approach, we take into account your clinical stage, PSA level, and Gleason score.
Low risk
Your cancer may be at low risk of spreading if:
- Your PSA level is less than 10 ng/mL
- You Gleason score is 6 or less
- Your cancer is stage T1 or T2a
Medium risk
Your cancer may be at medium risk of spreading if:
- Your PSA level is between 10 and 20 ng/mL
- Your Gleason score is 7
- Your cancer is stage T2b
High risk
Your cancer may be at high risk of spreading if:
- Your PSA level is higher than 20 ng/mL
- Your Gleason score is 8, 9 or 10
- Your cancer is stage T2c, T3 or T4
The Bogus Gleason 6 Prostate Cancer
The very common Gleason 6 type of prostate cancer href=http://www.ascopost.com/issues/june-10-2016/prostate-cancer-opinions-vary-on-gleason-scores-and-surgery/ rel=noopener> fails to behave as a cancer and should NOT be called a cancer. The all-inclusive prostate cancer label is deceitful by implying that all prostate cancers are equal and have the power to kill rapidly. It has been well established fact that the common Gleason 6 type of prostate cancer should not be called a cancer at all.
Dont Miss: Best Prostate Over The Counter Medicine
Also Check: What If Prostate Biopsy Is Positive
What Does It Mean To Have A Gleason Score Of 6 7 8 Or 9
Because grades 1 and 2 are not often used for biopsies, the lowest Gleason score of a cancer found on a prostate biopsy is 6. These cancers may be called well differentiated or low-grade and are likely to be less aggressive that is, they tend to grow and spread slowly.
Cancers with Gleason scores of 8 to 10 may be called poorly differentiated or high-grade. These cancers are likely to grow and spread more quickly, although a cancer with a Gleason score of 9-10 is twice as likely to grow and spread quickly as a cancer with a Gleason score of 8.
Cancers with a Gleason score of 7 can either be Gleason score 3+4=7 or Gleason score 4+3=7:
- Gleason score 3+4=7 tumors still have a good prognosis , although not as good as a Gleason score 6 tumor.
- A Gleason score 4+3=7 tumor is more likely to grow and spread than a 3+4=7 tumor, yet not as likely as a Gleason score 8 tumor.
Also Check: What Does Prostate Cancer Feel Like
How Important Is The Gleason Score

The Gleason Score is very useful for predicting the behavior of a prostate cancer. However, other factors also contribute to determining the stage of prostate cancer, including:
- The PSA level
- Findings from a rectal exam
- The number of biopsy core samples that contain cancer
- The percentage of cancer making up each biopsy core sample
- If cancer is found in one or both sides of the prostate
- If the cancer has spread outside the prostate
You May Like: What Is Prostate Gland Enlargement
What Happens When Prostate Cancer Is Left Untreated
While most men undergo some form of treatment for their prostate cancer, some men today choose to not be treated for their prostate cancer. Instead, they may choose to have their healthcare providers monitor their cancer.
Known as active surveillance, it is common when the cancer is expected to grow slowly based on biopsy results, confined to the prostate, not causing any symptoms, and/or small. In active surveillance, healthcare providers will initiate cancer treatment only if cancer starts growing.
Others men may choose to not undergo cancer treatment because of a short life expectancy or other serious medical problems. They may feel that the risks or side effects of cancer treatment outweigh their potential benefits.
This option is certainly OK and reasonable in the right circumstancesrequiring a careful and thoughtful discussion with your healthcare provider and family.
Prostate Cancer Grading & Prognostic Scoring
The Gleason Score is the grading system used to determine the aggressiveness of prostate cancer. This grading system can be used to choose appropriate treatment options. The Gleason Score ranges from 1-5 and describes how much the cancer from a biopsy looks like healthy tissue or abnormal tissue . Most cancers score a grade of 3 or higher.
Since prostate tumors are often made up of cancerous cells that have different grades, two grades are assigned for each patient. A primary grade is given to describe the cells that make up the largest area of the tumor and a secondary grade is given to describe the cells of the next largest area. For instance, if the Gleason Score is written as 3+4=7, it means most of the tumor is grade 3 and the next largest section of the tumor is grade 4, together they make up the total Gleason Score. If the cancer is almost entirely made up of cells with the same score, the grade for that area is counted twice to calculated the total Gleason Score. Typical Gleason Scores range from 6-10. The higher the Gleason Score, the more likely that the cancer will grow and spread quickly.
You May Like: How Do You Die From Prostate Cancer
The Gleason Grading System
Screening for prostate cancer involves the prostate-specific antigen test and a digital rectal exam. If results are suspect, your doctor may recommend a prostate biopsythe only way to confirm the diagnosis.
During a prostate biopsy, a urologist uses a small needle to remove tissue samples from different parts of the prostate. These samplesalso called coresare then sent to a pathologist so they can review each one under a microscope.
The pathologist uses a pattern scale, developed by Donald Gleason, MD, PhD in 1966, to give each sample a grade from 1 to 5. Grade 1 cells are well-differentiated and look like normal tissue. Grade 5 cells, on the other hand, are “poorly differentiated” or even unrecognizable from normal tissue.
Your Gleason score is the sum of the two numbers that represent the most common types of tissue found in your biopsy. The first number in the equation is the most common grade present, the second number is the second most common grade. For example, if seven of your cores are grade 5 and five are grade 4, your Gleason score would be 5+4, or a Gleason 9.
Today, pathologists typically only flag tissue samples that are grade 3 or higher, making 6 the lowest Gleason score.
In 2014, a revised grading system for prostate cancercalled Grade Groupswas established. This system builds on the Gleason scoring system and breaks prostate cancer into five groups based on risk. This can help make it easier to understand the Gleason score scale.
Active Surveillance Testing Schedule
Medical experts offer various recommendations regarding frequency of testing and when to start treatment during active surveillance. The American Society of Clinical Oncology recommends the following periodic evaluations while under active surveillance for prostate cancer:
-
PSA testing every three to six months
-
A digital rectal exam at least once a year
-
A prostate biopsy at least every two to five years
If test results or symptoms indicate the cancer is progressing, treatment is recommended with the intention of curing the disease.
Also Check: Do Prostate Supplements Really Work
Associations Of Clinical Parameters With Survival
The mean overall survival of the entire patient collective was 14.3 years .
A low Gleason Score of 46 was found in 24 cases , whereas 26 showed a GS of 7 or higher. Patients with a GS of 46 had a longer OS of 17.9 years compared to 11 years for patients with a GS of 710 . Furthermore, the GS was a significant predictor of OS in univariable cox regression analysis . Neither pathological stage nor preoperative PSA value showed a significant association with OS .
Gleason : Is It A Cancer
This important question has significant clinical and public health implications. Unfortunately, there is no simple answer. There are substantial limitations to our ability to accurately risk stratify detected prostate cancers. As a result of random systematic biopsies, Gleason 6 disease often coexists with undetected higher-grade disease. Some argue that this alone justifies labeling Gleason 6 disease as a cancer. We disagree. By extension of this guilt-by-association reasoning, high-grade prostatic intraepithelial neoplasia and atypical small cell acinar proliferation, both of which are known to coexist with undetected cancer, should be labeled as cancers. In fact, we know that many cancers remain undiagnosed owing to a false-negative biopsy that shows only benign prostatic hyperplasia. Is benign prostatic hyperplasia cancer? Where do we draw the line?
Don’t Miss: What Does Grade 4 Prostate Cancer Mean
Active Surveillance For Prostate Cancer
If diagnosed with localized prostate cancer , disease management can take many forms, depending on the risk category of disease. Patients with low-grade, slow-growing tumors confined to the prostate gland may consider active surveillance. This involves monitoring prostate cancer in its localized stage until your doctor feels that further treatment is needed to halt the disease at a curable stage.
According to the American Society of Clinical Oncology, patients with low-risk, low-grade disease can consider active surveillance. It may also be an option for patients with a Gleason score of 7. Patients within these categories may choose to postpone prostate cancer treatment because of its associated risks and side effects.
Study Population And Data Collection
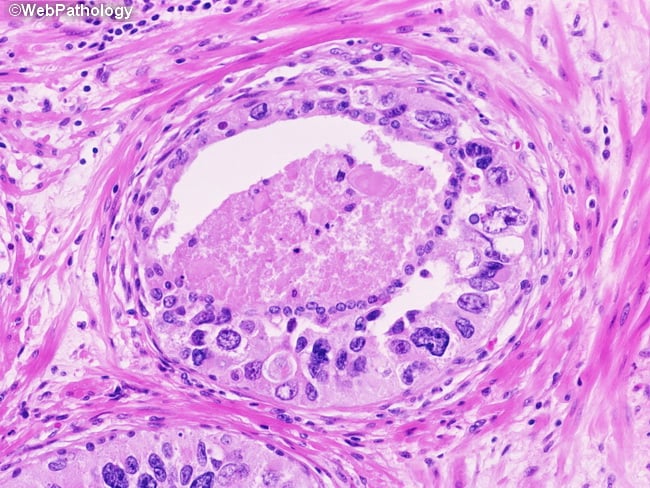
This was a population-based study in which potential cases were identified from six cancer registries in Great Britain. Within each region, collaborating hospitals were sought and cases from these hospitals were reviewed. National approval was obtained from the Northern Multi-Research Ethics Committee, followed by local ethics committee approval at each of the collaborating hospital trusts .
Men were included in this study if they were under age 76 years at the date of diagnosis and had clinically localised prostate cancer diagnosed by transurethral resection of the prostate or needle biopsy. Diagnosis between 1990 and 1996 and a baseline PSA were required.
Patients treated by radical prostatectomy or radiation therapy within 6 months of diagnosis were excluded. In addition, those with objective evidence of metastatic disease or clinical indications of metastatic disease , or a PSA measurement over 100ngml1 at or within 6 months of diagnosis were also excluded. These exclusions were a pragmatic method of focusing the study on patients who were very likely to have truly localised disease at presentation. Men who had hormone therapy prior to diagnostic biopsy were also excluded, because of the influence of hormone treatment on interpreting Gleason grade. We also excluded men who died within 6 months of diagnosis, or had less than 6 months of follow-up.
Figure 1
You May Like: How To Treat Inflamed Prostate
Also Check: Can You Be Asleep During A Prostate Biopsy
What Are The Damico Risk Categories
The DAmico system provides an estimate of the risk of recurrence at five years after treatment. This system is one of the most widely used for risk assessment. It combines the PSA, Gleason score, and the clinical stage to create low, intermediate, and high risk categories. The higher the risk category, the higher the chance of recurrence is five years after treatment.
The DAmico risk categories are below. If one factor is putting you in a lower category but another is putting you in a higher category, then the higher category takes precedent.
Read Also: What Kind Of Doctor Checks For Prostate Cancer
Gleason Score For Grading Prostate Cancer
Prostate cancer is also given a grade called a Gleason score. This score is based on how much the cancer looks like healthy tissue when viewed under a microscope. Less aggressive tumors generally look more like healthy tissue. Tumors that are more aggressive are likely to grow and spread to other parts of the body. They look less like healthy tissue.
The Gleason scoring system is the most common prostate cancer grading system used. The pathologist looks at how the cancer cells are arranged in the prostate and assigns a score on a scale of 3 to 5 from 2 different locations. Cancer cells that look similar to healthy cells receive a low score. Cancer cells that look less like healthy cells or look more aggressive receive a higher score. To assign the numbers, the pathologist determines the main pattern of cell growth, which is the area where the cancer is most obvious, and then looks for another area of growth. The doctor then gives each area a score from 3 to 5. The scores are added together to come up with an overall score between 6 and 10.
Gleason scores of 5 or lower are not used. The lowest Gleason score is 6, which is a low-grade cancer. A Gleason score of 7 is a medium-grade cancer, and a score of 8, 9, or 10 is a high-grade cancer. A lower-grade cancer grows more slowly and is less likely to spread than a high-grade cancer.
Also Check: Best Over The Counter For Enlarged Prostate
How Do I Know The Gleason Grade Is Accurate
Assigning the correct Gleason score is a skill just like any other that is developed through experience and practice. It is often prudent to have the biopsy material referred for a second opinion at a reference center to confirm the accuracy of the initial Gleason score that was assigned.
References:
What Is Advanced Prostate Cancer
When prostate cancer spreads beyond the prostate or returns after treatment, it is often called advanced prostate cancer.
Prostate cancer is often grouped into four stages, with stages III and IV being more advanced prostate cancer.
- Early Stage | Stages I & II: The tumor has not spread beyond the prostate.
- Locally Advanced | Stage III: Cancer has spread outside the prostate but only to nearby tissues.
- Advanced | Stage IV: Cancer has spread outside the prostate to other parts such as the lymph nodes, bones, liver or lungs.
When an early stage prostate cancer is found, it may be treated or placed on surveillance . Advanced prostate cancer is not curable, but there are many ways to treat it. Treatment can help slow advanced prostate cancer progression.
There are several types of advanced prostate cancer, including:
Biochemical Recurrence
With biochemical recurrence, the prostate-specific antigen level has risen after treatment using surgery or radiation, with no other sign of cancer.
Castration-Resistant Prostate Cancer
Non-Metastatic Castration-Resistant Prostate Cancer
Prostate cancer that no longer responds to hormone treatment and is only found in the prostate. This is found by a rise in the PSA level, while the testosterone level stays low. Imaging tests do not show signs the cancer has spread.
Metastatic Prostate Cancer
- Other organs, such as liver or lungs
Metastatic Hormone-Sensitive Prostate Cancer
Don’t Miss: How Do You Screen For Prostate Cancer
Survey: Perception Of Gleason 6 Prostate Cancer
There are many management options for men diagnosed with Gleason 6 prostate cancer. Treatment with radiation or surgery remains relatively common. There are significant concerns regarding proper patient counseling, a significant potential for overtreatment, and a possible lack of shared decision-making between physicians and their patients.
Ragheed Saoud, SUO Fellow at the University of Chicago Alejandro Berlin, Radiation Oncologist at the University of Toronto and Scott Eggener, Urologic Oncologist at the University of Chicago, have developed a survey, evaluating the perception of ISUP Grade Group 1 prostate cancer among treating physicians across multiple specialties . Additionally, the survey will evaluate physician practices across the world to understand their thoughts on how indolent or lethal Gleason 6 prostate cancer is. Additionally, the survey will explore the extent to which very low and low-risk prostate cancer is managed.
The goal is to reach as many people as possible. Once published, results from this study will be a valuable contribution to the literature. The hypothesis being that ISUP GG1 disease remains overtreated due to common misconceptions regarding its true natural history. This hypothesis dovetails with initiatives suggesting GG1 cancer should be considered for renaming and perhaps even eliminate the term cancer to better frame the discussion and shared decision-making with patients.
How Is Active Surveillance Done
Although the protocol can vary, recommendations for active surveillance generally call for routine PSA tests and prostate biopsies to check for any indication that the cancer might be growing.
For example, patients at Montefiore Health System in New York City get a PSA test every 36 months, at least initially, and an MRI-guided biopsy a year after diagnosis, said Kara Watts, M.D., a urologist at the hospital who specializes in treating prostate cancer but was not involved in the study.
After the initial PSA tests and biopsy, how often they are performed depends largely on the patients particular situation, Dr. Watts explained.
We have a flexible protocol, particularly for people at both ends of the spectrum, she continued. For a man in his 70s and a life expectancy of 510 years , she said, additional PSA tests or biopsies may only be conducted every few years or only if he has symptoms. An otherwise healthy man in his 50s, on the other hand, will usually continue to have PSA tests and MRI-guided biopsies on a schedule similar to the initial protocol.
At the NIH Clinical Center, where Dr. Parnes sees patients, in addition to routine PSA testing, MRI-guided biopsies are used to help inform decisions around whether to pursue active surveillance and as part of the surveillance protocol.
Recommended Reading: What Are The Side Effects Of Having Prostate Removed