Getting The Results Of The Biopsy
Your biopsy samples will be sent to a lab, where they will be looked at with a microscope to see if they contain cancer cells. Getting the results usually takes at least 1 to 3 days, but it can sometimes take longer. The results might be reported as:
- Positive for cancer: Cancer cells were seen in the biopsy samples.
- Negative for cancer: No cancer cells were seen in the biopsy samples.
- Suspicious: Something abnormal was seen, but it might not be cancer.
If the biopsy is negative
If the prostate biopsy results are negative , and the chance that you have prostate cancer isnt very high based on your PSA level and other tests, you might not need any more tests, other than repeat PSA tests sometime later.
But even if many samples are taken, biopsies can still sometimes miss a cancer if none of the biopsy needles pass through it. This is known as a false-negative result. If your doctor still strongly suspects you have prostate cancer , your doctor might suggest:
- Getting other lab tests to help get a better idea of whether or not you might have prostate cancer. Examples of such tests include the Prostate Health Index , 4Kscore test, PCA3 tests , and ConfirmMDx. These tests are discussed in Whats New in Prostate Cancer Research?
- Getting a repeat prostate biopsy. This might include getting additional samples of parts of the prostate not biopsied the first time, or using imaging tests such as MRI to look more closely for abnormal areas to target.
Prostate cancer grade
Gleason score
In The Case Where Aggressive Cancer Is Present A Prostate Mri Can Help Prevent A Missed Diagnosis
When a doctor performs a biopsy, multiple tissue samples are taken at random. While this method technically has the capability to find cancer, it can easily miss the cancerous parts of the prostate. In such cases, a repeat test may be ordered. This means another uncomfortable and expensive procedure, and also doubles a patients already high exposure to infection.
Getting a prostate MRI before a biopsy allows radiologists to identify exact areas in the prostate that are suspicious for cancer so that they can be marked as the best targets for a needle biopsy. Advanced technology can then fuse MRI images with real-time ultrasound to help guide the prostate needle biopsies to the specific areas of concern. This increases the accuracy of diagnoses, reduces the risk of infection from the procedure, and helps accelerate treatment planning for positive patients.
As mentioned above, prostate MRIs are complex images. Getting a second opinion by a subspecialist before undergoing biopsy can further improve the accuracy of the procedure, as well as the overall diagnosis. Benign prostatic hyperplasia , enlarged prostate, and bacterial prostatitis can often be mistaken as prostate cancer. A second opinion can help rule out these conditions before proceeding with treatment.
How accurate is MRI in diagnosing prostate cancer?
CONNECT WITH A SPECIALIST
What Does An Mri Scan Involve
MRI scans require the removal of all metal factors including jewelry, zips and buttons internal implants such as metal plating or pacemakers could make MRI scanning impossible. Initial discussions about a patients general health will account for such factors, as well as other conditions such as claustrophobia are known to impact on the MRI procedure.
To clarify scan images, a small amount of dye may be injected into the patients bloodstream those who are pregnant or suffering from allergies, asthma or kidney related illness should include this information in the questionnaire provided. Patients may be required to drink a large amount of water and to lie still on a table until the scan is complete, usually around forty minutes or less.
Also Check: Is Dark Chocolate Good For The Prostate
Ok So A Prostate Mri Is Pretty Important
Yes! The mpMRI and PI-RADS score will give Dr. Bevan-Thomas detailed information that will help determine whether you need a prostate biopsy and if there is an area to target for the fusion biopsy. Before mpMRI technology, if a doctor suspected cancer, patients would go straight to an ultrasound-guided prostate biopsy. With the mpMRI, if your PI-RADS score is low meaning low risk for intermediate or high-grade cancer you may not need a biopsy.
A multiparametric prostate MRI is accurate for finding intermediate and high-grade cancers around 85% of the time. A negative MRI does not always mean that a biopsy is not recommended, but it is extremely helpful in finding lesions to target. There is roughly a 15% chance of having a focus of cancer not seen on the MRI, so other parameters are often used in terms of recommending a course of action. Ultrasound continues to have a role in diagnosing many prostate cancers.
But if your PI-RADS score is higher, you may need a fusion biopsy. In this case, the multiparametric MRI results will give Dr. B-T an exact location to target. By fusing the ultrasound image with the MRI image, a specific area can be targeted with a needle biopsy.
How Should I Prepare
Your MRI exam may use anendorectal coil, a thin wire covered with a latex balloon. The doctor places the coil a short distance into the rectum. The rectum is located immediately behind and up against the prostate. Placing the coil into the rectum so close to the prostate helps generate more detailed images. It also enables yourradiologist to perform magnetic resonance spectroscopy. MR spectroscopy can provide additional information on the chemical makeup of cells in the prostate. Additionally, prostate MRI may examine water molecule motion and blood flow within the prostate to help differentiate between diseased and normal prostate tissue.
Your doctor will typically use an endorectal coil with low-field MRI magnets if you have a metal orthopedic implant. Metal implants may interfere with imaging when using a high-field magnet MRI. The doctor will typically not use an endorectal coil with high-field MRI units.
You will need to change into a hospital gown. This is to prevent artifacts appearing on the final images and to comply with safety regulations related to the strong magnetic field.
Guidelines about eating and drinking before an MRI vary between specific exams and facilities. Take food and medications as usual unless your doctor tells you otherwise.
If you have claustrophobia or anxiety, ask your doctor to prescribe a mild sedative prior to the date of your exam.
- some cochlear implants
- some older cardiac defibrillators and pacemakers
- vagal nerve stimulators
Don’t Miss: How Long Can You Live With Gleason 6 Prostate Cancer
Ways Prostate Mri Can Improve Diagnostic Accuracy
This year, the American Cancer Society estimates that nearly 175,000 men will be diagnosed with prostate cancer . But despite being the most common cancer among men, excluding skin cancer, theres no one size fits all solution for determining prostate cancer risk.
So how can men find a balance between avoiding the drawbacks of screening, while also ensuring nothing goes undetected? Prostate MRI, combined with a second opinion, could be the answer.
Prostate Adenocarcinoma With A Large Right Seminal Vesicular Cyst
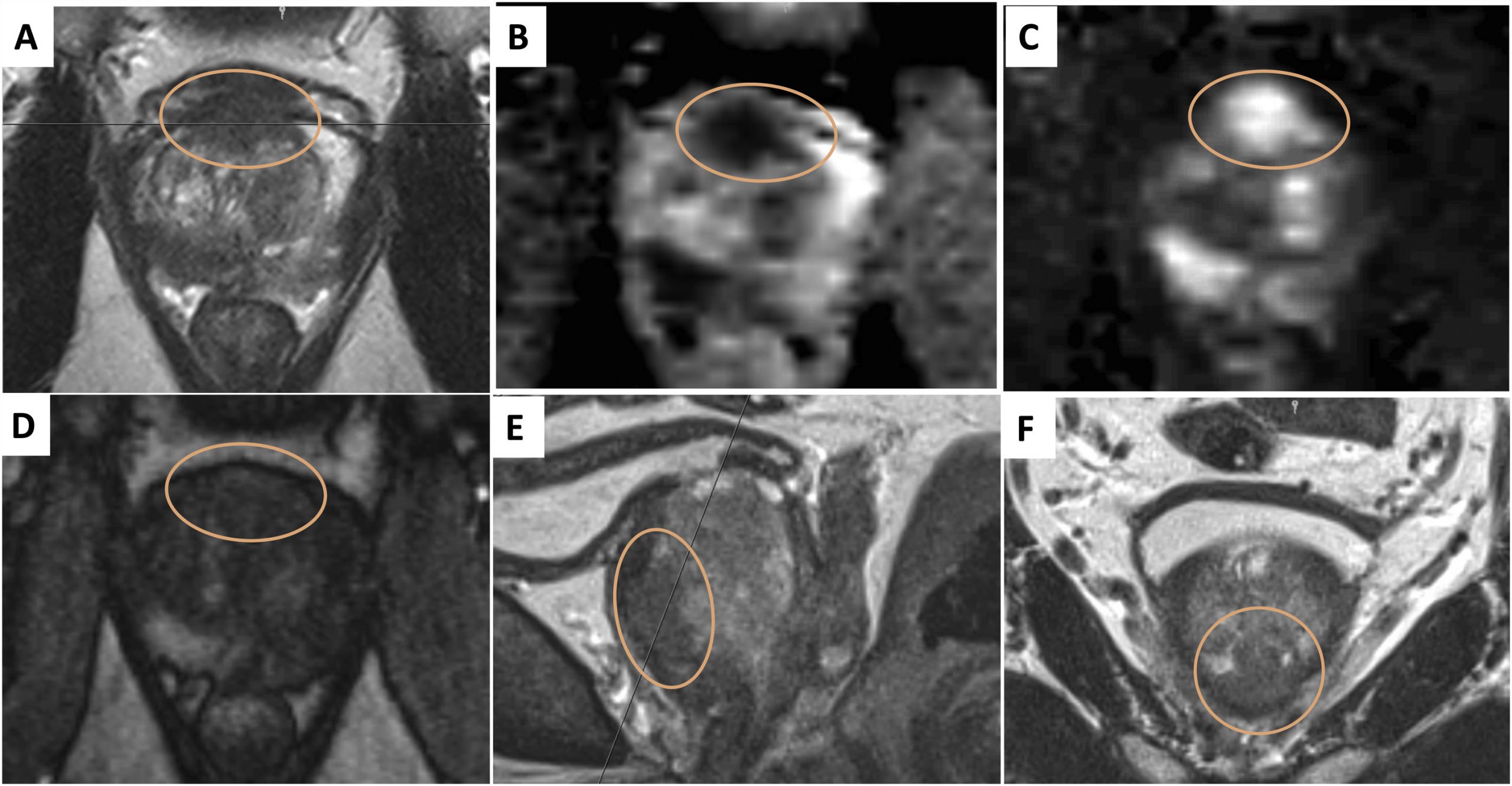
Malignancy associated with cystic lesions of the prostate is rare. Both benign and malignant prostate neoplasms may contain cystic components. In this case, histology post-radical prostatectomy revealed Gleason score 5+4=9 prostate adenocarcinoma with involvement of both seminal vesicles. The large right-sided cystic structure was identified as arising from the right seminal vesicle which was invaded by the adenocarcinoma, leading to obstruction and distention. Due to the cystic nature of the lesion, there was no avidity within it on PSMA PET. When the cystic component grows as large as in this case, it can be associated with lower urinary tract symptoms. Other tumours of the prostate gland which can have cystic components include papillary cystadenocarcinoma and combined transitional cell/ adenocarcinoma and leiomyoma or liposarcoma can also show this although are much rarer . The aspirate of the cystic component is usually haemorrhagic and contains malignant cells with a high concentration of prostate specific antigen and Y-seminoprotein .
Fig. 9
Cystic prostate adenocarcinomaac Axial T2W images demonstrate multiple large high T2 signal lesions in keeping with cysts surrounding the prostate with small fluid-fluid levels likely due to internal haemorrhage
You May Like: Agent Orange Prostate Cancer Compensation
Having The Mpmri Scan
You need to lie as still as possible. The scan is painless but it can be uncomfortable to stay still. Tell the radiographer if you’re getting stiff and need to move.
The scan usually takes up to 10 minutes.
Once youre in the right position on the couch, your radiographer leaves the room. They can see you on a TV screen or through a window at all times from the control room. You can talk to each other during the scan, usually through an intercom.
The couch moves through the MRI scanner. It takes pictures as you move through it. Your radiographer might ask you to hold your breath at times.
The scanner makes a very loud clanging sound throughout the scan. You wear headphones to protect your hearing. You can also listen to music. Keeping your eyes closed can help.
This 1 minute video shows you what happens when you have an MRI scan.
Positron Emission Tomography Scan
A PET scan is similar to a bone scan, in that a slightly radioactive substance is injected into the blood, which can then be detected with a special camera. But PET scans use different tracers that collect mainly in cancer cells. The most common tracer for standard PET scans is FDG, which is a type of sugar. Unfortunately, this type of PET scan isnt very useful in finding prostate cancer cells in the body.
However, newer tracers, such as fluciclovine F18, sodium fluoride F18, and choline C11, have been found to be better at detecting prostate cancer cells.
Other newer tracers, such as Ga 68 PSMA-11, 18F-DCFPyl , and Ga 68 gozetotide , attach to prostate-specific membrane antigen , a protein that is often found in large amounts on prostate cancer cells. Tests using these types of tracers are sometimes referred to as PSMA PET scans.
These newer types of PET scans are most often used if its not clear if prostate cancer has spread. For example, one of these tests might be done if the results of a bone scan arent clear, or if a man has a rising PSA level after initial treatment but its not clear where the cancer is in the body. PSMA PET scans can also be used to help determine if the cancer can be treated with a radiopharmaceutical that targets PSMA.
Doctors are still learning about the best ways to use these newer types of PET scans, and some of them might not be available yet in all imaging centers.
You May Like: How Many Cases Of Prostate Cancer Per Year
Why Do You Need A Urologist With Mpmri Experience
Dr. Bevan-Thomas has experience with the most advanced technology including the mpMRI dating back to 2012. He was the first urologist in Arlington, Texas, to use the prostate MRI and fusion technology.
Why is that experience important? Because state-of-the-art equipment has a better chance of finding aggressive prostate cancer earlier in the disease process.
Dr. B-T will also support you throughout the process. He will review your MRI results with you prior to scheduling a biopsy. He will be sure that you understand the need for the biopsy, how the procedure is done, and the pathology results. He will then guide you through your treatment options, and together you will decide on the best course of treatment.
Preparing For Your Mpmri Scan
Before you go to your appointment, or when you arrive, you fill in a safety checklist. This asks about:
- any operations youve had
- whether you have any metal implants or other metals in your body
An MRI scan uses strong magnetism which could affect any metal in your body. This includes:
- pacemakers or an implantable defibrillator
- surgical clips, pins or plates
- cochlear implants
- metal fragments anywhere in your body for example from an injury, dental fillings and bridges
You can still have an MRI scan if you have some metals in your body, but your doctor and radiographer decide if its safe for you. Tell the scanner staff about any metals in your body.
Some people feel claustrophobic or closed in when theyre having an MRI scan. Contact the department before your test if youre likely to feel like this. The hospital staff can take extra care to make sure youre comfortable and that you understand whats going on. Your doctor can give you medicine to help you relax if you need to.
The radiographers let you know whether you need to empty your bowels of any poo or gas before having the scan. In some departments, you might be given an enema. An enema is a liquid filled pouch that has a nozzle that you can put into your back passage and it helps to empty your bowels.
Also Check: Enlarged Prostate Blood In Urine
How Is The Procedure Performed
MRI exams may be done on an outpatient basis.
The technologist will position you on the moveable exam table. They may use straps and bolsters to help you stay still and maintain your position.
The technologist may place devices that contain coils capable of sending and receiving radio waves around or next to the area of the body under examination.
MRI exams generally include multiple runs , some of which may last several minutes. Each run will create a different set of noises.
Your exam may use an endorectal coil. If so, a nurse or doctor will place a disposable cover over the coil. They will lubricate the assembly and insert the coil a short distance into your rectum. After insertion, the doctor inflates the circular balloon that sits around the coil and holds it in place during the exam. When the exam is complete, the doctor deflates the balloon and removes the coil.
If your exam uses a contrast material, a doctor, nurse, or technologist will insert an intravenous catheter into a vein in your hand or arm. They will use this IV to inject the contrast material.
You will be placed into the magnet of the MRI unit. The technologist will perform the exam while working at a computer outside of the room. You will be able to talk to the technologist via an intercom.
If your exam uses a contrast material, the technologist will inject it into the intravenous line after an initial series of scans. They will take more images during or following the injection.
Why Shouldnt I Have The Assessment
The MRI procedure is loud and noisy mild side effects include feeling warm, queasy, skin rashes, headaches and dizziness. Despite these factors, patients are usually allowed to return home on the same day and resume their usual activities Note that this is impacted if patients have undergone sedation during their scan.
Patients can discuss sedation with their doctors far ahead of their scan date. Patients who have had a sedative will need to be accompanied for 24 hours following their scan and should avoid driving or operating heavy machinery.
Patients with metal implants or similar may require an initial X-ray. Patients with metal plates, artificial joints, pacemakers, nerve stimulators, dental bridges, surgical wires, medical screws or rods, prosthetic heart valves, some tattoo inks, intrauterine devices, implantable cardioverter-defibrillators, penile implants, eye, cochlear or drug pump implants, tubal ligation or brain aneurysm clips may be precluded.
Read Also: Where Does Prostate Cancer Metastasis To First
Undifferentiated Pleomorphic Sarcoma Of The Spermatic Cord
Primary spermatic cord tumours are rare and clinically significant urologic lesions which may be encountered while examining the prostate on imaging. Table highlights common benign and malignant neoplasms of the spermatic cord that the radiologist should be aware of.
Fig. 17
UPS of the spermatic corda Coronal T1 fat sat post-contrast and b axial T2 fat sat images show a large heterogeneously enhancing high T1 and T2 signal mass within the left inguinal canal and scrotum . c Axial DWI and d ADC images demonstrate a predominantly solid mass with restricted diffusion in keeping with necrosis or cystic change within
Prostate Tb Abscess In A Patient With Bladder Tcc After Intravesical Instillation Of Bcg
Adjuvant intra-vesical immunotherapy with BCG for bladder transitional cell carcinoma can lead to a rare complication of tuberculous infection in the prostate via haematogenous spread and direct extension which can cause a prostate abscess .
The granulomatous reaction that occurs in prostate tissues following the topical instillations of BCG after resection of bladder cancer can present MRI features similar to prostate cancer . It appears as an ill-defined region with moderate contrast enhancement, diffusion restriction and very low ADC values due to the high cellular density. These are a well-recognised cause of false positive MRI. However, frank abscess formation related to BCG is rare with only a handful of cases described in the literature. History and biochemical correlation are important to consider this as a differential diagnosis and a biopsy may be needed to confirm .
Fig. 7
Prostate abscessa, b Axial T2W images show left lateral bladder wall thickening and heterogeneous but predominantly low T2 signal in the left prostate , respectively. c Post-contrast, the lesion demonstrates strong peripheral contrast enhancement and on DWI/ ADC in d, e, respectively, the central element of the left prostate lesion shows restricted diffusion with a very low ADC value
You May Like: What Foods Can Prevent Prostate Cancer
Use In Men Who Might Have Prostate Cancer
The PSA blood test is used mainly to screen for prostate cancer in men without symptoms. Its also one of the first tests done in men who have symptoms that might be caused by prostate cancer.
PSA in the blood is measured in units called nanograms per milliliter . The chance of having prostate cancer goes up as the PSA level goes up, but there is no set cutoff point that can tell for sure if a man does or doesnt have prostate cancer. Many doctors use a PSA cutoff point of 4 ng/mL or higher when deciding if a man might need further testing, while others might recommend it starting at a lower level, such as 2.5 or 3.
- Most men without prostate cancer have PSA levels under 4 ng/mL of blood. Still, a level below 4 is not a guarantee that a man doesnt have cancer.
- Men with a PSA level between 4 and 10 have about a 1 in 4 chance of having prostate cancer.
- If the PSA is more than 10, the chance of having prostate cancer is over 50%.
If your PSA level is high, you might need further tests to look for prostate cancer.
To learn more about how the PSA test is used to look for cancer, including factors that can affect PSA levels, special types of PSA tests, and what the next steps might be if you have an abnormal PSA level, see Screening Tests for Prostate Cancer.