> > > All Natural Technique Fixes Enlarged Prostate Watch Here< <
Surgical procedures to remove the diseased prostate are usually necessary. Surgical procedures are not always necessary. If the disease is caused by bacterial infections, a doctor can treat the symptoms using alpha-blockers or surgery. Physical therapy, relaxation exercises, and warm baths are all recommended. A physician may also prescribe antibiotics to cure the infection. A bacterial infection can also cause a recurrence of the condition.
An enlarged prostate can be uncomfortable for both men and women. Some of the symptoms of an enlarged male reproductive organ include a weakened urine stream, urgent need to urinate, and urinary tract infections. BPH can also cause damage to the kidneys. A sudden inability to urinate can be life-threatening, as it can lead to bladder and kidney damage. Unfortunately, most men with enlarged prostrates put up with the symptoms for years before they seek treatment. However, many of the men with symptoms finally decide to go to a doctor for proper gynecological evaluation and to begin enlarged prostatic therapy.
Arent Nomograms More Predictive Of Prognosis
Nomograms are mathematical models used to attempt to individualize prognosis for individual patients. They use the PSA, stage and grade to predict results of various treatments. But nomograms are only as good as the data that is entered into them. For example, the current MSKCC nomogram for brachytherapy is VERY outdated. It includes patients Dr. Grimm treated from 1988-1990, but not his more recent patients with modern techniques. This data is incorrectly compared to updated surgical data. It is well recognized that within all treatment regimens the results have improved over the past 15 years primarily because the patients are diagnosed earlier and that the treatments are improved. Dr. Steven Frank at MD Anderson reported on the expected results of the MSKCC nomogram for brachytherapy compared to modern brachytherapy results and found the nomogram extremely inaccurate. Article
Thus, using the current MSKCC nomogram to compare surgical versus brachytherapy outcomes is extremely misleading. Therefore, rather than using a dated nomogram to decide on treatment, instead, look at modern results. Prostate Cancer Results Study Group
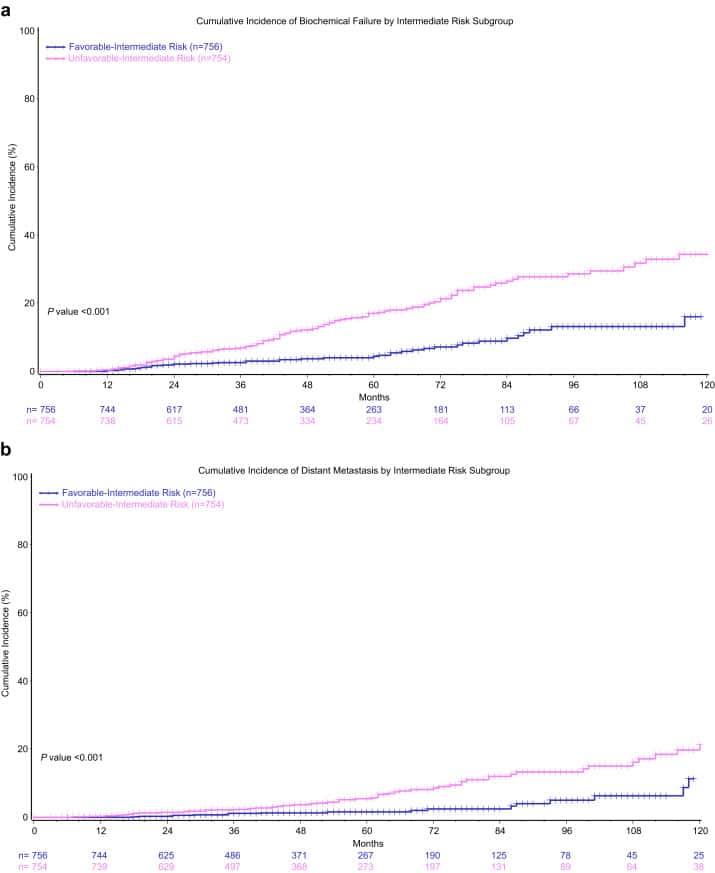
What You Need To Know About The Prostate Nccn Favorable Intermediate Risk Prostate Cancer
A enlarged prostate can also cause blockages in the urethra. A blocked urethra can also damage the kidneys. A patient suffering from an enlargement of the prostate may have pain in his lower abdomen and genitals. If pain is present, a digital rectal examination will reveal hard areas. A doctor may prescribe surgery or perform an endoscopic procedure. If the enlarged prostate is not completely removed, it will shrink.
While the size of an enlarged prostate will influence the extent of urinary symptoms, men may experience a range of urinary symptoms. Some men have minimal or no symptoms at all. Some men will have a very enlarged prostate, whereas others will have a mild enlargement. Generally, the symptoms can stabilize over time. Some men may have an enlarged prostate but not notice it. If they have an enlarged colon, their physician can perform a TURP procedure.
Recommended Reading: Best Over The Counter For Enlarged Prostate
American Society Of Clinical Oncology/cancer Care Ontario Recommendations
ASCO and CCO released a joint clinical practice guideline for treatment of men with metastatic CRPC in 2014. The guideline recommendations include the following :
-
Pharmacologic androgen deprivation therapy should be continued indefinitely
-
Offer patients one of three treatment optionsabiraterone/prednisone, enzalutamide, or radium-223 in addition to hormone deprivation
-
When considering chemotherapy, docetaxel/prednisone should be an option but side effects must be discussed
-
Offer cabazitaxel to men whose disease worsens even if docetaxel has been tried, but again, discuss side effects
-
Offer sipuleucel-T to men with no symptoms or minimal symptoms of cancer
-
Offer mitoxantrone, but include a discussion of the drug’s limited clinical benefit and side effect risk
-
Offer ketoconazole or the anti-androgen therapies bicalutamide, flutamide or nilutamide but discuss the limited clinical benefit for these three medications
-
Do not offer the drugs bevacizumab , estramustine, or sunitinib
-
Begin discussion of palliative care early on while discussing treatment options
National Comprehensive Cancer Network Recommendations
The NCCN guidelines for prostate cancer include treatment recommendations for CRPC based on the presence or absence of visceral metastases. For the most part, these recommendations are based on high-level evidence and are supported by uniform NCCN consensus .
CRPC without distant metastasis
-
Enrollment in clinical trial is preferred
-
Observation is acceptable
-
Secondary hormone therapy can be considered for patients with prostate-specific antigen doubling < 10 months anti-androgen therapy is acceptable for patients who previously received medical or surgical castration, ketoconazole, corticosteroids, diethylstilbestrol or other estrogens
CRPC with bone metastases
Measures to promote bone health include the following:
-
Zoledronic acid or denosumab
-
Avoidance of invasive dental surgery during treatment
-
Calcium and vitamin D supplements to prevent hypocalcemia during treatment
Radium-233 can be used to treat symptomatic bone metastases without visceral metastases.
Metastatic CRPC with no visceral metastases
-
Sipuleucel-T for asymptomatic or minimally symptomatic patients
-
Abiraterone plus prednisone or enzalutamide for asymptomatic patients
-
Docetaxel with prednisone for symptomatic patients may also be considered in a symptomatic patients with signs of rapid progression
-
Radium-233 for symptomatic patients
-
Secondary hormone therapy or enrollment in clinical trial may be considered
Metastatic CRPC with visceral metastases
-
Other secondary hormone therapy
-
Best supportive care
Don’t Miss: Prostate Massage Therapy For Erectile Dysfunction
Other Ways To Measure Risk Of Prostate Cancer Growing And Spreading
In addition to the risk groups above, doctors are still learning about the best use of other types of tests and prognostic models to help decide the most effective treatment options for someone. If your doctor suggests using one of these ways to help determine your treatment options, have them explain what it can tell you, as well as how accurate its likely to be.
About Dr Dan Sperling
Dan Sperling, MD, DABR, is a board certified radiologist who is globally recognized as a leader in multiparametric MRI for the detection and diagnosis of a range of disease conditions. As Medical Director of the Sperling Prostate Center, Sperling Medical Group and Sperling Neurosurgery Associates, he and his team are on the leading edge of significant change in medical practice. He is the co-author of the new patient book Redefining Prostate Cancer, and is a contributing author on over 25 published studies. For more information, contact the Sperling Prostate Center.
Search the spc blog
You May Like: End Of Life Prostate Cancer Symptoms
Nomograms And Predictive Models
Optimal treatment of prostate cancer requires assessment of risk: how likely is a given cancer to be confined to the prostate or to spread to the regional lymph nodes? How likely is the cancer to progress or metastasize after treatment? How likely is salvage with adjuvant radiation after an unsuccessful radical prostatectomy? Prostate cancers are best characterized by clinical stage determined based on DRE, Gleason score in the biopsy specimen, and serum PSA level. Imaging studies have been investigated intensively but have not been accepted as essential adjuncts to staging.
Predicting prognosis is essential for patient decision-making, treatment selection, and adjuvant therapy. These guidelines incorporate a risk stratification scheme that uses a minimum of stage, grade, and PSA to assign patients to risk groups. These risk groups are used to select the appropriate options that should be considered for treatment and to predict the probability of biochemical failure after definitive local therapy.7 This risk group stratification has been published widely and validated, and provides a better basis for treatment recommendations than clinical stage alone.8,9
Can Adt Compensate For Dose Escalation
The Prostate Cancer Study III examined the addition of ADT to SDRT and DERT in intermediate-risk patients . The preliminary results of this trial have now been published in abstract form. A total of 600 patients were enrolled. Intermediate-risk prostate cancer was defined as T1/T2 disease, GS 6, PSA level 1020 ng/mL or T1/T2 disease, GS of 7, PSA level 20 ng/mL. Patients were randomly assigned to one of three arms: 6 months of ADT plus 70 Gy to the prostate , 6 months of ADT plus 76 Gy , or 76 Gy alone . ADT consisted of bicalutamide and goserelin for 6 months. RT was delivered using a 3D conformal technique and started 4 months after the beginning of ADT. Median follow-up was 6.75 years. Primary endpoints were biochemical failure and disease-free survival . Secondary endpoints included OS, as well as hormonal and radiation-related toxicities. Biochemical failure was defined as 2 ng/mL above the PSA nadir.
Don’t Miss: Incontinence After Robotic Prostate Surgery
Psa Response And Biochemical Control
The overall 5-year actuarial FFBF for the whole group was 92.7% . Six patients out of the entire cohort of 142 patients, all in the low dose group, experienced BF two were high risk, three intermediate risk, and one low risk. The low-dose and high-dose groups median PSA nadirs were 0.3 and 0.1 ng/mL, respectively. Five year actuarial FFBF was 100% for the high dose group and 93.75% for the low dose group, p= 0.05, hazard ratio of 11.0 for low compared to high dose .
Table 2. Freedom from biochemical failure stratified by risk and descriptive statistics.
Figure 2. Years of freedom from biochemical failure by dose for all patients.
Figure 3. Years of freedom from biochemical failure by Gleason score for all patients.
Multivariate analysis evaluated the most significant factors in univariate analysis including risk stratification groups, GS, and dose. GS and dose were the most predictive factors in multivariate analysis but did not reach statistical significance at the p< 0.05 level. Of note, with only six failures, we only have the power to detect a single significant predictor of failure in the multivariate analysis.
Modifying Risk Level Classification
The new millennium brought changes as 1) more epidemiological and demographic data accumulated, 2) the nature of PCa was better understood, and 3) sub-radical therapies such as focal ablation or hemi-ablation were developed to offer comparable cancer control but with far fewer side effect risks. A need was seen to add qualifiers to low risk PCa. Thus, the National Comprehensive Cancer Network subdivided this category into very-low and low-risk types to help doctors and patients determine for which men Active Surveillance or a sub-radical treatment would be safe choice.
The NCCN system did not qualify intermediate risk PCa. It differs a bit from DAmico, defining it as stage T2b or T2c, Gleason score of 7, and PSA level 10-20 ng/mL. However, by 2015 it was clear that this category was the largest group of PCa cases with the most heterogeneous disease characteristics. There was a wide range of PCa-specific mortality as well as biochemical or clinical recurrence after radical treatment by prostatectomy, beam radiation, and brachytherapy . Studies began to show that all Gleason 7 is not created equal men with Gleason 3+4=7 had better outcomes than those with Gleason 4+3=7, Therefore, In order to better understand this risk group, new classification systems have been proposed that help reduce its heterogeneity by subdividing men with intermediate-risk prostate cancer into favorable and unfavorable subgroups.
Also Check: Elevated Prostate Levels Blood Test
I Have Heard That Other Factors May Be Included When Evaluating Treatment
Yes, other factors such as the number of biopsies and the presence of Gleason Score 7 versus a Gleason Score may influence the treatment decision. The number of + biopsies is also strongly predictive of outcomes but not typically part of the risk grouping systems. An example would be a person with a multiple + biopsies Gleason 7. His cancer would be considered a High Intermediate Risk and require a combination of External Beam and radiation while another patient with only a few + biopsies could be a Low Intermediate Risk patient and be a good candidate for an implant alone. These factors should be discussed with you doctor.
©2013 Prostate Cancer Center of Seattle | All Rights Reserved | P 1.877.330.7722 OR 206.453.2992 |
Favorable Vs Unfavorable Intermediate

The DAmico risk groups, initially published in 1998, were designed to stratify patients according to the likelihood of biochemical recurrencefree survival after radical prostatectomy or radiotherapy. The current NCCN guidelines are a slight modification of this classification system. However, in 2005 an International Society of Urological Pathology conference was held in order to reach a consensus regarding the grading of prostate cancer. A consensus statement was published in 2005, and as a result of the adoption of this new grading system, the reporting of secondary pattern Gleason grade 4 disease became more prevalent. Several investigators have reported on their observation of grade migration from GS 3+3 to GS 3+4 . This grade migration could cause a number of men who previously would have been categorized as low-risk to be assigned to the NCCN intermediate-risk category because of their GS, thereby improving the prognosis of both groups . Thus, it has been hypothesized that some men with GS 3+4 intermediate-risk prostate cancer may have a low risk of PCSM and higher rates of overall survival , similar to what is seen in patients with low-risk prostate cancer.
Only one intermediate-risk factor .
GS of 3+4=7 or less.
Less than 50% of biopsy cores positive for cancer.
Those who were classified as unfavorable could have any of the following:
More than one intermediate-risk factor.
GS of 4+3=7.
Greater than 50% positive biopsy cores.
Read Also: Prostate Cancer Surgery Or Radiation Which Is Better
Patient And Treatment Characteristics
One hundred and forty-two consecutive patients were analyzed with pretreatment and treatment factors described in Table 1. NCCN risk groups are depicted in Table 1 with either three or five strata . Androgen deprivation therapy in the form of luteinizing hormone-releasing hormone agonist was used in 28.2% of patients . The use of ADT was dependent on individual urologist and radiation oncologist preference. Selected very low and low risk patients received ADT to shrink the prostate before SBRT.
Table 1. Patient and tumor characteristics.
Patients who received 35 or 36.25 Gy were termed the low-dose group and those who received 37.5 Gy the high-dose group. Most patients received their treatment over 58 days. The remainder completed treatment between 9 and 19 days with one non-compliant patient receiving his final fraction several weeks later, all due to poor adherence to their schedule. Treatment was delivered with an average of 187 non-coplanar beams. X-ray images were taken every three to five beams to track the prostates movement.
European Society Of Medical Oncology
The 2015 ESMO guidelines recommend watchful waiting with delayed hormone therapy as an option for localized disease or as an alternative for men with localized or locally advanced disease who are unwilling or unsuited for radical therapy.
Other recommended treatment options include :
-
Active surveillance for men with low-risk disease
-
Radical prostatectomy or radiotherapy for men with low- or intermediate-risk disease
-
Primary androgen deprivation therapy alone is not recommended for treatment of non-metastatic disease
-
For patients with high-risk or locally advanced prostate cancer, external beam RT plus hormone treatment or RP plus pelvic lymphadenectomy
Also Check: Preparation For Prostate Mri Scan
> > > This Simple Morning Test Will Fix Your Prostate
Another type of prostate issue is chronic prostatitis, or chronic pelvic pain syndrome. This condition causes pain in the lower back and groin area, and may cause urinary retention. Symptoms include leaking and discomfort. In severe cases, a catheter may be required to relieve the symptoms. If the problem is unresponsive to other treatments, your doctor may suggest a surgical procedure. If these do not work, your symptoms could progress and become chronic.
An acute bacterial infection can cause a burning sensation. Inflammation of the prostate can affect the bladder and result in discomfort and other symptoms. This is the most common urinary tract problem in men under 50, and the third most common in men over 65. The symptoms of acute bacterial prostatitis are similar to those of CPPS. Patients may experience a fever or chills as a result of the infection.
> > > One Crazy Prostate Trick All Men Over 40 Should Try
Symptomatic treatment of an enlarged prostate usually involves a combination of medication and lifestyle changes. A diet rich in fruits and vegetables may be the best option if you suffer from chronic urination. It will help the body adjust to the increased size of the prostate. Also, taking regular urination intervals will help retrain the bladder to function properly. Inactivity also contributes to urine retention, and cold temperatures can increase the urge to urinate.
Invasive treatment of enlarged prostate includes medication that relieves the pressure on the urethra and bladder. However, if the condition is severe, it may require surgical intervention. If treatment is not successful, the enlarged prostate can become a potentially life-threatening disease. As the hormone levels in the body change, the enlarged prostate can lead to various complications, including urinary retention and even cancer. This is why it is critical to see a doctor for further evaluation.
You May Like: How To Stimulate Your Prostate
Bisphosphonates And Prostate Cancer
In men with castration-recurrent prostate cancer and bone metastases, zoledronic acid every 3 to 4 weeks is recommended to prevent disease-related skeletal complications, including pathologic fractures, spinal cord compression, surgery, or RT to bone . Other bisphosphonates are not known to be effective for preventing disease-related skeletal complications.
In a pivotal multicenter study, 643 men with castration-recurrent prostate cancer and asymptomatic or minimally symptomatic bone metastases were assigned randomly to intravenous zoledronic acid or placebo.170 All men continued ADT throughout the study and received additional antineoplastic therapy at the discretion of the investigator. The primary study end point was the proportion of men who experienced one or more skeletal-related event by 15 months. Adverse renal events prompted 2 study amendments. In the first amendment, the infusion time for zoledronic acid was increased from 5 to 15 minutes. In the second amendment, the zoledronic dose in the 8-mg treatment group was reduced to 4 mg, serum creatinine monitoring was implemented before each dose, and the primary efficacy assessment became the comparison of the 4-mg group versus placebo.