Role Of Multiparametric Mri In Prostate Biopsy
Recent advances in imaging techniques including multi-parametric MRI have enabled non-invasive assessment of the prostate for suspicious lesions. mpMRI is a MRI technique that involves conjunctive use of multiple MRI sequences to more accurately characterize lesions. mpMRI reporting has been standardized by the European Society of Urogenital Radiology through the development of the Prostate Imaging Reporting and Data System , which was updated to version 2 in 2015. Park et al. demonstrated in a retrospective study of patients who underwent both mpMRI and radical prostatectomy that PI-RADS2 score greater than 4 was 77% and 73.8% sensitive for detection of clinically significant cancer for each of the two readers with excellent inter-reader agreement. A recent meta-analysis by Woo et al. assessing the diagnostic performance of PI-RADS2 included 3857 patients and found a pooled sensitivity of 89% and specificity of 73% for cancer detection. Lesions with PI-RADS2 scores of 4 or 5 indicate a high or very high likelihood of clinically significant cancer, respectively, and should be biopsied.
Currently, the AUA suggests that mpMRI-based screening should be considered purely investigational and awaiting results of PROMIS and PRECISION trials before making a statement on the change in adoption, but it will be intriguing to see how rapidly it will change clinical practice.
Comparison Of Mri/us Fusion
Emerging evidence has shown that multiparametric magnetic resonance imaging as an innovative guidance approach for prostate biopsy increases the detection rate of prostate cancer. Hence, we also reviewed RCT studies comparing MRI/US fusion-guided biopsy and traditional systematic transrectal biopsy. This review was not included in our meta-analysis as our aim was to assess the diagnosis accuracy of transperineal and transrectal biopsy.
In the other RCT study by Kasivisvanathan et al. , the authors randomized 252 patients in an MRI-targeted group and 248 patients in a standard biopsy group. In the MRI-targeted group, 71 patients did not undergo prostate biopsy because of negative MRI results. The patients in the MRI-targeted group received a 4-core MRI/US fusion biopsy and the patients in the standard biopsy group received a systematic transrectal biopsy. Clinically significant prostate cancer was diagnosed in 38% patients in the MRI-targeted group and 26% patients in the standard biopsy group. The detection rate of the MRI-targeted biopsy is significantly higher than the traditional biopsy.
Located In Bellingham Wa
When youre experiencing prostate symptoms that might indicate cancer, your urologist may recommend a prostate biopsy. At Pacific Northwest Urology Specialists in Bellingham, Washington, the skilled team offers the most advanced specialized care for the male reproductive system, including prostate cancer screenings, prostate biopsy, and prostate treatments. If youre looking for the highest quality prostate care, call Pacific Northwest Urology Specialists or schedule an appointment online today.
Also Check: Ablation Treatment For Prostate Cancer
Comparison Of Pain Scores Between Groups
Our study showed that patients reported a higher pain score at insertion of the TRUS probe in the PPNB group compared to the CB group, though this was not statistically significant. Similarly, Urabe et al. reported a statistically significant higher average pain score at the point of probe insertion for PPNB+IRLA group compared to the CB+IRLA group. This is probably due to the fact that insertion of the TRUS probe precedes the administration of the PPNB in the PPNB group, while the administration of CB preceded probe insertion which also had the effect of relaxing the anal sphincter. This point may confer an advantage on CB over PPNB as analgesia for prostate biopsy.
There was no significant difference in the experience of pain at administration of block in our study. However, Urabe et al. reported a significantly higher average pain score of 2.9±2.1 in the CB+IRLA group than in the PPNB+IRLA group at the moment of administering the analgesia. This could have been as a result of the fact that in their study, IRLA was instilled prior to the administration of PPNB.
Table 4 Protocols, findings and conclusions of studies that compared CB with PPNB
Recommended Reading: How To Stop Leaking After Prostate Surgery
Prostate Cancer Risk Groups
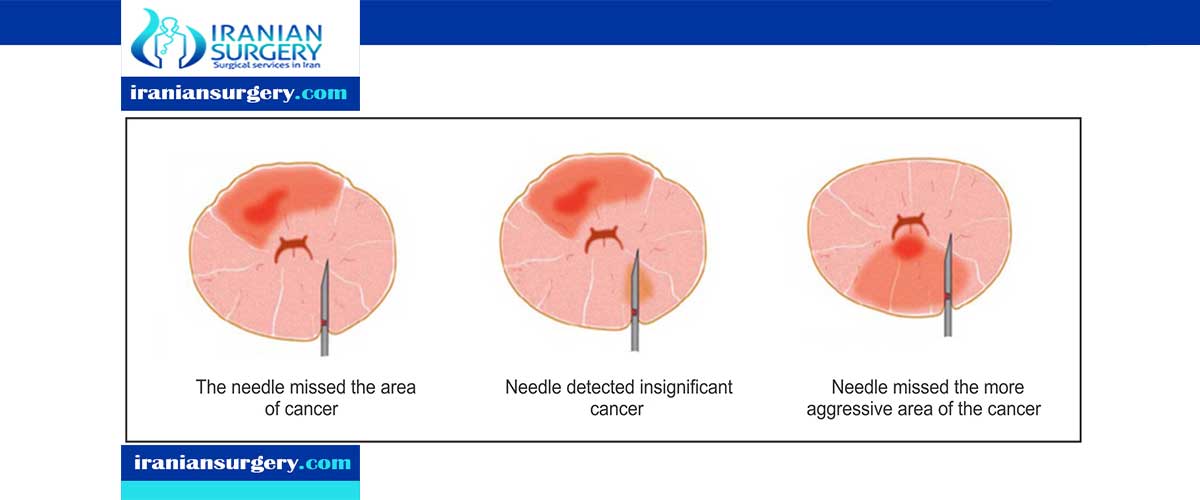
In addition to stage, doctors may use other prognostic factors to help plan the best treatment and predict how successful treatment will be. Examples of these include the National Comprehensive Cancer Network risk group categories and the Cancer of the Prostate Risk Assessment risk score from University of California, San Francisco.
Information about the cancers stage and other prognostic factors will help the doctor recommend a specific treatment plan. The next section in this guide is Types of Treatment. Use the menu to choose a different section to read in this guide.
You May Like: After Effects Of Radiation For Prostate Cancer
Treating Blood In Semen
The treatment your GP or urologist recommends will depend on what they think is the underlying reason for the blood in your semen.
In many cases, particularly if you have no other symptoms or the blood in your semen was an isolated incident, no treatment is necessary and the problem will usually resolve on its own.
If a clear reason is identified, the treatment youre offered will depend on the specific cause.
For example, you may be given antibiotics to treat an infection and cysts may need to be drained with a needle.
If theres a serious underlying cause, such as a blood clotting disorder or cancer, youll be referred to an appropriate specialist for any necessary treatment.
Page last reviewed: 18 July 2019 Next review due: 18 July 2022
Koelis Technology For Prostate Cancer Biopsies
For over a decade KOELIS® has assisted urologists and radiologists from around the world in their routine clinical practice providing the latest technology. In order to bring personalized answers to every patient in the respect of their quality of life, weve developed KOELIS Trinity® the first image-based cartographer. This system allows physicians to perform targeted transperineal or transrectal MRI/US fusion-guided biopsies under local or general anesthesia.
Quality management in patient diagnosis
It is equipped with the exclusive Organ-Based Tracking Fusion® technology which enhances the accuracy of the biopsy. Without changing the usual clinical practices, this technique brings an increased quality control over biopsy localizations. A precise, individual prostate biopsy mapping is a value for the accurate diagnosis and the further management of each patient.
To locate a clinic equipped with our solutions: Discover our interactive map.
Recommended Reading: Super Beta Prostate Where To Buy
Is Having Blood In My Semen Dangerous
Although its frightening to see blood in your semen, its rarely a symptom of a major health problem. A single episode of blood in your semen is usually not a sign of cancer. However, you may still want to see your healthcare provider to be reassured, to fully discuss this symptom and get an exam and perhaps other tests if your provider thinks theyre needed.
What Is An Mri
What makes an MRI different from other medical imaging techniques like X-rays and CT scans? X-rays take projection images of hard tissues like bones, while CT scans take images of both hard bony tissues and soft tissue. Both systems use ionizing radiation, which passes through the body to create images that are transferred to photographic film or to a video monitor.
An MRI works differently. Magnetic resonance imaging uses a magnetic field to create sound waves that are received, digitized, and displayed in real-time. When tissue is abnormal, its composition changes, so the images reflect damaged areas.
Read Also: How Would You Know If You Have Prostate Cancer
Description Of The Procedure
There are different types of surgery. The choice is made based on your health goals and where the growth is. Choices include:
- Transrectal biopsy A needle is sent through the rectum wall into the prostate. It will draw out a sample of tissue. A small ultrasound wand will be placed in the rectum. It will help to guide the needle.
- Transurethral biopsyA flexible tube is passed through the tip of the penis. It will be passed up through the tube to where the prostate sits. A cutting loop will be passed through the tube. It will removed a section of prostate.
- Perineal biopsyA small incision will be made in the area between the scrotum and the rectum. A small needle will be passed through the cut into the prostate gland. A sample will be drawn out with the needle.
Benefits Of Getting A Prostate Biopsy
A prostate biopsy is the only way to definitively determine whether you have prostate cancer and, if you do, how aggressive it is.
While prostate biopsies arent always conclusive, in general, a biopsy gives men the reassurance of knowing whether they have cancer or not. If you know you have prostate cancer, youre more likely to be appropriately treated.
Appropriate prostate cancer treatment options depend on several factors, including the stage of the cancer, your age, your general health and which risk category your cancer falls into.
Localized prostate cancer is categorized into six risk categories, which range from very low-risk to very high-risk. The risk group is determined by the stage of your cancer, your PSA levels and the Gleason score obtained from the biopsy pathology report.
The National Comprehensive Cancer Network guidelines outline appropriate treatment options based on risk categories and whether the cancer has already metastasized.
Patients whose cancer is confined to the prostate and falls into the very low-risk and low-risk categories tend to have slow-growing cancers. Treatment options for these patients often include active surveillance, radiation therapy or surgery. Similar treatment options may be recommended to patients in the low-risk and favorable intermediate prostate cancer risk categories.
The NCCN guidelines recommend immediate treatment for patients with high-risk disease or those patients whose cancer has metastasized.
You May Like: Are There Any Signs Of Prostate Cancer
Pros And Cons Of Transperineal Prostate Biopsy
In addition to potentially eliminating the need for antibiotics altogetheras the needle does not pass through the rectal wallthe newer method saves time instead of requiring separate appointments for both a pre-biopsy rectal swab and a subsequent biopsy once culture results are known, as is done using the TRUS system, the transperineal prostate biopsy can be completed in one in-office visit using only local anesthetic.
Duke began offering the transperineal prostate biopsy option in the clinic in October 2019, but Polascik has been performing the procedure in the operating room for the past 25 years using a cryotherapy grid. This larger transperineal prostate biopsy is done under anesthesia for the purpose of obtaining prostate tissue systematically every 5 mm, the results of which can be reconstructed into a 3-D framework of the prostate itself. Polascik gives two common reasons for why patients may opt for this larger 3-D transperineal mapping biopsy: to map out the exact size, number, and location of cancers within the prostate if interested in targeted ablation/focal therapy, and to confirm for patients in which there is still strong suspicion of having the disease, despite several rounds of conventional biopsies that have not detected prostate cancer.
Whats The Purpose Of A Transrectal Ultrasound
A transrectal ultrasound is a procedure that produces an image of the prostate. Its usually ordered after an abnormal PSA and DRE. For the test, a small probe is inserted into the rectum. The probe then uses sound waves to produce a picture on a computer screen.
The test is uncomfortable, but not painful. It can be done in your doctors office or on an outpatient basis in about 10 minutes. It can help estimate the size of the prostate and spot abnormalities that may indicate cancer. However, a TRUS cant confirm the diagnosis of prostate cancer.
A TRUS can also be used to guide a biopsy.
Also Check: How To Reduce Prostate Cancer
Types Of Prostate Biopsy
Historically, TRUS guided biopsy has been the standard approach. There are a variety of sampling schema with number of cores ranging from 6 to extensive 24 core saturation biopsy. Eichler et al. compared the cancer detection rates for several of these schemes and found that increasing number of cores was not associated with better cancer yield. Laterally directed sampling significantly improved detection while 1824 core sampling did not suggesting that 12 cores provides adequate sensitivity. Later studies demonstrated an improved sensitivity with 24 core saturation biopsy for men with suspicion of prostate cancer in spite of prior negative biopsy and in men with very large prostate volume., Brock et al. found a clinically significant CDR of 37.5% in men with elevated PSA using 12-core systemic biopsy which is approximate to sensitivity data obtained in similar studies.,
Contemporary MRI-guided biopsy strategies preferentially detect clinically important lesions and offer clear benefits over the traditional systematic biopsy. MRI-guided biopsy involves selective sampling of lesions identified as suspicious on mpMRI. There are several methods currently in use for targeted prostate biopsy: direct MRI-guided biopsy, cognitive fusion biopsy and MRITRUS fusion biopsy.
Technique And Anesthetic Agents Used For The Periprostatic Nerve Block
The technique for the periprostatic nerve block is based on the original method described by Nash et al. in 1996 for basal injections. The procedure can be performed in an out-patient setting, but resuscitation facilities should be available. The same protocol used for pre-procedure preparation of TRUS-guided prostate biopsy is followed. The bladder is emptied before the procedure to prevent urinary retention .
The optimal patient position for performing the periprostatic nerve block is the left lateral decubitus position with buttocks at or slightly beyond the side of the table, the left leg in a straight position, and the right leg flexed so as to touch the abdomen. The lithotomy position is an alternative, but it is associated with more discomfort .
Optimal position of ultrasound transrectal transducer with biopsy-guide attachment for periprostatic nerve block. Tip of ultrasound transducer is pressed against prostate and anterior rectal mucosa. Transducer is manipulated to direct needle towards neurovascular bundles at base and apex of prostate and local anesthetic drug is injected around bundles.
Also Check: Is Masturbation Good For Your Prostate
Don’t Miss: Hdr Radiation Therapy Prostate Cancer
Why You Should Not Have A Prostate Biopsy
Prostate biopsy risks There are risks associated with prostate biopsies, but physicians can take steps to reduce those risks. Risks and ways to manage them include: Infection: The most serious risk of a prostate biopsy is the risk of infection, including urinary tract infections and, less commonly, sepsis.
Other Cancer Treatment Effects On Ejaculation
Some cancer treatments reduce the amount of semen thats produced. After radiation to the prostate, some men ejaculate less semen. Toward the end of radiation treatments, men often feel a sharp pain as they ejaculate. The pain is caused by irritation in the urethra . It should go away over time after treatment ends.
In most cases, men who have hormone therapy for prostate cancer also make less semen than before.
Chemotherapy and other drugs used to treat cancer very rarely affects ejaculation. But there are some drugs that may cause retrograde ejaculation by damaging the nerves that control emission.
Also Check: Can Your Prostate Grow Back After Surgery
What Are The Different Types Of A Prostatebiopsy Procedures
A prostate biopsy is one of the last steps down the road after measuring prostate-specific antigen in the blood, performing a digital rectal examination, and considering each patients risk factors and symptoms.
The main goal is to obtain a prostate sample, especially if there is a visible lesion or tumor. But there are several ways to get this biopsy sample. The most common types are as follows:
The Transperineal Prostate Needle Biopsy
Requires a general anaesthetic, so you need to book out the day or even overnight. Remember, as noted above, your perineum is the part of the body between the anus and the scrotum. An incision is made in order to access the prostate for biopsy collection.
Now you know what type of prostate biopsy you might have, what about those seven questions I mentioned before? to see if they have been answered?
Also Check: Ebrt Therapy For Prostate Cancer
What New Biopsy Techniques Are Out There
Research is developing on other biopsy techniques that use MRIs. In this technique, doctors combine real-time ultrasound imaging with MRI data to guide a biopsy. A recent study published in the Journal of the American Medical Association that concludes using MRI with ultrasound produces better biopsy results1. This method aims to give a more accurate biopsy result while minimizing side effects including infection, bleeding, and potential damage to the urethra or nerves causing temporary incontinence and/or erectile dysfunction.
For men who have had a negative biopsy, there is a new test called ProMark. This helps to predict whether the next biopsy will also be negative, potentially cutting down on the number of biopsies a man will have to go through.
Prepare For The Immediate Complications
A prostate biopsy usually has the primary complication of bleeding. You can see blood in the urine, in the stool, or in your semen. Also, you may feel pain in your pelvic floor for up to one week. You need to understand before the procedure why this happens. That way, you will be able to tell when the bleeding is too much. Be sure to ask your doctor what to expect in your case.
You May Like: Robotic Operation For Prostate Cancer
My Prostate Biopsy Showed No Cancer But There Was High
High-grade prostatic intraepithelial neoplasia and atypical glands are sometimes precancerous changes, as about 25-30% of patients who have them may later be diagnosed with prostate cancer. Sometimes the conversion can take 10 years or more. My policy is to check the patients Prostate Health Index blood test quarterly for the next year and then decide whether a follow-up biopsy is indicated to rule out the development of cancer.
Read Also: What Is The Best Over The Counter Prostate Medicine
What Are The Different Types Of Prostate Biopsy
A biopsy is a key step in confirming a possible diagnosis of prostate cancer. It involves using thin needles to take small samples of prostate tissue, which are then looked at through a microscope. A biopsy might target specific areas of the prostate , or take samples from different areas of the prostate .
At the moment, most biopsies are done using the transrectal ultrasound-guided technique. This is where the needle goes through the wall of the back passage . However, it is becoming more common for a transperineal technique to be used. This is where the needle goes through the perineum, which is the skin between the testicles and the back passage.
An advantage of the TP biopsy is that it can now be performed using local anaesthetic. If there arent any problems, you will be able to go home from hospital on the same day.
Having any type of prostate biopsy can cause side effects, including urinary and sexual problems. Talk to your doctor or nurse about the possible side effects before having a biopsy, or call our Specialist Nurses on 0800 074 8383.
You May Like: Aggressive Prostate Cancer Survivor Stories