> > > This Simple Morning Test Will Fix Your Prostate
Another type of prostate issue is chronic prostatitis, or chronic pelvic pain syndrome. This condition causes pain in the lower back and groin area, and may cause urinary retention. Symptoms include leaking and discomfort. In severe cases, a catheter may be required to relieve the symptoms. If the problem is unresponsive to other treatments, your doctor may suggest a surgical procedure. If these do not work, your symptoms could progress and become chronic.
An acute bacterial infection can cause a burning sensation. Inflammation of the prostate can affect the bladder and result in discomfort and other symptoms. This is the most common urinary tract problem in men under 50, and the third most common in men over 65. The symptoms of acute bacterial prostatitis are similar to those of CPPS. Patients may experience a fever or chills as a result of the infection.
Table 1: American College Of Radiology Appropriateness Criteria
| Breast Cancer | |
| Rating = 5 used if MRI is contraindicated and the patient has neurological symptoms | |
| MRI with or without contrast head | Rating = 7 if the patient has neurological symptoms or if the patient is asymptomatic, but the tumour is > 3 cm and has adenocarcinoma histology or mediastinal adenopathy |
| MRI with or without contrast chest | Rating = 3 evaluating chest wall or cardiac invasion and for local staging of superior sulcus tumours. |
CT = computed tomography 18FDG = 18F-fluorodeoxyglucose MRI = magnetic resonance imaging NSCLC = nonsmall cell lung cancer PET = positron emission tomography PSA = prostate-specific antigen SPECT = single-photon emission computed tomography 99mTc = technetium-99m.
What Do My Test Results Mean
Your doctor will look at your test results to find out if the cancer has spread and how quickly it might be growing.
How far has my cancer spread?
The stage of your cancer tells you whether it has spread outside the prostate and how far it has spread. You might need scans, such as an MRI, CT or bone scan, to find out the stage of your cancer.
Depending on the results, your cancer may be treated as:
- localised prostate cancer its contained inside the prostate
- locally advanced prostate cancer its started to break out of the prostate or has spread to the area just outside it
- advanced prostate cancer its spread from the prostate to other parts of the body.
Is my cancer likely to spread?
Your doctor may talk to you about the risk of your cancer spreading outside the prostate or coming back after treatment.
Your prostate biopsy results will show how aggressive the cancer is in other words, how likely it is to spread outside the prostate. You might hear this called your Gleason grade, Gleason score, or grade group.
To work out your risk, your doctor will look at your PSA level, your Gleason score and the T stage of your cancer.
Low risk
Your cancer may be low risk if:
- your PSA level is less than 10 ng/ml, and
- your Gleason score is 6 or less , and
- the stage of your cancer is T1 to T2a.
Medium risk
Your cancer may be medium risk if:
- your PSA level is between 10 and 20 ng/ml, or
- your Gleason score is 7 , or
- the stage of your cancer is T2b.
High risk
What happens next?
Recommended Reading: Where Is A Mans Prostate
Bone Scans In Diagnosis Of Prostate Cancer
A bone scan uses tiny amounts of radioactive materials called tracers that are injected into the patient. These tracers accumulate in certain organs and tissues, such as bones, and give off a type of radiation called gamma radiation. The gamma rays can be seen by using a special camera, which produces images that can be interpreted by radiologists or by specialists in nuclear medicine.
A clever way to think about a bone scan is that it is the complete opposite of a X-ray examination. In an X-ray examination the radiation passes into or through your body from an external machine to create an image on film placed on the other side of your body. In a bone scan, the source of the radiation is inside your body and travels to the surface, where a camera detects it.
For patients who are newly diagnosed with prostate cancer, the value of a bone scan is limited. It would be unusal for the doctor to request a bone scan for any patient with a Gleason score of less than 7 and a PSA level of less than 20 ng/mL.
Patients with a Gleason score of 7 or higher may, however, be candidates for a bone scan, whatever their PSA level. A bone scan may be considered important in any patient with a Gleason score of 7 or higher who appears to be at high risk of bony metastatic disease. A bone scan is also indicated for any patient with prostate cancer who has symptoms suggesting bony metastases.
Content on this page last reviewed and updated April 26, 2008.
Lymph Node Biopsy As A Separate Procedure
A lymph node biopsy is rarely done as a separate procedure. Its sometimes used when a radical prostatectomy isnt planned , but when its still important to know if the lymph nodes contain cancer.
Most often, this is done as a needle biopsy. To do this, the doctor uses an image to guide a long, hollow needle through the skin in the lower abdomen and into an enlarged node. The skin is numbed with local anesthesia before the needle is inserted to take a small tissue sample. The sample is then sent to the lab and looked at for cancer cells.
Also Check: What Are The Early Warning Signs Of Prostate Cancer
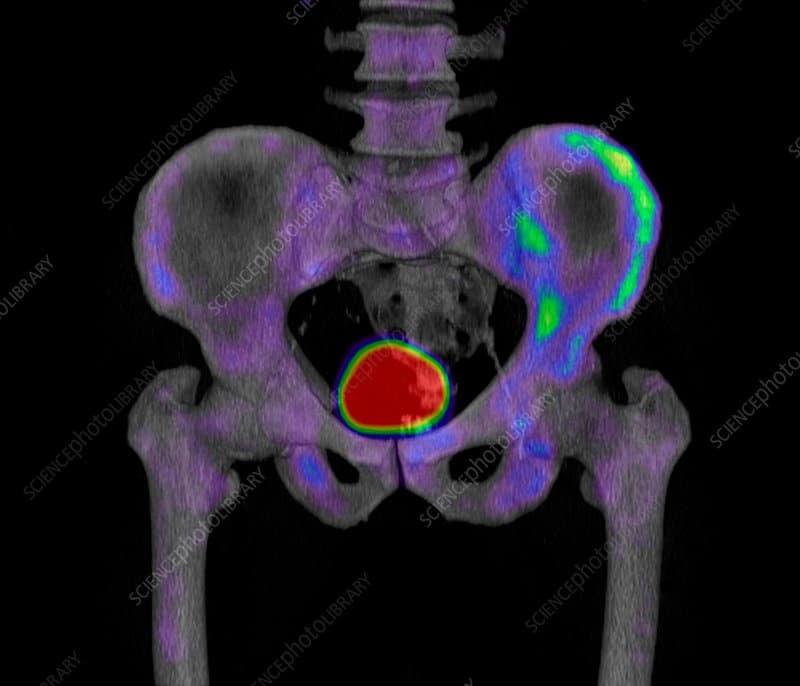
Table : Sensitivity And Specificity Of Diagnostic Methods To Detect Bone Metastasis10
| Test | |
| 0.978 | 0.978 |
BS = bone scan CI = confidence interval CT = computed tomography 18FDG =18F fluorodeoxyglucose PET = positron emission tomography SPECT = single-photon emission computed tomography.
Overall, the sensitivity and specificity of 18FDG-PET and 18FDG-PET/CT were higher for detection of bone metastasis compared with bone scan with or without SPECT. The authors concluded that 18FDG-PET or PET/CT can be substituted for bone scanning with 99mTc during a supply shortage. The radiation dose was reported to be higher for 18FDG-PET and PET/CT than bone scans , and therefore should be a consideration. A major limitation of this report is that it was not stated whether the patients with known cancer were symptomatic/asymptomatic or if imaging was being conducted for staging purposes. The list of included studies evaluated patient populations that are likely very different. For example, one study evaluated bone imaging in high-risk prostate cancer patients and another in newly diagnosed lung cancer patients.
Criterion 8: Relative risks associated with the test
Non-radiation Risks
PET The Pharmacopeia Committee of the Society of Nuclear Medicine conducted a four-year prospective evaluation of adverse reactions to PET and reported no adverse reactions among the 33,925 scans conducted in 22 participating PET centres in the United States.48
Radiation Exposure
Who Does A Bone Scan
A specially trained and certified nuclear medicine technologist performs the test. A nuclear medicine physician is a medical doctor who uses tracers to diagnose and treat disease. A radiologist or a nuclear medicine physician oversees the technologist. A radiologist is a medical doctor who uses imaging tests to diagnose disease. One of these doctors will read your scan and decide what it means.
You can have a bone scan done at:
-
A hospitals radiology or nuclear medicine department
-
An outpatient imaging center
Also Check: What Happens When You Remove Your Prostate
Other Factors Affecting Prostate Cancer Treatment Cost
Apart from the type of surgery or treatment and the choice of technology, the following are some of the factors that affect the overall prostate cancer treatment cost:
Type of Hospital
There are several hospitals around the world that provide world-class medical treatment to patients. The greater the number and quality of services offered by the hospital, the expensive is the treatment at the hospital.
Therefore, the total cost of prostate cancer treatment that you have to pay actually depends on the level of services that you expect from the hospital. To be able to receive five-star services from the hospital, you must be willing to pay lavishly for it.
Experience of the Surgeon
Expertise and skills of the treating doctor matter a lot when it comes to successful treatment of any cancer type. It takes a lot of patience, courage, and knowledge to treat a cancer patient and this is the reason why the most experienced surgeons tend to charge a greater fee for their services.
However, that does not mean that all the experienced and qualified surgeons charge fees that an average patient cannot afford. There are many highly educated and skilled doctors for prostate cancer treatment that offer their services with an equal compassion at a reasonable rate. Therefore, one must try to find a credible doctor with required credential who charges a fee that a patient can afford.
Length of Stay at the Hospital
Incidental Costs
Cost of Accommodation, Food, and Local Travel
| Cost per Day |
Will An Abdominal Ct Scan Show Back Problems
Our study suggests that abnormalities of the lumbar spine can be accurately detected on abdominal CT studies. The sensitivity, specificity, ppv, npv and accuracy of abdominal CT in lumbar spine evaluation on a per patient/per finding basis were 89.7/95.3%, 97.3/100%, 99.0/99.2%, 76.6/99.8% and 91.7/99.8%, respectively.
Don’t Miss: Porque Se Inflama La Prostata
Options For Dealing With Recurrence
With a persistently increasing PSA, the suspicion for recurrence increases. The most important factor in assessing your long-term outcome is determining the location of the prostate cancer cells producing the PSA. Advanced imaging techniques, such as MRI and PSMA PET/CT, are often helpful in learning where the cancer is located, and in the case of post-radiation recurrence, repeat biopsy may be required.
If a man underwent surgery as an initial treatment, revisiting the post-operative pathology report may help to identify what contributed to the recurrence. If there was still cancer present , the cancer was aggressive , or genomic profiling of the tumor showed high-risk features, several options are available:
- EBRT to the prostate bed with or without the pelvis.
- EBRT accompanied by hormone therapy. The duration of hormone therapy will depend on the PSA level just prior to radiation and to a lesser extent on the Gleason score and staging of the cancer.
- Systemic treatment using hormone therapy, other treatments for those at risk for metastatic disease, or a combination.
- Active surveillance if the remaining cancer appears insignificant. You and your doctor can decide whether to intervene more aggressively and, if so, when.
If youre seeking additional or different approaches, you may be eligible to participate in an appropriate clinical trial . You can research this with the help of your doctor.
Imaging For Metastasis In Prostate Cancer: A Review Of The Literature
- 1Department of Medical Oncology, CHU Lille, Lille, France
- 2Univ. Lille, CNRS, Inserm, CHU Lille, Institut Pasteur de Lille, UMR9020 UMR-S 1277 Canther Cancer Heterogeneity, Plasticity and Resistance to Therapies, Lille, France
- 3Medical Oncology Department, Centre Oscar Lambret, Lille, France
- 4Nuclear Medicine Department, CHU Lille, Lille, France
- 5Academic Department of Radiation Oncology, Centre Oscar Lambret, Lille, France
- 6CRISTAL UMR CNRS 9189, Lille University, Villeneuve-dAscq, France
- 7Department of Urology, CHU Lille, Lille, France
- 8Department of Radiology, CHU Lille, Lille, France
Background: Initial staging and assessment of treatment activity in metastatic prostate cancer patients is controversial. Indications for the various available imaging modalities are not well-established due to rapid advancements in imaging and treatment.
Methods: We conducted a critical literature review of the main imaging abnormalities that suggest a diagnosis of metastasis in localized and locally advanced PCa or in cases of biological relapse. We also assessed the role of the various imaging modalities available in routine clinical practice for the detection of metastases and response to treatment in metastatic PCa patients.
In routine clinical practice, conventional imaging still have a role, and communication between imagers and clinicians should be encouraged. Present and future clinical trials should use modern imaging methods to clarify their usage.
Recommended Reading: Blood In Urine After Prostate Surgery
Preparation For A Ct Scan
Some CT scans need special preparation beforehand.
For most scans, you have a drink or an injection of contrast medium, or both. This is a dye that shows up body tissues more clearly on the scan. You have the injection through a small thin tube in your arm. The tube is left in place until after your scan, in case you have any problems after having the injection.
Recommended Reading: Apple Cider Vinegar And Prostate Health
How Is Prostate Cancer Diagnosed And Evaluated
Your primary doctor will ask about your medical history, risk factors and symptoms. You will also undergo a physical exam.
Many patients undergo regular prostate cancer screening before symptoms appear. Screening may involve one or more of the following tests:
- Prostate-specific antigen : This test analyzes a blood sample for levels of PSA, a protein the prostate produces. Higher PSA levels could indicate cancer is present.
- Digital Rectal Exam :This test examines the lower rectum and the prostate gland to check for abnormalities in size, shape or texture. The term digital refers to the doctors use of a gloved, lubricated finger to conduct the exam.
If screening test results are abnormal, your doctor may perform the following imaging tests:
Read Also: Icd 10 Code For Prostate Cancer
How It Works And What To Expect
Most scans donât take more than an hour or so, though you may have to wait a few hours as health care workers prep you for the test.
These scans are usually done at a nuclear medicine or radiology department at a hospital. A little bit of radioactive material will go into your body. Doctors call this material a radioactive âtracer,â radionuclide, or radiopharmaceutical.
Hospital staff may inject this tracer or give it to you to swallow in a pill or inhale as a gas.
It can take from a few seconds to several days for the tracer to collect in the part of the body that will get scanned.
Before the scan, youâll remove all jewelry and metal that could interfere with the images. Medical staff may ask you to wear a hospital gown, though in some cases you can wear your own clothes.
Youâll lie on a table or sit on a chair for the scan. Technicians use a special camera, or âscanner,â on the appropriate parts of your body to detect gamma rays from the tracer. Technicians might ask you to change positions to get different angles as the scanner works.
The scanner sends the information to computer software that creates pictures, sometimes in three dimensions and with color added for clarity.
A specialized doctor called a radiologist will review the pictures and talk to your doctor about what they show.
Summary Of The Main Findings
The most thoroughly validated tests in clinical trials and in clinical practice are the good old tests such as bone scan and contrast-enhanced thorax, abdomen, and pelvis CT.
Nevertheless, most of the evidence based for bone scan and CT are old and retrospective. There is actually a much larger amount of prospective data for modern PET/CT. Prospective data also shows clear superiority of PSMA-PET or fluciclovine-PET to choline-PET. Data from a new study suggests that PSMA-PET imaging is superior to fluciclovine-PET for detecting biochemical recurrence in men with prostate cancer . However, whether one of these radiotracers improves patient survival over the other is unknown and further research is needed to determine which has the greater effect.
The new tracers do not have the same accessibility and need further validation in clinical trials to evaluate their benefits and clarify their usage in routine clinical practice. It is important that we consider the imaging requirements of the PCWG as this defines the imaging definitions for subjects in those clinical trials. EORTC algorithms also need to be considered for the imaging strategies. Experts in nuclear medicine and radiology should be represented in medical decision-making teams for PCa.
You May Like: How Long For Prostate Biopsy Results
When Further Treatment Is Needed
While prostate cancer diagnosis and treatment have improved significantly in recent years, the cancer can still recur. Thats why it is essential that you and your doctor continue to monitor your PSA on a quarterly basis for some period of time, no matter how successful your treatment seems to be. Patients usually can consider a number of treatment options to treat or control recurrent cancer. Choosing among them requires a new decision-making process.
Recommended Reading: Vaccine Treatment For Prostate Cancer
Statistical And Cost Analysis
We report the proportions of patients in each risk group who received a bone scan and subsequently underwent imaging and procedures. We further explore regional variation in use, as well as variation by primary treatment modality . The reason for the latter is that external beam radiation often includes a CT and/or MRI scan for treatment planning, which can be a source of confounding in this analysis for these 2 specific categories of imaging. Multivariate logistic regression models assessed for covariates associated with bone scan use in each risk group. All analysis was performed with SAS 9.2 , and a P value of < .05 was considered statistically significant.
Direct cost to Medicare was calculated based on the cost of a bone scan from the CPT code 78306, which accounted for the majority of Medicares bone scan claims among patients with prostate cancer. The 2012 Medicare national average reimbursement rate of $257.66 was multiplied by the estimated annual incidence of prostate cancer in patients older than 65. This figure was then multiplied by the proportion of patients receiving bone scans as reported in this study. Similarly, the costs of downstream imaging and procedures were estimated using 2012 national reimbursement rates multiplied by the relative frequency of each procedure.
You May Like: How Is Radiation Done For Prostate Cancer