Mri In Targeting Biopsies
TRUS guided biopsy is the most commonly used method for prostate cancer detection in patients with high PSA level and/or abnormal DRE. Although TRUS guided biopsy reveals even clinically insignificant cancerous foci within the prostate but it is also probability to miss really malignant prostate cancer. TRUS has 35% false NPV . Different studies were shown that performing Multi parametric MRI of prostate and then using it as a guide for prostate biopsy either directly in MR machine or after overlapping the images on real time TRUS images with fusion imaging methods will increase the detection rate of prostate cancer and is especially important in patients highly suspicious of prostate cancer due to abnormal PSA level and previous negative biopsy result .
Getting The Results Of The Biopsy
Your biopsy samples will be sent to a lab, where they will be looked at with a microscope to see if they contain cancer cells. Getting the results usually takes at least 1 to 3 days, but it can sometimes take longer. The results might be reported as:
- Positive for cancer: Cancer cells were seen in the biopsy samples.
- Negative for cancer: No cancer cells were seen in the biopsy samples.
- Suspicious: Something abnormal was seen, but it might not be cancer.
If the biopsy is negative
If the prostate biopsy results are negative , and the chance that you have prostate cancer isnt very high based on your PSA level and other tests, you might not need any more tests, other than repeat PSA tests sometime later.
But even if many samples are taken, biopsies can still sometimes miss a cancer if none of the biopsy needles pass through it. This is known as a false-negative result. If your doctor still strongly suspects you have prostate cancer , your doctor might suggest:
- Getting other lab tests to help get a better idea of whether or not you might have prostate cancer. Examples of such tests include the Prostate Health Index , 4Kscore test, PCA3 tests , and ConfirmMDx. These tests are discussed in Whats New in Prostate Cancer Research?
- Getting a repeat prostate biopsy. This might include getting additional samples of parts of the prostate not biopsied the first time, or using imaging tests such as MRI to look more closely for abnormal areas to target.
Prostate cancer grade
Gleason score
Why Should I Have An Mri Scan
Consultants usually identify prostate cancer and measure its growth rate using MRI scans although non-problematic cancers are typically found using biopsy. Whenever biopsies detect prostate cancer MRI scans can be used retrospectively and facilitate quicker patient treatment planning and to clarify if and where further biopsy should be taken.
In-depth studies on MRI scanning and the powerful magnetic fields involved have shown no risks to patients, making the procedure one of the safest stages of treatment available. Ongoing global research and development is already producing breakthrough technologies with scanners that can accommodate a patients medical condition or limitation.
Patients can often be accompanied by a close friend or family member throughout their MRI scan listening to music via headphones for the duration is also a popular option. Its important to remember that the MRI procedure is physically painless and any mild discomfort thats experienced during the scan is short-lived and gone the same day.
Recommended Reading: What Is Good For Prostate Health
This Video Describes The Process
Note that in the USA the breakpoint for having a concern is a PSA of 4. In the UK, this number varies with age between 3 and over 5 .
© Copyright Prostate Edinburgh 2020-22 A company incorporated in Scotland, Company No SC564971. Email : Prostate Edinburgh
Are you a man over 50 years of age? Do you know your PSA? If not, then please take steps to find it out, and track it if in the normal range.
Local Staging Of Prostate Cancer
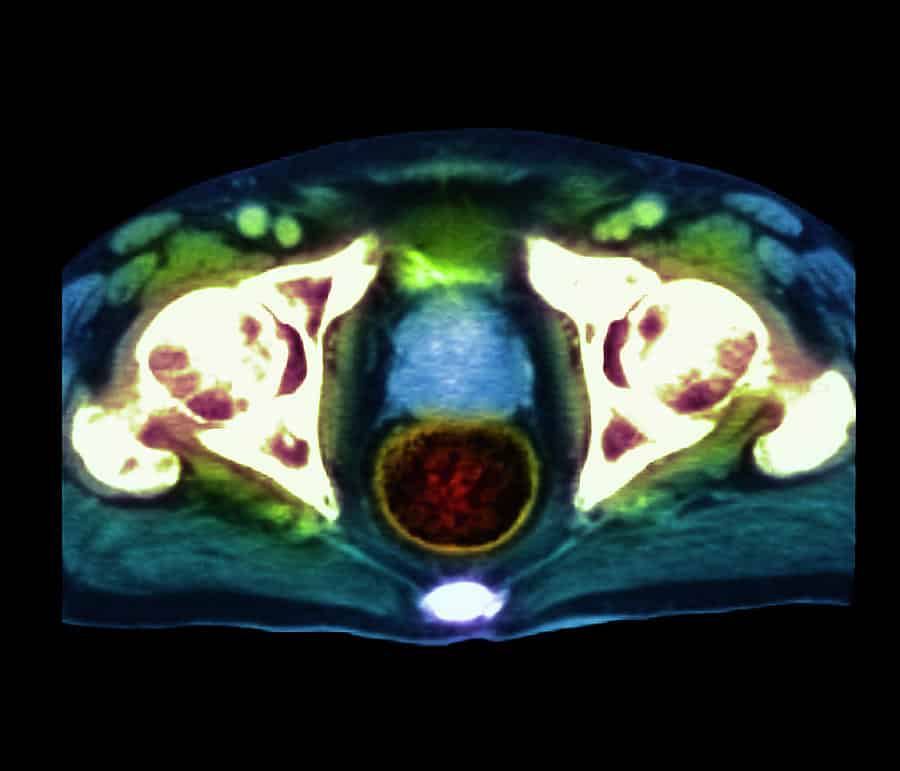
Determining the extension of prostate cancer and local staging is one of the main roles of a radiologist after detection of prostate cancer. Staging of prostate cancer is very important in therapy decision making as well as prognosis determination. Imaging techniques play a significant role in staging of prostate cancer and MRI is the most accurate imaging modality used for prostate cancer staging . High resolution MR images especially with the use of endorectal coil can show with high accuracy whether the tumor is confined to prostate gland or there is involvement of prostate capsule and extra capsular extension that is considered the T component of TNM staging system. Extension of tumor to periprostatic fat, invasion to neurovascular bundles and involvement of seminal vesicles and Denonvilliers fascia are well detected by MRI .4).
Biopsy Proven Prostate Cancer, Stage T3, Gleason Score 8.
A)Axial T2w. image of prostate gland: A hyposignal tumoral mass is evident in peripheral zone in right base of prostate. B) Axial T2w. image of prostate gland in more cephalic level: Involvement of seminal vesicles by prostate cancer is noted. C) Coronal T2w. image of prostate gland: Involvement of seminal vesicles is well shown.
Axial T2w. image of prostate gland: A hyposignal tumoral mass is noted at the right side of prostate. The capsule of prostate is disrupted with invasion of tumor to periprostatic fat, neurovascular bundle and Denonvilliers fascia.
Don’t Miss: What Is C61 Malignant Neoplasm Of Prostate
What Will I Experience During And After The Procedure
Most MRI exams are painless. However, some patients find it uncomfortable to remain still. Others may feel closed-in while in the MRI scanner. The scanner can be noisy.
You may feel pressure while the doctor inserts the endorectal coil into your rectum. This is similar to that experienced during a digital rectal exam.
It is normal for the area of your body being imaged to feel slightly warm. If it bothers you, notify the radiologist or technologist. It is important that you remain perfectly still while the images are being recorded, which is typically only a few seconds to a few minutes at a time. For some types of exams, you may be asked to hold your breath. You will know when images are being recorded because you will hear tapping or thumping sounds when the coils that generate the radiofrequency pulses are activated. You will be able to relax between imaging sequences but will be asked to maintain your position as much as possible.
You will usually be alone in the exam room during the MRI procedure. However, the technologist will always be able to see, hear, and speak with you using a two-way intercom. They will give you a squeeze-ball that alerts the technologist that you need attention right away. Many MRI centers allow a friend or parent to stay in the room if they are also screened for safety in the magnetic environment.
Histologic Correlation Of T2wi And Dwi
To summarize, healthy PZ tissue on T2WI and DWI appears as a region with both high T2 and high ADC. When luminal space and stromal matrix is lost to cancer, which consists of highly compacted cells, water diffusion becomes generally more restricted and macromolecular content increases. Water molecules encountering membrane boundaries and macromolecules within cancerous zones demonstrate observable decreases in both T2 and ADC . Two recent studies by Wang et al. and Gibbs et al. utilized histological measurements of cancer cell density to obtain inverse relationships between prostate cancer tumor cellularity and ADC values.
Healthy CG contains not only the same tissue components as the PZ but also more smooth muscle cells within the stromal matrix and frequently regions of benign prostatic hyperplasia . There are two histological types of BPH â glandular and stromal. The former appear as hyperintense nodules and the latter appear as hypointense nodules, which can occasionally mimic the appearance of cancer. However, the typical stromal tissue is curvilinear or band-like as it permeates between the glandular elements of BPH. Since muscle tissue has one of the lowest T2 values, healthy CG appears more hypointense and heterogeneous than the surrounding PZ on T2WI of the normal prostate, making CG tumor detection more difficult.
Also Check: Does Drinking Cause Prostate Cancer
Genetic Testing For Some Men With Prostate Cancer
Some doctors now recommend that some men with prostate cancer be tested to look for certain inherited gene changes. This includes men in whom a family cancer syndrome is suspected, as well as men with prostate cancer that has certain high-risk features or that has spread to other parts of the body. Talk to your doctor about the possible pros, cons, and limitations of such testing.
The Emergence Of Quantitative Image Analysis
As sequences and analyses evolve, the information gathered is being used in either a qualitative or quantitative fashion. The T2W images acquired provide exquisite qualitative visualization of sub-glandular structures that can be used for immediate image interpretation. Since T2W images are a composite of multiple effects, including the T2-weighting specific echo time , proton density , residual T1-weighting reflected by the selected repetition time , sensitivity of the receiver coil, main static field , and RF transmission inhomogeneity, the quantitative values of individual signal intensities in any given voxel have no specific meaning outside of their relation to their neighbors. However, if images are collected at more than one echo time, then estimates of T2 values may be made for each voxel and displayed as T2 maps with tissue-specific T2 values. T2 maps have largely been restricted to research settings, but the quantitative analysis of what are now largely qualitative acquisitions may prove beneficial in clinical settings.
However, having errors in measurement between institutions causes obvious difficulty when attempting to evaluate quantitative methods in multi-center trials. As a result, these complications make quantitative image analysis an active area for research for the development and testing of improved measurement techniques and rigorous testing of biophysical models for better determination of quantitative tissue characterization parameters.
Recommended Reading: Prostate Cancer Center Of New Jersey
What Body Areas Are Seen During An Mri Of The Abdomen And Pelvis
Body organs that can be seen during an MRI of the abdomen and pelvis include:
- Stomach, intestines , liver, gallbladder, pancreas, and spleen. These organs help break down the food you eat and get rid of waste through bowel movements.
- Kidneys, ureters, bladder, and urethra . These organs make urine and allow you to urinate.
Treatment Planning For Radiation Therapy
Radiation therapy is one of the main prostate cancer treatment methods that can be used in low stage up to high stage of disease and even in bone metastasis of prostate cancer. According to patients condition and stage of disease, radiation therapy performs alone or in combination with other therapy methods like surgery or hormonal therapy.
There are two kinds of radiation therapy methods: External beam radiation therapy and Brachytherapy . Radiation therapy can use in low risk patients for curing the cancer completely and it calls radical radiotherapy. In higher stage of prostate cancer and when bone metastasis are existence and patients suffer from pain radiation therapy is used for shrinking cancerous cells on nerves systems and bones to decrease pain . After radical prostatectomy radiation therapy is useful for preventing and decreasing cancer recurrence and distal metastasis. In intermediate to high risk patients, radiation therapy can be used in combination with hormonal therapy before or after radical prostatectomy . MR images can be used reliably for treatment planning of radiation therapy.
Also Check: Stage 2 Prostate Cancer Definition
Has The Radiologist Who Will Read The Study Undergone Pi
The Prostate Imaging Reporting and Data System, or PI-RADS®, refers to standards that have been developed by several organizations to improve early diagnosis and treatment of prostate cancer.
Prostate cancer is the most commonly diagnosed cancer in men, with one out of nine men diagnosed in their lifetime. And while many cases dont require treatment, it is a leading cause of cancer death among men, second only to lung cancer. The broad range between cancer that does not require treatment and life-threatening prostate cancer means that proper diagnosis is key to determining next steps.
How Do I Prepare For A Prostate Ultrasound
You dont need to do much to prepare for a prostate ultrasound. Its an outpatient procedure that usually takes less than an hour. Your doctor may refer you to a hospital or clinic that has the proper ultrasound equipment for this test. You may also need to sign a consent form before the test.
Some possible instructions that your doctor might give you before the test include:
- Dont eat for a few hours before the test.
- Take a laxative or enema to help clear out your intestines a few hours before the test.
- Stop taking any medications that can thin your blood, such as nonsteroidal anti-inflammatory drugs or aspirin, about a week before the procedure. This is usually recommended if your doctor plans to take a biopsy of your prostate.
- Dont wear any jewelry or tight clothes to the clinic on the day of the procedure.
- Take any medications recommended to help you relax during the procedure. Your doctor may recommend a sedative, such as lorazepam .
- Make sure someones available to take you home in case your doctor gives you a sedative.
Read Also: Can An Mri Detect Prostate Cancer
Pet/mri Basics And Image Acquisition
PET/MRI imaging systems can be either in tandem or integrated. Tandem systems have the MRI and PET machines located either in adjacent rooms or side-by-side in the same room with a moveable patient table between . Tandem PET/MRI units such as the Phillips Ingenuity were the initial systems developed because the magnetic field generated by the MRI machine did not interfere with the PET unit. Due to the large footprint and cumbersome nature of tandem PET/MRIs, these have largely been supplanted by their integrated counterparts. A major hurdle of integrated or simultaneous systems is the fact that the photomultiplier tubes used in traditional PET scanners cannot function within a strong magnetic field. The development of avalanche photodiodes, photon detectors insensitive to magnetic changes, was the breakthrough that allowed development of and commercialization of modern integrated PET/MRIs . While one drawback of avalanche photodiodes is the inability to measure time of flight, silicon photomultiplier detectors have been developed to circumvent this limitation .
Existing relevant experience on the multi-faceted use of PET/MRI in prostate cancer is summarized in Table 1.
Table 1
How The Test Will Feel
An MRI exam causes no pain. If you have difficulty lying still or are very nervous, you may be given a medicine to relax you. Too much movement can blur MRI images and cause errors.
The table may be hard or cold, but you can request a blanket or pillow. The machine produces loud thumping and humming noises when turned on. You can wear ear plugs to help reduce the noise.
An intercom in the room allows you to speak to someone at any time. Some MRIs have televisions and special headphones that you can use to help the time pass.
There is no recovery time, unless you were given a medicine to relax. After an MRI scan, you can resume your normal diet, activity, and medicines.
Donât Miss: What Age Do Males Get Prostate Cancer
Don’t Miss: Prostate Cancer Surgery Or Radiation Which Is Better
Preparing For Your Mri Scan
Before you go to your appointment, or when you arrive, you fill in a safety checklist. This asks about:
- any operations youve had
- whether you have any metal implants or other metals in your body
An MRI scan uses strong magnetism which could affect any metal in your body. This includes:
- pacemakers or an implantable defibrillator
- surgical clips, pins or plates
- cochlear implants
- metal fragments anywhere in your body for example from an injury, dental fillings and bridges
You can still have an MRI scan if you have some metals in your body, but your doctor and radiographer decide if its safe for you. Tell the scanner staff about any metals in your body.
Some people feel claustrophobic or closed in when theyre having an MRI scan. Contact the department before your test if youre likely to feel like this. The hospital staff can take extra care to make sure youre comfortable and that you understand whats going on. Your doctor can give you medicine to help you relax if you need to.
The radiographers let you know whether you need to empty your bowels of any poo or gas before having the scan. In some departments you might be given an enema. An enema is a liquid filled pouch that has a nozzle that you can put into your back passage and it helps to empty your bowels.
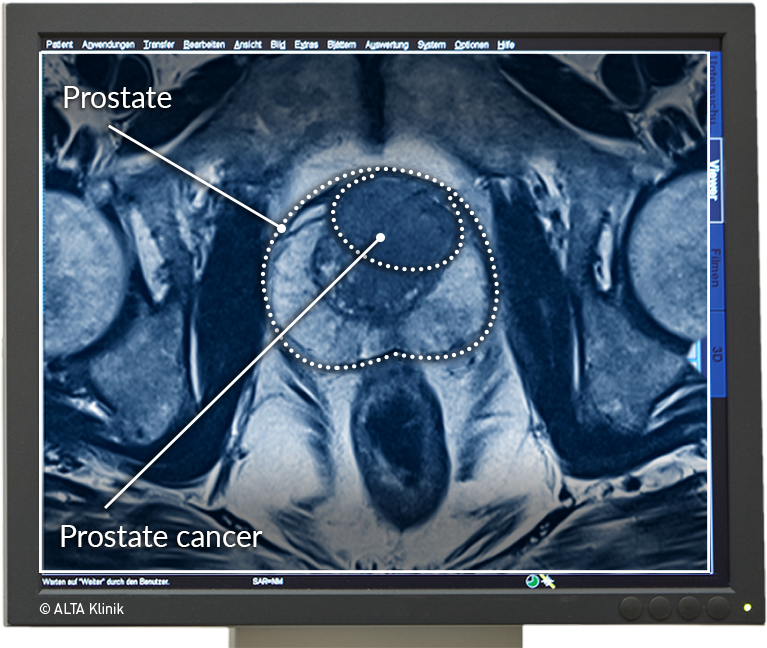
Detection Of Prostate Cancer
Figure 1.Biopsy Proven Prostate Cancer, Stage T2, Gleason Score 7.
A) Axial T2w. image of prostate gland: A hyposignal tumoral mass is well depicted within the peripheral zone at the left side of prostate. Endorectal coil is seen in the lumen of rectum. B) Post contrast fat suppressed T1w. image: tumoral mass shows enhancement after contrast injection. C) Diffusion weighted image: water restriction is noted in tumoral lesion in ADC map.
Don’t Miss: First Signs Of Prostate Cancer
B Role Of Mpmri In Selecting Therapy Local Management Surgical Choice And Technique
Identification of pathologic features of cancer is important to help guide therapy in individual patients. Results from mpMRI can be integrated into currently available clinical staging systems, and the information can be extrapolated to help risk stratify patients, guide therapy choice, and inform surgical technique. Therapeutic technique including surgical technique, radiation planning, and antihormonal therapy may be modified based upon the improved accuracy of radiologic staging over clinical staging.
1. Radical Prostatectomy Planning
2. Radiation Therapy Planning and Androgen Deprivation Therapy Duration
Accurate radiological staging is important for target volume definition and dose prescription in conformal radiotherapy when treating prostate cancer. Kamrava et al. showed 12% of patients were stratified into a higher risk category using an mpMRI/TRUS fusion biopsy, and 18% were upgraded to intermediate or high risk from the low risk group.102 Panje et al. studied 122 patients who underwent radiation therapy and found tumor stage shift occurred in 56% of patients after mpMRI. Upstaging was most prominent in patients showing high PSA but was also substantial in patients presenting with low-risk PSA levels and low-risk Gleason scores . Risk group changes occurred in 29% with consequent treatment adaptations regarding target volume delineation and duration of androgen deprivation therapy.103
3. Use of mpMRI for Focal Therapy Planning