Survival Statistics For Prostate Cancer
Survival statistics for prostate cancer are very general estimates and must be interpreted very carefully. Because these statistics are based on the experience of groups of people, they cannot be used to predict a particular personâs chances of survival. In general, most men diagnosed with prostate cancer do not die from the disease itself and will die from other causes.
There are many different ways to measure and report cancer survival statistics. Your doctor can explain the statistics for prostate cancer and what they mean to you.
Also Check: Malignant Prostate Cancer Survival Rate
About Dr Dan Sperling
Dan Sperling, MD, DABR, is a board certified radiologist who is globally recognized as a leader in multiparametric MRI for the detection and diagnosis of a range of disease conditions. As Medical Director of the Sperling Prostate Center, Sperling Medical Group and Sperling Neurosurgery Associates, he and his team are on the leading edge of significant change in medical practice. He is the co-author of the new patient book Redefining Prostate Cancer, and is a contributing author on over 25 published studies. For more information, contact the Sperling Prostate Center.
Tertiary Grade On Needle Core Biopsy
In contrast to the original Gleason grading system, it is now recommended that on a needle core biopsy both the most common and highest grade are added together for the Gleason score . For example, if there is 60 % Gleason pattern 3, 35 % Gleason pattern 4, and 5 % Gleason pattern 5, the Gleason score would be 3+5=8. Needle core biopsy is an imperfect, non-targeted, random sampling of the prostate gland. Thus any amount of high-grade tumor sampled on needle biopsy most likely indicates a more significant amount of high-grade tumor within the prostate. In all specimens, in the setting of high-grade cancer, one should not report a lower grade if it occupies less than 5 % of the total tumor. For example, if there is 98 % Gleason pattern 4 and 2 % Gleason pattern 3, the Gleason score would be reported as 4+4=8 .
Don’t Miss: What’s A Prostate Do
How The Study Was Performed
During the study, scientists randomized 1,071 men with intermediate- or high-risk localized prostate cancer into four groups. One group received radiation and six months of an anti-testosterone drug called leuporelin, and the second group received radiation plus 18 months of leuporelin therapy. Two other groups were treated with the same regimens of either radiation plus six or 18 months of leuporelin therapy, along with another drug called zoledronic acid, which helps to limit skeletal pain and related complications should cancer spread to the bones. Study enrollment occurred between 2003 and 2007 at 23 treatment centers across New Zealand and Australia.
Donât Miss: How Early Can You Get Prostate Cancer
Monitoring And Treatment Decisions
In the past, men with prostate cancerregardless of whether it was aggressive or notwere almost always treated right away with a targeted therapy like surgery or radiation. However, in recent years, experts have revisited this one-size-fits-all approach to prostate cancer.
Experts now understand that low-risk prostate cancerlike Gleason 6 tumorsmay not need treatment right away. In fact, major medical associations, including the American Urological Association and the Society for Urologic Oncology, now recommend the use of active surveillance for low-risk prostate cancer.
Don’t Miss: Prostate Artery Embolization Side Effects
Independent Predictors On Css
Deaths from non-PCa causes were regarded as competing events of cancer-specific mortality. Fine-Gray competing-risk regression models revealed that race, AJCC TNM stage, PSA levels, marital status, treatments, and GP were independent predictors for CSS in the univariate and multivariate analyses . Specifically, GP 5 + 4 was associated with a poorer CSS compared with GP 4 + 5. The GP 4 + 5 group had a lower 3, 5, and 10-year CIF than the GP 5 + 4 group. In the multivariate analysis, the GP 5 + 4 group had a higher risk of CSM than the GP 4 + 5 group . Although the AJCC T stage was not proven to be an independent predictor for OS in the multivariate Cox analyses, the higher T stage indicated higher risks of CSM in the multivariate competing-risk regression . Age at diagnosis was not proven to be significantly associated with CSS. Given that age at diagnosis was a powerful predictor for OS, we included it into the final multivariate competing-risk model.
Figure 4. The CIF curves of CSM before PSM. CIF curves for age at diagnosis CIF curves for race CIF curves for AJCC stage CIF curves for AJCC T stage CIF curves for AJCC N stage CIF curves for AJCC M stage CIF curves for Gleason patterns CIF curves for PSA levels CIF curves for marital status CIF curves for treatments. CIF, cumulative incidence function CSM, cancer-specific mortality PSM, propensity score-matching PSA, prostate-specific antigen.
What Will Happen In The Last Few Days
It can help to know what is normal in the last few days of life so that you know what to expect. You might not be aware of these changes when they happen because you may be drowsy or unconscious.
If youre supporting someone who is dying, read about what you can do to help and how you can get support.
Pain
Many people worry about being in pain when they are dying. Some people do get pain if their prostate cancer presses on their nerves or makes their bones weak. But not everyone dying from prostate cancer has pain. And if you are in pain, there are things that can help to reduce and manage pain.
You should tell your doctor or nurse if youre in pain or if your pain gets worse. They can talk with you about how best to manage your pain and can help keep it under control.
You may find sitting or lying in some positions more comfortable than others, so ask if you need help getting into a different position.
Your doctor can give you medicines to help manage pain. The type of medicines they give you will depend on what is causing the pain and which medicines are suitable.
Your doctor will monitor how the pain medicines are working and may change the type of medicine or the dose. If youre still in pain or get pain in between taking medicines, its important to tell your doctor or nurse.
Sleeping and feeling drowsy
Changes in skin temperature or colour
Changes in breathing
Changes in urinating or bowel movements
Also Check: How To Do A Prostate Biopsy
What Are The Stages Of Prostate Cancer
Cancer staging is first described using what is called a TNM system. The “T” refers to a description of the size or extent of the primary, or original, tumor. “N” describes the presence or absence of, and extent of spread of cancer to lymph nodes that may be nearby or further from the original tumor. “M” describes the presence or absence of metastases — usually distant areas elsewhere in the body other than regional lymph nodes to which cancer has spread. Cancers with specific TNM characteristics are then grouped into stages, and the stages are then assigned Roman numerals with the numerals used in increasing order as the extent of the cancer being staged increases or the cancer prognosis worsens. Prognosis is finally reflected by considering the patient’s PSA score at presentation as well as their Gleason score in assigning a final stage designation.
The American Joint Commission on Cancer system for prostate cancer staging is as follows:
The primary tumor
Traditionally, advanced prostate cancer was defined as a disease that had widely metastasized beyond the prostate, the surrounding tissue, and the pelvic lymph nodes and was incurable. However, a more contemporary definition includes patients with the lower-grade disease with an increased risk of progression and/or death from prostate cancer in addition to those with widely metastatic disease.
CT scan is used for the initial staging in select patients including
The regional lymph nodes
The distant metastasis
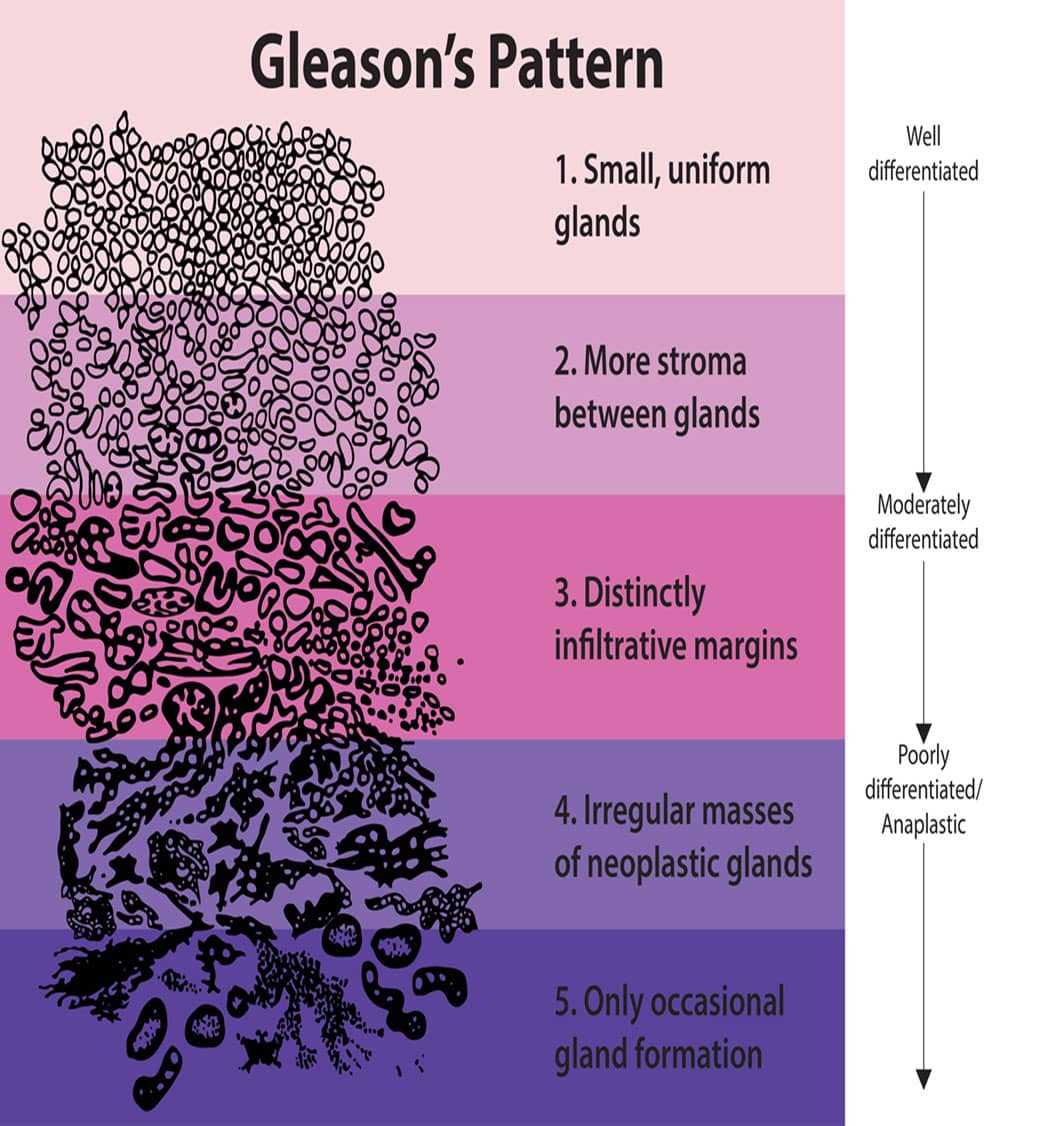
What Is A Gleason Score
If you have prostate cancer, your Gleason score is one factor healthcare providers consider to develop your treatment plan.
Your score reflects what providers learned about your cancer after examining tissue samples from your prostate cancer biopsy. They looked for patterns of normal and abnormal cells, noting where your cells look more like cancerous cells and where they look more like healthy cells.
Then they graded each piece of the pattern on a 3 to 5 scale. Pattern pieces with cancer cells that look like healthy cells were graded low. Pieces with cancer cells that don’t look like healthy cells get high grades.
Providers add those scores to set an overall Gleason score between 6 and 10. They might refine their analysis by classifying your cells by group, with Gleason scores listed in grade groups 1 to 5.
Also Check: Does Drinking Water Help Enlarged Prostate
What Is The Gleason Grading System
Your Gleason score isn’t a separate test. It’s a number based on the results of your biopsy. You usually get it when you’re first diagnosed with prostate cancer.
The doctor uses the numbers 1 to 5 to grade the most common and second most common patterns of cells found in a tissue sample:
- Grade 1. The cells look very much like normal prostate cells.
- Grades 2-4. Cells that score lower look closest to normal and represent a less aggressive cancer. Those that score higher look the furthest from normal and will probably grow faster.
- Grade 5. Most cells look very different from normal.
The two grades added together are your Gleason score. Cancers will score 6 or more. A score of 7 means the cancer is intermediate, and a higher score means the cancer is more likely to grow and spread.
Your doctor will use this combined score along with the results of your PSA blood test and digital rectal exam to see how advanced your prostate cancer is. They’ll use this information to suggest the best treatment for you.
Overview Of The Staging System
After a thorough assessment by your oncologist, your cancer will be assigned a stage between I and IV. Prostate cancer stages are based on the American Joint Committee on Cancer TNM system. Using the TNM system, your oncologist:
- Examines the tumor
- Determines if the cancer has spread to any lymph nodes
- Assesses whether the cancer has metastasized
- Considers the prostate-specific antigen level from blood testing
- Assigns a grade group based on how abnormal the cancer appears under a microscope
With this information in mind, you can better understand how stages are assigned and what they mean for patients in general.
Also Check: Prostate Surgery Incontinence Recovery Time
You May Like: What Kind Of Cancer Is Prostate Cancer
Stage Iv Prostate Cancer Prognosis
Prostate cancers detected at the distant stage have an average five-year survival rate of 28 percent, which is much lower than local and regional cancers of the prostate. This average survival rate represents stage IV prostate cancers that have metastasized beyond nearby areas to lymph nodes, organs or bones in other parts of the body.
Locally Advanced Prostate Cancer
Doctors may describe prostate cancer as localised, locally advanced and metastatic. Locally advanced prostate cancer means that the cancer has broken through the capsule of the prostate gland. It may have spread into the:
- tissue around the prostate
- the tubes that carry semen. These are the seminal vesicles
- body organs nearby such as the back passage or bladder
- lymph nodes close to the prostate gland
In the TNM staging system, locally advanced prostate cancer is the same as T3 or T4. Below is a simplified description of the T3 and T4 stage:
T3 means the cancer has broken through the capsule of the prostate gland.
T4 means the cancer has spread into other body organs nearby, such as the back passage, bladder, or the pelvic wall.
Recommended Reading: Prognosis Of Prostate Cancer Spread To Bones
What Does It Mean If My Biopsy Report Also Mentions Atrophy Adenosis Or Atypical Adenomatous Hyperplasia
All of these are terms for things the pathologist might see under the microscope that are benign , but that sometimes can look like cancer.
Atrophy is a term used to describe shrinkage of prostate tissue . When it affects the entire prostate gland it is called diffuse atrophy. This is most often caused by hormones or radiation therapy to the prostate. When atrophy only affects certain areas of the prostate, it is called focal atrophy. Focal atrophy can sometimes look like prostate cancer under the microscope.
Atypical adenomatous hyperplasia is another benign condition that can sometimes be seen on a prostate biopsy.
Finding any of these is not important if prostate cancer is also present.
What Is The Gleason Score
The Gleason grading system estimates the aggressiveness of the cancer by assigning a pattern to the cancer cells depending on their appearance under the microscope. A number from 1 to 5 is used as a measure of how aggressive the cancer looks under the microscope.
- If the cancerous tissue looks much like normal prostate tissue, a grade of 1 is assigned.
- If the cancer cells and their growth patterns look very abnormal, a grade of 5 is assigned.
- Grades 2 through 4 have features in between these extremes.
The most common type of prostate biopsy is a core needle biopsy. For this procedure, the doctor inserts a thin, hollow needle into the prostate gland. When the needle is pulled out it removes a small cylinder of prostate tissue called a core. This is typically repeated several times to sample different areas of the prostate.
Since multiple core biopsy samples are evaluated and prostate cancers in a single patient often have areas with different grades the pathologist assigns two grades to the examined prostate tissue. The first grade is the most common pattern seen after review of all the biopsy specimens and the 2nd grade is assigned to the next most common pattern.
Recommended Reading: Removing Prostate Due To Cancer
Prostate Cancer Survival Trends Over Time
As with most cancers, survival for prostate cancer is improving. However, interpretation of prostate cancer survival trends is difficult as the case-mix on which they are based is likely to have changed over time with earlier diagnoses following the advent of TURP and PSA testing. The detection of a greater proportion of latent, earlier, slow-growing tumours in more recent time periods will have the effect of raising survival rates due to lead-time bias . Lead-time bias for prostate cancer is estimated to be between five and 12 years, varying with a mans age at screening. Data from the European Randomized Study of Prostate Cancer estimates that for a single screening test, mean lead times are 12 years at age 55 and six years at age 75. Some of the increase may also be attributed to genuine improvements in survival due to more effective treatment, for both early, aggressive prostate cancers and advanced cases.
One-year age-standardised net survival for prostate cancer has increased from 66% during 1971-1972 to 94% during 2010-2011 in England and Wales an absolute survival difference of 28 percentage points.
Prostate Cancer , Age-Standardised One-Year Net Survival, Men , England and Wales, 1971-2011
Prostate Cancer , Age-Standardised Five-Year Net Survival, Men , England and Wales, 1971-2011
Prostate Cancer , Age-Standardised Ten-Year Net Survival, Men , England and Wales, 1971-2011
Treatment By Stage Of Prostate Cancer
Different treatments may be recommended for each stage of prostate cancer. Your doctor will work with you to develop a specific treatment plan based on the cancers stage and other factors. Detailed descriptions of each type of treatment are provided earlier on this same page. Clinical trials may also be a treatment option for each stage.
Early-stage prostate cancer
Early-stage prostate cancer usually grows very slowly and may take years to cause any symptoms or other health problems, if it ever does at all. As a result, active surveillance or watchful waiting may be recommended. Radiation therapy or surgery may also be suggested, as well as treatment in clinical trials. For those with a higher Gleason score, the cancer may be faster growing, so radical prostatectomy and radiation therapy are often recommended. Your doctor will consider your age and general health before recommending a treatment plan.
ASCO, the American Urological Association, American Society of Radiation Oncology, and the Society of Urologic Oncology recommend that patients with high-risk early-stage prostate cancer that has not spread to other areas of the body should receive radical prostatectomy or radiation therapy with hormonal therapy as standard treatment options.
Locally advanced prostate cancer
Watchful waiting may be considered for older adults who are not expected to live for a long time and whose cancer is not causing symptoms or for those who have another, more serious illness.
You May Like: Stage 4 Metastatic Prostate Cancer Life Expectancy
Interobserver Reproducibility Of Percent Pattern 4
It has been documented that interobserver reproducibility for the recognition of Gleason pattern 4 in prostate needle biopsies is not high. In particular, the rate of the agreement between an expert genitourinary pathologist and general pathologists was lower in cases where pattern 4 was scattered among pattern 3 than in those with discrete tumor foci . In a recent study , interobserver reproducibility of percent Gleason pattern 4 in prostate needle biopsy was also assessed in a prospective manner. In 422 biopsy cores received for a second opinion at their institution, 75% of cores were within ±10%, with 32% being a perfect match, between an expert genitourinary pathologist and 1 of 4 genitourinary pathology fellows nearing the end of their fellowship. However, in 88 cases with less than10% tumor involvement of the core, an agreement rate was lower . As a result, the authors did not recommend recording the percentage of pattern 4 in a small focus of Gleason score 7 cancer where grading only a few cancer glands might radically overestimate the amount of pattern 4 in the case.