Different Seminal Vesicles Problems
There could be so many different medical conditions that tend to affect the seminal vesicles. However, these cases are very rare. Here are some medical conditions that tend to have an effect on the seminal vesicle.
-
Infection in Seminal Vesicle
There might be some abscess forming in the seminal vesicle in case there is a bacterial infestation in the area. This can occur from the infections that happen in the prostate gland as well as the urethra of the male. In this situation, the enlarged seminal vesicles causes the gland to swell and have some pain. There might also be some pus as a result of the infection. It is important to drain the abscess in order to overcome the problem.
-
Seminal Vesicle Cysts
There might be some cysts that are formed in the seminal vesicle. Although they are asymptomatic, they can cause some problems in the future for sure. Some prior infections and surgery could be the reason for the formation of the cyst in the seminal vesicle. Some of the major symptoms of such medical conditions include penile pain, enlarged seminal vesicles, blood in the urine, and much more.
Apart from that, stones and cancer in the seminal vesicles are also considered to be effective medical conditions that take place in the seminal vesicle. It is important for the person to go see the doctor and get a seminal vesicle ultrasound to get more details on their medical condition.
Accessory Reproductive Glands Add Seminal Fluid To Semen
Sperm cells depend on seminal fluid to keep them moving and alive. This fluid is produced during ejaculation by accessory glands: the seminal vesicles, the prostate, and the bulbourethral glands. The seminal vesicles, two saclike structures, sit close behind the bladder and extend toward the bladder. There they each join one of the vas deferens to form the ejaculatory ducts. The vesicles secrete a whitish-brown fluid containing sugars, prostaglandins, and other substances that makes up two-thirds of the semen volume. The prostate, located under the bladder and above the start of the penis, contains the ejaculatory ducts and the prostatic urethra. As semen enters the urethra, the prostate secretes enzymes that help activate the sperm. The bulbourethral glands are pea-sized, with single ducts that connect to the urethra where it emerges from the prostate. These glands add mucus that helps with sperm motility.
Normal Anatomy And Radiographic Appearance
The normal prostate gland surrounds the most proximal aspect of the urethra and lies ventral to the rectum and caudal to the urinary bladder, typically within the pelvic canal. In many dogs, especially neutered dogs, the normal prostate gland is not visible radiographically. With slight enlargement, whether normal or abnormal, the prostate gland is recognized radiographically by its round shape and soft tissue opacity and by the relation of the gland to the organs around it. The absolute normal size of the prostate gland is dependent on the age, size and neuter status of the dog being imaged.1 Inability to see the normal prostate gland is influenced by the fact that it is usually in direct contact with the rectum, resulting in the dorsal border of the prostate gland being effaced, especially if the rectum contains feces. A full rectum may also obscure the prostate gland on the ventrodorsal view. Also, if the shape or position of the prostate gland is altered, it may not be recognizable other than as a nondescript opacity between the bladder, rectum, and pelvis.2
The normal prostate gland is not visible in the cat because of its location on the dorsal lateral surfaces of the mid pelvic urethra and its small size, measuring normally only about 10mm in length.3 Prostatic diseases causing clinical signs in cats are very rare and will not be considered further in this chapter.
Donald E. Thrall DVM, PhD, DACVR , Ian D. Robertson BVSc, DACVR, in, 2016
Also Check: What’s The Difference Between Colon Cancer And Prostate Cancer
Clinical Relevance Seminal Gland Abscess
Inflammation of the seminal vesicles may result after microbial infection of the urethra and prostate gland. Symptoms such as vague perineal or penile pain, discomfort during ejaculation and haemospermia are suggestive of such infection.
Treatment consists of proper antibiotic regimens. In rare cases, obstruction of the seminal vesicle duct may lead to abscess formation. In such cases paracentesis is the mainstay of treatment. Drainage of these abscesses may be facilitated by transrectal ultrasound guided aspiration.
Cancer Of The Seminal Vesicle
Cancer that develops in the seminal vesicles is very rare. As of the year 2000, there were only 48 cases confirmed in American or European medical literature. Its currently unclear as to what causes cancer to arise in the seminal vesicles.
Many cancers that involve the seminal vesicles occur because of invasion of the seminal vesicles due to another malignant cancer, typically prostate cancer. The closeness of the seminal vesicles with the prostate makes this invasion possible.
Read Also: Prostate Cancer Spread To Colon
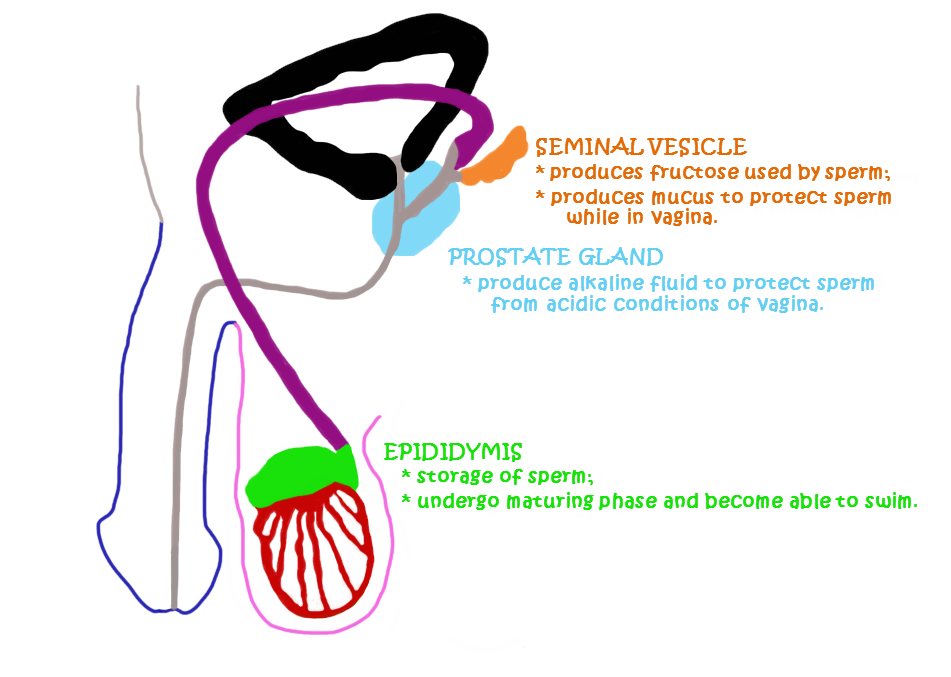
Anatomy And Function Of Seminal Vesicles
The seminal vesicles are located below the bladder and above the prostate gland. An individual seminal vesicle consists of a single coiled tube off of which several pouches branch.
The tube of a seminal vesicle is made up of three different layers:
- moist inner layer of specialized cells that work to produce seminal vesicle fluid
- middle layer of smooth muscle tissue
- outer layer of connective tissue
Part of the seminal vesicles and the vas deferens combine to form the ejaculatory duct, which eventually drains into the prostatic portion of the urethra. During ejaculation, the smooth muscle layer of the seminal vesicles contracts, releasing the seminal vesicle fluid into the ejaculatory duct.
The function of the seminal vesicles is to both produce and store fluid that will eventually become semen. This fluid comprises about 70 percent of the fluid thats released during ejaculation.
The fluid produced in the seminal vesicles provides an environment thats very important for the proper functioning and survival of sperm. The main components of this fluid are:
- fructose, a sugar that provides sperm with energy
- alkaline fluid, which helps to neutralize the acidic nature of the male urethra and the female vagina
- proteins like semenogelin, which forms a gel-like protective layer around sperm
- phosphorus and potassium, which help sperm move
- prostaglandins, hormones that have a role in lowering the female immune response to semen
Closing The Urethra During Ejaculation
During ejaculation, the prostate contracts and squirts prostatic fluid into the urethra. Here, it mixes with sperm cells and fluid from the seminal vesicles to create semen, which the body then expels.
When the prostate contracts during ejaculation, it closes off the opening between the bladder and urethra, pushing semen through at speed. This is why, in normal anatomic situations, it is impossible to urinate and ejaculate simultaneously.
Recommended Reading: Are Colon Cancer And Prostate Cancer Related
Another Common Issue: Enlarged Prostate Or Benign Prostatic Hyperplasia
Noncancerous prostate enlargement is the most common prostate problem for men over 50 years old, according to the NIDDK.
It’s not well understood what causes prostate enlargement, also known as benign prostatic hyperplasia , but research suggests age-related hormonal changes may be to blame. Men younger than 40 rarely experience symptoms of BPH.
In men with BPH, the prostate presses into and pinches the urethra as it enlarges.
This pressure can negatively affect the urine-holding bladder, which is connected to the urethra, by weakening it and preventing it from emptying completely.
Prostate enlargement can cause a number of related urination symptoms, such as:
- Increased urinary frequency and urgency
- Weak or interrupted urine stream
- Urine with an unusual color or smell
- Nocturia, or frequent urination during periods of sleep
- Pain after urination
Over time, BPH may cause complications, including urinary tract infections, damage to the bladder or kidneys, and bladder stones, among other things.
Treatment of BPH includes lifestyle changes, medication, and surgery, which may be minimally invasive.
Spongy Internal Tissue Is Key To The Reproductive Function Of The Penis
The penis is part of the male external genitalia, suspended from the body at the front and sides of the pubic arch. Internally, the penis consists of three connected columns of tissue. The paired corpora cavernosa extend together from the root of the penis through the body. The corpus spongiosum runs along the underside of the cavernosa. It contains the spongy urethra and expands past the body of the penis to form the glans penis . The tissue of the corpora cavernosa and the corpus spongiosum is spongelike in structure. During arousal and intercourse, the spaces in the tissue fill with blood. The penis stiffens. Now it can penetrate the vagina to deliver semen directly into the female reproductive system.
Also Check: Foods To Avoid For Prostate
Anatomical Position And Structure
The seminal glands are a pair of 5cm long tubular glands. They are located between the bladder fundus and the rectum .
Their most important anatomical relation is with the vas deferens, which combine with the duct of the seminal vesicles to form the ejaculatory duct, which subsequently drains into the prostatic urethra.
Internally the gland has a honeycombed, lobulated structure with a mucosa lined by pseudostratified columnar epithelium. These columnar cells are highly influenced by testosterone, growing taller with higher levels, and are responsible for the production of seminal secretions.
What Is The Main Function Of The Prostate Gland
The main function of the prostate gland is to secrete an alkaline fluid that comprises approximately 70% of the seminal volume. The secretions produce lubrication and nutrition for the sperm. The alkaline fluid in the ejaculate results in liquefaction of the seminal plug and helps to neutralize the acidic vaginal environment.
The prostatic urethra is a conduit for semen and prevents retrograde ejaculation by closing off the bladder neck during sexual climax. Ejaculation involves a coordinated contraction of many different components, including the smooth muscles of the seminal vesicles, vasa deferentia, ejaculatory ducts, and the ischiocavernosus and bulbocavernosus muscles.
Recommended Reading: Incontinence After Robotic Prostate Surgery
Urinary Tract Infections In Men: Symptoms Diagnosis And Treatment
Nonbacteria microbes may cause a different type of chronic prostatitis, known as chronic pelvic pain syndrome, which may also develop as a result of chemicals in the urine, a urinary tract infection, or pelvic nerve damage.
Affecting 10 to 15 percent of the U.S. male population, chronic pelvic pain syndrome is the most common type of prostatitis, but also the least understood.
Symptoms vary depending on the type of prostatitis, but can include urination problems, pain , fever, and body aches, among other things.
Some people develop asymptomatic inflammatory prostatitis, in which the prostate is inflamed but doesn’t produce any symptoms or require treatment.
Bacterial prostatitis is most often treated with antibiotics. Chronic pelvic pain syndrome may require drugs, surgery, and lifestyle changes.
Over time, prostatitis may cause sexual dysfunction, abscesses in the prostate, inflammation of nearby reproductive organs, and infection of the bloodstream.
Learn More About Prostate Problems and Complications
How Does The Prostate Work
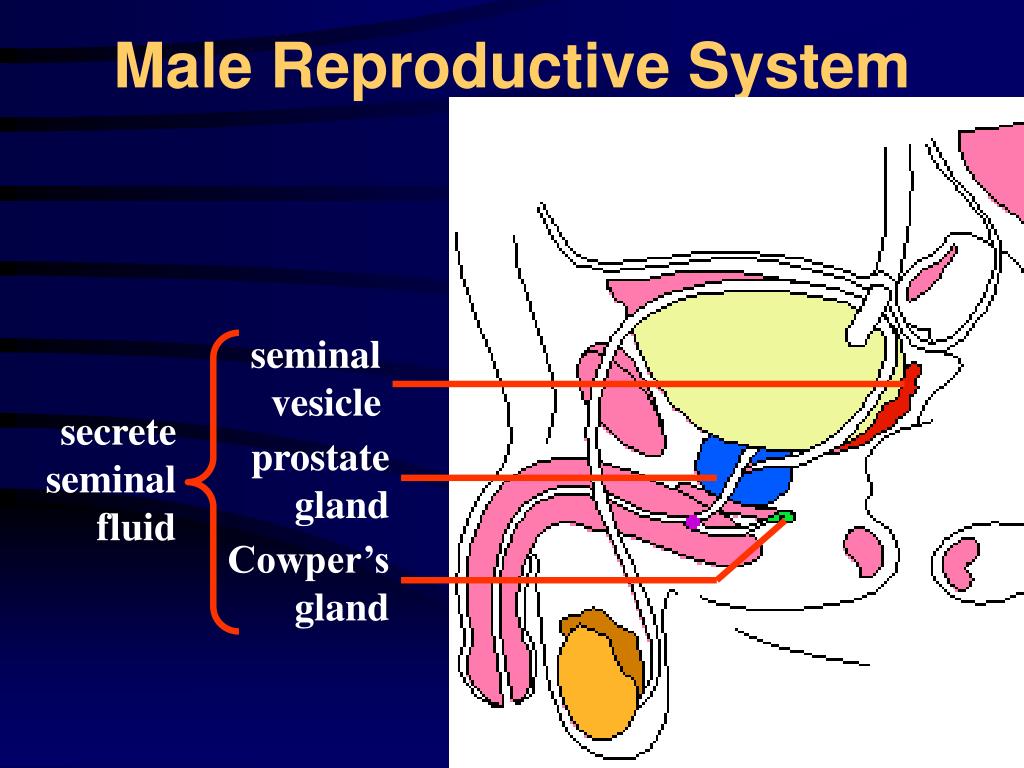
The prostate is a gland about the size of a chestnut and weighs about 30 grams . It is part of the male reproductive system and is located inside the body. The prostates most important function is the production of a fluid that, together with sperm cells from the testicles and fluids from other glands, makes up semen. The muscles of the prostate also ensure that the semen is forcefully pressed into the urethra and then expelled outwards during ejaculation.
The prostate is located directly below the bladder and above the muscles of the pelvic floor. The rectum is behind the prostate, making it possible to feel the gland from the rectum using the finger. The ducts in the prostate gland flow into the urethra, which passes through the prostate. The word prostate is taken from the Greek expression meaning one who stands before, which describes the position of the prostate gland. Viewed from below, where the urethra leaves the gland, the prostate stands before the bladder.
The tissue of the prostate gland can be divided into three different zones, listed here from innermost to outermost, which encircle the urethra like layers of an onion:
The prostate has various functions:
Production of fluid for semen:
Hormone metabolism: In the prostate the male sex hormone testosterone is transformed to a biologically active form, DHT .
Don’t Miss: Foods That Shrink Your Prostate
Clinical Relevance Examination And Investigation
Physical examination of the seminal glands through digital rectal examination is difficult.
A laboratory investigation of fructose levels in a sperm specimen may provide indirect evidence of seminal vesicle dysfunction, obstruction or congenital absence.
Try again to score 100%. Use the information in this article to help you with the answers.
bookmarksperson
Our 3D anatomical model provides you with hands-on, interactive and valuable learning tool right here on your device. To access the TeachMeAnatomy 3D Model, you must be a premium subscriber.
The seminal vesicles are a pair of glands found in the male pelvis, which function to produce many of the constituent ingredients of semen. They ultimately provide around 70% of the total volume of semen.
In this article we will consider the anatomical relations, functions, neurovascular relations and clinical significance of the seminal vesicles.
What Does The Prostate Gland Actually Do
The prostate gland isn’t essential for life, but it is vital for reproduction and is part of the male reproductive system.
The function of the prostate is to produce a slightly alkaline fluid called the prostatic fluid that makes up part of the seminal fluid, or semen.
The rest of semen is composed of sperm cells from the testicles, fluid from the seminal vesicles, and secretions from the pea-sized bulbourethral gland.
The prostatic fluid contains substances that are important to the functioning and survival of sperm cells, such as the enzyme prostate-specific antigen , which thins or loosens up semen, helping the tadpole-like sperm cells swim freely to reach the egg.
You May Like: Genetic Testing For Prostate Cancer Risk
If You Are A Trans Woman
If you are a trans woman and have had genital-gender affirming surgery as part of your transition, you still have a prostate. It is important to talk to your GP or nurse if you are worried about prostate cancer or have symptoms.
Prostate cancer UK have detailed information about trans women and prostate cancer.
The LGBT Foundation can also give you confidential advice and support. You can also talk to one of our cancer support specialists.
What Is The Primary Function Of The Male Accessory Reproductive Glands
The male accessory ducts serve to store spermatozoa and to transport them outside urethra during ejaculation. Male accessory glands are seminal vesicles, prostate glands, and bulbourethral glands which contribute seminal plasma to semen.
In this regard, what is the function of the male accessory glands?
Male accessory gland. Male accessory glands in humans are the seminal vesicles, prostate gland, and the bulbourethral glands . In insects, male accessory glands produce products that mix with the sperm to protect and preserve them, including seminal fluid proteins.
Similarly, what is the primary function of the Cowper’s glands? Cowper’s glands are pea sized glands present inferior to the prostate gland in the male reproductive system. They produce thick clear mucus prior to ejaculation that drains into the spongy urethra.
In this manner, what are the male reproductive accessory glands?
The accessory glands of the male reproductive system are the seminal vesicles, prostate gland, and the bulbourethral glands. These glands secrete fluids that enter the urethra.
What is the function of accessory glands?
Well, accessory glands are specialized structures found in males that produce fluids essential for the motility, nourishment and protection of sperm. These are the topics of today’s lesson. Males have three of these glands, and each one contributes to the production of semen.
You May Like Also
Don’t Miss: Signs Prostate Cancer Has Spread
Prostatitis: A Common Prostate Problem In Younger Men
Prostatitis, or prostate inflammation, is the most common prostatic and urinary tract problem for men under age 50, according to the National Institute of Diabetes and Digestive and Kidney Diseases . It accounts for 2 million doctor visits in the United States each year.
There are several types of prostatitis.
Prostatitis caused by bacteria is known as bacterial prostatitis, and it can cause an acute or chronic infection.
What A High Psa Level Means If Its Not Prostate Cancer
Other important components of prostatic fluid include an enzyme called prostatic acid phosphatase, citric acid, zinc, spermine and prostatic inhibin .
During an orgasm, prostate muscles squeeze the gland’s stored fluid into the urethra, where it mixes with the sperm cells and other semen components.
This expulsive process also helps propel the semen out of the body during ejaculation.
Read Also: Bladder Recovery After Prostate Surgery
What Is Seminal Fluid
Seminal fluid is the fluid emitted from the male reproductive tract. The semen contains sperm cells capable of fertilizing female eggs. It also consists of seminal plasma, i.e., other liquids that maintain the viability of sperm cells.
For centuries, scientists have been exploring seminal fluid to see how it works. The spermatozoa were first observed in ejaculate specimens in the 17th century. Until the discovery of ovum in 1827, the underlying mechanisms of human fertilization werent fully understood.
The interest in the development of technologies for seminal fluid analysis increased significantly in the early 1900s.
Scientists designed the standard methodologies for the seminal fluid analysis in the first half of the 20th century. Before the 1930s, the semen analysis was clinically unavailable. This was due to the lack of tools or methods that would test the characteristics of the sperm.
The development of methodologies offered valuable insight into the seminal fluid. They learned a lot about its functions and its relationship with mens health. Regardless of the available methodologies, the analysis of the seminal fluid is a controversial subject.
For instance, the analysis of the seminal fluid is the gold standard for evaluating sperm production and quality. But, it is a poor predictor of mens reproductive capacity. We will discuss the role of seminal fluid further in this post.