How Does Axumin Work
While normal bone scans use radioactive substances that indicate which bones are affected by cancer, Axumin links a radioactive tracer to a certain amino acid that the cancer processes much faster than ordinary cells. This tracer becomes concentrated in cancer, making it visible in bones and soft tissues as well. Salvage Radiation Therapy needs to be initiated at lower PSA levels for best results, and Axumin allows detection at these levels that standard scans do not. An earlier detection combined with a more specific treatment will yield significant benefits to patients with recurrent prostate cancer, who will be able to get a head start on their recovery and better manage their illness.
Our Expert Radiology Services are Offered in Pioneer Valley in Partnership with Baystate Health Locations.
Additional Pet Scanning Faq
Is PET scanning safe?
While PET scanning does involve the use of radioactive tracers, these are diagnostic levels of radiation that are completely safe and have no known side effects.
How long does it take to get the results after a PET Scan?
Images are captured and created during the PET scan procedure, and afterward, a radiologist will utilize their training and experience to interpret the scan and produce a written report of findings and conclusions. This report is then transmitted to your referring physician who would then review those results with you and discuss any further treatment if needed.
What is it like for a patient to have a PET Scan?
Please watch this video we created that clearly walks one through the experience of having a PET scan and answers all common questions about PET scanning.
Getting My Scan Results
Your doctor or nurse will tell you how long it will take for the results of all the tests to come back. Its usually around two weeks.
Your doctor will use your scan results to work out the stage of your cancer in other words, how far it has spread. This is usually recorded using the TNM system.
- The T stage shows how far the cancer has spread in and around the prostate.
- The N stage shows whether the cancer has spread to the lymph nodes.
- The M stage shows whether the cancer has spread to other parts of the body.
You May Like: New Radiation Treatment For Prostate Cancer
What To Expect After A Bone Scan
Bone scans do not generally cause any after effects. The dye does not remain active in your body. It passes out of your body through your urine over about 24 hours. You may be instructed to take special precautions after urinating, to flush the toilet twice and to wash your hands thoroughly. You will be advised to drink plenty of water for a day after the scan to help flush the dye out of your system.
Recommended Reading: Cialis For Prostatitis
Summary Of The Main Findings
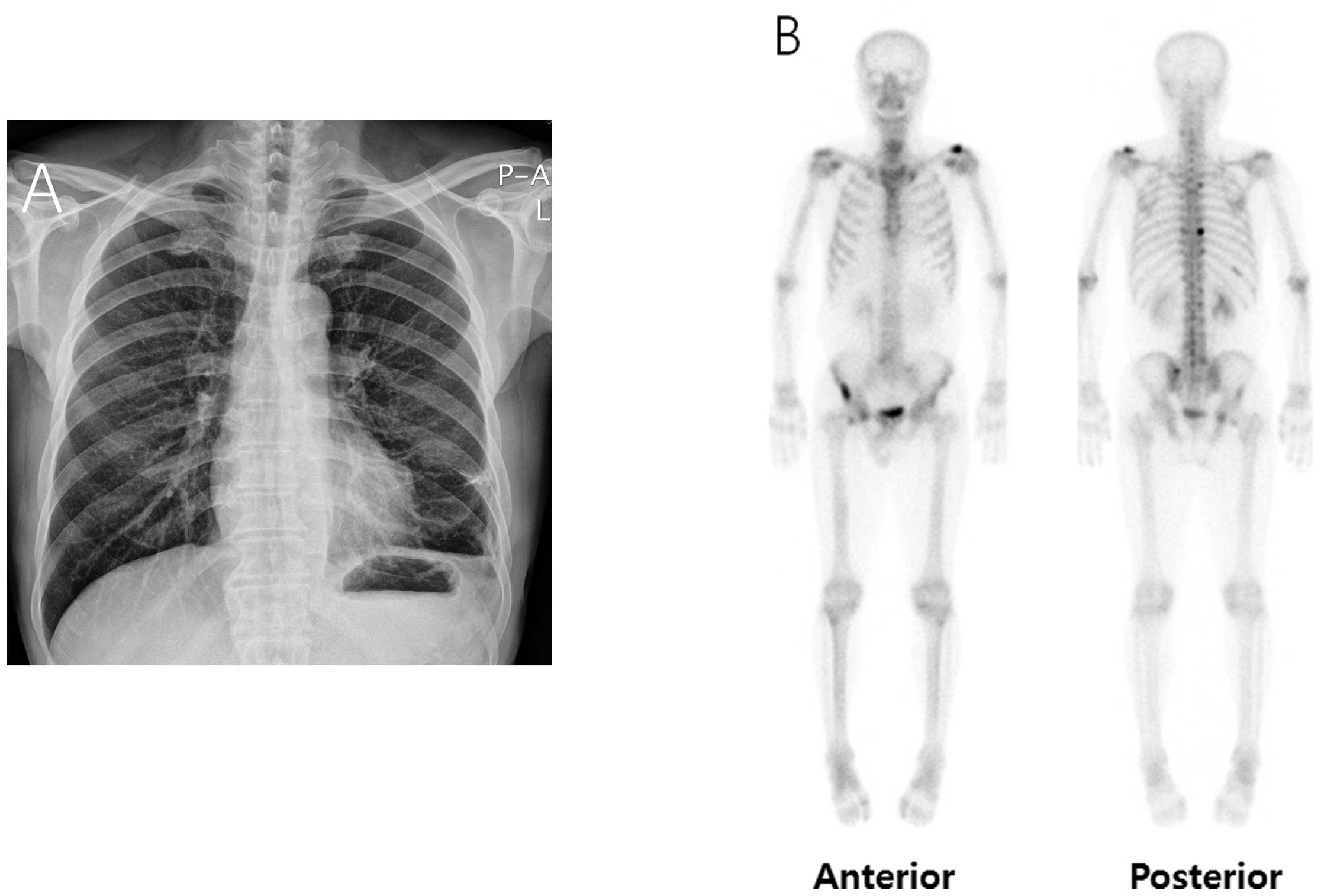
The most thoroughly validated tests in clinical trials and in clinical practice are the good old tests such as bone scan and contrast-enhanced thorax, abdomen, and pelvis CT.
Nevertheless, most of the evidence based for bone scan and CT are old and retrospective. There is actually a much larger amount of prospective data for modern PET/CT. Prospective data also shows clear superiority of PSMA-PET or fluciclovine-PET to choline-PET. Data from a new study suggests that PSMA-PET imaging is superior to fluciclovine-PET for detecting biochemical recurrence in men with prostate cancer . However, whether one of these radiotracers improves patient survival over the other is unknown and further research is needed to determine which has the greater effect.
The new tracers do not have the same accessibility and need further validation in clinical trials to evaluate their benefits and clarify their usage in routine clinical practice. It is important that we consider the imaging requirements of the PCWG as this defines the imaging definitions for subjects in those clinical trials. EORTC algorithms also need to be considered for the imaging strategies. Experts in nuclear medicine and radiology should be represented in medical decision-making teams for PCa.
Read Also: What Is The Gleason Score For Prostate Cancer
What Do My Scan Results Mean
Your TNM stage is used to work out if your cancer is localised, locally advanced or advanced. This can help your doctor see how far it has spread and which treatment might be suitable for you.
Cancer that’s contained inside the prostate. Sometimes called early prostate cancer. Possible TNM stages are:
- T stage: T1 or T2
- N stage: N0 or NX
- M stage: M0 or MX.
Cancer that’s started to break out of the prostate, or has spread to the area just outside it. Possible TNM stages are:
- T stage: T1 or T2
- N stage: N1
- T stage: T3 or T4
- N stage: N0 or N1
- M stage: M0.
Local Detection And Primary Staging
More than 90% of primary PCa lesions show moderate to high PSMA expression levels on PSMA PET , and many current studies have indicated that PET/MRI could be the single ideal imaging modality for staging PCa patients ,,. There are already proposed protocols that are potentially viable for routine clinical application that have Prostate Imaging Reporting and Data System 2.0-compliant multiparametric MRI acquisitions of the prostate bed and whole-body PSMA PET .
The MRI component is the imaging modality of choice for precise morphologic evaluation and has higher spatial resolution and provides clearer anatomic delineation of the prostatic fossa and surrounding anatomical structures than PET , while PSMA PET is the superior modality for detecting metastases to the locoregional and extrapelvic lymph nodes, bones and visceral organs .
Consequently, PSMA PET/MRI yields greater diagnostic accuracy for PCa localization than multiparametric MRI or PET alone. These encouraging data indicate that hybrid imaging using morphologic, functional, and molecular information enhances diagnostic performance in patients with PCa for TNM staging .
T Staging
Multimodal evaluation might facilitate biopsy orientation and lead to an impact on management, especially for predicting and monitoring tumor aggressiveness during active surveillance, determining more important targets when planning radiation therapy and planning appropriate surgical technique and intraoperative management.
N Staging
Recommended Reading: Monoclonal Antibody Therapy For Prostate Cancer
Developing Landscape For Non
Non-metastatic CRPC prevalence has been estimated at 7% of PCa in the European Union . Owing to the advent of modern imaging, the prevalence of this subgroup has declined. These newer imaging agents i.e., fluciclovine or PSMA can identify local recurrence or metastases at PSA levels far below the traditional PSA threshold for other imaging modalities such as CT or bone scan. Some of the new PET agents can identify metastatic lesions at PSA values as low as 0.20.5 ng/mL, allowing the prompt identification of M1 CPRC . This is interesting given the recent randomized studies in this field , which show the efficacity of apalutamide and enzalutamide . The metastasis-free survival of patients with nmCRPC was previously estimated as ~2530 months, but can now be significantly prolonged using combination next-generation hormone therapy with ADT . The use of PSA doubling time to determine risk for progression can guide the appropriate timing for starting therapy. For instance, a PSA doubling time 10 months is appropriate to initiate therapy. There is no currently established standard of care option for treatment of this population, hence the need for enrollment in clinical trials .
When Is The Psma Pet Test Used
Your doctor might order a PSMA PET scan if youve recently received a new diagnosis of prostate cancer and they think it may have spread to other parts of your body. Or your doctor may use it to get a better idea of where prostate cancer has spread.
Prostate cancer is usually diagnosed in its early stages, before it has spread. However, some people are at heightened risk of metastatic prostate cancer.
Your doctor might order PSMA PET-CT at the time you are diagnosed with prostate cancer if you have any risk factors for metastatic disease, Dr. Michael Feuerstein, a urologist at Lenox Hill Hospital in New York City, tells Healthline.
According to Feuerstein, doctors use the following measurements to assess the risk of metastatic prostate cancer:
- Prostate-specific antigen . PSA is a protein made by the prostate thats found in the semen and blood. It tends to be elevated in people with prostate cancer. A PSA blood test is one of the first tests doctors order to diagnose prostate cancer. Youre considered at risk of metastatic prostate cancer if you have a PSA blood level of 20 or higher.
- Gleason grade. This system assigns a score to classify how many abnormal prostate cancer cells are found in a tissue biopsy. A Gleason grade of 7 or higher puts you at higher risk of metastatic prostate cancer.
Your doctor might also order the PSMA PET test if you still have detectable prostate cancer after undergoing surgery to treat it, says Feuerstein.
Also Check: How To Get A Biopsy Of The Prostate
How Long Does The Test Take
A whole body bone scan takes around 3-4 hours, which includes two separate visits. In the first visit you will be given an injection of a radioactive isotope into a vein in your arm. There are no side effects to this injection. The isotope takes 2-3 hours to circulate in the blood and get absorbed in the bone. You will be given a time to return to the Nuclear Medicine Department 2-3 hours after the injection. When you arrive for the second part you will be asked to use the restroom to empty your bladder. You will then be asked to remove all external metal and lay flat on our imaging table for a 30 minute scan from head to toe. We will then review these images with our nuclear radiologist to make sure we have all the information we need. Some additional images may be required.
How Do Nuclear Scans Work
In most cases youre given a tracer that sends out small doses of radiation. Some are swallowed while others are put into a vein or inhaled as a gas.
Over time the tracer collects in the part of the body thats being tested. This can take from a few seconds to several days. The collected tracer sends out gamma rays that are picked up by a special camera . The signals are processed by a computer, which turns them into 2- or 3-dimensional pictures, sometimes with color added for extra clarity. A radiologist or a doctor who specializes in nuclear medicine interprets the pictures and sends a report to your doctor.
These nuclear medicine scans are commonly used for cancer:
Bone scans: Bone scans look for cancers that may have spread from other places to the bones. They can often find bone changes much earlier than regular x-rays. The tracer collects in the bone over a few hours, then the scans are done.
Positron emission tomography scans: PET scans usually use a form of radioactive sugar. Body cells take in different amounts of the sugar, depending on how fast they are growing. Cancer cells, which grow quickly, are more likely to take up larger amounts of the sugar than normal cells. Youll be asked to not drink any sugary liquids for several hours before the test.
You May Like: Treatment Plan For Prostate Cancer
Improved Imaging For Prostate Cancer Withpsma Pet
Neil Osterweil
In men with newly diagnosed high-risk prostate cancer, a new imaging technique was significantly more accurate than the currently used conventional approach in determining the extent of disease, concludes a randomized trial conducted in Australia comparing the two methods.
A US expert says the novel imaging technique represents a major clinical advance.
“It is absolutely a game-changer for men with prostate cancer,” commented Andrei Iagaru, MD, chief of nuclear medicine and molecular imaging at Stanford Health Care in California.
“It has been shown in many studies that it is more sensitive and specific than conventional imaging in the scenario of biochemical recurrence as well as for initial diagnosis and staging prior to surgery,” he told Medscape Medical News.
Iagaru was not involved in the Australian study, but he has conducted clinical trials of PET-CT using a different prostate-specific membrane antigen radiotracer than the one used there.
The Australian proPSMA trial was conducted in 300 men with biopsy-proven prostate cancer with high-risk features. The new technique had a 27% greater accuracy than CT and bone scan for diagnosing pelvic nodal or distant metastatic disease, reported Michael S. Hofman, MBBS, from the Peter MacCallum Cancer Center in Melbourne, Australia, and colleagues.
“PSMA PET-CT is a suitable replacement for conventional imaging, providing superior accuracy, to the combined findings of CT and bone scanning,” they conclude.
What Is It Like Having A Nuclear Scan
![(A) [ 99m Tc]MDP bone scan and (B) FDG (A) [ 99m Tc]MDP bone scan and (B) FDG](https://www.prostateprohelp.com/wp-content/uploads/a-99m-tcmdp-bone-scan-and-b-fdg-pet-mip-image-of-a.png)
In most cases you will be given a tracer that sends out small doses of radiation. If its put into your blood, a needle will be used to put it into a vein in your hand or arm.
Because of the special materials and equipment needed, these scans are usually done in the radiology or nuclear medicine department of a hospital. You might be able to wear your own clothing or you might be given a gown to wear during the test. Youll need to remove all jewelry or metal items that could interfere with the scans.
The scanner has a hole in the middle and looks like a large doughnut. You lie on a padded table which moves back and forth through the hole in the scanner. You will need to be very still while the scans are done. The technician may ask you to change positions to allow different views to be taken. The table may become uncomfortable after a while.
For a thyroid scan, you may sit in a chair that faces the scanner. The scanner is set up so that its right in front of your neck and your chin rests on top of it.
To get a MUGA scan, you lie on a flat table and a large camera is positioned above your chest.
Also Check: Why Is Prostate Cancer So Common
Improving Pet Scans Are Good News For Doctors And Patients Alike
- By Charlie Schmidt, Editor, Harvard Medical School Annual Report on Prostate Diseases
A recent blog post discussed a newly approved imaging agent with an unwieldy name: gallium-68 PMA-11. Delivered in small amounts by injection, this minimally radioactive tracer sticks to prostate cancer cells, which subsequently glow and reveal themselves on a positron emission tomography scan. Offered to men with rising PSA levels after initial prostate cancer treatment , this sort of imaging can allow doctors to find and treat new tumors that they might otherwise miss. With currently available imaging technology, such tumors could potentially escape detection until they were larger and more dangerous.
But while gallium-68 PMA-11 is the latest PET tracer to win FDA approval, not everyone can get it. In the United States, its currently available only to patients treated at the University of California, Los Angeles, or the University of California, San Francisco, where the tracer is manufactured. However, two other PET tracers approved for prostate cancer imaging in the US are becoming more accessible.
In January 2021, a team at Stanford University published findings showing that one those tracers, called fluciclovine F18 , identified significantly more metastatic cancers than other conventional types of imaging. Axumin was approved in 2016, and these are among the first data to show how well the tracer performs in real-world settings.
How Do I Get Ready For A Nuclear Scan
The steps needed to prepare for a nuclear medicine scan depend on the type of test and the tissue that will be studied. Some scans require that you dont eat or drink for 2 to 12 hours before the test. For others, you may be asked to take a laxative or use an enema. Be sure your doctor or nurse knows everything you take, even over-the-counter drugs, vitamins, and herbs. You may need to avoid some medicines before the test. Your health care team will give you instructions.
Reactions to the radioactive material are very rare. Still, be sure to tell your doctor about any allergies and if youve had problems with nuclear medicine scans in the past.
You may get the radioactive material anywhere from a few minutes to many hours before the test. For example, in a bone scan, the tracer is put into a vein in your arm about 2 hours before the test begins. For gallium scans, the tracer is given a few days before the test.
You May Like: Do Men Need A Prostate
Imaging For Metastasis In Prostate Cancer: A Review Of The Literature
- 1Department of Medical Oncology, CHU Lille, Lille, France
- 2Univ. Lille, CNRS, Inserm, CHU Lille, Institut Pasteur de Lille, UMR9020 UMR-S 1277 Canther – Cancer Heterogeneity, Plasticity and Resistance to Therapies, Lille, France
- 3Medical Oncology Department, Centre Oscar Lambret, Lille, France
- 4Nuclear Medicine Department, CHU Lille, Lille, France
- 5Academic Department of Radiation Oncology, Centre Oscar Lambret, Lille, France
- 6CRISTAL UMR CNRS 9189, Lille University, Villeneuve-d’Ascq, France
- 7Department of Urology, CHU Lille, Lille, France
- 8Department of Radiology, CHU Lille, Lille, France
Background: Initial staging and assessment of treatment activity in metastatic prostate cancer patients is controversial. Indications for the various available imaging modalities are not well-established due to rapid advancements in imaging and treatment.
Methods: We conducted a critical literature review of the main imaging abnormalities that suggest a diagnosis of metastasis in localized and locally advanced PCa or in cases of biological relapse. We also assessed the role of the various imaging modalities available in routine clinical practice for the detection of metastases and response to treatment in metastatic PCa patients.
In routine clinical practice, conventional imaging still have a role, and communication between imagers and clinicians should be encouraged. Present and future clinical trials should use modern imaging methods to clarify their usage.
Who Does A Bone Scan
A specially trained and certified nuclear medicine technologist performs the test. A nuclear medicine physician is a medical doctor who uses tracers to diagnose and treat disease. A radiologist or a nuclear medicine physician oversees the technologist. A radiologist is a medical doctor who uses imaging tests to diagnose disease. One of these doctors will read your scan and decide what it means.
You can have a bone scan done at:
-
A hospital’s radiology or nuclear medicine department
-
An outpatient imaging center
Don’t Miss: What Are The Early Warning Signs Of Prostate Cancer