What Are The Procedures For Surgery Of Enlarged Prostate
The most commonly performed surgery for enlarged prostate is transurethral resection of the prostate .
This surgical procedure involves the insertion of a scope or an instrument through the penis to scrap the innermost portion of the prostate piece by piece. This is believed to be the most effective surgical procedure since it can relief your symptoms immediately as well.
Another procedure of enlarged prostate surgery is transurethral incision of the prostate .
This operation resembles TURP, but it is indicated when the size of prostate enlargement is relatively small. It is a non-invasive surgical procedure which means that you will not need to be hospitalized after it.
Similar to TURP, a scope is introduced through the penis till reaching the prostate afterward a small cut is done to widen the hole of urethra as well as bladder opening, rather than completely getting rid of prostate in TURP.
In Simple prostatectomy a small incision is performed in the abdominal area to remove the inner most part of the enlarged prostate, while the superficial part is left.
Simple prostatectomy is definitely performed under general anesthesia. This enlarged prostate surgery involves prolonged procedures and you will need to be hospitalized from five to ten days after having it.
Nowadays there are myriad less invasive techniques to treat prostate enlargement which can be done in your doctors clinic under local anesthesia or other sedations, you will not need to be hospitalized.
New Device Offers Less Invasive Treatment For Enlarged Prostate
A new medical device offers an alternative to open surgery and drugs for the treatment of benign prostatic hyperplasia.
A new medical device offers a less invasive way to treat symptoms caused by an enlarged prostate.
This walnut-sized gland in men sits below the bladder and surrounds the urethra, the tube that carries urine from the bladder out of the body.
As a man ages, it is common for the prostate to grow, a condition called benign prostatic hyperplasia . This rarely causes symptoms before age 40, but in older men the growing prostate can press on the urethra and reduce or block the flow of urine.
The U.S. Food and Drug Administration recently approved the marketing of the UroLift system, a permanent implant that has been shown to relieve symptoms of an enlarged prostate in men 50 years or older.
, over half of men in their sixties and almost 90 percent of men in their seventies have some symptoms of BPH, which include:
- more frequent urination, especially at night
- weak, hesitant, or interrupted stream of urine
- urgent need to urinate
- leaking or dribbling during or after urination
Severe BPH can lead to the retention of urine and strain on the bladder. Left untreated, this can cause urinary tract infections, damage to the bladder or kidneys, or difficulty controlling urine .
Current treatment options for BPH include open surgery, minimally-invasive surgery, and drug therapy.
Benefits And Risks Of The New Treatment
Other minimally-invasive therapies for BPH also access the prostate through the urethra, making the UroLift system similar in this respect. The other procedures, however, involve cutting or burning away excess prostate tissue. UroLift uses only a needle and suture to pull back the prostate tissue.
UroLift is also less invasive than open surgery, a procedure that requires the surgeon to make an incision in the lower abdomen. Open surgery has a greater risk of side effects, but is generally only used for men who have a very large prostate, damage to the bladder, or complicating conditions such as bladder stones.
The side effects reported by men treated with the UroLift system were all minor, and included:
- pain or burning during urination
- blood in urine
- frequent or urgent need to urinate
- incomplete emptying of the bladder
Rare complications, however, can occur when the UroLift procedureor any surgeryis done using general anesthesia, especially in older men or those with serious medical problems. Serious complications may include lung infections, temporary mental confusion, heart attack, stroke, or death.
Also Check: What Can You Do To Help An Enlarged Prostate
Laser Focal Therapy: What To Expect
You will receive both email and phone contact information for our medical team so that you can always reach us. In addition, we conduct a pre-operative consultation prior to the procedure, we meet the day of the procedure, and will see you frequently in follow-up.
Our team will have collected and reviewed your medical records to evaluate you for inclusion and suitability. Our surgical team will have discussed your case during Tumor Board and conducted a surgical plan based on size, number, shape and location of ablation areas. Prior to the procedure, we will review the Informed Consent Document with you to ensure you understand every aspect of the procedure. We will discuss the risk, benefits, and paperwork of the procedure.
The day of the procedure, our nurse will place an intravenous catheter in your arm so that she/he can administer IV antibiotics, pain medications and fluids . Should other medications be necessary, they will be administered through this IV as well.
You may have a urinary catheter placed so that we can provide cooled urethral saline through Continuous Bladder Irrigation protection. This catheter remains in place depending on the size, shape, and location of treatment. Our urologist will perform the insertion and removal.
Patients will return home or to their hotel room after at least two hours in the recovery room that same day. They must be accompanied by a family member or care giver as driving is not permitted.
Getting Ready For Your Surgery
You and your care team will work together to get ready for your surgery.
Help us keep you safe during your surgery by telling us if any of the following statements apply to you, even if you arent sure.
- I take a blood thinner, such as:
- Aspirin
About drinking alcohol
The amount of alcohol you drink can affect you during and after your surgery. Its important to talk with your healthcare providers about how much alcohol you drink. This will help us plan your care.
- If you stop drinking alcohol suddenly, it can cause seizures, delirium, and death. If we know youre at risk for these complications, we can prescribe medications to help keep them from happening.
- If you drink alcohol regularly, you may be at risk for other complications during and after your surgery. These include bleeding, infections, heart problems, and a longer hospital stay.
Here are things you can do before your surgery to keep from having problems:
About smoking
If you smoke, you can have breathing problems when you have surgery. Stopping even for a few days before surgery can help. Your healthcare provider will refer you to our Tobacco Treatment Program if you smoke. You can also reach the program by calling .
About sleep apnea
Please tell us if you have sleep apnea or if you think you might have it. If you use a breathing device for sleep apnea, bring it with you the day of your surgery.
Ask about medications
Recommended Reading: How Does A Urologist Check For Prostate Cancer
New Treatments For Enlarged Prostate Show Success
According to Harvard Medical School, by the age 60, half of all men will have an enlarged prostate, a condition also known as benign prostatic hyperplasia or BPH. By age 85, that proportion reaches 90 percent.
Thats the bad news.
The good news, according to Dr. Hugo Davila, one of Vero Beachs top urologists as well as a robotic and pelvic reconstruction surgery specialist, is there are multiple options for treating BPH, including two new procedures called Rezum and UroLift that are delivering excellent results.
The first step that we always do, says Davila, who is with Florida Healthcare Specialists, is try what we call behavioral changes.
What that means is we look into your diet and then if you tell me, Hey, Dr. Davila, I love to drink coffee. I like tea. I drink Coke, I may say, Well, we need to stop that because maybe the frequency, the urgency, the waking up at night is due to that. About 30 to 35 percent of the time well fix the problem just by looking to the diet.
Before going on to discuss other treatments, Davila is quick to quash one major misconception about the condition: BPH is not a symptom or precursor of prostate cancer. In fact, it doesnt even marginally raise your risk of getting prostate cancer.
One, he says, is retrograde ejaculation, meaning that when the man has an orgasm and an ejaculation, rather than going forward, it will go backward into the bladder.
The effects of both procedures tend to last about five years.
Radical Prostatectomy Retropubic Or Suprapubic Approach
You’ll be positioned on the operating table, lying on your back.
An incision will be made from below the navel to the pubic region.
The doctor will usually perform a lymph node dissection first. The nerve bundles will be released carefully from the prostate gland and the urethra will be identified. The seminal vesicles may also be removed if necessary.
The prostate gland will be removed.
A drain will be inserted, usually in the right lower area of the incision.
You May Like: What Can Cause Your Prostate To Swell
Risks Of Radical Prostatectomy
Radical prostatectomy has a low risk of serious complications. Death or serious disability caused by radical prostatectomy is extremely rare.
Important nerves travel through the prostate on the way to the penis. Skilled surgeons can usually protect most of these nerves during radical prostatectomy. Still, complications from inadvertent nerve damage do occur after radical prostatectomy. They include:
- Urinary incontinence: More than 95% of men younger than age 50 are continent after radical prostatectomy. Around 85% of men aged 70 or older maintain continence after the operation.
- Erectile dysfunction : Problems with erections are common after prostatectomy. Still, most men are able to have sex after prostatectomy while using medicines for ED , an external pump, or injectable medications. The younger the man, the higher the chance of maintaining potency after prostatectomy. A period of penile rehabilitation is often necessary.
Much of the skill involved in radical prostatectomy centers on sparing these nerves during the operation. A man undergoing radical prostatectomy by a surgeon at an advanced prostate cancer center has a better chance of maintaining sexual and urinary function.
Other complications of radical prostatectomy include:
- Bleeding after the operation
Harvard Experts Discuss Surgical Options For Benign Prostatic Hyperplasia
Benign prostatic hyperplasia is one of the most common disorders affecting men as they grow older. Yet there is much confusion about the best way to treat this disorder surgically, in part because it seems that every year, a new surgical option is introduced.
Harvard editors invited three experts to participate in a roundtable discussion to share their thoughts about the relative benefits and risks of current surgical treatments for BPH.
| Note: Men who decide to undergo surgery to relieve BPH symptoms have multiple options to choose from. Our panel of Harvard experts discusses the most common options, which are briefly defined below. See Table 3 for a comparison of recovery rates and other considerations. |
The panel consisted of these experts:
Transurethral resection of the prostate . Still the most common form of surgery, TURP is often inelegantly referred to as the Roto-Rooter technique. This procedure takes place in an operating room under general or spinal anesthesia. During the procedure, the surgeon uses an instrument called a resectoscope to view the prostate . The surgeon threads the resectoscope through the penis to the prostate, then uses the electrical loop to cut away the overgrown tissue thats pressing against the urethra.
Read Also: How To Fix A Swollen Prostate
Alternative Prostate Cancer Treatment
If youre exploring alternative prostate cancer treatment options, youve come to the right place. For over 23 years, weve offered men new treatment options for prostate cancer. And while conventional treatment for prostate cancer usually involves surgery, radiation and chemotherapy, we offer a gentler, less toxic approach.
Our clinic offers a combination of both conventional and alternative treatments for prostate cancer. This combination has been shown to be effective for a variety of cancers over two decades.
We offer a powerful integrative and complementary treatment for prostate cancer. This means we can use conventional approaches as needed but we also use very powerful alternative & holistic cancer treatments as well.
Our treatments are designed to fight cancer, strengthen your immune system and change the underlying conditions of the body so it can muster its full healing potential. We also work on the underlying reasons why your body may have become predisposed in the first place.
What Is The Urolift System
Treatment with the UroLift® System is typically a one-time, in-office solution that provides rapid relief and recovery of BPH symptoms.1 It can break the cycle of medications and how they make a person feel, all without the risks of more invasive surgery. The goal of the UroLift System treatment is to relieve symptoms so you can get back to your life and resume your daily activities.
The UroLift System treatment has demonstrated a significant improvement in quality of life for patients compared to medications.2,3 The UroLift System is the only BPH procedure shown not to cause new and lasting erectile or ejaculatory dysfunction*, while being a safe and effective treatment of lower urinary tract symptoms due to BPH.1,3-6
Recommended Reading: How Do Prostate Cancer Patients Die
What Are Other Benign Prostatic Hyperplasia Surgery Options
If your symptoms are severe or minimally invasive surgical treatments dont help with your enlarged prostate, your doctor will likely recommend another kind of surgery. Other prostate procedures include:
Transurethral resection of the prostate : This is the most common treatment for BPH. During this procedure, your urologist will insert a rigid instrument called a resectoscope into the urethra. This is why it is called transurethral. Inserting the scope this way means no cutting into the prostate. They will then use the charged resectoscope to remove the excess tissue that is blocking the urine from leaving the bladder.
You may be put to sleep with general anesthesia. Local anesthesia for the lower part of the body may be used for this procedure. The average in hospital stay for TURP is 1 to 2 days.
Transurethral incision of the prostate : This is a similar procedure to TURP. Instead of prostate tissue being removed the bladder neck and prostate are cut to relax the bladder opening, allowing urine to flow more freely. TUIP is most successful on men with smaller prostates.
Simple prostatectomy: This method is a surgical procedure in which an incision is made through the abdomen or performed laporoscopically. The inner portion of the prostate gland is removed, leaving the outer segment intact.
Fda Approves The New Device
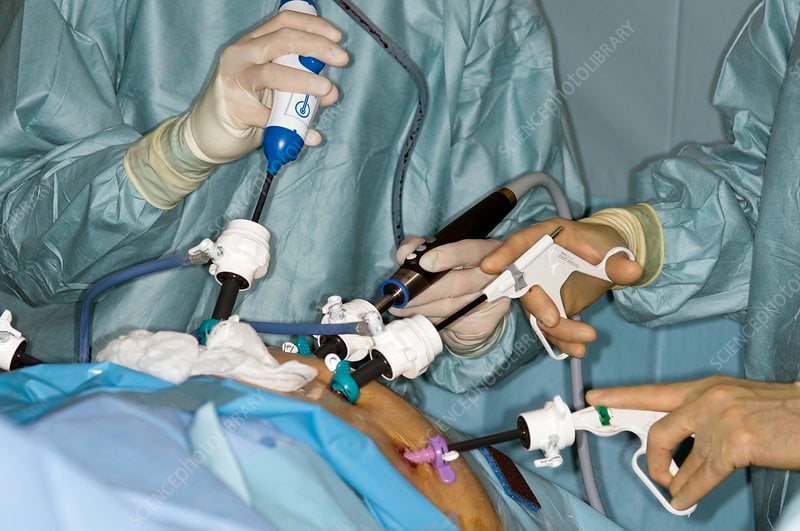
One of the main benefits of UroLift is that it offers men with BPH a less-invasive option than open surgery, with no incisions and no cutting or burning away of the prostate tissue. In addition, the results of the procedure can be seen immediately afterwards.
The FDA review was based on two clinical studies of men with BPH who were implanted with two or more UroLift sutures. In both studies, surgeons were able to insert the sutures in 98 percent of cases.
The larger study, published in June in the Journal of Urology, involved 206 men with BPH. The procedure, which is done under local or general anesthesia, took 66 minutes to perform on average.
Twelve months after treatment, men with the UroLift sutures had improved urine flow and were better able to empty their bladders. They also reported a decrease in their symptoms and an increase in their quality of life.
Also Check: What Is The Treatment For Prostate Cancer That Has Spread
Prostate Surgery: What To Expect On The Day Of Surgery
There are a few prostate surgery types and techniques, and what you can expect from your procedure depends on which one your surgeon uses. An incision may or may not be required all, some, or none of prostate gland may be removed and some surrounding tissue may or may not be excised as welljust to name a few differences.
The choice in prostate surgery largely comes down to whether you are having it to treat prostate cancer or the urinary symptoms or complications of an enlarged prostate, a.k.a. benign prostatic hyperplasia .
What Is A Prostatectomy
A prostatectomy is a surgical procedure for the partial or complete removalof the prostate. It may be performed to treatprostate cancerorbenign prostatic hyperplasia.
A common surgical approach to prostatectomy includes making a surgicalincision and removing the prostate gland . This may beaccomplished with either of two methods, the retropubic or suprapubicincision , or a perineum incision .
Prior to having a prostatectomy, it’s often necessary to have aprostate biopsy. Please see this procedure for additional information.
Prostate Cancer: Treatment Advances You Should Know About
Prostate cancer treatment has entered the robotics age. Using advancedrobotic technology, Johns Hopkins surgeons can see the prostate in 3-D,magnifying everything 10 times. Johns Hopkins urologist Mohamad Allaf, M.D., explains what this means for patients, including fewer side effects.
Also Check: How Would You Know If You Have Prostate Cancer
Treatments Options For High
The prostate is a walnut-sized organ that is part of the male reproductive system. It sits in front the bladder and above the rectum. The prostate is responsible for the production and supply of fluid that helps nourish sperm in the ejaculate. The urethra, where urine travels from the bladder to the penis, runs through the prostate.
As a result of family history, lifestyle, diet, and natural hormonal changes, the prostate begins to grow in size as men age, starting in their mid-30s. When the prostate becomes more enlarged over time, it might press against the urethra and block urine flow . This condition is called benign prostatic hyperplasia, or BPH.
Enlarged prostates differ in size. The size can be estimated on digital rectal exam or prostate imaging like an ultrasound. People with very enlarged prostates have several treatment options. However, size is not the only factor used to choose a treatment.
When doctors evaluate the prostate, symptoms are just as important as size. In addition, size and symptoms donât always correspond. For example, one person might have a mildly enlarged prostate with noticeable symptoms, while another person could have a very large prostate with no symptoms.
All of this information is the basis of a personalized treatment plan. Here are the options for patients with very enlarged prostates, with or without symptoms.