When Do I Need A Biopsy
Your doctor may order a biopsy if your prostate-specific antigen level in your blood work is elevated or there is an abnormal lump found during a digital rectal exam. During a digital rectal exam, your doctor inserts a finger up your bottom to feel if your prostate is enlarged or has bumps. Another option before a biopsy is an ultrasound. Instead of a finger, a small probe is inserted to take pictures of the prostate.
An MRI-guided prostate biopsy may be used in patients who have a rising PSA level, yet a negative ultrasound-guided biopsy. It also may be used in situations where a diagnostic prostate MRI performed because of rising PSA demonstrates a very small abnormality that may not be easily targeted by ultrasound. An MRI image to guide a biopsy can improve the ability to detect prostate tumors which may require treatment.
When Is A Psa Test Needed
If you are age 50 to 74, you should discuss the PSA test with your doctor. Ask about the possible risks and benefits.
Men under 50 or over 75 rarely need a PSA test, unless they have a high risk for prostate cancer.
- You are more likely to get prostate cancer if you have a family history of prostate cancer, especially in a close relative such as a parent or sibling.
- Your risks are higher if your relative got prostate cancer before age 60 or died from it before age 75. These early cancers are more likely to grow faster.
- If you have these risks, you may want to ask your doctor about getting the PSA test before age 50.
This report is for you to use when talking with your healthcare provider. It is not a substitute for medical advice and treatment. Use of this report is at your own risk.
04/2014
What Does My Prostate Do
The prostate is beneath the bladder and in front of the rectum. Itâs a walnut-shaped gland that surrounds part of the urethra. . Hereâs what it does:
- It produces fluid for semen, which includes sperm produced in the testicles.
- It prevents urine from being included during ejaculation.
If it gets too big, your prostate can block pee from passing through the urethra and out the penis.
Also Check: How To Reduce Prostate Swelling Naturally
What Is A Transperineal Biopsy
This is where the doctor inserts the biopsy needle into the prostate through the skin between the testicles and the back passage . In the past, hospitals would only offer a transperineal biopsy if other health problems meant you couldnt have a TRUS biopsy. But many hospitals have stopped doing TRUS biopsies and now only do transperineal biopsies.
A transperineal biopsy is normally done under general anaesthetic, so you will be asleep and wont feel anything. A general anaesthetic can cause side effects your doctor or nurse should explain these before you have your biopsy. Some hospitals now do transperineal biopsies using a local anaesthetic, which numbs the prostate and the area around it, or a spinal anaesthetic, where you cant feel anything in your lower body.
The doctor will put an ultrasound probe into your back passage, using a gel to make this easier. An image of the prostate will appear on a screen, which will help the doctor to guide the biopsy needle.
If youve had an MRI scan, the doctor may just take a few samples from the area of the prostate that looked unusual on the scan images. This is known as a targeted biopsy.
Comparison Of Pain Scores Between Groups
Our study showed that patients reported a higher pain score at insertion of the TRUS probe in the PPNB group compared to the CB group, though this was not statistically significant. Similarly, Urabe et al. reported a statistically significant higher average pain score at the point of probe insertion for PPNB+IRLA group compared to the CB+IRLA group. This is probably due to the fact that insertion of the TRUS probe precedes the administration of the PPNB in the PPNB group, while the administration of CB preceded probe insertion which also had the effect of relaxing the anal sphincter. This point may confer an advantage on CB over PPNB as analgesia for prostate biopsy.
There was no significant difference in the experience of pain at administration of block in our study. However, Urabe et al. reported a significantly higher average pain score of 2.9±2.1 in the CB+IRLA group than in the PPNB+IRLA group at the moment of administering the analgesia. This could have been as a result of the fact that in their study, IRLA was instilled prior to the administration of PPNB.
Table 4 Protocols, findings and conclusions of studies that compared CB with PPNB
Recommended Reading: How To Stop Leaking After Prostate Surgery
Also Check: What Can You Do To Help An Enlarged Prostate
Things To Know Before Getting A Prostate Biopsy
What Will I Experience During And After The Biopsy
If you receive IV contrast for the MRI-guided procedure, you may feel coolness and a flushing sensation for a minute or two when the contrast material is injected. The intravenous needle may cause you some discomfort when it is inserted and you may experience some bruising once it is removed.
Rarely, patients may experience side effects from the MR contrast material, including nausea and local pain, hives, itchy eyes or other reactions. If you experience allergic symptoms, a radiologist or other physician will be available for immediate assistance.
When the ultrasound probe or endorectal coil is inserted into the rectum, you will feel pressure and may have some temporary discomfort.
You will hear a clicking noise when the biopsy needle samples the prostate, and you may feel a stinging or burning sensation in the area.
Some patients find it uncomfortable to remain still during MR imaging. Others experience a sense of being closed-in . Therefore, sedation can be arranged for those patients who anticipate anxiety.
If you feel heating on your skin at any time during MR imaging, the MR technician should be notified so that they can perform a closer examination of the area.
Some patients experience a small amount of bleeding from the rectum or perineum immediately after the biopsy procedure. If this occurs, it will cease with gentle pressure.
You may feel pain and discomfort in the area of the prostate for a day or two after the biopsy, particularly when you are seated.
Also Check: Prostate Cancer And Blood In Urine
Dr Dan Sperling Speaks Out About Robotic Surgery Proton Beam
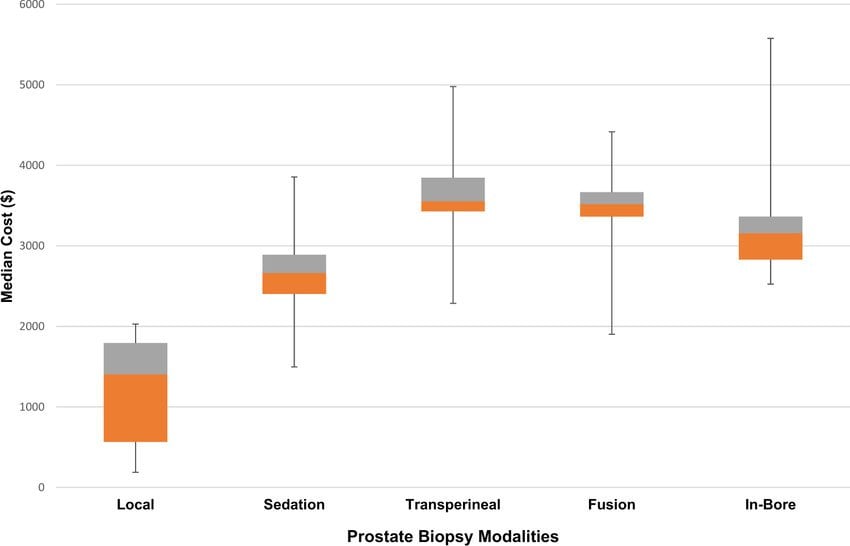
What makes an expensive prostate cancer treatment worth its cost? Dr. Dan Sperling, an authority on minimally invasive, MRI-guided biopsy and treatment for prostate tumors, challenges the high cost of two newer treatments that dont have a clinical edge over less costly therapies. In an editorial he reviews two articles exploring high dollar outlay vs. benefits for proton beam radiation and robotic surgery.
Dr. Sperling questions the use of very expensive treatment for prostate cancer when the U.S. healthcare system is already overburdened. Currently, Medicare pays about twice as much for proton beam radiation as for other types of radiation. He acknowledges that proton beam is excellent for some rare cancers, but for prostate cancer it lacks long term data on success and side effects. He says, Further research is needed to justify the cost of proton beam for prostate cancer, study that should be covered by industry and grants, not Medicare payments.
Dr. Sperling also points out that the so-called advantages of robot-assisted prostatectomy may be overhyped. He writes, the issue is whether robotic prostatectomy offers clear benefits over other techniques, pointing to a recently published study showing that open surgery vs. robotic surgery had the same rates of incontinence and impotence. As for the healthcare system, a single robotic device adds over a million dollars to the costs.
What Are Some Common Uses Of The Procedure
A prostate biopsy is currently the only way to definitively diagnose prostate cancer. It also helps differentiate cancer from benign prostatic hyperplasia or nodular enlargement of the prostate, a very common condition in middle-aged and older men that requires a different treatment approach than that of cancer.
A prostate biopsy may be ordered if the physician detects a nodule or other abnormality on the prostate during a digital rectal examination , a common prostate cancer screening test.
A biopsy also may be ordered when a blood test reveals elevated levels of prostate-specific antigen. While there are several reasons for an elevated PSA level, higher PSA levels are sometimes associated with cancer. PSA trends over time may trigger your physician to order a biopsy.
MRI-guided prostate biopsy may be used in patients who have a rising PSA level yet a negative ultrasound-guided biopsy. It also may be used in situations where a diagnostic prostate MRI performed due to rising PSA demonstrates a very small abnormality that may not be easily targeted by ultrasound. MRI is also useful in patients who have previously undergone a biopsy and want to improve the sensitivity of the procedure and the precision of the biopsy.
A biopsy not only detects cancer it also provides information on the aggressiveness of the cancer and helps to guide treatment decisions.
Recommended Reading: Prostate Cancer And Lung Cancer
Who Interprets The Results And How Do I Get Them
A pathologist examines the removed tissue specimens and makes a final diagnosis. The results usually are available to your physician within a few days of the procedure. The time it takes may vary based on the complexity of the examination, preparation time for the specimens, need for a second opinion and other factors.
Benefits Of Getting A Prostate Biopsy
A prostate biopsy is the only way to definitively determine whether you have prostate cancer and, if you do, how aggressive it is.
While prostate biopsies arent always conclusive, in general, a biopsy gives men the reassurance of knowing whether they have cancer or not. If you know you have prostate cancer, youre more likely to be appropriately treated.
Appropriate prostate cancer treatment options depend on several factors, including the stage of the cancer, your age, your general health and which risk category your cancer falls into.
Localized prostate cancer is categorized into six risk categories, which range from very low-risk to very high-risk. The risk group is determined by the stage of your cancer, your PSA levels and the Gleason score obtained from the biopsy pathology report.
The National Comprehensive Cancer Network guidelines outline appropriate treatment options based on risk categories and whether the cancer has already metastasized.
Patients whose cancer is confined to the prostate and falls into the very low-risk and low-risk categories tend to have slow-growing cancers. Treatment options for these patients often include active surveillance, radiation therapy or surgery. Similar treatment options may be recommended to patients in the low-risk and favorable intermediate prostate cancer risk categories.
The NCCN guidelines recommend immediate treatment for patients with high-risk disease or those patients whose cancer has metastasized.
Read Also: What Vitamins To Take For Prostate Health
How To Get The Most For Your Money
Even if your insurance does cover some or most of your prostate biopsy, youll likely pay a portion of the total cost out-of-pocket. To make sure youre getting the most care for your money:
-
Ask your insurance company about your costs, like co-insurance, copays, and deductibles.
-
Utilize your Health Savings Account , Flexible Spending Account , and Health Reimbursement Account to cover out-of-pocket expenses.
-
Use Amino to compare prices for different doctors.
-
Have a conversation with your doctor. This is especially important if you dont have insurance and are paying for the full cost of the biopsy yourself. Some doctors will offer a discount or an interest-free payment plan if they know youre shouldering the cost on your own.
Additional Tests That May Aid Prostate Cancer Diagnosis
There are few other diagnostic tools or tests, which can be performed before you have a prostate biopsy, that may help your physician gather more information about your specific case. These procedures may help determine the likelihood of the presence of cancer and its aggressiveness and increase the accuracy of a biopsy when performed. Those tests include:
4Kscore blood test is a molecular test that helps predict the likelihood and risk of a patient having aggressive prostate cancer. If you’re a patient whose PSA values are borderline for a prostate biopsy or you have a condition that could be aggravated by a biopsy, your physician may use this test before to help determine whether you should get a biopsy or a repeat biopsy.
Urine sample testlooks for biomarkers that may indicate the presence of prostate cancer cells in a patient’s body. This test may also be helpful when trying to determine whether a patient should be rebiopsied or not.
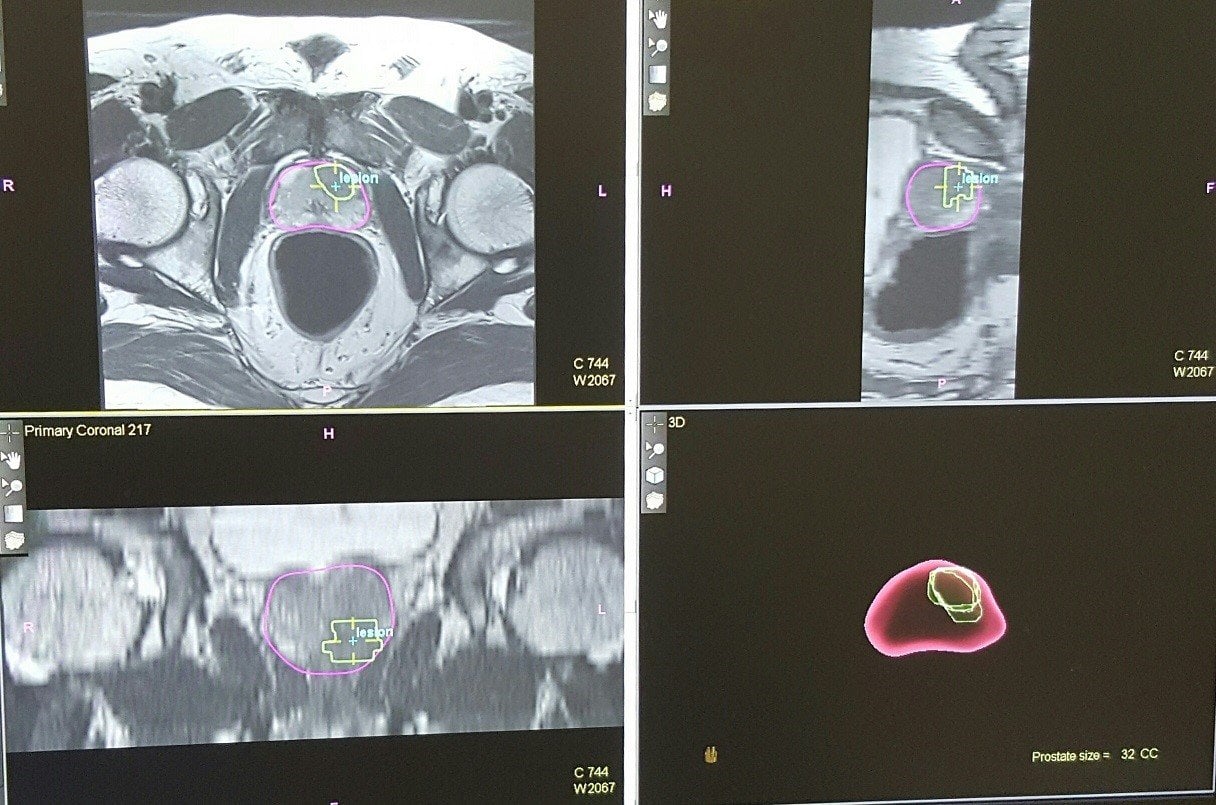
Multiparametric MRI
The use of multiparametric MRI imaging of the prostate gland before a biopsy has been a game changer in prostate cancer diagnosis, increasing the accuracy of biopsies over standard biopsies. The mpMRI doesn’t replace the standard biopsy, but by improving its accuracy, it may help decrease the number of biopsies needed.
The mpMRI has a higher resolution than a standard prostate ultrasound. This increases the ability to see suspicious lesions in the prostate, providing additional targets for the biopsy to sample.
Also Check: Prostate Cancer Pill Hope For Thousands
The Digital Rectal Exam
The prostate gland comprises three zones. Most cancers originate in the peripheral zone. Proctologists, urologists, and oncologists are trained to feel this area while performing a digital rectal exam .
Here, digital doesnt refer to technology. Instead, it refers to the fingers . In a DRE, your doctor inserts a well-lubricated gloved finger gently into the rectum to reach the prostate. Prostate enlargement and suspicious lesions may be felt during a DRE.
What Should I Expect From A Prostate Biopsy
A prostate biopsy may be recommended if the results of a digital rectal examination or prostate-specific antigen test suggest that prostate cancer may be present. The most common approach for performing this diagnostic test is transrectal, in which a needle is carefully passed through the wall of the rectum to retrieve a prostate tissue sample.
Recommended Reading: Monoclonal Antibody Therapy For Prostate Cancer
Prostate Biopsy Side Effects Are Common
Complications from prostate biopsies are common but usually not severe, a study in Urology reveals. Participants in the study had biopsies to look for cancer after an abnormal rectal exam or prostate-specific antigen blood test. In a biopsy, a fine needle punches quickly through the rectal wall to remove a tiny sample of prostate tissue for examination under a microscope. Doctors took 12, 18, or 24 samples per participant. Typical problems from biopsy include pain, soreness, and infections. A more serious complication, which may lead to hospital admission, is acute urinary retention, in which a man is temporarily unable to drain his bladder.
Here is what the study found:
-
40% of the men experienced a complication.
-
The complication rate was as high as 57% in men with 24-sample biopsies.
-
Only 1.2% of the men required hospital admission.
-
9.1% ended up visiting an emergency room.
-
6.7% developed acute urinary retention.
Prostate needle biopsy is the only way to diagnose prostate cancer, regardless of PSA test results. The complication rate would vary with the general health of the men involved.
To continue reading this article, you must log in.
- Research health conditions
- Prepare for a doctors visit or test
- Find the best treatments and procedures for you
- Explore options for better nutrition and exercise
Painful Prostate Biopsy Heres What You Need To Know
A standout amongst the most famous symptomatic tests performed to recognize Prostate Cancer is Biopsy. If you are experiencing pee issues, erectile brokenness, or any prostate-related indications and would look for medical counsel from a medical expert, the standard suggestion would either be for you to experience the PSA test first then Prostate Biopsy or the last quickly.
Dont Miss: Can Prostate Issues Cause Erectile Dysfunction
Don’t Miss: What Does Low Grade Prostate Cancer Mean
Men With Prostate Cancer Willing To Pay More For Advanced Biopsies
We were unable to process your request. Please try again later. If you continue to have this issue please contact .
Men with prostate cancer paid up to $2,000 out of health savings accounts for magnetic resonance imagingtransrectal ultrasound fusionguided prostate biopsies, according to an analysis published in Urology Practice.
We have increasingly observed that some insurance companies are not covering prostate magnetic resonance imagingtransrectal ultrasound fusion biopsies and that some patients are paying out of pocket for these biopsies because they have a health savings account or high deductible coverage,Chad Ellimoottil, MD, MS, assistant professor of urologic health services in the Dow Health Services Research division at University of Michigan, told HemOnc Today. The purpose of the study was to understand how much patients would be willing to spend from a health savings account for a biopsy intervention with attributes similar to prostate magnetic resonance imagingtransrectal ultrasound fusion biopsies.
Chad Ellimoottil
Over the last 10 years, the number of employers offering health care savings accounts has grown tenfold, and approximately 1 million individuals start a new account each year. The Employee Benefit Research Institute estimates $2,000 is the average amount individuals have in health care savings accounts.
The most common age group of men who participated in the conjoint survey was 61 to 65 years .
Reference:
For more information: